Abstract
Background:
There are many challenges that entail caring for an individual with dementia, affecting not only the individual with the condition but also their caregivers. This can lead to increased burden, frustration, and depression among those taking care of them. A research gap exists concerning the care of people with dementia in Egypt, particularly regarding the mental health of caregivers. Limited studies have been conducted in Egypt, particularly focusing on the mental health of caregivers. This lack highlights the need to understand the prevalence and impact of caregiver burden in this population.
Objectives:
The research aimed to evaluate the burden of dementia, levels of depression, and anxiety among family caregivers of individuals with dementia.
Methods:
A cross-sectional study was conducted at a geriatric unit clinic of a psychiatric hospital in Cairo University, Egypt. Caregiver burden, anxiety, and depression were assessed using questionnaires. These questionnaires included the Zarit Burden Interview (ZBI), Generalized Anxiety Disorder scale (GAD-7), and Patient Health Questionnaire-9 (PHQ-9), together with demographic data on the patients and caregivers.
Results:
The majority of the 141 participants (73% (n = 103)) were female, mostly daughters, with an average age of 40 years. Approximately 50% (n = 71) of the subjects exhibited mild to moderate burden, whereas 30% (n = 43) showed moderate to severe burden. About 31% (n = 44) of the subjects exhibited symptoms of moderate depression, whereas 9% (n = 13) had symptoms of severe depression. Furthermore, almost 43% (n = 60) of caregivers exhibited a moderate level of anxiety. Furthermore, a significant association was seen between caregiver burden and the presence of anxiety and depression.
Conclusion:
This study showed a substantial burden in providing care, elevated levels of despair, and anxiety among caregivers of PWD. The findings highlight how important it is to develop targeted therapies and support systems in order to lessen the load on caregivers, advance their mental health, and improve overall care for both caregivers and their patients in Egypt. Policy-makers should prioritize investing in dementia-related support systems and services to empower caregivers and improve the quality of life for both caregivers and their patients.
Introduction
An increasing public health issue that requires immediate attention is the growing number and problematic states of older adults affected by major Neurocognitive Disorders (NCD). Nevertheless, we should be braced to look after a growing number of older adults as long-term global life expectancy keeps on rising. Providing care for this population will require significant effort from care providers, who often face significant challenges and lack adequate support. 1 Typical caregiving responsibilities for individuals with dementia include providing personal care, managing medication, assisting with daily activities, and dealing with behavioral changes. 2
Dementia is the major NCD that has the highest challenge among non-communicable diseases, especially for both caregivers and health care professionals, exacerbated by resource constraints from aging populations. In 2019, dementia afflicted an estimated 57.4 million people worldwide. The rising likelihood of this disease is alarming as it has been continually revealed in the data through the years escalating, with projections of 83.2 million cases by 2030 and 152.8 million by 2050. 3
Dementia caregivers worldwide represent a diverse population, predominantly comprising family members, particularly spouses, children, and siblings, though friends, neighbors, and paid professionals also contribute significantly. 4 While the majority of caregivers are women reflecting traditional gender roles, their experiences are shaped by a variety of factors, including socioeconomic constraints, cultural norms, and access to resources. 5
Dementia is a progressive illness; this implies that as the patient’s condition gets worse, caregivers will have to do more and more of the duties. Dementia caregivers will also have to handle the rise of dementia-related symptoms exacerbated by longer lifespans. Caregivers will be under more stress and burden as the extended lifespan of dementia patients correspondingly lengthens the period of their cognitive and physical decline. 6
The term “caregiver’s burden” describes how much a caregiver’s responsibilities to take care of their relative adversely impact their social life, financial status, and mental or physical health. Compared to those who care for older adults without dementia, caregivers of those who had dementia reported significantly higher levels of burden. 7 Moreover, those who care for individuals with dementia are more prone to suffer with mental health issues like depression and anxiety. The psychological anguish of the caregivers might be caused in part by their continuous caring obligations, social isolation, and psychological toll from seeing their patients’ gradual decline. 8 Identifying caregivers particular requirements and creating suitable support plans depend on an awareness of the stress, anxiety, and hopelessness felt by them. 9
The increasing prevalence of dementia in Egypt presents significant challenges for caregivers. In Egypt, prevalence of dementia ranges from 1.4% to 21.95%, with projections indicating a substantial increase in the coming years. 10 However, the availability of resources and support systems for dementia caregivers in Egypt remains limited particularly in rural areas, which further exacerbates the challenges faced by caregivers. 11 The majority of caregivers being female, often daughters or wives, who shoulder the primary responsibility for caregiving due to cultural norms and family structures. 12
Many caregivers face significant challenges, including limited access to specialized dementia care services, the substantial financial burden associated with dementia care, lack of awareness and stigma surrounding the condition, cultural factors that often place the primary burden of caregiving on family members, particularly women, and limited training and support for caregivers. These challenges highlight the urgent need for research that sheds light on the experiences and needs of dementia caregivers in Egypt. 13
Despite the growing prevalence of dementia and the documented burden experienced by caregivers, research specifically investigating the experiences of dementia caregivers in Egypt remains limited. 14 This highlights the need for further research to identify the specific challenges faced by caregivers in this context and inform the development of culturally appropriate interventions and support programs.
