Abstract

Introduction:
Benign prostatic obstruction is a leading cause of lower urinary tract symptoms (LUTS) in aging males. Anatomical endoscopic enucleation of the prostate has emerged as a gold standard surgical approach; however, its adoption is limited due to the risk of urethral trauma, sphincteric injury, and a steep learning curve. The MiPThuLEP-Ultra Slim technique addresses these concerns by combining pulsed thulium laser energy with ultra-slim bipolar instrumentation (18.5 Fr), enabling complete en bloc enucleation with early, progressive, and controlled sphincter disinsertion while minimizing mucosal and capsular trauma.
Materials and Methods:
A 52-year-old male with a 6-year history of progressive LUTS (IPSS 18, Qmax 13 mL/s, PVR 300 mL) and a prostate volume of 51 cc underwent enucleation using the MiPThuLEP-Ultra Slim technique. Urethrocystoscopy demonstrated trilobar growth, a 3 cm prostatic urethra, and bladder trabeculation. The procedure utilized an 18.5 Fr bipolar resectoscope with a 0.8 mm laser channel, a 30° 2.9 mm optic, and a continuous irrigation system. A pulsed thulium laser (CyberTM, 100 W) with a 600 µm fiber was used. Settings were adjusted to 60 W (0.6 J at 100 Hz) for mucosal incision and hemostasis and 100 W (2 J at 50 Hz) for adenoma dissection, with a short pulse width of <500 µs. Morcellation was performed using a 22 Fr morcelloscope and a Hawk blade under direct 0° visualization. Irrigation was gravity-fed using a saline bag 60 cm above the patient and connected to an inverted, single-entry metallic cone for closed-loop flow without bladder decompression.
Surgical Technique:
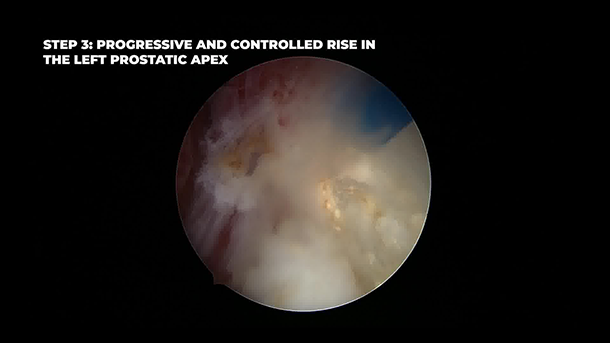
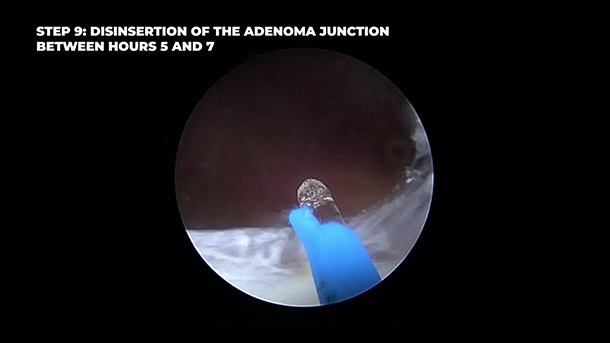
Step 1: Identification of the dissection plane at the verumontanum—left lobe commissure. Step 2: Mirror incision on the right lobe, forming an inverted U. Step 3: Left sphincter disinsertion 3 mm below mucosa, ascending to 12 o’clock. Step 4: Right sphincter disinsertion with symmetric technique. Step 5: Enucleation of the anterior apex using capsular fibers as an anatomical reference. Step 6: Circumferential detachment of the adenoma toward the bladder, preserving capsule contact. Step 7: Entry into the bladder at 12 o’clock via inverted U incision. Step 8: Clockwise bladder neck shaping (12–5 o’clock), identifying the left ureteral orifice. Step 9: Counterclockwise bladder neck dissection (12–7 o’clock), identifying the right ureteral orifice. Step 10: Detachment of posterior junction (5–7 o’clock) and targeted laser hemostasis. Step 11: Morcellation without bladder decompression using closed, gravity-based irrigation.
Results:
Operative time was 60 minutes. The enucleated lobe weighed 49 g. Blood loss was minimal (50 mL). The catheter was removed after 18 hours. At the 1-month follow-up, the patient reported no incontinence or hematuria. IPSS improved to 6, and Qmax to 18 mL/s. No strictures or bladder neck contractures were observed. Pathology confirmed benign prostatic hyperplasia.
Conclusion:
MiPThuLEP-Ultra Slim enables safe, efficient enucleation in medium-sized prostates (<80 g) using ultra-slim instrumentation and precise, energy-controlled dissection. It reduces morbidity, preserves continence, and offers reproducible outcomes.
Patient Consent:
Written informed consent for video recording and publication was obtained and archived.
The authors declare no financial support or industry affiliation.
Runtime of video: 9 mins 10 secs.
Keywords
Get full access to this article
View all access options for this article.
