Abstract
Perinatal communication is one factor driving racial disparities in maternal and infant morbidity. The murder of George Floyd in May 2020, in addition to the disproportionate impacts of the Covid-19 pandemic on communities of color, was a catalyst for American society to address racial injustices with a renewed sense of urgency. Drawing upon sociotechnical systems (STS) theory, this rapid review describes changes in the literature regarding the organizational, social, technical, and external subsystems that affect communication between perinatal providers and their Black patients. The goal of this work is to support health system optimization of health communication initiatives and, as a result, improve patient experience and parent and child outcomes. As part of a multi-year project designed to improve health communications about safe fish consumption during pregnancy, and in response to racial disparities among our health system’s patient population related to receipt of nutrition messages during prenatal visits, we conducted a rapid review of literature on Black parents’ experience of all communication while receiving perinatal care. A search of PubMed identified relevant articles published in English since 2000. Articles were screened to include articles that focused on Black people receiving perinatal care. Article content was then coded using deductive content analysis guided by STS theory to inform healthcare system improvement efforts. Differences in the prevalence of codes pre- and post-2020 are compared using chi-square statistics. The search in PubMed yielded 2419 articles. After screening, 172 articles were included in the rapid review. There was an increased recognition of communication as a key component of quality perinatal care after 2020 (
Keywords
Introduction
In the United States, Black women are 3 times more likely to die as a result of childbirth than white women, and Black infants are twice as likely to be born premature than white infants.1,2 Evidence suggests social determinants of health, health behaviors during pregnancy, and access to quality health care all contribute to these disparities.
3
The quality of Black women’s health care experience is negatively impacted by provider unconscious bias and systemic racism and/or discrimination.4,5 Many studies have found that Black patients feel disrespected and misunderstood by their health care provider due to these biases.6,7 This discrimination can manifest in lower quality rapport and communication between perinatal clinicians and their Black patients. Therefore, patient-provider communication about health care and health behaviors during the perinatal period, including throughout prenatal visits, labor and delivery, and postpartum care, has been uniquely described as both a
Many health systems have launched communication initiatives to address racial disparities in care quality, and more specifically the disparities in perinatal patient-clinician communication, to improve care and support health behaviors during pregnancy. 11 The disproportionate impact of the Covid-19 pandemic on communities of color and the murder of George Floyd in the spring of 2020, and the resulting recognition that the United States must acknowledge and address the harm done to Black Americans across society, including healthcare, brought this issue to the forefront.
As part of an ongoing partnership to disseminate safe dietary fish intake information during prenatal visits, our team compared provider- and patient-reported communication of messaging. Our analysis showed no difference in provider-reported delivery of fish messages by patient race, but respondents identifying as Black were 25% less likely to report receiving the message compared to respondents who identified as white. 12 In light of this disparity, our team set out to understand the literature to better support Black patients receiving perinatal health messages in our health system, and more specifically, how changes in the literature after 2020 could support vital transformation in service of racial equity.
To date, little is known about how providers share information about critically important care delivery or health behaviors topics differently based on patient identity and risk factors.13,14 It appears these differences in communication can contribute to poorer quality of care, patient understanding and adherence, and mental, emotional, and physical health for Black parents and babies. Socio-technical systems theory (STS) provides a useful framework to examine the drivers of differences in communication. STS considers human factors and organizational issues when a system, such as a healthcare system, needs to make improvements and is especially relevant to communication initiatives. 15 In contrast to traditional “top-down” approaches to quality improvement, STS is a “bottom-up” approach that focuses on those most directly impacted by a practice or policy (in this case, pregnant people and their care providers) and considers their social and technical needs. 16 STS defines subsystems and aims for “joint optimization” in which all subsystems align in order to improve experience and outcomes. 17
Given the timely nature of this topic and the sense of urgency to address injustices experienced by Black Americans, nationally and within our health system, we used a rapid review approach as outlined by Khangura et al. 18 As Langlois et al 19 describes, “[r]apid reviews have emerged as an efficient solution to support health policy-making and health systems strengthening by providing high-quality evidence in a timely and cost-effective manner.” While there are tradeoffs with using this approach rather than a more rigorous systematic review, we determined the rapid review provided the information we needed on an expedited timeline. Drawing upon sociotechnical systems theory, this rapid review describes:
the STS subsystems that affect quality communication between perinatal providers and their Black patients and
how the literature related to these subsystems may have changed after the racial reckoning of 2020.
Our findings can support health systems in efforts to align the STS subsystems for optimization of patient experience and parent and child outcomes, as well as address current disparities, especially those experienced by Black families.
Methods
Design
In order to synthesize evidence published since 2000 and evaluate changes in the content of the literature post-2020, we performed a rapid review. Following the rapid review method, we identified our research question prior to conducting the comprehensive literature search to identify articles at the intersection of the literature regarding racial disparities, patient-provider communication, and perinatal care (see Figure 1 below). 18 Then, we used a single reviewer to identify articles that were relevant to our topic, using the a priori inclusion and exclusion criteria below. We also performed an abbreviated deductive content analysis using developed STS codes for each subsystem. We performed a general linear regression to calculate the trend in number of publications from 2000 to 2020 and predicted values within 95% confidence intervals for articles published in 2021 and 2022. Then, we used chi-square statistics to measure any significant differences in the prevalence of STS codes in 2020 and earlier, as compared to 2021 and 2022.

Approach to comprehensive literature search.
Search Strategy
First, we conducted a comprehensive search of PubMed to identify literature on racial disparities in communication during perinatal care. The medical subject headings (MeSH) defined the concepts of racial groups, disparities, or inequities; communication, experiences, perceptions, or professional-patient relations; and obstetric or maternal health services during the perinatal period. For optimal retrieval, MeSH terms were supplemented with relevant title, abstract, and text words. We applied the English language filter and date parameters of January 2000 to June 2022 to the final search statement. Dissertations, books, books chapters, and conference proceedings were excluded. Full search parameters are available on request. This PubMed search yielded 2419 articles.
Screening Process and Eligibility Criteria
All titles and abstracts were reviewed by a single reviewer for eligibility based on a protocol created a priori. Articles were included if they focused on Black or African American people receiving perinatal care within the United States, or exploring racial differences between groups, including Black or African American parents. Perinatal care could include prenatal care, labor/delivery, postpartum, or postnatal care, but did not include pre-conception nor contraceptive care. Articles also needed to relate to communication, including technical communication, patient-provider relationship, patient-centered care, and/or perinatal care experience; articles specific to family or partner communication or relationships were excluded. All articles were published in the United States, in English, and in 2000 or later. When additional information was needed to determine eligibility, the full-text article was retrieved and reviewed. All article information was downloaded from PubMed, compiled into Microsoft Excel, and reviewed using inclusion criteria. Our team removed articles that did not specifically focus on communication-related aspects of care quality.
Data Abstraction Process and Data Elements
A data abstraction rubric was developed a priori to align with STS. One code was created for each of 4 STS subsystems. STS considers the
Analysis
Then, we used a deductive content analysis approach to review abstracts and code for whether or not the article mentioned any of the 4 STS subsystems (social, technical, organizational, or external), and read each article using an inductive approach to understand emergent themes within each subsystem code. 20 This information guided the development of our conceptual model on this topic, which presents the emergent themes present in the perinatal literature for each STS subsystem code.
Finally, we imported this dataset into SAS to identify any significant changes (using chi-square tests) in the literature over time, comparing articles published from 2000 to 2020 to those published in 2021 and the first half of 2022. This cut point allowed for manuscripts to go through the publication pipeline after the onset of the racial reckoning that occurred throughout 2020.
Results
Search and Selection Results
From the 2419 articles found in the PubMed search, 2034 articles were removed because they did not focus on our population of interest—Black parents receiving perinatal care in the United States. An additional 212 articles were removed during a second review because they did not focus on our topic of interest—communication during the perinatal period. As shown in Figure 2, this resulted in 172 articles to include in the rapid review.