The present study sought to evaluate the level of burden experienced by caregivers for people with dementia (PWD), the degrees of anxiety and depression they may have felt. In Egypt, caregivers’ health and the quality of care given to dementia patients may both be enhanced by this study, which can facilitate the creation of tailored programs and supporting services that suit their specific requirements.
We are hypothesizing that caregivers of PWD undergo a substantial burden of care, elevated levels of depression and anxiety. The study research question was “What are the levels of burden, depression, and anxiety encountered by family caregivers of PWD?”
Methods
A cross-sectional study was conducted at a geriatric unit clinic of a psychiatric hospital at Cairo University, Egypt. The cross-sectional design was chosen to provide a snapshot of the prevalence of caregiver burden, depression, and anxiety among dementia caregivers in Egypt at a specific point in time. This design is appropriate for assessing the prevalence of these factors at a single point in time, which aligns with our research objectives.
Settings, Sampling, and Participants
The research was conducted at a geriatric outpatient clinic of a psychiatric hospital in Cairo University. Data collection took place between May 2023 and March 2024. The study’s target population consisted of adult family caregivers providing home care. These caregivers were responsible for individuals diagnosed with mild to moderate dementia based on DSM-5 criteria. Researchers contacted family caregivers (19 years or older) who were providing care for individuals diagnosed with mild to moderate dementia as per DSM-5 and who had visited the geriatric unit clinic. Only caregivers meeting specific inclusion criteria were invited to participate. A total of (216) participants were invited to participate in the study, and (187) agreed to participate.
Inclusion Criteria
They were responsible for providing home care for individuals who had dementia.
They were 19 years of age or older.
Caregivers were excluded from the study if:
They were caring for individuals who had severe dementia according to DSM-5.
They were caring for individuals who had another severe psychiatric conditions.
Being paid for their caregiving role.
To ensure statistically significant results, the study’s minimum sample size was determined using assumptions derived from a previous study in this field by Liu et al, 15 using Epi-calc 2000 software. Assuming 80% power, a confidence level of 95% to test the following hypothesis, null hypothesis: there is no significant caregiver burden, anxiety and depression and alternative hypothesis: there is a strong significant level of caregiver burden, anxiety, and depression, the minimum sample size was 86 participants.
