Abstract

Introduction and Objectives:
Traditionally, robot-assisted kidney transplant (RAKT) has been performed using the transperitoneal approach (TP-RAKT), which presents certain limitations. One of the main concerns is the requirement for a steep Trendelenburg position for an extended period of time. Additionally, this approach violates the peritoneal barrier, potentially resulting in prolonged postoperative ileus and postoperative pain. In this video, we describe the surgical steps and techniques of multi-port extraperitoneal RAKT (EP-RAKT). Additionally, we have compared the outcomes of the EP-RAKT cohort with the transperitoneal approach.
Materials and Methods:
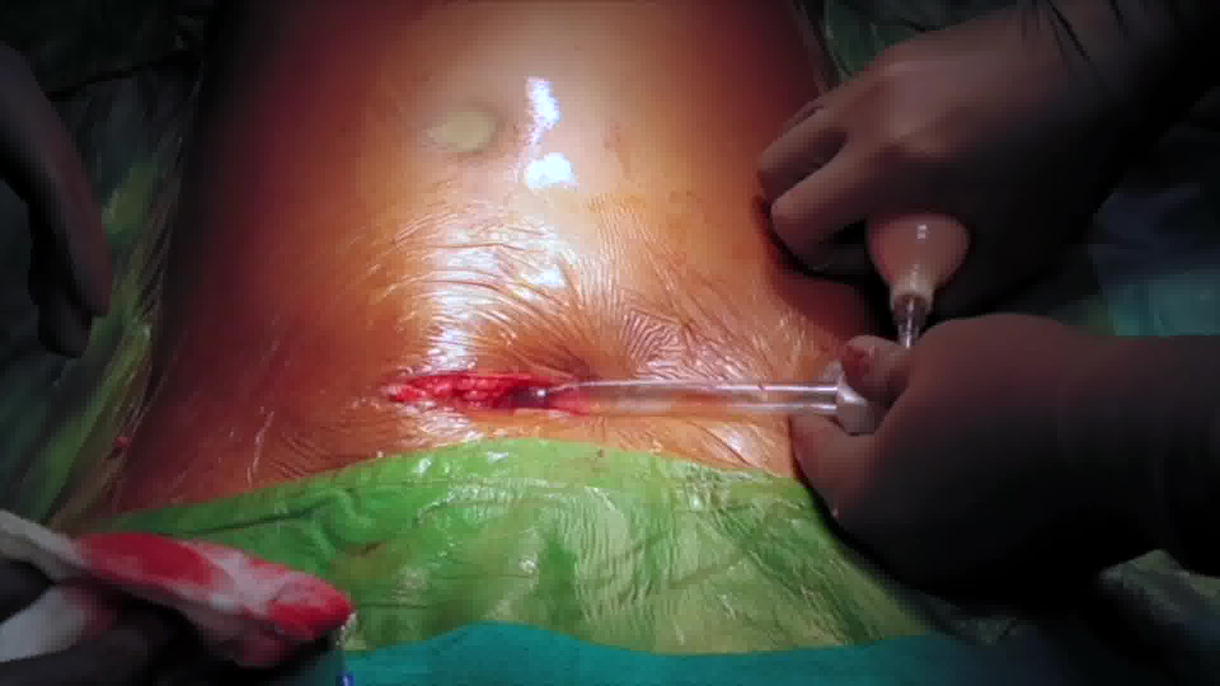
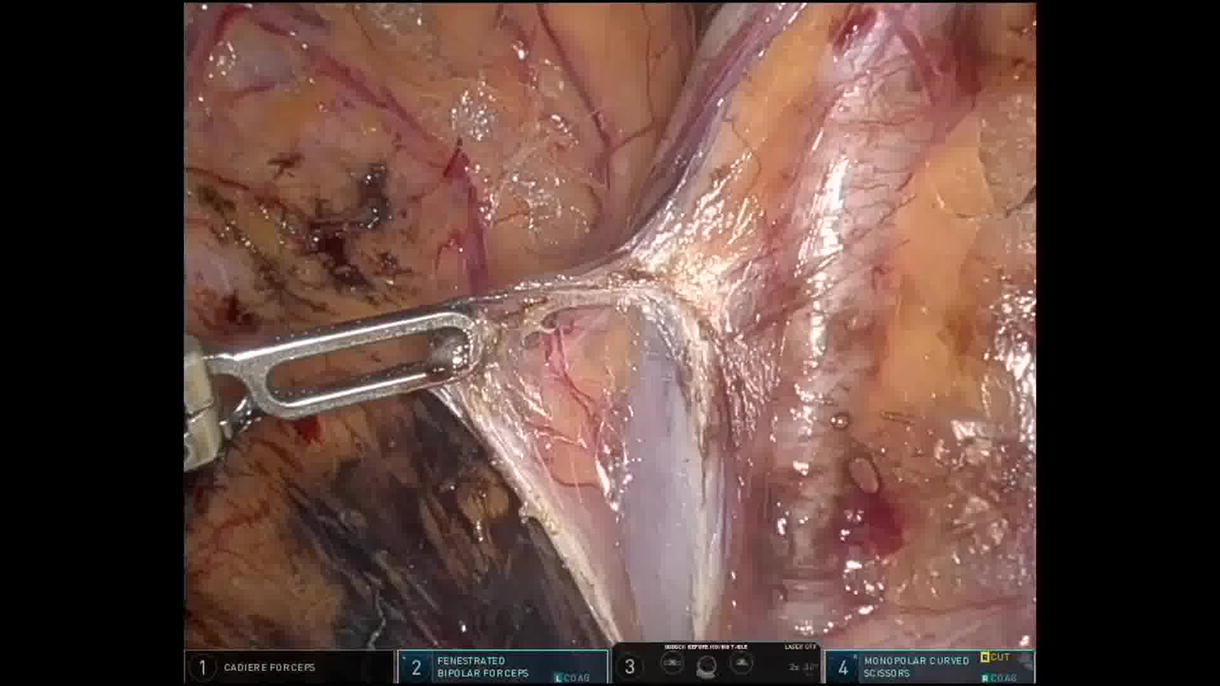
After infield catheterization, a 5–6 cm Pfannenstiel incision was made in the supine position. Extraperitoneal space was developed with a Spacemaker PDB® balloon (Medtronic, Dublin, Ireland). The ALEXIS® access device was placed, and four standard robotic and one assistant port were inserted. Patient was positioned in a mild Trendelenburg position (5°−10°), and side docking was done from the left side of the patient. The external iliac artery and vein were carefully dissected after sweeping the peritoneum, and at last the bladder was prepared. The kidney was then wrapped in a jacket full of ice and introduced into the extraperitoneal space via the ALEXIS® port. The venous and arterial anastomoses were performed using 6-0 GORETEX® sutures. After vascular anastomosis, the robot was undocked, and the Trendelenberg position was slightly increased from 10° to 20° for 20–25 minutes to displace the bowel cranially and flip the kidney to the lateral side to perform ureterovesical anastomosis. We reviewed our prospective database of patients who underwent RAKT with an extraperitoneal approach between June 2023 and May 2024.
Results:
