Abstract
Introduction:
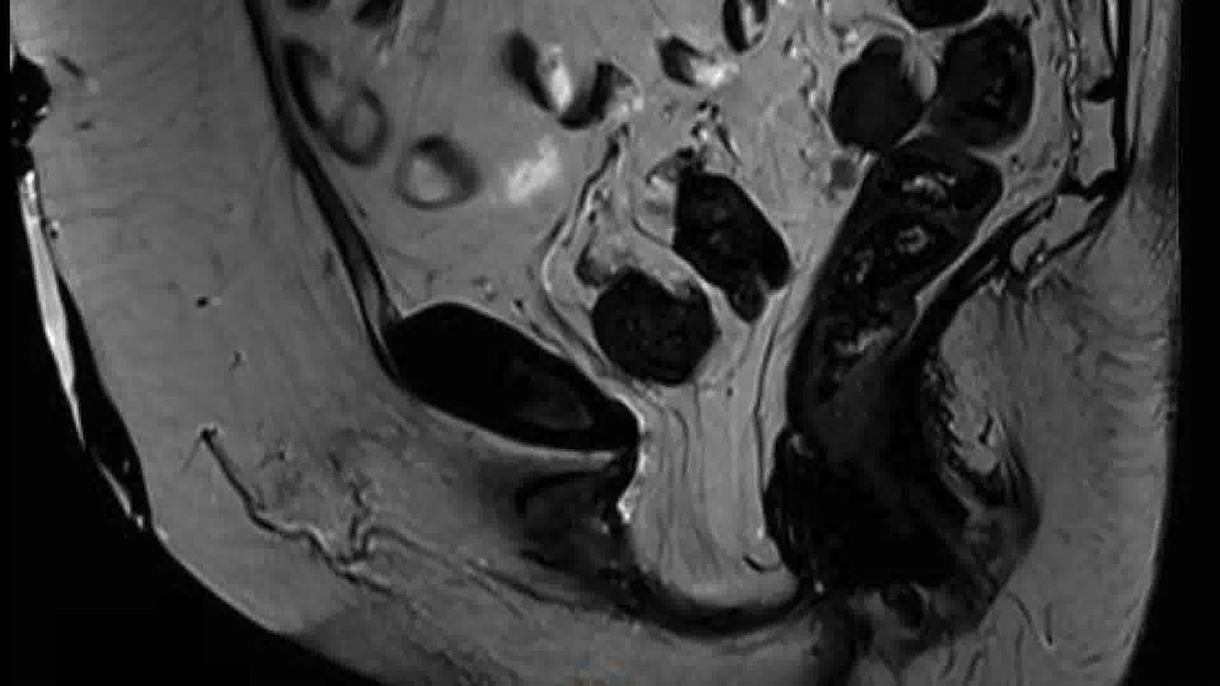
Vaginal complications are diagnosed in around 20% of women following radical cystectomy. Vaginal dehiscence is the most frequently observed of the three types of complications seen, which also include vaginal prolapse and fistula. A dehiscence occurs when the vaginal closure fails and a hernia is formed. It can present early, within 3 months of surgery, but has also been described as presenting over 12 months after cystectomy. The hernia sack is lined with peritoneum and may be empty or contain pelvic contents. Symptoms include vaginal discharge, vaginal bulge, or a more acute presentation with evisceration of the pelvic contents and bowel obstruction. Surgical repair of dehiscence is therefore recommended, but the optimum technique is not known. Open, robotic, and vaginal techniques have been described using primary closure, myo-cutaneous flaps, and synthetic meshes. Here, we present a robotic-assisted transabdominal approach utilizing a biological mesh. To our knowledge, this is the first description of this technique.
Materials and Methods:
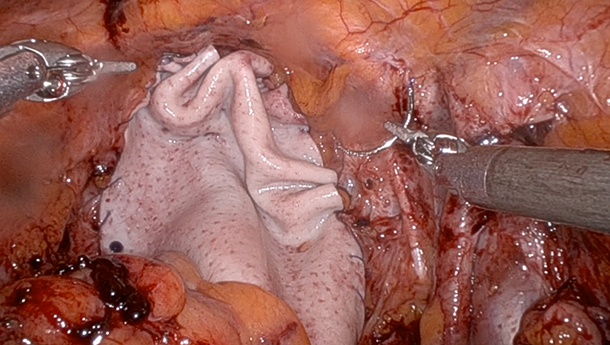
The steps of the technique presented are described in the video. The robotic-assisted approach utilizes STRATTICE™ Reconstructive Tissue Matrix (RTM), a porcine-derived soft tissue patch. Four patients underwent repair of vaginal dehiscence using this technique between January and May 2024 at a single center. They were followed up prospectively, using a symptoms enquiry at 3 and 12 months. MRI imaging was performed in the case of recurrent vaginal symptoms. Routine cancer follow-up imaging was also performed.
