Abstract
The pediatric provider of record has a significant role in newborn screening and maintaining infant health after birth. Procedural errors and delays in communication can hinder the identification of infants with critical illnesses or follow up of unsatisfactory NBS samples. For this study, key stakeholders, including nurses, physicians, and midwives were interviewed to understand how the pediatric provider of record is selected by parents and examine factors affecting the newborn screening education and processes in the perinatal period. Provider responsibilities, timing of parent education, and social determinants of health played a role in parents’ choices of the pediatric provider. Investment in future intervention programs is needed for reducing the number of infants without a designated pediatric provider of record. Research is needed to understand social complexities and healthcare systems which affect parents’ choices of pediatric providers and newborn screening processes to optimize clinical outcomes for infants.
Choosing a pediatric healthcare provider for a newborn is an essential task for all parents. The pediatric provider of record (PoR) may be a physician or advanced practice provider who is responsible for follow-up of all infants after hospital discharge, including timely follow up of newborn screening (NBS). Newborn screening is a life-saving public health program aimed at improving infant health outcomes.1,2 All U.S. states and territories provide NBS for the early diagnosis and treatment of many inborn errors of metabolism and other conditions.3,4 Newborn screening programs require coordination between hospitals, laboratories, and public health systems.5,6 This process is facilitated by key stakeholders such as nursery nurses, newborn providers, and others who play vital roles in ensuring the collection of NBS samples and timely follow-up of NBS screening results.7,8 The PoR may be directly involved in returning newborn screening results to parents, coordinating follow up testing, and providing referral visits to specialized clinics for managing NBS conditions.
Fortunately, most NBS results are returned to parents within the normal range. However, impediments to the NBS process can cause delays in timeliness of reporting out-of-range results, initiating medical treatments, and retesting unsatisfactory results. 6 In a study by Desposito et al, 9 28% of PoR participants stated they did not receive notifications of NBS results for up to 10 days after birth. In addition, 31% PoRs reported no notification at all if the NBS results were negative. Inconsistencies in delivering NBS findings have caused NBS laboratory facilities in some cases to communicate directly to families to deliver results. While this method of notification ensures families receive the result, the responsibility for follow-up then rests on families, bypassing PoRs and interrupting the continuity of care. 10 Timely communications between families and the PoR can facilitate interactions with specialist healthcare teams for appropriate care.11,12 The timeliness of specimen collection and results reporting have become critical areas for quality improvement in NBS systems. 13
The PoR is responsible for preventative care and treatments for the neonate beginning with the first visit to the office. 14 Jaundice, feeding difficulties and other common newborn issues require prompt attention by the PoR. To facilitate the choice of a PoR before delivery, women are encouraged to visit potential pediatric practices. However, this was not often achieved. Fewer than half of first-time mothers availed themselves of pre-delivery visits, with rates of prenatal visits among poor urban women as low as 5%. 15
The American Academy of Pediatrics 16 recommends that healthy newborns be evaluated within 72 h of nursery discharge by their PoR. Failure of timely follow- up for newborns occurs frequently. Research suggests that some parents may misunderstand the need to establish a PoR for the infant post-discharge.9,17 In a retrospective chart review, Profit et al 18 found that delayed first visits with the PoR accounted for 440 (63%) of 698 total appointments seen by pediatricians at 6 days or more post-delivery. Issues interfering with timely follow-up included transportation problems, language barriers, limited parent education, lower income and ineffective communication between state agencies, hospitals, and PoR.19,20 O’Donnell et al 21 examined the medical records of a large cohort in the Bronx, New York, and found that 44% of newborns had their first outpatient visit beyond the recommended three-day window. Factors that facilitated visits with the pediatric provider included having an existing appointment, primipara status, breast-feeding, infants at risk for hyperbilirubinemia, and visits from a home health nurse. Alternatively, factors that contributed to later follow up times included having Medicaid insurance, c-section, greater gestational age, and discharge on a Thursday or Friday. 21 Shakib et al 20 found that infants in a Utah cohort seen within the correct prescribed number of discharge days, had significantly fewer rehospitalizations for infections, episodes to rule out sepsis, poor feeding, or jaundice.