EP-RAKT with living donor nephrectomy has been performed successfully for 10 patients without any complications or conversions, and they were propensity matched with 20 patients for confounding variables (age, sex, BMI, graft kidney GFR, and graft number of vessels) who underwent TP-RAKT. Mean vein and artery anastomosis times were 18.5 ± 4.03 and 17.5 ± 3.04 minutes, respectively, with no significant difference between the transperitoneal cohort. However, the mean total operative time (288 ± 35.2 vs. 240 ± 28.2 min, p < 0.0001) and the mean time spent in port placement and bed preparation (50.8 ± 8.4 vs. 28.3 ± 6.1 min, p < 0.0001) were longer in EP-RAKT versus TP-RAKT. All grafts were perfused well, and serum creatinine levels returned to normal between 4 and 7 days. The extraperitoneal approach is associated with overall decreased postoperative ileus (1.3 ± 0.48 vs. 2.9 ± 0.6 days, p < 0.0001), pain scores (10.2 ± 1.75 vs. 14.8 ± 2.3 on VAS, p < 0.0001), and drain output (131.5 ± 34.16 vs. 786 ± 151.6 mL, p < 0.0001), as compared to the transperitoneal approach. Tacrolimus levels were consistently in the therapeutic range in the early postoperative period. Mean creatinine levels were 1.01 ± 0.17 mg/dL at 3 months of follow-up.
Conclusions:
The EP-RAKT has similar functional outcomes of graft but with reduced morbidity and minimal complications, compared to TP-RAKT. These findings suggest that EP-RAKT is a safe and feasible alternative for patients and has the potential to become the standard for minimally invasive kidney transplant.
Patient Consent Statement:
Informed consent to participate was obtained from the patient. Written informed consent for the publication of details, images, and videos was obtained from the patient.
Conflict of Interest Statement:
The authors declare that they have no competing interests of conflict of interest.
Author Disclosure Statement:
The authors declare that they have had no commercial associations during the last 3 years that might create a conflict of interest in connection with the video. Authors have received and archived patient consent for video recording/publication in advance of the video recording of the procedure.
Source of Support and Funding:
No funding involved.
Runtime of video: 8 mins.
Keywords
Get full access to this article
View all access options for this article.
