Abstract
Vaccine preventable diseases are responsible for a substantial degree of morbidity in the United States as over 18 million annual cases of vaccine preventable disease occur in the U.S. annually. The morbidity due to vaccine preventable disease is disproportionately borne by adults as over 99% of the deaths due to vaccine preventable diseases occur within adults, and national data indicates that there racial disparities in the receipt of vaccines intended for elderly adults. A literature review was conducted by using the PubMed database to identify research articles that contained information on the vaccination rates among minority populations for selected vaccines intended for use in elderly populations including those for herpes zoster, tetanus, diphtheria, pertussis, hepatitis A, and hepatitis B. A total of 22 articles were identified, 8 of which focused on tetanus related vaccines, 2 of which focused on hepatitis related vaccines, and 12 of which focused on herpes zoster. The findings indicate that magnitude of the disparity for the receipt of tetanus and herpes related vaccines is not decreasing over time. Elderly patients having a low awareness of vaccines and suboptimal knowledge for when or if they should receive specific vaccines remains a key contributor to suboptimal vaccination rates. There is an urgent need for more intervention-based studies to enhance the uptake of vaccines within elderly populations, particularly among ethnic minorities where culturally sensitive and tailored messages may be of use.
Keywords
Introduction
Vaccines play an invaluable role in preventing morbidity and mortality associated with infectious disease. Vaccination within the United States saves 12 000 lives and prevents 20 million cases of disease annually. 1 While vaccination rates among children routinely exceed 90%, adults have suboptimal vaccination rates and incur more morbidity and mortality from vaccine preventable diseases. 2 Overall, 99% of deaths from vaccine preventable diseases occur within adults, 2 and over 18 million cases of these diseases occur in adults each year with an economic burden of $9 billion. 3 The most common vaccine preventable disease is influenza, which typically affects more than 16 million adults in the United States annually. 3 Although the annual incidence of influenza is slightly greater among adults younger than 50, 4 adults over age 50 have far higher mortality rates due to influenza. 5 Non-influenza vaccine preventable diseases such as pneumonia and herpes zoster occur more frequently in elderly adults at least 50 years old and are more likely to lead to fatality in older adults. 6
Racial and ethnic minorities are disproportionately affected by vaccine preventable diseases. Blacks are nearly twice as likely as whites to be hospitalized for influenza,7,8 and Hispanics are also more likely to be hospitalized for influenza. 7 Blacks and Native Americans are also more likely to be hospitalized for pneumonia compared to whites. 9 Moreover, Blacks hospitalized for pneumonia are more likely to die within the hospital and have a longer length of stay compared to Whites. 10 Numerous social, economic, and geographical determinants contribute to the disproportionate burden of vaccine preventable diseases borne by minority populations. Individuals living in impoverished, crowded conditions, and households headed by females are more likely to be hospitalized for influenza.7,8 Living in a socioeconomically deprived neighborhood is also a risk factor for higher mortality among those hospitalized for pneumonia. 11 Geographic areas with higher proportions of Blacks such as the Southeastern United States have higher pneumonia related hospitalization and mortality rates in comparison to regions such as the West where there are fewer Blacks.9,12
A substantial amount of research has focused on the persistent racial and ethnic disparities in influenza and pneumococcal vaccination rates with most of the evidence focused on African Americans. 13 Among elderly African Americans, prominent reasons for not receiving the influenza vaccine include not having a regular physician, lower income, and lack of private insurance coverage. 14 African Americans also mistrust institutions and systems involved in vaccine development such as pharmaceutical companies and the federal government. 15 Social norms play a role in the decreased uptake of vaccines among African Americans wherein they are less likely to believe their friends and loved ones want them to receive a vaccination. 16 While individuals living in the Southeast United States and metropolitan regions may be less likely to receive the influenza vaccine in general, 17 there are notable differences within regions regarding the receipt of the vaccine among different ethnic groups. For example, within New York City and metropolitan Los Angeles, Blacks are less likely to receive the influenza vaccine in comparison to Hispanics, Chinese, Korean, Filipino, and Vietnamese individuals, although there were no differences of note between these populations with receipt of the pneumococcal vaccine. 18
In a fashion similar to Blacks, income and lack of private insurance are associated with vaccine related disparities among Hispanics, yet geographical region plays a larger role. 14 This is illustrated by a study in metropolitan Chicago that included Mexican and Puerto Rican respondents that found the percentage of those receiving the pneumococcal vaccine among those at least 65 varied from 18% to 91% based on location. 19 Emerging evidence examines influenza vaccine uptake among groups other than African Americans and Hispanics. For example Arab Americans in California were 10% less likely to receive the influenza vaccine in comparison to whites, yet there were no appreciable differences after adjusting for health behaviors, sociodemographic variables and acculturation status. 20 National level data indicate that some Asian American subgroups such as Asian Indians and select other Asian groups may actually have higher influenza vaccination rates in comparison to Whites in some instances. 21 Collectively the data indicates that Blacks and Hispanics are the most vulnerable racial and ethnic subgroups with regards to influenza and pneumococcal related vaccine disparities.
