Abstract
Purpose:
Few studies have examined the relationship between the intersections of lesbian, gay, and bisexual (LGB) sexual orientation, Latine ethnicity, and lifetime suicide attempts in Latine individuals with substance use disorder. This study examines this intersection and controls for social determinants of health, mental health disorder symptoms, and substance use disorder symptoms in a sample of Latine adults entering treatment for co-occurring disorders.
Method:
Bivariate statistics and multivariate logistic regression were used to analyze assessment data (n = 360) from a bilingual/bicultural integrated behavioral health system serving Latine communities in Massachusetts to examine the relationship between sexual orientation, Latine ethnicity, and history of lifetime suicide attempts. We controlled for social determinants of health, mental health disorders, and substance use disorder (SUD) factors significantly associated with lifetime suicide attempts at the bivariate level.
Results:
Over 27% of the sample and 35% of Puerto Ricans (PR) reported lifetime suicide attempts. The logistic regression identified that PR clients were 78% more likely to have attempted suicide in a lifetime compared to non-PR clients. Clients identifying as LGB were 3.2 times more likely to report having attempted suicide in their lifetime compared to heterosexual clients. Unemployed clients were 2.4 times more likely to report having attempted suicide in their lifetime compared to employed clients.
Conclusion:
Findings identify high rates of lifetime suicide attempts among LGBs and PRs entering SUD treatment. Targeted outreach and treatment efforts designed to address intersectionality for this underserved population are needed.
Keywords
Introduction
As the second leading cause of death among Latine individuals aged (15-34 years), 1 suicide is a significant public health concern. Historically, Latine individuals had lower suicide rates than White individuals 2 ; however, over the years, the suicide rate among Latines has drastically increased by over 26.7% from 2015 to 2020. 3 Among Latine individuals, negative immigration experiences, acculturation, discrimination, socioeconomic constraints, and family conflict are associated with suicidality.2,4,5 Furthermore, in Latine subgroups, suicidality differs, with Puerto Ricans (PR) having a higher prevalence of suicidality, along with depression and substance use disorder (SUD), compared to other Latine subgroups.6,7
Latine individuals who identify as lesbian, gay, and bisexual (LGB) are at the intersection of their sexual orientation and ethnic identity. Intersectionality, coined by Crenshaw (1989), refers to the multiple social identities of privilege and oppression an individual can experience.8,9 Intersectionality suggests that the intersections of race, gender, sexuality, class, and other identities are informed by unique historical, cultural, social, and political factors that can profoundly influence and shape an individual’s life experiences. 10 Moreover, LGB Latine individuals frequently encounter increased levels of mental distress due to cultural values, such as the importance of family loyalty 11 and the pervasive concept of machismo. 12 This traditional norm highlighted attributes and behaviors associated with masculinity, such as the dominance of power over women, bravery, and aggression, 13 which reinforces traditional gender roles. These cultural norms often result in the marginalization of Latine individuals identifying as LGB within their communities. The influence of religiosity shaping attitudes and perceptions toward sexuality and gender identity cannot be underestimated. The Latine community has been heavily influenced by Catholicism, which enforces heteronormative values through its teachings and social impact. 14 For example, the church teaches that marriage is a sacred bond between a man and a woman, with the primary purpose of bringing forth new life. 14 Therefore, the intersections of religion and cultural influences often compound the challenges LGB Latine individuals face as they navigate their identities in environments that do not fully accept or understand them.
Intersectionality theory is especially relevant to this study because LGB Latine individuals deal not only with their sexual orientation but also their ethnicity, cultural heritage, and cultural expectations. LGB Latine individuals have faced unique challenges associated with their sexual orientation and ethnicity, including discrimination, stigma, 15 family rejection, 16 and barriers to accessing LGB-affirming mental health services. 17 Additionally, with minoritized sexual identities, sometimes these individuals can be given outsider-within status 18 as they may experience homophobia and racism, both externally and within the LGB community.19,20 As a result, persistent exposure to these situations increases their risk for adverse mental health outcomes and lifetime suicide attempts.21,22 Additionally, previous research has found that LGB individuals are more likely to attempt suicide than their heterosexual counterparts. 23
Using an intersectional approach to understanding the multiple social identities of LGB Latine individuals, we can better gain insight into the complexities contributing to suicide attempts among this population. Therefore, this study examines the relationship between the intersections of LGB and Latine ethnicity and lifetime suicide attempts in Latine individuals with substance use disorder.