Results:
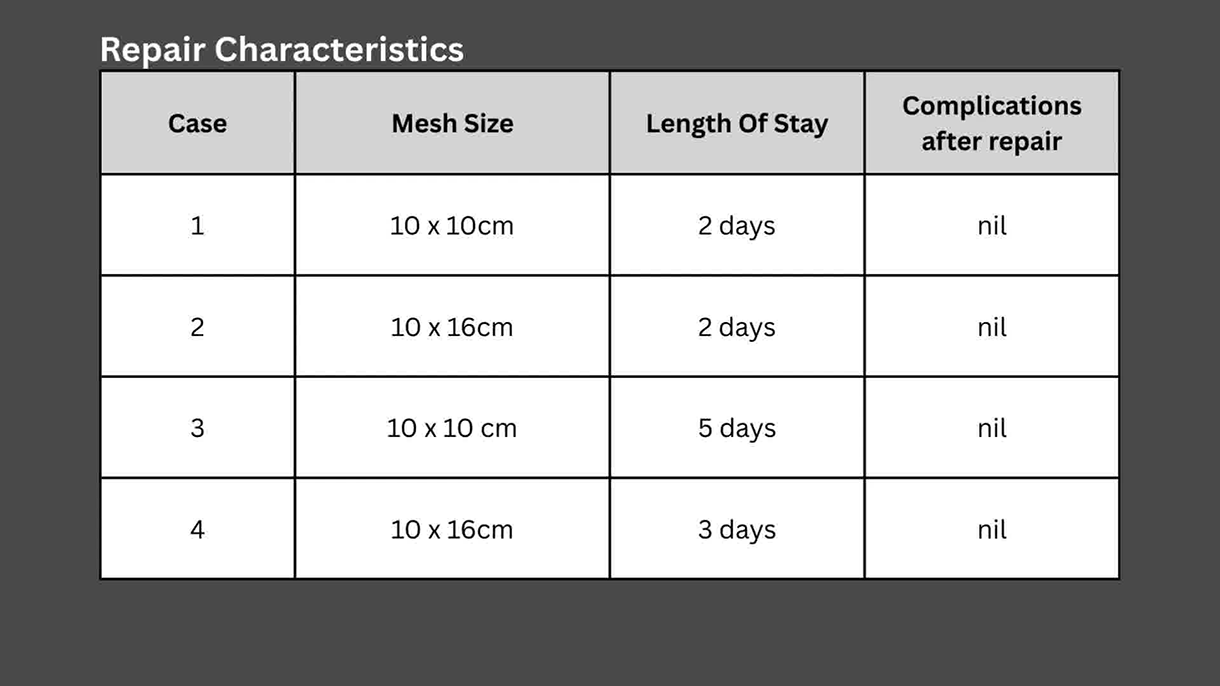
Full patient characteristics are described in the video presentation. The four women were aged between 68 and 77 years and were diagnosed with vaginal dehiscence between 4 and 46 months following robotic-assisted radical cystectomy for bladder cancer. In the 30 days following repair, there were no postoperative complications. In the 12 month follow-up period, two patients had recurrent vaginal symptoms and had evidence of pelvic organ prolapse on examination and imaging. Both patients had a history of pelvic organ prolapse before radical cystectomy and opted for conservative management of their symptoms going forward. No patient experienced a recurrence of vaginal dehiscence.
Conclusions:
We have demonstrated the successful repair of vaginal dehiscence through a robotic-assisted transabdominal approach using a soft tissue patch. The effect was durable for 12 months, but further follow-up will be needed to assess longer-term outcomes. The technique is straightforward and achievable by robotically trained pelvic surgeons, offering an advantage over vaginal repair or flaps, which some cystectomists may have limited familiarity with. The key disadvantage of the repair is that it does not address pelvic organ prolapse. Women with a history of prolapse should be counselled that a prolapse will not be treated and some vaginal symptoms are likely to persist.
The authors confirm they have received and archived patient consent for video recording/publication in advance of video recording of the procedure.
The authors have no relevant conflicts of interest to declare.
Runtime of video: 7 mins 25 secs.
Get full access to this article
View all access options for this article.