There are also racial and ethnic disparities with regards to other vaccines recommended for elderly adults in the U.S such as the (tetanus and diphtheria with acellular pertussis [Tdap], hepatitis A (hep A), hepatitis B (hep B), and herpes zoster vaccines. 22 Ameliorating these disparities would be quite beneficial, as achieving health equity for herpes zoster related vaccination rates in Blacks that are similar to those seen within whites would prevent over 34 000 cases of herpes zoster among the current cohort of elderly Blacks while averting over $180 million in economic costs. 23 Although the reasons surrounding the disparities seen between majority populations and Blacks regarding influenza and pneumococcal vaccine related disparities have been well studied,14,24,25,26 the mechanisms underlying the persistent disparities seen among elderly minority and majority populations for other adult vaccinations are less understood. Accordingly, this review was undertaken to evaluate the trends seen in immunization related disparities for elderly adults in the hepatitis, herpes zoster, and Tdap vaccines and elucidate the reasons contributing to these disparities.
Methods
Search Strategy
A predetermined protocol was used to search for and identify relevant articles by using the PubMed database. The search strategy was designed to find articles that contained information on minorities and had some means of assessing their vaccination rates and their knowledge, attitudes, and beliefs toward receiving these vaccines. The search was also conducted in a manner to elicit information regarding vaccination among adults within the United States. Further information regarding the search strategy is available in Table 1.
Description of Search Terms.

Inclusion/Exclusion Criteria
The search was restricted to articles written in the English language. Articles were excluded if they did not have any data documenting immunization rates for Tdap, hepatitis A, hepatitis B, or herpes zoster vaccines in a minority population. In order to be included, studies had to have information presented on vaccination rates for elderly minority populations at least 60 years old.
Selection of Studies
The titles and abstracts of studies were screened to determine if they were in conformity with the predefined inclusion an exclusion criteria. The full text of articles was retrieved in cases where there was some degree of uncertainty regarding the relevance of an article. Reviewers also scanned the reference section of relevant articles identified during searches. Information that was obtained from the articles was placed into a Microsoft Excel file for data abstraction. The data that was placed in the Excel sheet contained information on the inclusion and exclusion criteria, the study population, location, and the primary findings of the study.
Results
Tetanus and TDAP Related Studies
As seen in Table 2, there were 8 studies that documented immunization rates amongst minorities for TDAP from 2000 to 2016.22,27,28-33 All of these were observational studies. Many of the studies utilized data from the National Health Interview Survey (NHIS) which is conducted on a yearly basis by the CDC to gather nationally representative data about the health status of the United States population. These studies generally demonstrated that Blacks, Hispanics and in many cases Asians received tetanus related vaccines at significantly lower rates than whites.22,28-30,32,33 Lu et al 27 utilized data from the 2012 NHIS survey to analyze the proportion of minority patients that had received the pertussis vaccine during the previous decade. In unadjusted analysis, whites were found to have higher immunization rates than both Blacks and Hispanics. However in unadjusted analysis, the immunization rate for whites (56.4%) was only significantly higher than that of Blacks (48.7%).
Findings Related to Disparities in Vaccinations Among Adults at Least 60 Years Old.