Method
The sample for this study consisted of (n = 360) adults with baseline data collected at intake to a substance use disorder treatment between 2020 and 2022 at Casa Esperanza Inc. Casa Esperanza is a bilingual/bicultural integrated behavioral health facility that focuses on serving Latine populations. Casa Esperanza was selected as the study site because of its inclusive approach to behavioral healthcare. This inclusivity is crucial in settings where LGB individuals encounter discrimination in more traditional healthcare settings. Casa’s reputation for being a secure and welcoming space for all patients presents a unique opportunity to examine these individuals within an environment where they are likely to feel supported and understood. Clients can enter treatment through referrals, community outreach, and word of mouth. A bilingual staff conducts an initial assessment interview, including a range of validated instruments such as the Patient Health Questionnaire 24 and questions from the U.S. Government Performance and Results Act (GPRA) and the National Outcomes Measures (NOMs) 25 required by the Substance Abuse Mental Health Services Administration, which funds many of Casa’s integrated services. The assessment is conducted in English or Spanish by reading it to the clients and documenting their responses. Detailed information about Casa Esperanza Inc., including services and community outreach, is available at https://www.casaesperanza.org/who-we-are/ and in other publications. 26 The University of Denver Institutional Review Board reviewed and approved the study as exempt.
Measures
Outcome variables
The outcome variable of interest was reported as having a history of lifetime suicide attempts. It was measured as a binary variable based on the following question: “Have you ever in your lifetime attempted suicide?” Responses to these questions were dichotomized as “yes” or “no.” It is important to note that the study ensured ethical compliance as the clients received comprehensive mental health care from a licensed mental health professional upon entering treatment. This approach ensured the clients had access to professional support to mitigate the risk of discussing a sensitive topic. Also, clients can access mental health professionals 24/7 while in treatment.
Primary exploratory variable
Sexual orientation was assessed by asking the clients, “Which one of the following do you consider yourself to be?” Data from clients who self-identified as lesbian, gay, or bisexual were coded as 0; self-identifying as heterosexual was coded as 1.
Control Variables
The following demographic factors and social drivers of health were examined as control variables. Age was measured in years, and gender was coded as a binary variable, male or female (no client identified as other than female or male). We could only define Latine ethnicity as Puerto Rican and others. This coding was due to sample size and the need to keep the data anonymous. Forty-nine percent of Latine clients clients were Puerto Rican. Also, in a preliminary analysis, only Puerto Rican ethnicity had a significant association with lifetime suicide attempts at the bivariate level. We also controlled for HIV-positive status, employment status (currently employed, yes or no), and whether or not they self-identified as homeless using binary variables with answer categories of “yes” or “no.” Based on existing suicide attempt literature,27,28 the following covariates were also examined. Clients were asked the following questions about their lifetime of substance use and mental health and trauma indicators: (a) “How many years in your lifetime have you used cocaine or crack?” (b) “How many years in your lifetime have you used heroin?” (c) “Have you ever experienced serious anxiety in your lifetime?” (d) “Have you ever experienced serious depression in your lifetime?” (e) “Have ever experienced hallucination in your lifetime?” (f) “Have you ever experienced trouble understanding, concentrating or remembering?” (g) “Have you ever experienced trouble controlling violent behavior?” (h) “Have you ever been prescribed psychiatric medications for psychological or emotional problems?” (i) “Were you ever treated for any psychological or emotional problem in a hospital or inpatient setting?” (j) “Were you ever treated for any psychological or emotional problem in a private or outpatient setting?” (k) “While you were growing up, during your first 18 years of life, did you live with anyone who was a problem drinker or alcoholic or who used street drugs?” Each response was coded as 0 = no and 1 = yes.