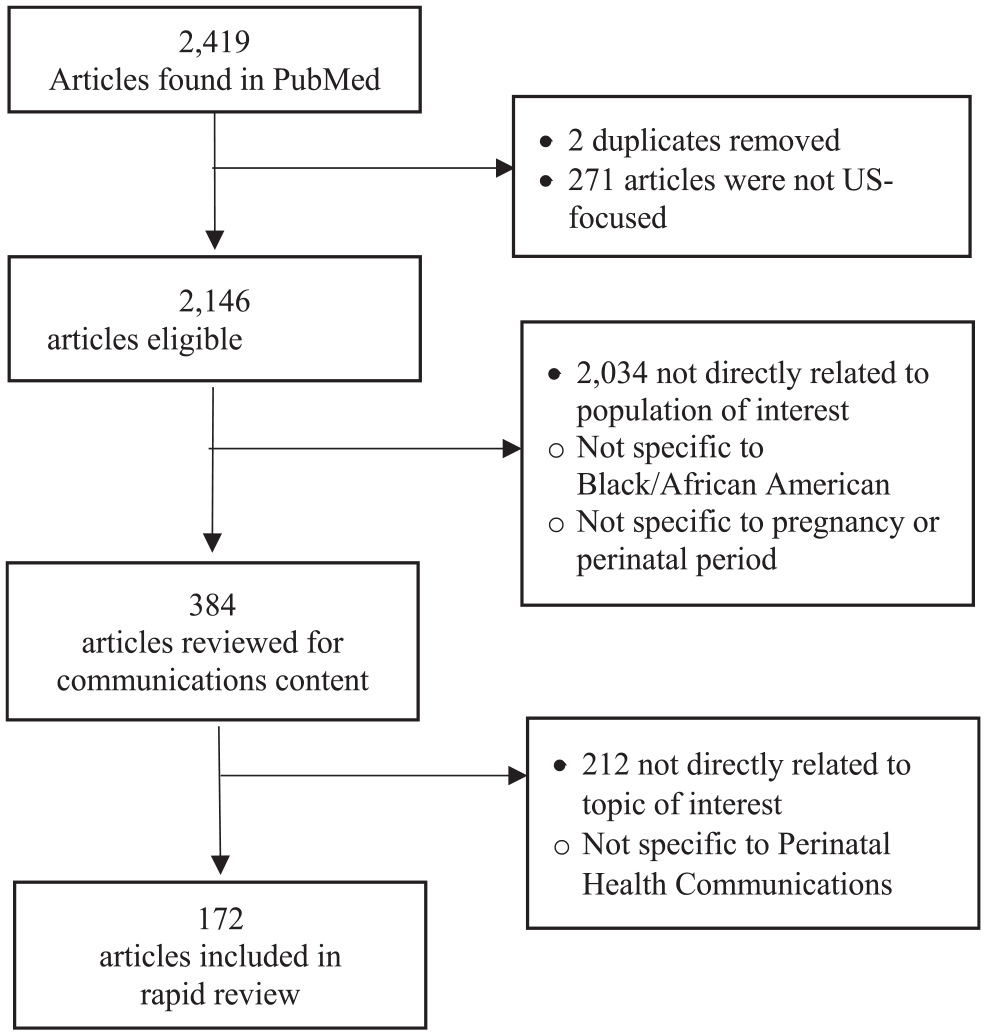
Study selection process.
Descriptive Characteristics of Included Articles
A total of 172 articles were identified for the rapid review. Descriptive characteristics are provided in Table 1 (see Appendix for more detailed results). Most articles explored racial differences between groups (56%), rather than focusing specifically on the Black population (44%) Articles were most likely to include organizational subsystem content (73%) followed by external subsystems content (66%); only 3% of articles included in this rapid review addressed all 4 subsystems.
Descriptive Characteristics of Included Articles, n = 172.
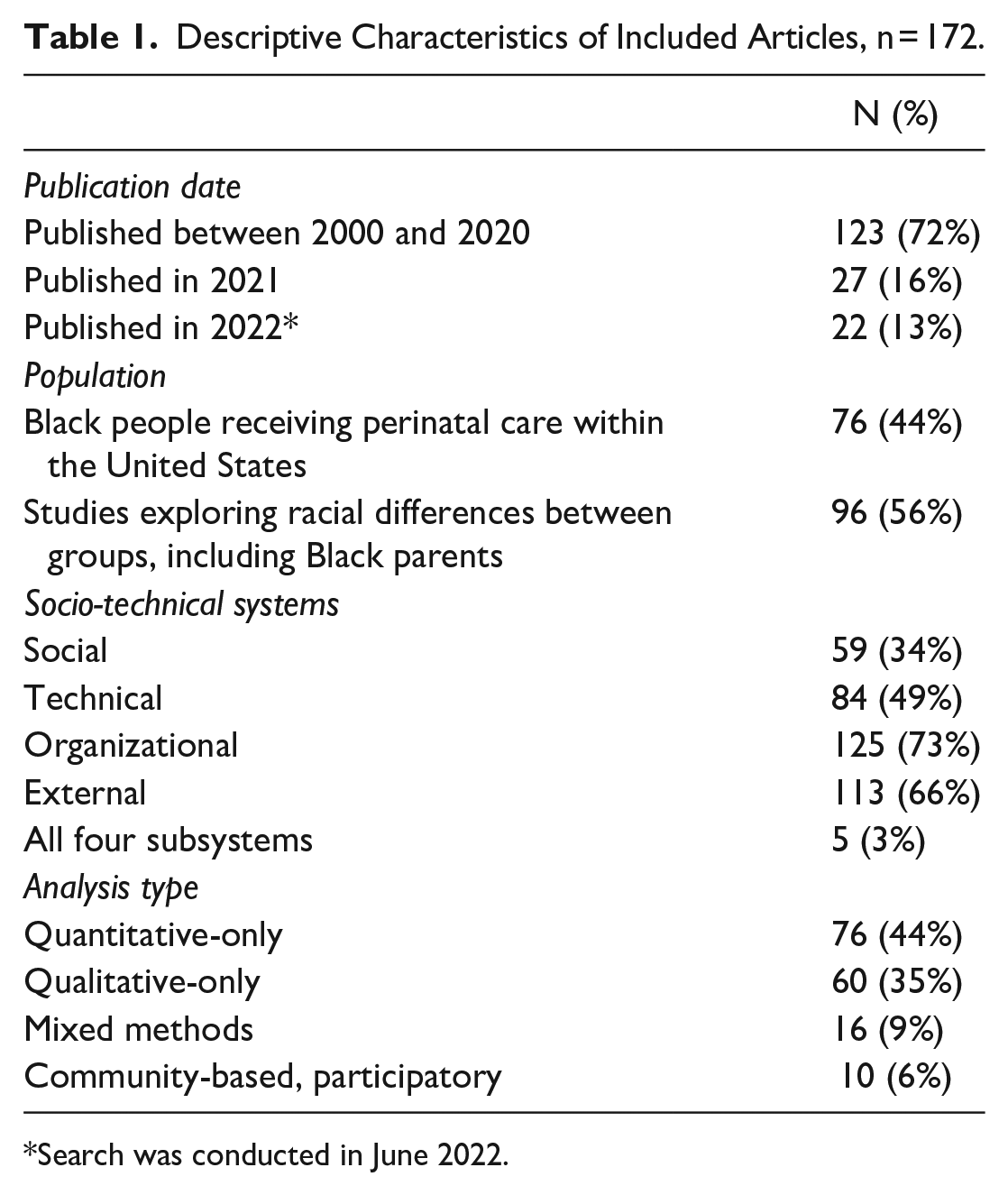

Search was conducted in June 2022.