To understand how parents choose a PoR, the perspectives of pediatricians, nurses, midwives, and others are often missing from the narrative. There is sparce literature that speaks to their experiences of timely referrals of infants to the PoR. Ensuring that all parents have a pediatric provider for their infant is an essential part of newborn physicians’ and nurses’ work, but this does not always go smoothly. Women may choose a provisional PoR while in the nursery then later change their minds. An incorrect PoR recorded in the medical record or on the newborn screening blood spot card can delay communication of NBS results or follow up of other health issues. There is limited understanding of these processes which are central to the transition of an infant to the community. The aim of this study was to examine women’s choice of a PoR from the perspectives of key stakeholders and explore issues in parents’ education about NBS and well-baby health.
Methods: Setting, Sample, Ethics, and Study Design
Nurse researchers from a large land grant university in the southern United States met with medical, nursing, and administrative staff at a major health center serving metropolitan and rural areas. The overall racial and ethnic demographics for this region are white (70%), black (16%), hispanic (7%), two or more races (5%), asian (2%), and other (1%). 22 The aim was to discuss newborn screening practices to determine if there was a need for quality improvement projects at their institution. An important concern for medical center staff was understanding how women chose the PoR for their newborns. Hospital personnel explained that women often did not have a named PoR at admission or through their nursery stay. If women did not choose a PoR, a proxy would be assigned to the infants. In some cases, women had a designated PoR, but switched to a different one post discharge. Subsequently, staff fielded results from the state laboratories for abnormal NBS and tried to locate families and/or identify the definitive PoR. This greatly increased hospitalist and hospital personnel’s workload. The nurse researchers and medical center personnel proposed an action research project to explore stakeholders’ perspectives of parents’ selection of a PoR, newborn screening and parent education. The study was funded through a cooperative seed grant from both agencies.
In the tradition of action research, the aim of a study is to improve a process or system and benefit those directly involved in it. 23 Action research is a means of giving voice to people who may not have a say in a process, even though they have a stake in a process. 24 An important facet of action research is that those involved in the study co-create the research aims, research questions, and agenda. This method places researchers and research participants on equal footing through collaborative partnerships. 25 Ultimately, participants use the research findings to foster change in a system. 24
Institutional Review Board (IRB) approval was obtained. The researchers and hospital medical and nursing staff met multiple times to discuss the study objectives, design, interview questions and scope of the project. All participants recruited for the study engaged in some aspect of the pre-post-delivery care of newborns, nursery care, and the NBS process. The research team used snowball sampling to identify potential study participants. Researchers obtained informed consent from each participant prior to beginning each interview. Study participants received a $25 incentive card for taking part in the interviews. Individual open ended, semi-structured interviews were conducted by phone or in person to assess stakeholders understanding of the parents’ choice of physician of record and the NBS process. All interview data was de-identified, and no information about participant gender, race, or ethnicity was documented to protect participants’ privacy. Audio recordings were not obtained to maintain confidentiality due to the sensitive nature of the interviews. Researchers took notes, summarizing interview content, clarified statements with study participants, and immediately converted the notes to typed text. Three study team members reviewed results individually and then came together for group interpretations of the findings. Data was grouped into substantive categories. Key themes from the interviews emerged from the data.