Data Analysis
Descriptive, bivariate, and multivariate analyses were conducted using SPSS Statistic Version 27 (IBM Corp, 2020). First, descriptive statistics were used to examine the general distribution of all the variables used in the analysis. Secondly, a bivariate analysis was conducted
using Pearson’s chi-square association test using Yate’s continuity correction and, where sample sizes were small, Fisher’s Exact test to examine the relationship between sexual orientation and a history of lifetime suicide attempts among Latine ethnicity while controlling for social drivers of health, substance use, and mental health factors. The variables significantly associated with a history of lifetime suicide attempts at the bivariate level were then entered into the multivariate logistic regression model (see Table 3). To assess the model fitness, we also performed a pseudo R2 square, the Wald chi-square test, and the log pseudolikelihood ratio test statistic. Odds ratios were reported with 95% confidence intervals (CIs) at an alpha level <.05. A listwise deletion was used to handle missing data.
Results
Sample Characteristics
The general distribution of the variables in this study is presented in Table 1. The mean age of the study sample was 42%, and 90% were identified as Latine. Over half were men 61%, and 5% identified as lesbian, gay, and bisexual. 27% of the total sample reported a suicide attempt during their lifetime. 21% of the sample had a mental health disorder diagnosis, 10% had been diagnosed with a substance use disorder, 69% had a dual diagnosis of both a mental health disorder and a substance use disorder. Finally, 39% were prescribed psychiatric medication and 82% were unemployed.
Sample Characteristics (n = 360).

Bivariate Association Between Lifetime Suicide Attempts and Sample Characteristics
Bivariate analyses were conducted using chi-square to examine the relationship between lifetime suicide attempts and the variables listed in Table 1. Only the following variables had a significant association with lifetime suicide attempts at P-value <.05: sexual orientation, Puerto Rican nationality, employment status, lifetime heroin use, and ever-prescribed psychiatric medications (see results in Table 2.) We then created a multiple logistic regression model that included only those variables significantly associated with lifetime suicide attempts at the bivariate level.
Bivariates Analysis.

Variables significantly associated with lifetime suicide attempt(s) at P < .05 using chi-square with Yates continuity correction or Fisher’s Exact Test as appropriate due to the small sample size.
Not included in the logistic regression model as it is an outcome variable.
Logistic Regression Results
Table 3 shows the multivariate logistic regression between LGB Latine and lifetime suicide attempts, controlling for other predictors. At the multivariate level, the results indicated that Puerto Rican clients were 1.7 times more likely to have attempted suicide (OR = 1.78, P < .05, 95% CI [1.02 – 3.10]) than non-Puerto Rican clients during their lifetime. Clients who reported being LGB were 3.2 times more likely to have attempted suicide (OR = 3.2, P < .05. 95%CI [1.16 – 9.42]) than heterosexual clients during their lifetime. Unemployed clients were 2.4 times more likely to attempt suicide (OR= 2.49, P < .05, 95% CI [1.09 – 5.69]) than employed clients during their lifetime. Additionally, clients who used heroin were 1.2 times more likely to attempt suicide (OR= 1.22, P < .001, 95% CI [0.69 – 2.14]) than clients who did not use heroin within their lifetime. Finally, the logistic regression model was statistically significant, χ2(4) = 19.048, P < .0005. The model explained 8.3% (Nagelkerke R2) of the variance in lifetime suicide attempts and correctly classified 72.0% of cases.
Logistic Regression Analysis—Lifetime Suicide Attempts.