Socio-Technical Systems (STS) Theory and Perinatal Communication
Resulting from this rapid review content analysis, the developed conceptual model (see Figure 3) illustrates that information related to all 4 subsystems are present in the literature related to perinatal communication and themes emerged under each subsystem.

Resulting conceptual model describing the relationships between social technical system constructs and outcomes in perinatal communication.
Thirty-four percent (34%) of all articles included in this rapid review mentioned social subsystems.
Forty-nine percent (49%) of all articles included in this rapid review mentioned
Seventy-three percent (73%) of all articles included in this rapid review mentioned organizational subsystems. Emergent themes underneath
Sixty-six percent (66%) of the 172 articles mentioned
Changes in the Literature Post-2020
There were significantly more articles published on this topic than predicted in 2021 and 2022 (see Figure 4). In addition, as shown in Table 2, articles published before 2020 were 2.4 times more likely to have technical communication as the primary communication theme compared with articles published in the last 2 years (χ2 = 9.84,

Predicted versus actual number of articles published in 2021 and 2022.
Changes in the Literature Post-2020, n = 172.

Finally, there appears to be an increase in studies that consider communication to be a key component of broader perinatal care quality. Based on our analysis of primary STS code, we found articles published after 2020 were 2 times more likely to focus on “optimized” patient care compared to articles published earlier (χ2 = 5.69,
Discussion and Implications for Practice
Our analysis aimed to describe the subsystems that affect quality perinatal communication and to understand if the national sense of urgency to address racial disparities in America after 2020 potentially had an impact on the ways researchers were studying perinatal communication and/or journals were accepting papers on this topic.
37
The results of our rapid review show there was an increased recognition of communication as a key component of quality perinatal care after 2020 (
Black maternal morbidity is a public health crisis. Health systems and health research must quickly and effectively address the root causes of these disparities. Emerging literature included in this review suggests improving perinatal communication, understood in the broadest sense of quality patient experiences in relationship with a knowledgeable and trustworthy provider throughout the perinatal care continuum, could address some of the racial disparities in perinatal patient and baby outcomes.
To do so, health systems can view this issue through STS framing and consider joint optimization of social, technical, organizational, and external subsystems when undertaking efforts to improve perinatal communication. STS theory-driven intervention design helps a health system map the facilitators and barriers of implementation in each of the 4 subsystems and prompts the system to align all 4 in order to provide quality patient care and communication. We offer our conceptual model (Figure 3) as a tool to facilitate this strategic planning process. Theory-driven intervention design within a health system can be used to assess existing problems according to theory constructs (eg, subsystems) and create solutions that map to those specific constructs. To use this model, health systems must identify current practices and map the determinants prior to selecting intervention methods, and then commit to evaluating the resulting intervention. 38 Consider this example: a health system is considering adoption of a new patient-facing communication tool (technical)—such as our safe fish consumption handout and accompanying website. The system must also identify the current practices, drivers, and barriers behind providers’ ability to effectively introduce these tools to patients during visits (social), provide guidance for providers on expectations related to how and when to have this conversation with patients (organizational), and review the material content to ensure its messages are culturally relevant and respectful of the patient population beliefs and practices (external).
The rapid review approach provides more timely information to decision-makers but lacks the comprehensiveness and rigor of a traditional systematic review. One limitation of our approach is that only one team member coded each article to the STS framework. In addition, our chi-square analysis confirms statistically significant differences in article content during these 2 time periods, but we cannot ascertain the causes of these differences. In particular, we do not know if the change in published articles is driven by changes in researcher perspectives or editorial interests. For our comparative analysis, we selected 2021 as a cut point to explore potential differences, which allowed approximately 7 months after the murder of George Floyd to account for the time it takes for manuscripts to go through the publication pipeline. We acknowledge this process can vary widely and limits our ability to draw conclusions about causality. In addition, our study focused on the United States context and only included articles published in the United States, so there is limited applicability of our study in international contexts.
We found a decrease in studies after 2020 that focused solely on the technical subsystem. This is a promising shift that appears to acknowledge the need for providers to build a strong rapport with patients and prioritize the socioemotional components of communication. Adaptive challenges cannot be solved with technical solutions. 39
If outcomes for Black pregnant people and their children are to improve, health systems must continue to seek to understand and provide for the specific and unique perinatal communication needs of Black or African American pregnant parents and their families. Considering external subsystems is critical in planning; community-based participatory approaches that center community and cultural expertise supports the relationship between health information and health behaviors. Adopting an approach of cultural humility, which “incorporates a lifelong commitment to self-evaluation and critique, to redressing the power imbalances in the physician-patient dynamic, and to developing mutually beneficial and non-paternalistic partnerships with communities on behalf of individuals and defined populations,”
40
may also improve patient-provider communication and rapport. Still, more work is needed to understand
Footnotes
Appendix
Summary of Included Articles.

| Author(s) | Year | Title | Study type and methodology | Focus population | Primary communication theme | Social subsystems | Technical subsystems | Organizational subsystems | External subsystems |
|---|---|---|---|---|---|---|---|---|---|
| Durant T, Colley Gilbert B, Saltzman LE and Johnson CH | 2000 | Opportunities for intervention: discussing physical abuse during prenatal care visits | Quantitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 0 |
| Kaskutas LA | 2000 | Understanding drinking during pregnancy among urban American Indians and African Americans: health messages, risk beliefs, and how we measure consumption | Quantitative | Pregnant people | Information | 1 | 1 | 1 | 1 |
| Raines DA and Morgan Z | 2000 | Culturally sensitive care during childbirth | Quantitative | Postpartum people | Patient Care | 1 | 1 | 0 | 0 |
| Bechtel-Blackwell DA | 2002 | Computer-assisted self-interview and nutrition education in pregnant teens | Quantitative | Black/African American | Technical | 1 | 1 | 1 | 1 |
| Robinson DC, Reitan RE, Jones GN and Gist RS | 2002 | Knowledge of neonatal car seat location in a predominantly disadvantaged prenatal population | Quantitative | Low income | Information | 1 | 1 | 1 | 0 |