Results
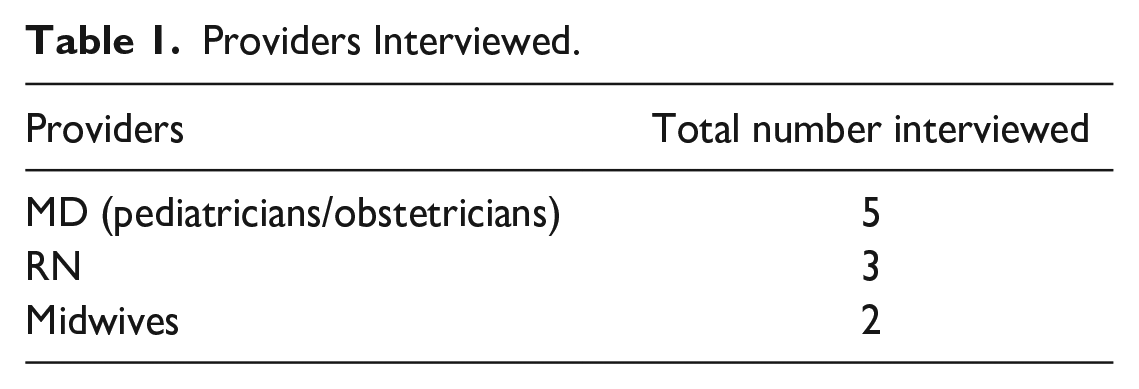
A total of ten healthcare providers were recruited for the study (Table 1). Interview time with participants ranged from 30 to 75 min. From the interviews, themes emerged which centered on provider responsibilities, timing of NBS education, health priorities, and determinants of health reflected in providers’ perspectives of women’s choices of a PoR. The study participants also offered suggestions for improving the selection of the PoR and education for mothers on NBS and well-baby care. Study participants also shared their thoughts and discussed the impact of the Covid pandemic on service delivery and PoR choice.
Providers Interviewed.
Responsibility for Ensuring a Provider of Record for Every Infant
Ideally, healthcare providers and parents shared responsibility for the identification of a pediatric provider of record for infants. However, study participants reported that newborn providers assumed the major responsibility for ensuring a PoR for infants. Nurses and hospitalist staff frequently encountered mothers who had not yet chosen a PoR. Those without a designated PoR received a list of local pediatric and family practices so they could choose a provider. One nursery nurse participant estimated that 30% of mothers in her care did not have a designated PoR after delivery and roughly, 20% of mothers did not know and were surprised by the request to select a PoR. Staff continued to encouraged mothers to choose a PoR and asked them at every encounter. One provider felt that talking about the PoR with mothers took valuable time away from parent education for well-baby health and NBS screening. Obstetrician and community pediatric providers were less aware of the issue of the lack of designated PoRs for newborns. Midwives in the study typically discussed choice of PoR and NBS in the third trimester. The importance of acquiring a PoR was stressed, but it was common for mothers to not have a PoR by delivery. One study participant suggested that despite the emphasis on choosing a PoR, the main focus during the pregnancy was on the mother and less on the baby after delivery.
In the nursery, a PoR name was needed to complete the state’s NBS blood spot form. Study participants said that if a PoR was not chosen by the time of NBS sampling, staff selected a provisional PoR name, typically a provider associated with a large public pediatric practice. In some cases, if mothers had not decided, they would pick a provider located closest to them. Consequently, the PoR name on the blood spot card and record might not be the PoR parents followed up with. Furthermore, some parents changed their PoR after they returned to the community. One study participant opined that parents were less likely to follow up with a PoR if they did not select a PoR by the time of the NBS screen sample was taken.
Newborn screening results are typically returned to the PoR within 5 to 7 days or be sooner for critically abnormal values. Officially, the PoR was charged by the state for all NBS follow-up, however, the newborn and nursery providers frequently felt responsible for this task. All NBS results were pooled and returned to the hospital, which served as a double check to ensure that no NBS slipped through without a PoR. The state did not mandate this safeguard, but providers worried that a baby could fall through the cracks. The providers also reasoned they were libel if they ordered screening tests but did not follow up. When abnormal NBS results were returned, hospital personnel attempted to locate the PoR or identify where parents were taking the baby for care. If the hospitalist followed up with a misidentified PoR, there could be delays in communicating results and time lost for establishing the diagnosis and treatment. The state laboratory no longer called actionable NBS results to the metabolic specialists, so they did not automatically receive notifications of a critical result. When parents did not go to PoR appointments, this too led to delays in addressing NBS and other health concerns such as bilirubin levels, weight loss or feeding issues.
The majority of study participants across disciplines maintained that the PoR was critically important to ensuring that babies received the best possible care upon discharge from the hospital. Provider participants felt responsible for documenting the correct PoR and following up abnormal NBS results with the PoR. Responsibility for NBS and infant well-health education was shared among the different healthcare disciplines. The concerns were considered vital for ensuring appropriate follow-up for infant health.