Before data collection, researchers thoroughly explained the study’s purpose, procedures, potential benefits, and participants’ right to withdraw. Written informed consent was obtained from all participants. Researchers were independent of the medical team treating the patients, and consent forms were securely stored, following standard data protection protocols. Data collection was done through the questionnaire that covers the demographic and personal data of the family caregivers (age, gender, relationship to patient, education, occupation, and medical condition) and their patients (age, gender, number of years since diagnosis, type of disease, occupation, and marital status), Zarit Burden Interview (ZBI) to assess caregiver burden, Patient Health Questionnaire-9 (PHQ-9) to assess caregiver depression, Generalized Anxiety Disorder scale (GAD-7) to assess caregiver anxiety
Measures
The Arabic version of Zarit Burden Interview (ZBI)
The ZBI is a widely used instrument that measures the extent to which the caregiver feels burdened by the responsibilities of providing care for their loved one with dementia. It addresses various aspects of the caregiver’s experience, including their emotional well-being, physical health, social life, and financial situation. The ZBI was originally developed by Zarit et al 16 and has since been widely translated and validated for use in various cultural contexts. The instrument’s comprehensive approach ensures a thorough assessment of the caregiver’s overall burden. Higher scores (0-88) indicate higher burden.17,18
The Arabic version of Patient Health Questionnaire-9 (PHQ-9)
It is a translated and validated self-administered questionnaire for assessing depression symptoms. It consists of 9 questions that measure the frequency and severity of depression symptoms experienced in the past 2 weeks. The PHQ-9 scores range from 0 to 27, with scores of 5 to 9 indicating mild depression, 10 to 14 indicating moderate depression, 15 to 19 indicating moderately severe depression, and 20 to 27 indicating severe depression. 19
The Arabic version of Generalized Anxiety Disorder scale (GAD-7)
It is a translated and validated self-administered instrument for assessing anxiety symptoms. It consists of 7 items that evaluate the frequency and severity of anxiety manifestations experienced within 2 weeks prior to the survey. The GAD-7 is scored from 0 to 3 points for each item, with a total score ranging from 0 to 21. A score of 10 or more may indicate clinically significant anxiety symptoms. 20
Data Collection
Data was collected through paper-based questionnaires in Arabic, administered at the geriatric unit clinic during scheduled appointments. Researchers were present during the administration of the questionnaires, providing instructions and ensuring participants understood the questions. All data were anonymized using a unique identification number assigned to each participant, removing any personally identifiable information. The research team was responsible for the secure of the data.