| Beal AC, Kuhlthau K and Perrin JM | 2003 | Breastfeeding advice given to African American and white women by physicians and WIC counselors | Quantitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Handler A, Rosenberg D, Raube K and Lyons S | 2003 | Prenatal care characteristics and African-American women’s satisfaction with care in a managed care organization | Mixed methods | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 0 |
| Handler A, Rosenberg D, Raube K and Lyons S | 2003 | Satisfaction and use of prenatal care: their relationship among African-American women in a large managed care organization | Quantitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Moran S, Thorndike AN, Armstrong K and Rigotti NA | 2003 | Physicians’ missed opportunities to address tobacco use during prenatal care | Quantitative | Pregnant people | Information | 1 | 1 | 1 | 0 |
| Sharps PW, El-Mohandes AA, Nabil El-Khorazaty M, Kiely M and Walker T | 2003 | Health beliefs and parenting attitudes influence breastfeeding patterns among low-income African-American women | Quantitative | Black/African American | Information | 1 | 1 | 1 | 0 |
| Nicholson WK, Brickhouse B, Powe NR and Bronner Y | 2004 | Prenatal patients’ views of prenatal care services: a medical center-based assessment of knowledge and intent to use support services | Quantitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Sheppard VB, Zambrana RE and O’Malley AS | 2004 | Providing health care to low-income women: a matter of trust | Quantitative | Low income | Pt-provider communication | 1 | 1 | 1 | 0 |
| Wong ST, Korenbrot CC and Stewart AL | 2004 | Consumer assessment of the quality of interpersonal processes of prenatal care among ethnically diverse low-income women: development of a new measure | Quantitative | Low income | Pt-provider relationship | 1 | 1 | 1 | 1 |
| de Jong-Van den Berg LT, Hernandez-Diaz S, Werler MM, Louik C and Mitchell AA | 2005 | Trends and predictors of folic acid awareness and periconceptional use in pregnant women | Quantitative | Pregnant people | Information | 1 | 1 | 1 | 0 |
| Herman J, Mock K, Blackwell D and Hulsey T | 2005 | Use of a pregnancy support web site by low-income African American women | Quantitative | Black/African American | Technical | 1 | 1 | 1 | 0 |
| Bennett I, Switzer J, Aguirre A, Evans K and Barg F | 2006 | “Breaking it down”: patient-clinician communication and prenatal care among African American women of low and higher literacy | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Cricco-Lizza R | 2006 | Black non-Hispanic mothers’ perceptions about the promotion of infant-feeding methods by nurses and physicians | Qualitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Proctor A, Jenkins TR, Loeb T, Elliot M and Ryan A | 2006 | Patient satisfaction with 3 methods of postpartum contraceptive counseling: a randomized, prospective trial | Qualitative | Postpartum people | Information | 1 | 1 | 1 | 1 |
| Ickovics JR, Kershaw TS, Westdahl C, Magriples U, Massey Z, Reynolds H and Rising SS | 2007 | Group prenatal care and perinatal outcomes: a randomized controlled trial | Qualitative | Pregnant people | Patient Care | 1 | 1 | 1 | 1 |
| Vonderheid SC, Norr KF and Handler AS | 2007 | Prenatal health promotion content and health behaviors | Qualitative | BIPOC | Information | 1 | 1 | 1 | 1 |
| Jesse DE, Dolbier CL and Blanchard A | 2008 | Barriers to seeking help and treatment suggestions for prenatal depressive symptoms: focus groups with rural low-income women | Qualitative | Pregnant people | Pt-provider relationship | 1 | 1 | 1 | 1 |
| O’Mahen HA and Flynn HA | 2008 | Preferences and perceived barriers to treatment for depression during the perinatal period | Qualitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Wheatley RR, Kelley MA, Peacock N and Delgado J | 2008 | Women’s narratives on quality in prenatal care: a multicultural perspective | Qualitative | Low income | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Yi CH, Lori J and Martyn K | 2008 | Development of prenatal event history calendar for Black women | Qualitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Clinch CR, Grzywacz JG, Tucker J, Walls JK and Arcury TA | 2009 | Characteristics of mother-provider interactions surrounding postpartum return to work | Qualitative | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Evenson KR, Moos MK, Carrier K and Siega-Riz AM | 2009 | Perceived barriers to physical activity among pregnant women | Qualitative | Pregnant people | Information | 1 | 1 | 1 | 0 |
| Feinberg E, Smith MV and Naik R | 2009 | Ethnically diverse mothers’ views on the acceptability of screening for maternal depressive symptoms during pediatric well-child visits | Qualitative | Low income | Pt-provider communication | 1 | 1 | 1 | 1 |
| Humbert L and Roberts TL | 2009 | The value of a learner’s stance: lessons learned from pregnant and parenting women | Qualitative | Low income | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Klima C, Norr K, Vonderheid S and Handler A | 2009 | Introduction of CenteringPregnancy in a public health clinic | Qualitative | Black/African American | Information | 1 | 1 | 1 | 0 |
| Lang CW, Stark AP, Acharya K and Ross LF | 2009 | Maternal knowledge and attitudes about newborn screening for sickle cell disease and cystic fibrosis | Qualitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Shieh C, McDaniel A and Ke I | 2009 | Information-seeking and its predictors in low-income pregnant women | Qualitative | Low income | Information | 1 | 1 | 1 | 1 |
| Cannella D, Lobel M and Monheit A | 2010 | Knowing is believing: information and attitudes towards physical activity during pregnancy | Community-based participatory approach | Pregnant people | Information | 1 | 1 | 1 | 1 |
| Jones L, Wright K, Wright A, Brown ND, Broussard M and Hogan V | 2010 | The Healthy African American Families’ risk communications initiative: using community partnered participatory research to address preterm birth at the local level | Qualitative | Black/African American | Patient Care | 1 | 1 | 0 | 0 |
| Thornberry JS, Murray KB, El-Khorazaty MN and Kiely M | 2010 | Acceptance, Communication Mode and Use of Audio Computer-Assisted Self Interview Using Touchscreen to Identify Risk Factors among Pregnant Minority Women | Community-based participatory approach | Pregnant people | Technical | 1 | 1 | 1 | 1 |
| Wright K, Jones L and Hogan V | 2010 | A roadmap for authentic community/academic engagement for developing effective community preterm birth education | Qualitative | Black/African American | Information | 1 | 1 | 0 | 1 |
| Leis JA, Mendelson T, Perry DF and Tandon SD | 2011 | Perceptions of mental health services among low-income, perinatal African-American women | Qualitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Ley CE, Copeland VC and Flint CS | 2011 | Healthy start program participation: the consumers’ perspective | Qualitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 0 |
| Lori JR, Yi CH and Martyn KK | 2011 | Provider characteristics desired by African American women in prenatal care | Qualitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 0 |
| Mauriello L, Dyment S, Prochaska J, Gagliardi A and Weingrad-Smith J | 2011 | Acceptability and feasibility of a multiple-behavior, computer-tailored intervention for underserved pregnant women | Qualitative | Pregnant people | Technical | 1 | 1 | 1 | 0 |
| Pati S, Feemster KA, Mohamad Z, Fiks A, Grundmeier R and Cnaan A | 2011 | Maternal health literacy and late initiation of immunizations among an inner-city birth cohort | Qualitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Shieh C and Weaver MT | 2011 | Comparisons in perceived importance of and needs for maternal gestational weight information between African American and Caucasian pregnant women | Qualitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Yee L and Simon M | 2011 | Urban minority women’s perceptions of and preferences for postpartum contraceptive counseling | Quantitative | BIPOC | Pt-provider communication | 1 | 1 | 1 | 1 |