Timing of Education About PoR Choice and NBS
The timing of choices for the PoR and perinatal education delivery were considered key for fostering continuous quality care of mother and baby. Study participants agreed that parent education should be initiated during the pregnancy, and this also helped women in their decision-making for a PoR. The vast majority of study participants favored obstetric service providers for assisting women with PoR selection and offering NBS education by the third trimester, when families were less stressed so they could prepare for delivery and aftercare. As noted earlier, midwives routinely provided NBS information and assessed women’s decisions for PoR choice. One obstetrics provider shared that they did not routinely ask patients about NBS or the PoR arrangements.
Health Priorities
Identifying the correct PoR is an essential element in NBS follow up if emergent care is needed. Study participants described a variety of reasons offered by women who did not decide on the PoR prior to delivery and their nursery stay. Per study participants, a portion of first-time mothers did not prioritize choosing a PoR. Often, these women had not yet asked family or friends for a recommendation of a pediatric provider. Women who delivered early were caught short because they thought they had more time to decide. For women delivering their third and fourth baby, PoR choice was not considered to be of importance, but a matter of routine. Other mothers, unhappy with their current provider, wished to switch to a new practice but had not yet decided. Study participants described some parents as being indecisive in choosing a provider while others appeared indifferent or did not grasp the importance of follow-up for the newborn. Additional reasons providers identified which affected mothers’ choice of a newborn provider included mothers who had recently moved from a different part of town, were new to their area, or were undecided between multiple providers. In some cases, mothers who received Medicaid services assumed they would be assigned a PoR and did not know they needed to pick a newborn provider instead. Although some mothers were unprepared to choose a PoR, others were anxious about making the right decision. As one participant noted, choosing a PoR meant mothers were making a commitment to a relationship with a provider for the care of their baby, and this was an important decision.
Several participants noted that for some parents a distrust of mainstream medicine drove their lack of decision-making for choice of a PoR. They recounted a minority of parents who resisted choosing a PoR because they expressed vaccine hesitancy. Participants noted that more parents with these views were seen in the nursery in recent years, and fewer providers were willing to accept families who are vaccine hesitant. Although study participants educated parents about the benefits of vaccinations, some still did not want to go the “wellness route.” Study participants wanted to respect parents’ autonomy and did not want to engage in fear mongering. Nevertheless, study participants asserted the importance of choosing a provider who followed recommended guidelines, including vaccinations. Participants noted that families could decline state NBS screening if they chose through filing form for religious objection and more parents were declining NBS screening lately. According to participants, some parents were worried about having their babies’ DNA stored and on record.
Social Determinants of Health and Community Context
Social determinants of health, such as language, insurance status, distance to travel to providers, and age were identified by the stakeholder participants as key factors that affected choice of a pediatric provider and factored into parent education. Education on well-baby health and NBS, delivered in a meaningful way, was important for study participants. Parents served by study participants came from diverse nationalities and ethnic backgrounds. Participants felt that educational materials should be provided in the parents’ primary language and that interpretation services should be available for discussions with families. Language and cultural barriers, and low health literacy, made it difficult, from the provider participant perspective, for parents to navigate the healthcare system and also impeded their decisions making. There were no appreciable racial differences between women who had or had not yet picked out a PoR for their infants per study participants. There was a difference, however, between those with commercial or private insurance and government-funded insurance programs. Mothers with commercial insurance more often had a designated PoR upon admission to the nursery. These women were often cared for in private or select obstetric and midwifery practices. Younger mothers more often lacked prenatal care. They were less likely to be educated about NBS, well-baby care and other health-related topics and also had less understanding of the need for choosing a PoR.