Data Analysis
The statistical software package, Statistical Package for Social Science (SPSS), version 21, was used to code, input, display, and analyze the collected data. Descriptive statistics (frequencies and percentages) were used to describe the characteristics of the caregivers and the individuals with dementia. Scores on the ZBI, PHQ-9, and GAD-7 were examined to assess levels of caregiver burden, depression, and anxiety among the caregivers. To examine relationships between caregiver burden (Zarit Burden Interview, ZBI) and levels of anxiety (Generalized Anxiety Disorder-7, GAD-7) and depression (Patient Health Questionnaire-9, PHQ-9), bivariate analyses were conducted using the chi-square test. The following coding schemes were used for the variables: ZBI: Categorized into 4 groups: 0 (no burden), 1 (mild-moderate burden), 2 (moderate-severe burden), and 3 (severe-extremely severe burden). GAD-7: Categorized as “Mild/Moderate” anxiety and “None.” PHQ-9: Categorized as ‘Minimal,” “Mild,” “Moderate,” and “Moderately Severe” depression. When the predicted number of cells was fewer than 5, the Fisher exact test was used. A P-value of .05 or less was considered statistically significant. All data were anonymized using a unique identification number assigned to each participant, removing any personally identifiable information. The research team was responsible for the secure of the data.
Results
A total of 216 adult family caregivers were invited to participate in the study, and 187 agreed to participate. Of the 187 caregivers initially invited to participate, 46 were excluded for the following reasons: severe dementia (n = 43), severe psychiatric conditions( n = 2), and paid caregivers (n = 1). The response rate for this study was 75% (141/187).
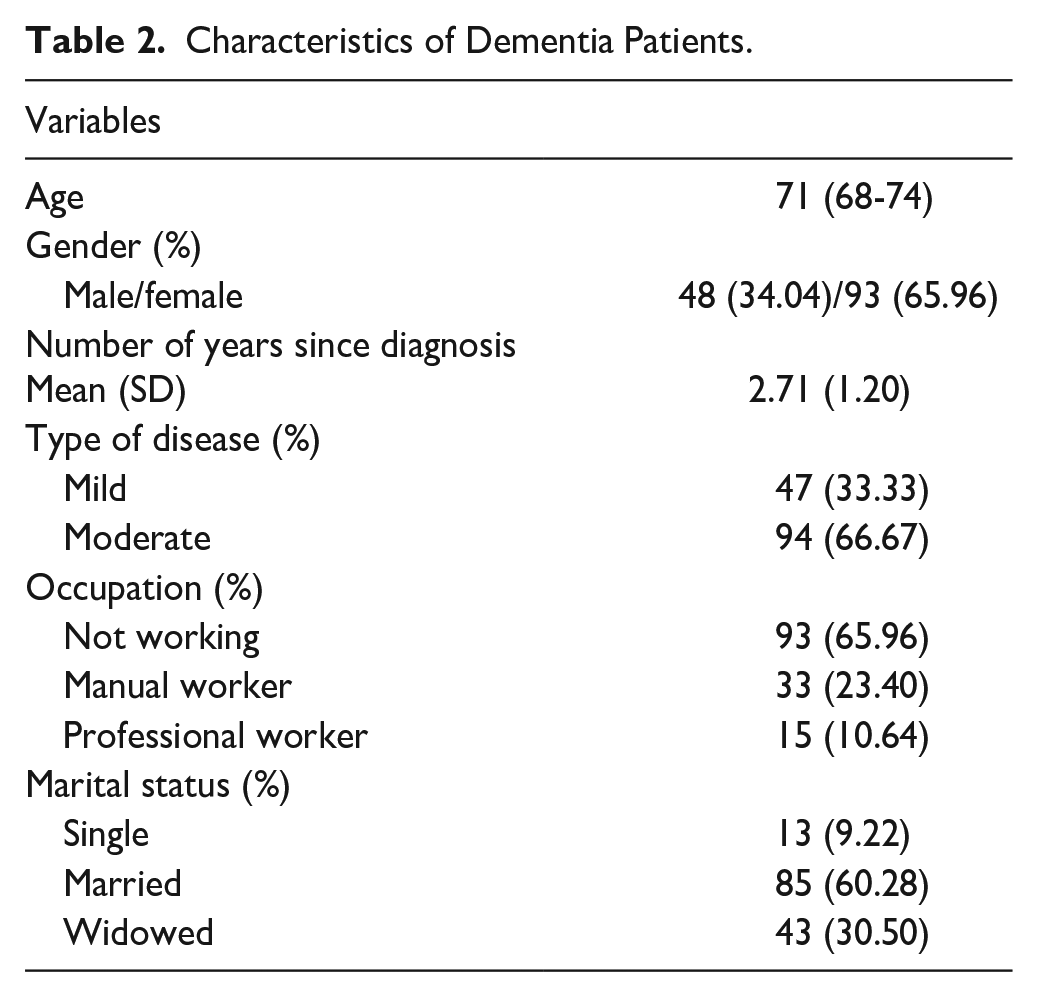
Caregivers’ ages ranged from 36 to 43 years, with a mean age of 40 years (SD = 2.6). The proportion of male caregivers was lower (27% (n = 38)) compared to the majority of female caregivers (73% (n = 103)). The most common relationship to the patient was daughters (58% (n = 82)), followed by sons (24% (n = 34)) and wives (11% (n = 15)). The educational background of the caregivers varied, with the majority having secondary education (50% (n = 70)) followed by basic education (33% (n = 46)). A smaller proportion had higher education degrees (14% (n = 20)), and a few were illiterate (4% (n = 5)) (Table 1). The median age of dementia patients was 71 years, (IQR = 68-74). Nearly two-thirds (66% (n = 94)) of the patients had moderate dementia (Table 2).
Demographic Statistics of the Caregivers for the Studied Population (n = 141).

Characteristics of Dementia Patients.
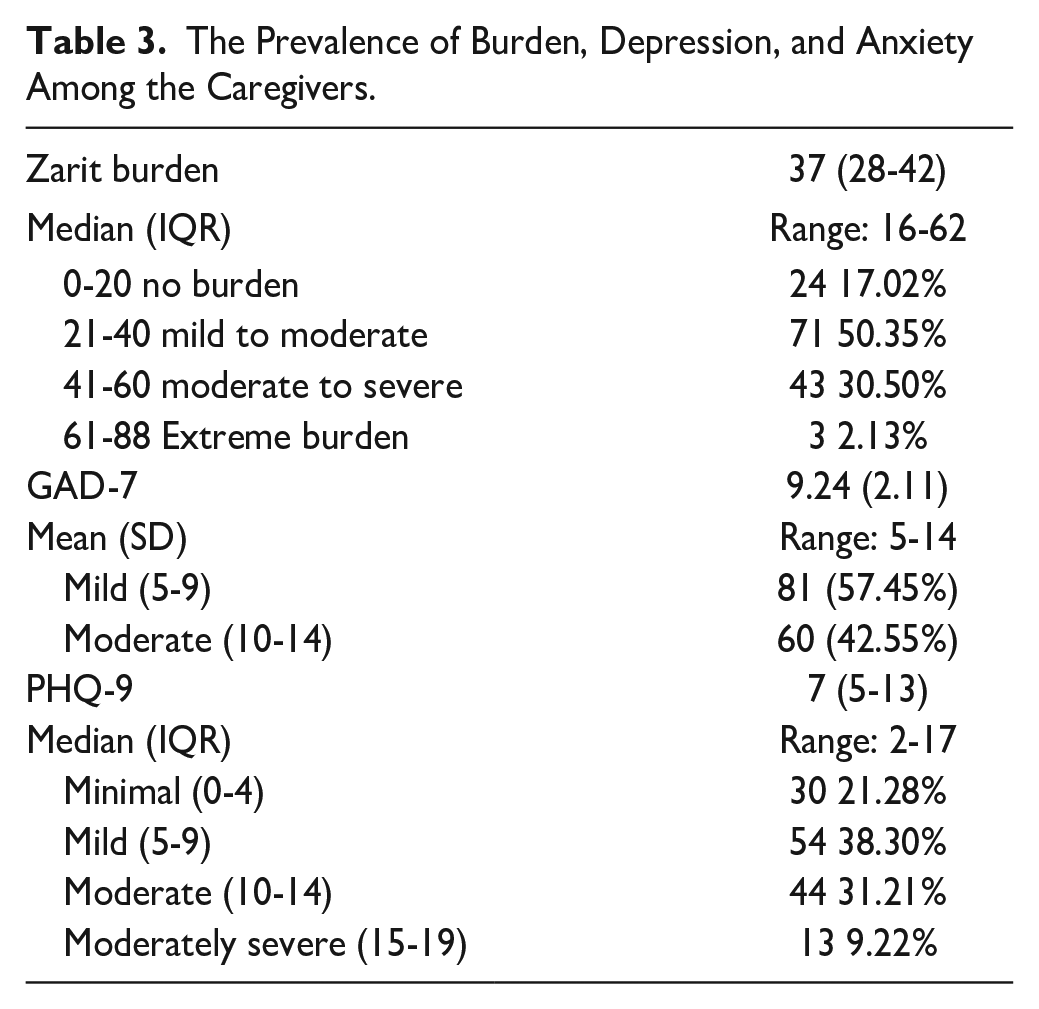