| Yee LM and Simon MA | 2011 | Perceptions of coercion, discrimination and other negative experiences in postpartum contraceptive counseling for low-income minority women | Quantitative | BIPOC | Pt-provider communication | 1 | 1 | 1 | 1 |
| Baffour TD and Chonody JM | 2012 | Do empowerment strategies facilitate knowledge and behavioral change? The impact of family health advocacy on health outcomes | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Cross-Barnet C, Augustyn M, Gross S, Resnik A and Paige D | 2012 | Long-term breastfeeding support: failing mothers in need | Quantitative | Low income | Information | 1 | 1 | 1 | 1 |
| Gold KJ, Boggs ME, Mugisha E and Palladino CL | 2012 | Internet message boards for pregnancy loss: who’s on-line and why? | Mixed methods | Pregnant people | Technical | 1 | 1 | 1 | 1 |
| Janssen SM and Lagro-Janssen AL | 2012 | Physician’s gender, communication style, patient preferences and patient satisfaction in gynecology and obstetrics: a systematic review | Quantitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Johnson AM, Nwana C, Egan JF and Dumont-Mathieu T | 2012 | Reported experiences with prenatal care: is there a difference in patient satisfaction based on racial and ethnic background? | Quantitative | Pregnant people | Patient Care | 1 | 1 | 1 | 0 |
| Liu CH and Tronick E | 2012 | Do patient characteristics, prenatal care setting, and method of payment matter when it comes to provider-patient conversations on perinatal mood? | Mixed methods | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Munro ML, Dahlem CH, Lori JR and Martyn KK | 2012 | Prenatal psychosocial risk assessment using event history calendars with Black women | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Ondersma SJ, Svikis DS, Lam PK, Connors-Burge VS, Ledgerwood DM and Hopper JA | 2012 | A randomized trial of computer-delivered brief intervention and low-intensity contingency management for smoking during pregnancy | Quantitative | Black/African American | Technical | 1 | 1 | 1 | 0 |
| Walker LO, Im EO and Vaughan MW | 2012 | Communication technologies and maternal interest in health-promotion information about postpartum weight and parenting practices | Quantitative | Postpartum people | Technical | 1 | 1 | 1 | 0 |
| Cottrell BH and Detman LA | 2013 | Breastfeeding concerns and experiences of African American mothers | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Elek E, Harris SL, Squire CM, Margolis M, Weber MK, Dang EP and Mitchell B | 2013 | Women’s Knowledge, Views, and Experiences Regarding Alcohol Use and Pregnancy: Opportunities to Improve Health Messages | Qualitative | Pregnant people | Information | 1 | 1 | 1 | 1 |
| Ferrari RM, Siega-Riz AM, Evenson KR, Moos MK and Carrier KS | 2013 | A qualitative study of women’s perceptions of provider advice about diet and physical activity during pregnancy | Qualitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Frew PM, Zhang S, Saint-Victor DS, Schade AC, Benedict S, Banan M, Ren X and Omer SB | 2013 | Influenza vaccination acceptance among diverse pregnant women and its impact on infant immunization | Qualitative | Pregnant people | Information | 1 | 1 | 1 | 0 |
| Salm Ward TC, Mazul M, Ngui EM, Bridgewater FD and Harley AE | 2013 | You learn to go last: perceptions of prenatal care experiences among African-American women with limited incomes | Mixed methods | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Attanasio LB, McPherson ME and Kozhimannil KB | 2014 | Positive childbirth experiences in U.S. hospitals: a mixed methods analysis | Qualitative | Postpartum people | Patient Care | 1 | 1 | 1 | 1 |
| Cha S and Masho SW | 2014 | Discussions about intimate partner violence during prenatal care in the United States: the role of race/ethnicity and insurance status | Qualitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Lee King PA and Pate DJ | 2014 | Perinatal HIV testing among African American, Caucasian, Hmong and Latina women: exploring the role of health-care services, information sources and perceptions of HIV/AIDS | Qualitative | Low income | Information | 1 | 1 | 1 | 1 |
| Marsh HA, Malik F, Shapiro E, Omer SB and Frew PM | 2014 | Message framing strategies to increase influenza immunization uptake among pregnant African American women | Qualitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Mobley SC, Thomas SD, Sutherland DE, Hudgins J, Ange BL and Johnson MH | 2014 | Maternal health literacy progression among rural perinatal women | Qualitative | Pregnant people | Information | 1 | 1 | 1 | 0 |
| Morris T and Schulman M | 2014 | Race inequality in epidural use and regional anesthesia failure in labor and birth: an examination of women’s experience | Qualitative | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Peters RM, Benkert R, Templin TN and Cassidy-Bushrow AE | 2014 | Measuring African American women’s trust in provider during pregnancy | Qualitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 0 |
| Attanasio L and Kozhimannil KB | 2015 | Patient-reported Communication Quality and Perceived Discrimination in Maternity Care | Qualitative | Postpartum people | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Broom MA, Ladley AS, Rhyne EA and Halloran DR | 2015 | Feasibility and Perception of Using Text Messages as an Adjunct Therapy for Low-Income, Minority Mothers with Postpartum Depression | Community-based participatory approach | Low income | Technical | 1 | 1 | 1 | 1 |
| Bryant AS, Norton ME, Nakagawa S, Bishop JT, Pena S, Gregorich SE and Kuppermann M | 2015 | Variation in Women’s Understanding of Prenatal Testing | Qualitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Chilukuri N, West M, Henderson JL, Lawson S, Ehsanipoor R, Costigan K, Polk S and Bennett W | 2015 | Information and Communication Technology Use Among Low-Income Pregnant and Postpartum Women by Race and Ethnicity: A Cross-Sectional Study | Qualitative | Low income | Technical | 1 | 1 | 1 | 1 |
| Dahlem CH, Villarruel AM and Ronis DL | 2015 | African American women and prenatal care: perceptions of patient-provider interaction | Qualitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Healy CM, Rench MA, Montesinos DP, Ng N and Swaim LS | 2015 | Knowledge and attitudes of pregnant women and their providers towards recommendations for immunization during pregnancy | Qualitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Kaptein S, Evans M, McTavish S, Banerjee AT, Feig DS, Lowe J and Lipscombe LL | 2015 | The subjective impact of a diagnosis of gestational diabetes among ethnically diverse pregnant women: a qualitative study | Qualitative | Pregnant people | Information | 1 | 1 | 1 | 0 |
| Kim HK, Niederdeppe J, Guillory J, Graham M, Olson C and Gay G | 2015 | Determinants of Pregnant Women’s Online Self-Regulatory Activities for Appropriate Gestational Weight Gain | Qualitative | Pregnant people | Technical | 1 | 1 | 1 | 1 |
| Kominiarek MA, Gay F and Peacock N | 2015 | Obesity in Pregnancy: A Qualitative Approach to Inform an Intervention for Patients and Providers | Qualitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Oza-Frank R, Kachoria R, Keim SA, Lynch CD and Klebanoff MA | 2015 | Receipt and timing of pregnancy-related preventive health messages vary by message type and maternal characteristics | Qualitative | Postpartum people | Technical | 1 | 1 | 1 | 0 |
| Pollick SA, Beatty JR, Sokol RJ, Strickler RC, Chang G, Svikis DS, Tzilos GK and Ondersma SJ | 2015 | Acceptability of a computerized brief intervention for alcohol among abstinent but at-risk pregnant women | Qualitative | Black/African American | Technical | 1 | 1 | 1 | 1 |
| Roter DL, Erby LH, Rimal RN, Smith KC, Larson S, Bennett IM, Cole KW, Guan Y, Molloy M and Bienstock J | 2015 | Empowering Women’s Prenatal Communication: Does Literacy Matter? | Qualitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Tucker Edmonds B, Mogul M and Shea JA | 2015 | Understanding low-income African American women’s expectations, preferences, and priorities in prenatal care | Qualitative | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Backonja U, Robledo CA, Wallace ME, Flores KF and Kiely M | 2016 | Reproductive Health Knowledge among African American Women Enrolled in a Clinic-Based Randomized Controlled Trial to Reduce Psychosocial and Behavioral Risk: Project DC-HOPE | Qualitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 0 |
