Abstract
A surgically challenging case of an unruptured Sinus of Valsalva aneurysm (SoVA) with severe aortic regurgitation (AR) due to cusp prolapse is presented. Sinus reconstruction with a patch cut out from the sinus portion of a Gelweave Valsalva graft (Terumo Vascutek) was performed. Intraoperative measurements showed insufficient effective height of the right coronary cusp; therefore, cusp plication and pericardial patch augmentation of the right coronary cusp were performed with satisfying result.
Introduction
Sinus of Valsalva aneurysm (SoVA) is an uncommon clinical entity. In the majority of cases, repair of the SoVA is performed using a polytetrafluoroethylene (PTFE) or autologous pericardial patch. 1 Additional aortic valve repair or replacement is often necessary for patients with aortic regurgitation (AR). We present a patient with a large SoVA with severe AR who was treated with selective reconstruction of the right coronary sinus with a Valsalva graft patch and additional cusp plication and extension.
Case
A 62-year-old man presented at the emergency department after syncope during exertion. On physical examination, he had a diastolic murmur and blood pressure of 171/66 mm Hg. Transthoracic echocardiography (TTE) showed severe AR. Three-dimensional transesophageal echocardiography (3D-TEE) revealed a large SoVA of the right coronary sinus with prolapse of the right coronary cusp resulting in leaflet malcoaptation and consequent severe eccentric AR (Figure 1A) with a preserved annular dimension (25 mm). Additional computed tomography (CT) imaging was performed to assess the relation between the aneurysm and the origin of the right coronary artery (RCA), which was just distal to the SoVA at the sinutubular junction (Figure 1B).

(A) Transesophageal echocardiography: sinus of Valsalva aneurysm with prolapse of the right coronary cusp with severe eccentric aortic regurgitation. (B) Computed tomography: relation between sinus of Valsalva aneurysm (*) and right coronary artery (arrow).
Under general anesthesia, a median sternotomy was performed and cardiopulmonary bypass was instituted. After transection of the aorta, the sinus of Valsalva aneurysm was inspected. Neither rupture of the aneurysm into the right ventricle nor a ventricular septal defect was found (Figure 2A). Selective sinus reconstruction using a patch cut from the sinus portion of a 26 mm Valsalva aortic prosthesis Gelweave ValsalvaTM graft (Terumo Vascutek) was performed. The Gelweave ValsalvaTM graft sinus part has longitudinal corrugations and is concave shaped, which is appropriate for use as a neo-sinus. The SoVA was entirely excluded by implantation of the Valsalva graft patch. In addition, the prolapse of the right cusp was addressed. The effective height of the right coronary cusp was <9 mm; therefore, central plication and extension of the cusp with a strip of untreated autologous pericardium were performed. Perioperative 3D-TEE showed a satisfying result with good coaptation length (10-11 mm) and effective height (13-14 mm) with only a trace residual central AR (grade <1). The postoperative course was uneventful, and the patient was fully recovered 3 months postoperatively.