About half (50% (n = 71)) of caregivers of PWD had mild-moderate burden, while 30% (n = 43) had moderate to severe burden. The median Zarit Burden score was 37 (IQR = 28-42), ranging from 16 to 62. Among the caregivers, 43% (n = 60) had moderate anxiety. The mean GAD-7 score was 9.24 (SD = 2.11), ranging from 5 to 14. A significant proportion of caregivers reported experiencing depression. About 31% (n = 44) had moderate depression, while 9% (n = 13) had severe depression. The median PHQ-9 score was 7 (IQR = 5-13), ranging from 2 to 17 (Table 3).
The Prevalence of Burden, Depression, and Anxiety Among the Caregivers.
When studying the association between Zarit burden category and PHQ 9 and GAD 7 scores, there was a significant association between caregiver burden with depression and anxiety (Table 4).
The Association Between Zarit Burden Category and Other Scores.

Discussion
An aging population will drive a rise in dementia cases, resulting in greater involvement of family caregivers in providing care and support. 21 The diagnosis of dementia poses significant challenges for both the individual with the condition and their caregivers. The caregiving responsibilities might make caregivers more stressed, depressed, and anxious, compromising their overall well-being. 22
The study found that family caregivers of individuals with dementia in Egypt consistently reported burdened. Mild to moderate burden was found in approximately 50% (n = 71) of the samples and for 30% (n = 43), it was moderate to severe, with a median (IQR) ZBI score of 37 (28-42). This matched what Riffin et al 23 found in their study. Over half of the study’s family caregivers reported experiencing burden. The studies by Shata et al 24 and Salama and Abou El-Soud, 25 which also reported high levels of caregiver burden, further emphasize the universal challenges associated with this role.
However, while caregivers face common challenges globally, the specific challenges faced by caregivers in Egypt are influenced by cultural norms, resource availability, and access to specialized services. 26 Traditional family structures and cultural norms often place the primary responsibility for caregiving on family members, particularly women. This can create a significant burden, especially considering the lack of readily available professional support services. Additionally, there may be a stigma associated with dementia, which can hinder caregivers from seeking help and accessing support. 27
The high prevalence of caregiver burden, depression, and anxiety found in our study likely reflects these challenges faced by caregivers in Egypt. The limited access to resources, cultural norms that place a heavy burden on family caregivers, and a lack of awareness and support systems can negatively impact the quality of life for caregivers. This can potentially lead to increased stress, physical and mental health problems, and challenges in fulfilling their daily responsibilities.