| Frew PM, Kriss JL, Chamberlain AT, Malik F, Chung Y, Cortés M and Omer SB | 2016 | A randomized trial of maternal influenza immunization decision-making: A test of persuasive messaging models | Qualitative | Black/African American | Technical | 1 | 1 | 1 | 1 |
| Nypaver CF and Shambley-Ebron D | 2016 | Using Community-Based Participatory Research to Investigate Meaningful Prenatal Care Among African American Women | Qualitative | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Shulman R and Kottke M | 2016 | Impact of maternal knowledge of recommended weight gain in pregnancy on gestational weight gain | Community-based participatory approach | Black/African American | Information | 1 | 1 | 1 | 1 |
| Whitaker KM, Wilcox S, Liu J, Blair SN and Pate RR | 2016 | Patient and Provider Perceptions of Weight Gain, Physical Activity, and Nutrition Counseling during Pregnancy: A Qualitative Study | Qualitative | Pregnant people | Information | 1 | 1 | 1 | 1 |
| Yee LM, Niznik CM and Simon MA | 2016 | Examining the Role of Health Literacy in Optimizing the Care of Pregnant Women with Diabetes | Mixed methods | Pregnant people | Information | 1 | 1 | 1 | 1 |
| Attanasio L and Kozhimannil KB | 2017 | Health Care Engagement and Follow-up After Perceived Discrimination in Maternity Care | Qualitative | Postpartum people | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Bodnar-Deren S, Benn EKT, Balbierz A and Howell EA | 2017 | Stigma and Postpartum Depression Treatment Acceptability Among Black and White Women in the First Six-Months Postpartum | Qualitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 0 |
| Enlow E, Faherty LJ, Wallace-Keeshen S, Martin AE, Shea JA and Lorch SA | 2017 | Perspectives of Low Socioeconomic Status Mothers of Premature Infants | Mixed methods | Black/African American | Pt-provider communication | 1 | 1 | 1 | 0 |
| Gold KJ, Treadwell MC, Mieras ME and Laventhal NT | 2017 | Who tells a mother her baby has died? Communication and staff presence during stillbirth delivery and early infant death | Quantitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 0 |
| Guendelman S, Broderick A, Mlo H, Gemmill A and Lindeman D | 2017 | Listening to Communities: Mixed-Method Study of the Engagement of Disadvantaged Mothers and Pregnant Women with Digital Health Technologies | Quantitative | Low income | Technical | 1 | 1 | 1 | 1 |
| Mazul MC, Salm Ward TC and Ngui EM | 2017 | Anatomy of Good Prenatal Care: Perspectives of Low Income African-American Women on Barriers and Facilitators to Prenatal Care | Qualitative | Black/African American | Patient Care | 1 | 1 | 1 | 0 |
| Roman LA, Raffo JE, Dertz K, Agee B, Evans D, Penninga K, Pierce T, Cunningham B and VanderMeulen P | 2017 | Understanding Perspectives of African American Medicaid-Insured Women on the Process of Perinatal Care: An Opportunity for Systems Improvement | Quantitative | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Stones RE, Stulberg DB and Bello Kottenstette JK | 2017 | Patient Experiences with Pregnancy Planning and Perspectives on Reproductive Care in Community Health Centers: A Qualitative Study of African American Women in Chicago | Quantitative | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Attanasio LB, Kozhimannil KB and Kjerulff KH | 2018 | Factors influencing women’s perceptions of shared decision making during labor and delivery: Results from a large-scale cohort study of first childbirth | Mixed methods | Postpartum people | Patient Care | 1 | 1 | 1 | 1 |
| Coley SL, Zapata JY, Schwei RJ, Mihalovic GE, Matabele MN, Jacobs EA and Anderson CK | 2018 | More Than a “Number”: Perspectives of Prenatal Care Quality from Mothers of Color and Providers | Mixed methods | Black/African American | Patient Care | 1 | 1 | 0 | 0 |
| Delgado A, Stark LM, Macri CJ, Power ML and Schulkin J | 2018 | Provider and Patient Knowledge and Views of Office Practices on Weight Gain and Exercise during Pregnancy | Quantitative | Black/African American | Information | 1 | 1 | 1 | 1 |
| Ellingson M and Chamberlain AT | 2018 | Beyond the verbal: Pregnant women’s preferences for receiving influenza and Tdap vaccine information from their obstetric care providers | Quantitative | Pregnant people | Technical | 1 | 1 | 1 | 1 |
| Flanagan T, Alabaster A, McCaw B, Stoller N, Watson C and Young-Wolff KC | 2018 | Feasibility and Acceptability of Screening for Adverse Childhood Experiences in Prenatal Care | Quantitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Howell EA | 2018 | Reducing Disparities in Severe Maternal Morbidity and Mortality | Community-based participatory approach | Pregnant people | Patient Care | 1 | 1 | 1 | 0 |
| McGinnis S, Lee E, Kirkland K, Miranda-Julian C and Greene R | 2018 | Let’s Talk About Breastfeeding: The Importance of Delivering a Message in a Home Visiting Program | Quantitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Mukherjee S, Fennie K, Coxe S, Madhivanan P and Trepka MJ | 2018 | Racial and ethnic differences in the relationship between antenatal stressful life events and postpartum depression among women in the United States: does provider communication on perinatal depression minimize the risk? | Quantitative | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Walker LO, Sterling BS, Becker H, Hendrickson S and Xie B | 2018 | Development and evaluation of a mother-centered toolkit for postpartum behavioral and psychosocial health | Quantitative | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Acquavita SP, Krummel DA, Talks A, Cobb A and McClure E | 2019 | Assessing the Digital Divide Among Low-Income Perinatal Women: Opportunities for Provision of Health Information and Counseling | Quantitative | Black/African American | Technical | 1 | 1 | 1 | 0 |
| Altman MR, Oseguera T, McLemore MR, Kantrowitz-Gordon I, Franck LS and Lyndon A | 2019 | Information and power: Women of color’s experiences interacting with health care providers in pregnancy and birth | Quantitative | BIPOC | Pt-provider relationship | 1 | 1 | 1 | 0 |
| Attanasio LB and Hardeman RR | 2019 | Declined care and discrimination during the childbirth hospitalization | Quantitative | Postpartum people | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Boyd RC, Price J, Mogul M, Yates T and Guevara JP | 2019 | Pilot RCT of a social media parenting intervention for postpartum mothers with depression symptoms | Quantitative | Black/African American | Technical | 1 | 1 | 1 | 1 |
| Evans NM and Sheu JJ | 2019 | Validating a path model of adherence to prenatal care recommendations among pregnant women | Quantitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Fenstermacher KH and Hupcey JE | 2019 | Support for Young Black Urban Women After Perinatal Loss | Community-based participatory approach | Black/African American | Patient Care | 1 | 1 | 1 | 0 |
| Hirshberg A, Sammel MD and Srinivas SK | 2019 | Text message remote monitoring reduced racial disparities in postpartum blood pressure ascertainment | Qualitative | Postpartum people | Technical | 1 | 1 | 1 | 0 |
| Kamke K, Grenen E, Robinson C and El-Toukhy S | 2019 | Dropout and Abstinence Outcomes in a National Text Messaging Smoking Cessation Intervention for Pregnant Women, SmokefreeMOM: Observational Study | Qualitative | Pregnant people | Technical | 1 | 1 | 1 | 1 |
| Karbeah J, Hardeman R, Almanza J and Kozhimannil KB | 2019 | Identifying the Key Elements of Racially Concordant Care in a Freestanding Birth Center | Qualitative | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Miller CA, Roe AH, McAllister A, Meisel ZF, Koelper N and Schreiber CA | 2019 | Patient Experiences with Miscarriage Management in the Emergency and Ambulatory Settings | Qualitative | Pregnant people | Patient Care | 1 | 1 | 1 | 1 |