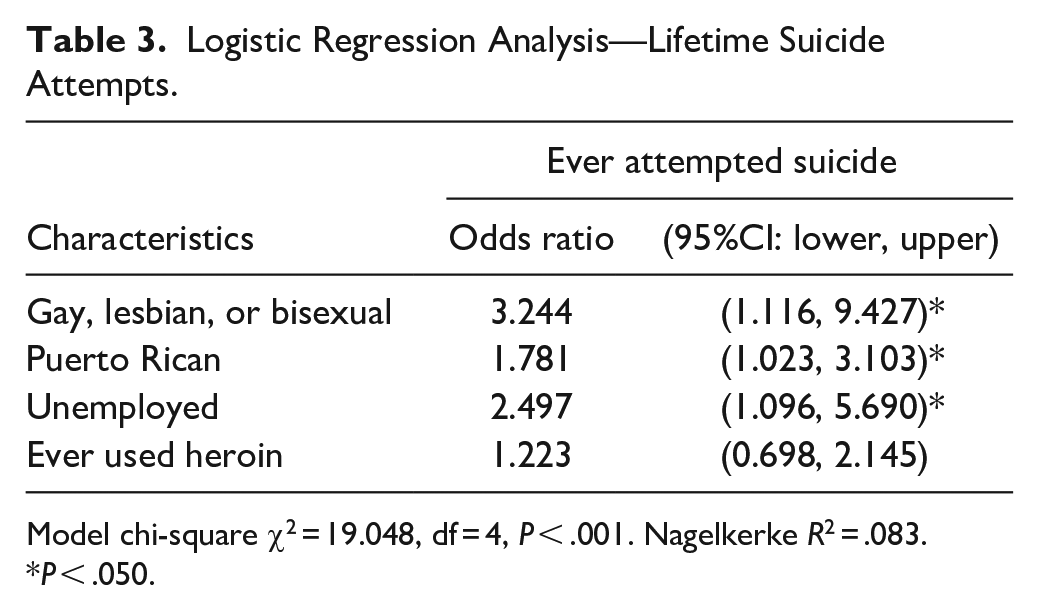
Model chi-square χ2 = 19.048, df = 4, P < .001. Nagelkerke R2 = .083.
P < .050.
Discussion
Our study’s novelty is apparent when we examine the intersection of risk factors. Specifically, we found that individuals who identified as Puerto Rican, LGB, had a history of heroin use, and were unemployed reported a significantly higher risk for lifetime suicide attempts among a sample of Latine ethnicity entering treatment for substance use disorder, mental health disorder, or co-occurring disorder. The findings of this study are deeply concerning, revealing that approximately one-fourth of the participants had attempted suicide at some time in their lives. In addition, the percentage is significantly greater among the Puerto Rican subgroup, with more than a third of individuals reporting a suicide attempt. A significant concern is the intersections of ethnicity, employment, and drug use with those who identify as LGB, increases their risk of suicide attempts. The stigma of having a substance use disorder or a mental health disorder, being unemployed, and also facing cultural stigma 29 can all contribute to a heightened risk of suicide attempts. This suggests that treatment organizations should tailor their suicide prevention to meet the intersectional needs of race/ethnicity and sexuality and how these intersecting factors can contribute to suicide among this population. For example, treatment organizations can improve the effectiveness of their suicide prevention efforts by adopting a culturally sensitive, strength-based counseling approach, especially for the Latine community.30,31 Recognizing and utilizing the inherent strengths and resilience within the Latine culture is crucial in suicide prevention efforts, especially considering the complex dynamics between cultural and gender norms, sexual orientation, and gender identity. Additionally, by doing so, treatment organizations can assist in reducing cultural mistrust, which often hinders individuals from seeking mental health services. This approach can promote a trusting and understanding environment, resulting in increased engagement and more positive outcomes in suicide prevention efforts.32,33 By adopting this approach, treatment organizations can create more impactful and culturally sensitive interventions that deeply connect with the Latine population.