The type and severity of dementia, 28 age, sex, presence of other responsibilities, along with neuropsychiatric symptoms of de/mentia, can affect the perceived burden experienced by a caregiver. 29 While we did not specifically evaluate health literacy in our study, we acknowledge its significance and potential impact on caregiver burden, depression, and anxiety. Future research should investigate the association between health literacy and caregiver outcomes, as well as explore interventions that can improve health literacy among caregivers to empower them to better manage the challenges of dementia care.
The prevalence of anxiety and depression among caregivers was also highlighted in our research. Based on our research, the mean GAD-7 score was 9.24, with a standard deviation of 2.11. Moreover, the respondents indicated mild anxiety in 43% (n = 60) cases. The study conducted by Wulff et al 30 revealed that about 36% of family caregivers had anxiety and supported our finding. Besides, Kaddour et al 31 in their meta-analysis showed that the prevalence of anxiety was 32%.
Our research found that whereas 31% (n = 44) of participants showed moderate depression, 9% (n = 13) of them had severe depression. These results matched with the research of Collins and Kishita, 32 where 31% of respondents had depression.
Our study showed that there was significant association between caregiver burden with depression and anxiety the same as McAuliffe et al, 33 who found that perceived burden was directly and significantly related to depression for both spouse caregivers and adult child caregivers. This highlights the importance of addressing caregiver burden as a key factor influencing mental health outcomes.
According to Sharma et al, 34 the results highlighted that among many countries of the globe, female elder caregivers formed the highest portion (73%). Comprising between 57% and 81% of the caregivers. This may be ascribed to the possibility that females would be more likely to use the health services and show follow-up visits. This is also mostly due to female participants’ reluctance to accept placing their relatives in need of care into an institution. 35 Furthermore, considering the cultural viewpoint, individuals have clearly grasped the accepted responsibilities of women. 36
Our findings emphasize the urgent need for comprehensive programs and policies in Egypt to support dementia caregivers. These should address key challenges, including providing access to affordable and accessible healthcare services, alleviating the financial burden, raising awareness about dementia and reducing stigma, offering support groups and community services, and providing targeted training programs for caregivers. The prevalence of female caregivers, often daughters or wives, underscores the importance of culturally sensitive interventions and the need to address cultural norms that disproportionately burden women in caregiving roles.
Limitations
- Self-report tools as the ZBI, PHQ-9, and GAD-7 are prone to memory bias or social desirability because they rely on the caregivers’ self-reported experiences and perceptions.
- The data was collected from caregivers at a single facility in Cairo, which may not fully represent the experiences of caregivers in other parts of Egypt.
Conclusion
The findings revealed patterns of burden, among caregivers along with elevated levels of anxiety and depression in families with a suffering, from dementia. This is why the study emphasizes the importance of specific interventions and support services to address the challenges faced by caregivers manage their well-being, which is often impacted and improve their overall health.
Recommendations
Further research should use longitudinal methodologies to analyze the evolution of caregiver burden, depression, and anxiety over time. Culturally tailored interventions are needed to address specific challenges, provide education and skills training, and promote caregiver well-being and resilience. Policymakers should prioritize investing in comprehensive dementia-related services and support systems to empower caregivers. This includes increasing access to affordable healthcare, providing financial assistance, developing education and awareness campaigns to reduce stigma, and investing in support groups and community services.
Future research could focus on:
- Exploring the effect of cultural factors on caregiver burden, depression, and anxiety in Egypt.
- Investigating the experiences of caregivers in diverse regions of Egypt, considering the impact of cultural differences, access to resources, and socioeconomic factors on caregiver well-being.
- Developing culturally appropriate interventions and support services that address the Egyptian caregivers needs.
- Assessing the impact of access to specialized dementia care services on caregiver outcomes.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The study underwent revision and received approval from the Family Medicine Department and the study and Ethical Committees of the Faculty of Medicine, Cairo University. The research was done after the participants comprehended the significance and objectives of the study. Only those who gave their permission were included.
Availability of Data and Materials
The data sets collected and/or analyzed during the current study are available from the corresponding author on request.