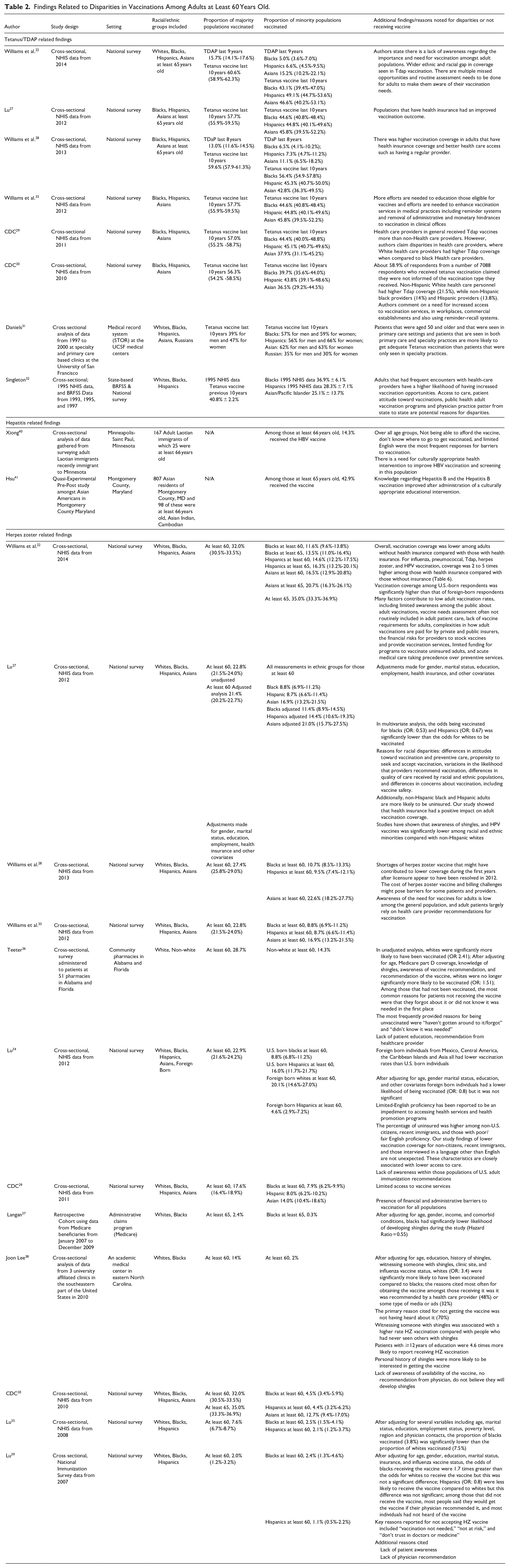
There were 2 studies that explored factors associated with receipt of vaccines containing tetanus. While using national level data, Singleton et al 32 found that Asian/Pacific Islanders and Hispanics at least 65 were less likely to receive the tetanus vaccine compared to Non-Hispanic whites. The study findings also indicated that lower education and income levels were associated with being less likely to receive the tetanus vaccine. A study conducted in San Francisco demonstrated that Hispanics, Blacks, and Asians at least 65 were actually more likely to receive the tetanus vaccine compared to Whites. 31 Moreover, elderly adults who saw a primary care physician were more likely to receive the vaccine compared to those only visiting a specialty clinic.
Herpes Zoster Vaccine
Several studies have been conducted that document the immunization rates of herpes zoster in minorities. The majority of these studies employ a cross sectional study design and utilize data from the NHIS.22,27,28-30,33-35 These studies conclusively demonstrate that Whites consistently have higher immunization rates than Blacks and Hispanics in those at least 60. Recent data indicates that the immunization rate for whites at least age 60 is 32.0% which is significantly higher than the rates seen in Blacks (11.6%) and Hispanics (14.6%) in 2014. These data demonstrate how much the immunization rates have increased since 2008. At that time less than 8% of whites had received the vaccine and less than 3% of Blacks and Hispanics had received the vaccine. 35
Several of the studies examining disparities in herpes zoster vaccination rates examined additional factors beyond race and ethnicity that may influence immunization rates.27,34-39 In many cases, after adjusting for gender, marital status, education, employment, insurance status, and age whites were still more likely to be vaccinated than other groups.27,35,37,38 However, there were some cases where whites were not more likely to be vaccinated after adjusting for other factors.34,36,39 Data from these studies suggest that the absolute differences observed in immunization rates between whites and minorities may at least in part be explained by knowledge of shingles, awareness of recommendations to receive the vaccine, and receipt of the influenza vaccine.