Focusing on these intersectional identities and their relationship with the social drivers of health, such as employment, our study offers a deeper insight into the challenges faced by this group, revealing their high risk of suicide. Furthermore, our findings advance the body of knowledge of suicide attempt factors among Latine adults, emphasizing the urgent need to address structural inequalities, discrimination, and disparities in mental health care that disproportionately affect this community, as Latine are less likely to access medical care for their mental health needs. 2 Additionally, Latines are less likely to complete treatment for substance use disorders due to various factors such as socioeconomic, language, and cultural differences around reluctancy in seeking treatment options. 34
Close to a third of the total sample had attempted suicide in their lifetime, and 35% of those identifying as Puerto Rican reported having attempted suicide in their lifetime. These results are significantly higher than rates of suicide attempts by clients who were not Puerto Rican (21.3%) and compared to the national population of 6% 35 and other treatment samples, which found that among Latine, only 10% reported using mental health treatment options in the last year. 36 Additionally, our findings of higher rates of suicide attempts among Puerto Rican nationals compared to other Latine ethnicities are consistent with previous research. 7
Treatment organizations should conduct an initial assessment of suicidal history and provide evidence-based suicide prevention services as part of their integrated behavioral health and primary care services. These services also need to target LGB clients who were 3.2 times more likely to have attempted suicide compared to their counterparts. This study identified as prior studies37-40 have shown that social determinants of health, specifically unemployment, were significantly and strongly associated with having a history of suicide attempts. For example, Latines often reside in areas that can be perceived as unsafe. This heightened exposure to violence can potentially increase their risk for psychiatric disorders 41 and experiencing suicidal behaviors. Providing not only suicide prevention services but also employment, training, and placement is critically important to treatment populations since lack of work is a driving social factor associated with suicide attempts.
Interestingly, of the various lifetime mental health and substance use indicators examined, only being prescribed psychiatric medication and heroin use were significantly associated with suicide attempts among this treatment sample. Previous research has indicated that mental health 42 and substance use 43 are risk factors for Latine populations. It is important to note that this sample is entering treatment; therefore, the above findings suggest that individuals whose mental health symptoms were severe enough to require medications were more likely to have attempted suicide in their lifetime. It also suggests that clients had sought mental health services for their symptoms. Also, given the range of substance use in the sample, it is not surprising that heroin use was associated with suicide attempts. These findings are highly similar to other national and international studies. 44
Limitations
There were several limitations worth mentioning. First, this cross-sectional study was conducted with a convenience sample, limiting causal inference and clear generalizability. However, the sample entered bilingual/bicultural behavioral health treatment, providing valuable insight into this marginalized population. Second, while all the staff interviewers received identical training by the evaluation team to administer standardized questions, no information about inter-reliability was available. Third, the study focused on the LGB population in treatment at Casa Esperanza collectively rather than examining each subgroup individually. It is essential to note that the LGB community is not monolith, with each subgroup encountering unique challenges. Consequently, by combining these subgroups, the study does not accurately capture the nuances of each group’s unique experiences and challenges. For example, bisexual individuals encounter unique challenges, including discrimination and exclusion not just from the heterosexual community but also within the queer communities.45,46 Fourth, while race is an important variable, we did not examine race with this sample, given that many Latines do not identify with standard racial categories. 47 Also, we included clients who did not identify as Latine, as research demonstrates that most Latine respondents identify with their family’s country of origin rather than using terms such as Hispanic/Latine. 47 Fifth, it should be noted that Casa Esperanza collects data on a range of gender and sexual identities. However, when the data was collected, it included only clients who identified as LGB. Finally, the subsample sizes of Latine ethnicities beyond Puerto Ricans were relatively small, so we could not analyze Latines who were not Puerto Ricans compared to Puerto Ricans and non-Latines.
Conclusion
In conclusion, an effective course of treatment must take into account the whole person, including their sexual identity, cultural heritage, and exposure to trauma. This approach is essential in establishing an environment conducive to fostering recovery and resilience. When treatment programs adopt an intersectional perspective, they can address not only the substance use disorder but also the unique mental health needs of LGB Latine persons, reducing their risk for suicide attempts.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding was supported in part by Casa Esperanza, Inc., and U.S. SAMHSA grants CSAT TI080784, CSAT TI081614, CSAT TI080903, TI080655, CMHS SM80754, CSAT TI082188, and CMHS SM82420. There are several co-authors from Casa Esperanza, Inc. The federal funding sources were not involved in conceptualizing, analyzing, or writing the study.