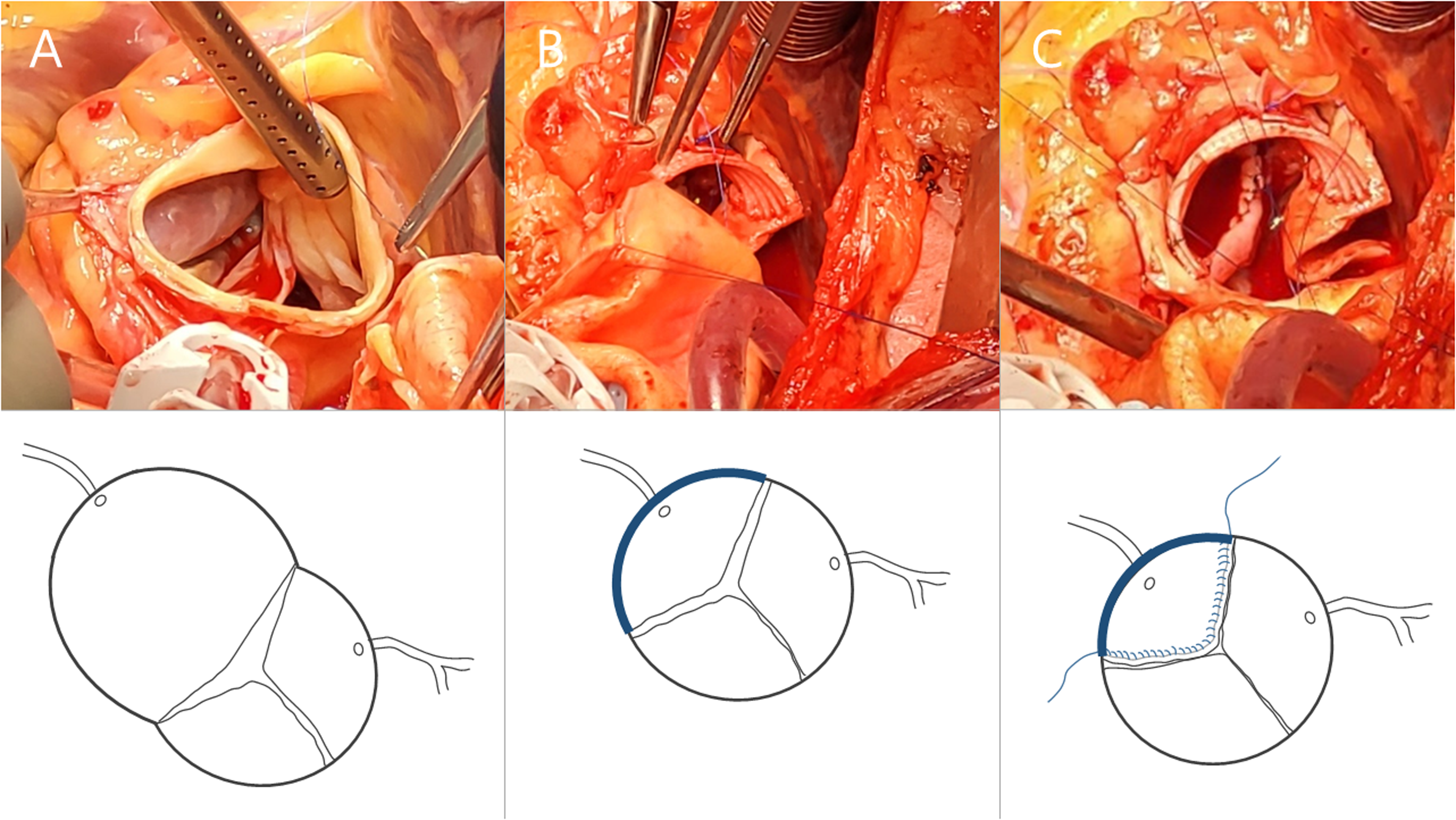
Intraoperative photographs and schematic line drawings of the various surgical stages. (A) Inspection of the sinus of Valsalva aneurysm. (B) 26 mm GelweaveTM Valsalva prosthesis of which the left- and noncoronary sinus of the graft are removed, is implanted in the right coronary sinus. (C) Extension of the right coronary cusp with a strip of autologous pericardium to increase effective height to >9 mm.
Comment
The diagnosis of SoVA is made using multimodality imaging. In particular, when there is an indication for surgery due to the size of the aneurysm and/or severe AR, TEE, and CT are useful to clarify the exact anatomy and determine the surgical strategy. 2 In cases with significant AR, accurate preoperative echocardiographic analysis is of paramount importance when a valve-sparing approach is desired. 3 The preoperative TEE protocol consists of measurement of aorta diameters, determination of aortic valve phenotype (bicuspid or tricuspid), assessment of the mechanism of AR, and evaluation of valve tissue (by measuring effective height and coaptation length). 3
Even when the coexisting AR is mild in SoVA, there is a substantial risk of postoperative worsening of the AR. In a series of 198 SoVA cases, 75 had accompanying AR of which 74 were mild and none were severe. 4 Of these cases, 44 underwent aortic valve repair or replacement. However, in almost 20%, postoperative AR progression was present, which was newly developed in about half of the cases. 4 This observation highlights the importance of considering restoring valvular competence even in cases with limited AR. Lansac and colleagues have proposed a standardized approach aiming for an effective height of ≥9 mm, which is protective from postoperative significant AR and reoperation. 5 In addition, even mild residual AR (grade ≥1) on intraoperative TEE may be associated with recurrent significant AR during follow-up. 6 Controversy persists regarding the preferred material for aortic valve cusp extension. In some reports, the use of glutaraldehyde-treated pericardium for aortic valve cusp extension has been associated with recurrent AR and the need for reoperation.7,8 When the effective height is <9 mm, our preference is to utilize other cusp repair techniques, including central plication, and to use untreated autologous pericardium when cusp extension is required. In the case presented, both the aneurysm and cusp prolapse could be effectively repaired by limited surgery creating a new sinus wall and repairing the pertinent coronary cusp.
Conclusion
In patients with SoVA and associated AR, repair of the sinus and cusp should be performed, aiming for an effective height of ≥9 mm to obtain a durable result. The use of the concave-shaped Gelweave ValsalvaTM graft allows shaping of the neo-sinus and might improve valvular competence.
Footnotes
Authors’ Statement
The permission to publish this case report was obtained from the parents.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