| Molina F, Dehlendorf C, Gregorich SE and Kuppermann M | 2019 | Women’s preferences for and experiences with prenatal genetic testing decision making: Sociodemographic disparities in preference-concordant decision making | Qualitative | Pregnant people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Newcomb P, True B, Wells JN, Walsh J and Pehl S | 2019 | Informing New Mothers about Newborn Screening Bloodspot Repositories during Postpartum Hospitalization | Mixed methods | Postpartum people | Information | 1 | 1 | 1 | 0 |
| Robinson A, Davis M, Hall J, Lauckner C and Anderson AK | 2019 | It Takes an E-Village: Supporting African American Mothers in Sustaining Breastfeeding Through Facebook Communities | Qualitative | Black/African American | Technical | 1 | 1 | 1 | 1 |
| Shorten A, Shorten B, Fagerlin A, Illuzzi J, Kennedy HP, Pettker C, Raju D and Whittemore R | 2019 | A Study to Assess the Feasibility of Implementing a Web-Based Decision Aid for Birth after Cesarean to Increase Opportunities for Shared Decision Making in Ethnically Diverse Settings | Qualitative | Postpartum people | Information | 1 | 1 | 1 | 1 |
| Vedam S, Stoll K, Taiwo TK, Rubashkin N, Cheyney M, Strauss N, McLemore M, Cadena M, Nethery E, Rushton E, Schummers L and Declercq E | 2019 | The Giving Voice to Mothers study: inequity and mistreatment during pregnancy and childbirth in the United States | Quantitative | Pregnant people | Patient Care | 1 | 1 | 1 | 1 |
| Ahlers-Schmidt CR, Okut H and Dowling J | 2020 | Impact of Prenatal Education on Breastfeeding Initiation Among Low-Income Women | Quantitative | Low income | Information | 1 | 1 | 1 | 1 |
| Anderson CA and Ghirmazion E | 2020 | The Adolescent Birth Experience: A Comparison of Three Diverse Groups | Quantitative | Postpartum people | Patient Care | 1 | 1 | 1 | 0 |
| Blackwell TM, Dill LJ, Hoepner LA and Geer LA | 2020 | Using Text Messaging to Improve Access to Prenatal Health Information in Urban African American and Afro-Caribbean Immigrant Pregnant Women: Mixed Methods Analysis of Text4baby Usage | Quantitative | Black/African American | Technical | 1 | 1 | 1 | 1 |
| Bryant AS, Riley LE, Neale D, Hill W, Jones TB, Jeffers NK, Loftman PO, Clare CA and Gudeman J | 2020 | Communicating with African-American Women Who Have Had a Preterm Birth About Risks for Future Preterm Births | Mixed methods | Black/African American | Pt-provider communication | 1 | 1 | 1 | 0 |
| Declercq E, Sakala C and Belanoff C | 2020 | Women’s experience of agency and respect in maternity care by type of insurance in California | Mixed methods | Low income | Pt-provider relationship | 1 | 1 | 1 | 0 |
| Dillon B, Albritton T, Saint Fleur-Calixte R, Rosenthal L and Kershaw T | 2020 | Perceived Discriminatory Factors that Impact Prenatal Care Satisfaction and Attendance Among Adolescent and Young Adult Couples | Commentary | Pregnant people | Patient Care | 1 | 1 | 1 | 0 |
| Hardeman RR, Karbeah J and Kozhimannil KB | 2020 | Applying a critical race lens to relationship-centered care in pregnancy and childbirth: An antidote to structural racism | Quantitative | Black/African American | Pt-provider relationship | 1 | 1 | 0 | 0 |
| Janevic T, Piverger N, Afzal O and Howell EA | 2020 | Just Because You Have Ears Doesn’t Mean You Can Hear-Perception of Racial-Ethnic Discrimination During Childbirth | Quantitative | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Adebayo CT, Parcell ES, Mkandawire-Valhmu L and Olukotun O | 2021 | African American Women’s Maternal Healthcare Experiences: A Critical Race Theory Perspective | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Afulani PA, Altman MR, Castillo E, Bernal N, Jones L, Camara TL, Carrasco Z, Williams S, Sudhinaraset M and Kuppermann M | 2021 | Development of the person-centered prenatal care scale for people of color | Quantitative | Black/African American | Patient Care | 1 | 1 | 0 | 1 |
| Attanasio LB, Ranchoff BL and Geissler KH | 2021 | Perceived discrimination during the childbirth hospitalization and postpartum visit attendance and content: Evidence from the Listening to Mothers in California survey | Quantitative | Postpartum people | Patient Care | 1 | 1 | 1 | 0 |
| Basile Ibrahim B, Kennedy HP and Combellick J | 2021 | Experiences of Quality Perinatal Care During the US COVID-19 Pandemic | Quantitative | BIPOC | Patient Care | 1 | 1 | 1 | 0 |
| Bookhart LH, Joyner AB, Lee K, Worrell N, Jamieson DJ and Young MF | 2021 | Moving Beyond Breastfeeding Initiation: A Qualitative Study Unpacking Factors That Influence Infant Feeding at Hospital Discharge Among Urban, Socioeconomically Disadvantaged Women | Mixed methods | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 0 |
| Carter EB and Mazzoni SE | 2021 | A paradigm shift to address racial inequities in perinatal healthcare | Quantitative | Black/African American | Pt-provider relationship | 1 | 1 | 0 | 1 |
| Collins CC, Brown PL, Rice H, Bronson C, Cherney E, Farmer C and DeRigne L | 2021 | Experiences of Black women during pregnancy: The meaning of perinatal support | Community-based participatory approach | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Collins CC, Rice H, Bai R, Brown PL, Bronson C and Farmer C | 2021 | I felt like it would’ve been perfect, if they hadn’t been rushing: Black women’s childbirth experiences with medical providers when accompanied by perinatal support professionals | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 0 |
| Deichen Hansen ME, James BA, Sakinah I, Brown Speights JS and Rust G | 2021 | Traversing Traditions: Prenatal Care and Birthing Practice Preferences Among Black Women in North Florida | Quantitative | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Duryea EL, Adhikari EH, Ambia A, Spong C, McIntire D and Nelson DB | 2021 | Comparison Between In-Person and Audio-Only Virtual Prenatal Visits and Perinatal Outcomes | Quantitative | Postpartum people | Technical | 1 | 1 | 1 | 0 |
| Glazer KB, Sofaer S, Balbierz A, Wang E and Howell EA | 2021 | Perinatal care experiences among racially and ethnically diverse mothers whose infants required a NICU stay | Quantitative | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 0 |
| Green CL, Perez SL, Walker A, Estriplet T, Ogunwole SM, Auguste TC and Crear-Perry JA | 2021 | The Cycle to Respectful Care: A Qualitative Approach to the Creation of an Actionable Framework to Address Maternal Outcome Disparities | Quantitative | Black/African American | Patient Care | 1 | 1 | 1 | 0 |
| Iturralde E, Hsiao CA, Nkemere L, Kubo A, Sterling SA, Flanagan T and Avalos LA | 2021 | Engagement in perinatal depression treatment: a qualitative study of barriers across and within racial/ethnic groups | Mixed methods | Pregnant people | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Janevic T, Maru S, Nowlin S, McCarthy K, Bergink V, Stone J, Dias J, Wu S and Howell EA | 2021 | Pandemic Birthing: Childbirth Satisfaction, Perceived Health Care Bias, and Postpartum Health During the COVID-19 Pandemic | Quantitative | BIPOC | Patient Care | 1 | 1 | 1 | 0 |
| Jefferson UT, Bloom TL and Lewis KR | 2021 | Infant Feeding Exposure and Personal Experiences of African American Mothers | Quantitative | Black/African American | Information | 1 | 1 | 1 | 0 |
| Leziak K, Birch E, Jackson J, Strohbach A, Niznik C and Yee LM | 2021 | Identifying Mobile Health Technology Experiences and Preferences of Low-Income Pregnant Women with Diabetes | Quantitative | Low income | Technical | 1 | 1 | 1 | 0 |
| Markin RD and Coleman MN | 2021 | Intersections of gendered racial trauma and childbirth trauma: Clinical interventions for Black women | Quantitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 1 |