For non-English speaking women, the use of an interpreter, plus telephone and virtual interpreter phone calls were helpful in bridging the communication gap. Spanish speaking women who had their first birth needed more help in some instances and may not have chosen a PoR prior to delivery. In some cases, they did not have a substantial family or friend support or resources. Interestingly, teenagers from diverse groups often had support of grandmothers and great-grandmothers at delivery. More women of European background were delivering locally. Few families with immigrant backgrounds chose a PoR prior to admission to the nursery, especially those new to the area or who had language issues. This was attributed to language or literacy barriers or lack of internet access. However, these families expressed interest and wished to establish care with a primary provider, they just did not know how to go about it.
Transportation barriers were also a significant obstacle to accessing a PoR for those individuals with limited access to private or public transportation and those who lived in rural areas. When a staff member assigned a PoR to an infant, every attempt was made to choose a provider near their home.
Healthcare access
There were additional factors described by study participants that contributed to concerns about healthcare accessibility. There was a prevailing fear, for some mothers, and another reason for not choosing a PoR, that providers would not accept their insurance. Charges for pediatric care were an important concern. Mothers worried about out of pocket costs. In this region, NBS is not free. One participant lamented they were seeing more families with self-pay for NBS, “It comes down to money. If you have insurance or Medicaid, you are covered.”
Questions concerning Medicaid coverage were most often asked by younger women of color, with and without Hispanic backgrounds. It was notable that Medicaid patients followed by private obstetric practices were often better prepared educationally and familiar with obtaining a PoR for their baby. Several study participants provided care primarily to women who had Medicaid coverage and did not see privately insured patients. Study participants noted that having a community-based child health center that accepts newborn referrals and provides social work follow-up is vital.
Impact of Covid
Covid-19 significantly shaped the healthcare system in terms of childbirth and pediatric care. Women and infants had shorter hospital stays, and NBS samples were obtained around 24 h of life for promoting earlier discharge from the nursery. Changing the timing of NBS and hospital discharge impacted the identification pediatric providers because women were more rushed to decide about PoR. Covid limited the number of visiting persons that could be with the laboring mother, which limited their support. Not having visitors was particularly hard on the young mothers who did not have their boyfriends or mothers present. Language interpreters, formally in-person, moved to phone-only systems. Increased home births and free births attended by family members only were noted and with concern by study participants. Fear of COVID-19 also kept families from seeking medical care when needed. Sick children in greater numbers were evaluated, but medical practices often did not perform virtual sick visits for children under age 2. Covid did not change the difficulty of identifying the PoR, but it did push the technology more into mainstream use with direct scheduling of appointments, which may have helped with infant follow up in some instances.
Discussion
The action research model engages stakeholders in the best position to identify problems and who will directly benefit from research findings. In this study, provider-participants discussed their concerns, engaged in study planning, and identified potential solutions for improving education and recruitment of PoRs. A number of themes emerged in this research that serve as useful starting points for improving perinatal care delivered in overlapping systems. The PoR connects with infants for routine follow up, health related issues, and in crisis in the event of abnormal NBS results. When a proxy PoR is in place, valuable time may be lost trying to locate the correct PoR. Newborn providers in the hospital shouldered the major responsibility of following abnormal NBS results and tracking the PoR in cases of misinformation which immensely increases their workload. Study participants shared different reasons why they believed women may not choose a PoR by the time of delivery or NBS sampling. A number of these concerns aligned with the Social Determinants of Health specified by Healthy People 2030. 26 These included economic stability, community, and healthcare access, but other factors such as pediatric vaccination policies, were unique to this study.
The study participants strongly recommended that education about well-baby health, NBS, and choice of PoR be instituted well in advance of delivery. While this may appear an optimal time for patient education, this may not always be the case. Education in the third trimester may be too late if a woman delivers early. Although midwives worked diligently with parents to identify a PoR, a PoR was still missing for some infants. Other factors may be driving the lack of uptake in this area and have profound effects. Bernstein et al 27 suggested that women who were not asked to schedule their first office visit while in the hospital were more likely to see themselves as unready for discharge.