Quite a few studies demonstrated that Asians also have lower rates of the shingles vaccine than whites as well.22,28-30,33 There were also analyses that demonstrated that foreign born individuals had lower immunization rates than whites, but these results were not significant after accounting for other factors. 34
One of the most consistent reasons cited for not being vaccinated for herpes zoster among seniors was a lack of awareness of the vaccine or the fact that the vaccine is recommended for them.36,38,39 African Americans were less likely to be aware of the vaccine when compared to Whites.38,39 One reason given for lack of awareness is the lack of recommendations from health care providers, although the majority of the elderly state that if a health care provider had recommended the vaccine, they would have accepted the vaccine.38,39
Hepatitis A and Hepatitis B
Two studies evaluated vaccination rates for hepatitis B vaccines in elderly minority patients. Xiong et al 40 conducted an observational study of Laotian immigrants in Minnesota. Out of a cohort of 125 patients, a total of 25 were at least 66 years old, and 2 of these patients (8%) had received the hepatitis B vaccine. The majority of respondents from all ages indicated that they had no knowledge of the vaccine, and the most common barriers to receiving the vaccine were affordability and not knowing where to go to get it. Hsu et al 41 conducted a quasi-experimental pre-post study evaluating the use and knowledge of hepatitis B vaccine in Asian populations of Montgomery County, Maryland. Administration of a culturally appropriate educational intervention to the patients increased their knowledge of hepatitis B and the hepatitis B vaccine.
Discussion
In this review, African Americans, Hispanics, and Asians were consistently demonstrated to have lower immunization rates in comparison to whites for vaccines indicated for elderly adults, many times after adjusting for other important factors. There were some factors which contributed to differences in receipt of the vaccines including senior’s awareness of the vaccines,36,38,39 health care provider recommendations,36,39,42 and interaction with primary care providers. 31 There were some instances where financial payments presented an obstacle, 40 but this was not a universal occurrence, most likely due to the vaccines being covered by Medicare insurance.
One of the most concerning findings from this study is the realization that the disparities in immunization rates among elderly adults have not decreased in an appreciable manner over time. Recent data indicate there was a 17.5% gap in the national immunization rates between elderly Whites and Blacks for the tetanus vaccine, 22 which was an increase from a gap of less than 5% in national data abstracted from 1995. 32 Likewise, when comparing Blacks and Whites at least 60 years old, there was a disparity of about 5% in herpes zoster immunization rates in 2008, 21 however the disparity had grown to over 20% by 2014. 22
Few studies incorporated an intervention to reduce the disparities seen in immunization rates, especially with regards to hepatitis and TDAP related vaccines. However, there is emerging evidence of interventions that have helped to increase vaccination rates for herpes zoster. Many of these studies have been conducted in community pharmacy settings. One study assessed the impact of “personal selling” by community pharmacists for a herpes zoster vaccine wherein the pharmacist’s actively promoted the vaccine and sent personalized letters to patients and demonstrated that this intervention had a significant impact on the patient’s stated intention to receive the vaccine. 42 Another community pharmacy made use of automated telephone messaging to promote uptake of the and found this strategy significantly increased uptake of herpes zoster vaccines. 43 Another community pharmacy-oriented intervention utilized a personalized letter sent to patients, an informational flyer dispensed with the prescriptions, and a 1-time newspaper advertisement during an intervention month as strategies to increase herpes zoster vaccination rates. 44 The procedures adopted in these community pharmacy settings could conceivably be implemented with similar success in physician’s offices, especially those involved in primary care. However, one glaring limitation with these studies is the lack of data regarding the effectiveness of these interventions within ethnic minorities as this information was lacking.
This study has some limitations. Due to the cross-sectional nature of most of the studies, causal inferences are limited. In addition, although this study assumes that African Americans may be a homogenous group, it may in fact be true that they are a heterogenous group with a growing population of first or second generation immigrants. Moreover, although the Hispanics have been treated as a homogenous group in these studies, there are also likely differences in vaccine preferences within this group as well. In addition, there is limited data on the vaccination rates for the vaccines following the first vaccine in a series. In addition, this search was limited to articles conducted in the English language, so this may exclude potentially useful information written in other languages such as Spanish.
Despite the limitations, the data from this study suggest that disparities in immunizations among elderly adults are not decreasing over time. However there are some strategies that could be used to increase vaccination rates among elderly minorities by increasing awareness of vaccines and adopting active strategies to promote the vaccines. Primary care-based physicians are likely to play an integral role in reducing immunization disparities in elderly adults, yet implementation of culturally sensitive messages tailored toward minority populations is indispensable in ameliorating these disparities.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