| McKinley EM, Knol LL, Turner LW, Burnham JJ, Graettinger KR, Hernandez-Reif M and Leeper JD | 2021 | Enhancing Patient-Provider Breastfeeding Conversations: Breastfeeding Intention and Prenatal Breastfeeding Self-Efficacy among a Sample of Pregnant Women | Mixed methods | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Mszar R, Gopal DJ, Chowdary R, Smith CL, Dolin CD, Irwin ML, Soffer D, Nemiroff R and Lewey J | 2021 | Racial/Ethnic Disparities in Screening for and Awareness of High Cholesterol Among Pregnant Women Receiving Prenatal Care | Quantitative | Pregnant people | Information | 1 | 1 | 1 | 1 |
| Peyton-Caire L and Stevenson A | 2021 | Listening to Black Women: The Critical Step to Eliminating Wisconsin’s Black Birth Disparities | Quantitative | Black/African American | Patient Care | 1 | 1 | 0 | 1 |
| Reissig M, Fair C, Houpt B and Latham V | 2021 | An Exploratory Study of the Role of Birth Stories in Shaping Expectations for Childbirth among Nulliparous Black Women: Everybody is Different (but I’m Scared) | Commentary | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Russell S | 2021 | Eradicating Racism from Maternity Care Begins with Addressing Implicit Bias | Quantitative | Black/African American | Pt-provider relationship | 1 | 1 | 0 | 1 |
| Schlaff RA, Baruth M and LaFramboise FC | 2021 | Preparing for postpartum: health care provider discussions and predictors of patient satisfaction | Commentary | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Ukoha EP, Davis K, Yinger M, Butler B, Ross T, Crear-Perry J, Perron-Burdick M and Nijagal MA | 2021 | Ensuring Equitable Implementation of Telemedicine in Perinatal Care | Quantitative | Pregnant people | Technical | 1 | 1 | 0 | 0 |
| Wang E, Glazer KB, Sofaer S, Balbierz A and Howell EA | 2021 | Racial and Ethnic Disparities in Severe Maternal Morbidity: A Qualitative Study of Women’s Experiences of Peripartum Care | Quantitative | Postpartum people | Pt-provider communication | 1 | 1 | 1 | 1 |
| Wishart D, Cruz Alvarez C, Ward C, Danner S, O’Brian CA and Simon M | 2021 | Racial and Ethnic Minority Pregnant Patients with Low-Income Experiences of Perinatal Care: A Scoping Review | Quantitative | BIPOC | Patient Care | 1 | 1 | 1 | 0 |
| Yee LM, Silver R, Haas DM, Parry S, Mercer BM, Wing DA, Reddy U, Saade GR, Simhan H and Grobman WA | 2021 | Association of Health Literacy Among Nulliparous Individuals and Maternal and Neonatal Outcomes | Commentary | Pregnant people | Information | 1 | 1 | 1 | 1 |
| Adams YJ and Young J | 2022 | Perceptions of Postpartum Teaching and Knowledge of Warning Signs among Black Mothers | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Afulani PA, Altman MR, Castillo E, Bernal N, Jones L, Camara T, Carrasco Z, Williams S, Sudhinaraset M and Kuppermann M | 2022 | Adaptation of the Person-Centered Maternity Care Scale in the United States: Prioritizing the Experiences of Black Women and Birthing People | Quantitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Alio AP, Dillion T, Hartman S, Johnson T, Turner S, Bullock S and Dozier A | 2022 | A Community Collaborative for the Exploration of Local Factors Affecting Black Mothers’ Experiences with Perinatal Care | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 1 |
| Almanza JI, Karbeah J, Tessier KM, Neerland C, Stoll K, Hardeman RR and Vedam S | 2022 | The Impact of Culturally-Centered Care on Peripartum Experiences of Autonomy and Respect in Community Birth Centers: A Comparative Study | Mixed methods | BIPOC | Patient Care | 1 | 1 | 1 | 1 |
| Bogdan-Lovis E, Zhuang J, Goldbort J, Shareef S, Bresnahan M, Kelly-Blake K and Elam K | 2022 | Do Black birthing persons prefer a Black health care provider during birth? Race concordance in birth | Quantitative | Black/African American | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Bonnevie E, Barth C, May J, Carey T, Knell SB, Wartella E and Smyser J | 2022 | Growing and Glowing: A Digital Media Campaign to Increase Access to Pregnancy-Related Health Information for Black Women During the COVID-19 Pandemic | Quantitative | Black/African American | Technical | 1 | 1 | 0 | 1 |
| Canty L | 2022 | The lived experience of severe maternal morbidity among Black women | Quantitative | Black/African American | Pt-provider relationship | 1 | 1 | 0 | 0 |
| Chinkam S, Ibrahim BB, Diaz B, Steer-Massaro C, Kennedy HP and Shorten A | 2022 | Learning from women: Improving experiences of respectful maternity care during unplanned caesarean birth for women with diverse ethnicity and racial backgrounds | Quantitative | Postpartum people | Patient Care | 1 | 1 | 1 | 1 |
| Collins C, Bai R, Brown P, Bronson CL and Farmer C | 2022 | Black women’s experiences with professional accompaniment at prenatal appointments | Quantitative | Black/African American | Pt-provider communication | 1 | 1 | 1 | 0 |
| Dailey RK, Peoples A, Zhang L, Dove-Medows E, Price M, Misra DP and Giurgescu C | 2022 | Assessing Perception of Prenatal Care Quality Among Black Women in the United States | Quantitative | Black/African American | Patient Care | 1 | 1 | 1 | 0 |
| Davis B, Baggett KM, Patterson AL, Feil EG, Landry SH and Leve C | 2022 | Power and Efficacy of Maternal Voice in Neonatal Intensive Care Units: Implicit Bias and Family-Centered Care | Community-based participatory approach | Black/African American | Pt-provider communication | 1 | 1 | 0 | 1 |
| Gomez-Roas MV, Davis KM, Leziak K, Jackson J, Williams BR, Feinglass JM, Grobman WA and Yee LM | 2022 | Postpartum during a pandemic: Challenges of low-income individuals with healthcare interactions during COVID-19 | Quantitative | Low income | Pt-provider relationship | 1 | 1 | 0 | 0 |
| Harrell T, Howell EA, Balbierz A, Guel L, Pena J, Janevic T and Gorbenko K | 2022 | Improving Postpartum Care: Identifying Opportunities to Reduce Postpartum Emergency Room Visits Among Publicly-Insured Women of Color | Qualitative | BIPOC | Pt-provider communication | 1 | 1 | 1 | 1 |
| McKenzie LB, Keim SA and Klebanoff MA | 2022 | Risk Perceptions about Cannabis Use and Receipt of Health-Related Information during Pregnancy | Literature Search | Pregnant people | Information | 1 | 1 | 0 | 1 |
| Miller MW and Baker S | 2022 | African American Women’s Experiences with Birth After a Prior Cesarean Section | Community-based participatory approach | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Mirabal-Beltran R, Hawks-Cuellar M, Powell TW and Strobino DM | 2022 | Women’s perceptions of provider communication on birth options after cesarean: A qualitative study | Mixed methods | Pregnant people | Pt-provider communication | 1 | 1 | 0 | 1 |
| Okpa A, Buxton M and O’Neill M | 2022 | Association Between Provider-Patient Racial Concordance and the Maternal Health Experience During Pregnancy | Literature Search | Pregnant people | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Prater C, Cohen L, Chau E, Carter EB, Kuebee B, Tepe M and Keegan M | 2022 | Perceived Discrimination During Prenatal Care at a Community Health Center | Literature Search | Pregnant people | Pt-provider relationship | 1 | 1 | 1 | 1 |
| Stanhope KK and Kramer MR | 2022 | Variation in the Content of Postpartum Visits by Maternal Race/Ethnicity, Preconception, and Pregnancy-Related Cardiovascular Disease Risk, PRAMS, 2016-2017 | Quantitative | Postpartum people | Technical | 1 | 1 | 1 | 0 |
| Thomas SP | 2022 | Street-Race in Reproductive Health: A Qualitative Study of the Pregnancy and Birthing Experiences among Black and Afro-Latina Women in South Florida | Community-based participatory approach | Black/African American | Patient Care | 1 | 1 | 1 | 1 |
| Waldron MK | 2022 | Parent Protector: Perceptions of NICU-to-Home Transition Readiness for NICU Parents of Black Preterm Infant | Literature Search | Black/African American | Patient Care | 1 | 1 | 1 | 0 |
| Witt RE, Colvin BN, Lenze SN, Forbes ES, Parker MGK, Hwang SS, Rogers CE and Colson ER | 2022 | Lived experiences of stress of Black and Hispanic mothers during hospitalization of preterm infants in neonatal intensive care units | Quantitative | Black/African American | Patient Care | 1 | 1 | 1 | 0 |
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Environmental Protection Agency’s Great Lakes Restoration Initiative through the Minnesota Department of Health [grant number GL00E01161].