Previous research has been conducted illustrating the successful implementation of programs for the PoR follow up of newborns. Goyal et al 28 directed 2 care coordination programs to improve timeliness of primary care newborn visits. In 1 study, 2 nurse discharge coordinators provided centralized support for arranging appointments with primary care or subspecialist services, created care plans for pursuing lab results and communicated with hospitalists for emergent issues. For the second implemented program, direct communication channels were opened to place “welcome” phone calls to parents to reinforce primary care visit times and track no shows for rescheduling. Investing in follow up systems promoted adherence to AAP guidelines and improved post-hospital visits for newborns for these studies. Scott et al 29 in another quality improvement program applied a physician learning project which included the use of a multidisciplinary team. This concluded with sustained advances in timely follow up of newborns.
Suggested Solutions by Study Participants
Study participants suggested solutions from their perspectives for identifying the PoR and timing of education about well-baby care and NBS:
Plan far ahead for naming a designated pediatric provider before delivery. Start conversations about PoR and NBS early, during OB/midwifery visits and promote the importance of choosing a pediatric provider during prenatal care. Provide education materials to OB services (which was already performed in some cases). Continue with RN and pediatrician discussions during the hospital stay. Hearing the same information multiple times can help with learning and ensure a smooth transition to the PoR.
Help families narrow down potential pediatric provider picks and assist with making post discharge PoR appointments for follow up.
Pediatric services are not adequately promoted. There are community maternity fairs and kid’s consignment, and all manner of promotional activities for these groups. Unique naming of pediatric practices and endorsing the special services they offer to families should be encouraged and broadcasted. This may make it easier for families to choose a pediatric provider that is a good fit for them and improve marketing. Pediatric practices can show how special they are!
Consider instituting preregistration services for infant deliveries. Mothers preregister with the hospital; then, only recent updates are needed for the medical record when they arrive for delivery. This would be another opportunity to ask parents about their choices for PoR.
Improve communication and coordination between state laboratories, metabolic specialty services, hospitals, and pediatric offices to enhance the care of infants with critical and out of range NBS results.
If a proxy PoR is assigned to an infant, establish a fallback service desk or registry that can contact the families to sort out appointments and referrals.
Focus on outreach and education efforts targeted for disadvantaged populations involving community organizations and clinics to provide information about primary care options, newborn education, NBS, and resources such as transportation assistance or language interpretation services.
A plan of action for postpartum care should be established during prenatal care, with discussions about the journey home well underway before admission to the nursery.
Limitations
The issues and themes described here may resonate with readers who have encountered these in their practices. These study results reflect the views and concerns solely of participating study providers. The study sample is small. Results may not represent the experiences of other providers, services, or hospital systems.
Unconscious bias is another potential limitation to the study. There are chances that the perceptions of some of the participants could reflect preconceived notions about mothers of different ethnicities and different socioeconomic statuses.
Conclusions and Suggested Future Research
The AAP 16 provides guidance on naming a newborn pediatric provider which is vital to ensuring continuity of care. A designated PoR should be in place by the time of hospital discharge as breakdowns in the communication of NBS results hinder the effectiveness of NBS programs. However, research has shown that even when the PoR is established, there may be uncertainty about their provider roles and effectively communicating NBS results.9,10,30 Earlier research suggested that pediatricians were unprepared to manage infants with positive newborn screen results, 31 while recent research suggests that pediatric residents felt better equipped to counsel families, follow and treat infants with NBS conditions. 32 These issues are an added layer of concern and research into providing effective NBS communications. Protocols clarifying PoR roles and access to educational resources may lead to better counseling, follow up, and decrease potential adverse clinical outcomes. 7
Investment in future intervention programs is needed for reducing the number of infants without a designated PoR. Further research which examines the barriers to identifying a POR is essential to implement intervention programs for the reduction of the numbers of infants discharged without a POR. 17 This future research could consist of studying specific groups and identifying unique barriers they face. Future research could also include investigating the key interventions and educational times that are best for women during their prenatal care to maximize their understanding of NBS and the chances of having a POR identified during the hospital admission assessment.
Footnotes
Acknowledgements
Thank you to our participants who so generously gave of their time, thoughts, and ideas for this research.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by Prisma Health HSC Seed Grant Award Number 2014669.
IRB Approval
Clemson IRB Human Subjects approval IRB2021-0287.
