Abstract
Introduction/Objectives:
With the emergence of COVID-19, the transition from in-person care to widespread use of telehealth raised many well-described challenges for primary care providers (PCP). The purpose of this study was to improve understanding of how this increased use of telehealth impacted PCPs in positive ways, and specifically focus on any “silver linings” of using telehealth.
Methods:
We interviewed PCPs working at a large Midwestern academic medical center between June and July 2020 and asked for perspectives about the use of telehealth during the pandemic. Verbatim transcripts were coded and analyzed using deductive dominant thematic analysis that allowed for categorization of data and identification of emergent themes.
Results:
PCPs noted 3 main benefits of using telehealth: (1) demonstrated remote care was feasible, (2) patients expressed gratitude; and (3) payers fully reimbursed for telehealth visits. PCPs also described “silver linings” they perceived for patients: (1) easier access to care, (2) more convenient follow-up care, and (3) ability to get quick specialty referrals.
Conclusions:
Study participants offered encouraging feedback regarding the potential for telehealth to offer a convenient and patient-centric alternative to in-person care. As a healthcare delivery mode, telehealth can remove personal and social barriers to care for many patients, but reimbursement parity and more evidence is needed to inform best practices for ongoing telehealth use in primary care. With the continuing use of telehealth, it will be important to monitor health outcomes as well as consider how these modalities may need to be adapted to mitigate potential care disparities.
Introduction
The use of telehealth expanded rapidly in primary care as providers pivoted their work to address patient care needs due to the emergence of Coronavirus Disease 2019 (COVID-19).1,2 Defined as “the use of electronic information and communication technologies to provide and support healthcare,” 3 telehealth has enabled the continued delivery of important clinical services while keeping aligned with public health guidance to minimize disease transmission of the highly contagious COVID-19. Of note, the surge in telehealth visits that started at the beginning of the pandemic has persisted, with current usage in primary care still 35 times higher than before the start of the pandemic, and as much as 38 times greater in other medical specialties. 4
Although the increased availability of telehealth visits has expanded access to care for many patients and has helped improve patient-provider communication,5,6 this rapid transition from face-to-face to virtual care delivery has also introduced major challenges for primary care providers (PCPs) such as workflow disruptions, staffing changes, and difficulties adapting to the use of new technologies. 7 At the same time, these challenges have been linked to lower work engagement, increased risks for physician burnout, and compromised patient care.8,9
While many studies have examined the increased use of telehealth since the emergence of COVID-19, much of this prior work has focused on the challenges and negative impacts of this change. In this analysis, we considered PCPs’ perspectives about the positive aspects, or “silver linings,” of this transition.
Methods
Study Sample and Data Collection
As previously described, 10 the study sample included 20 PCPs from the Department of Family and Community Medicine and the Division of General Internal Medicine and Geriatrics who were affiliated with a large Midwestern academic medical center (AMC). Between June and July 2020, we conducted one-on-one video interviews with PCPs. Following a semi-structured interview guide, we asked PCPs about the early impacts of COVID-19 on their work, including what they perceived were benefits of delivering primary care via telehealth. Interviews lasted an average of 35 min and were audio-recorded, transcribed verbatim, and de-identified prior to analysis. All interviewees provided verbal informed consent prior to their participation. The study was approved by the authors’ Institutional Review Board.
Data Analysis
We analyzed interview transcripts using a deductive dominant thematic approach to allow for data to be categorized based on general themes derived from the interview guide, as well as to allow for identification of emergent themes. This approach also enabled us to compare themes across interviews and to characterize the ways in which PCPs described any “silver linings” that accompanied their transitions to using telehealth for primary care provision.
Using this approach, 2 members of the research team first reviewed 2 of the transcripts and developed an initial coding dictionary based on the questions asked in the semi-structured interview guide and additional topics that emerged during interviews. The codebook was then refined, and the remaining transcripts were coded. Frequent meetings of the research team ensured consistency of coding across transcripts. For the results we present here, we focused on the “benefits of telehealth” code. All data analysis processes were supported by the ATLAS.ti (version 8.4.4) qualitative data analysis software.
Results
Study Participants
Characteristics of the 20 PCPs who participated in our study are presented in Table 1. On average, interviewees had 16 years of primary care experience (range = 3-41 years).
Interviewee Characteristics.

Perceived “Silver Linings” for Primary Care Physicians
Across interviews, PCPs’ comments about the rapid increase in use of telehealth because of the emergence of COVID-19 were largely positive, and they specifically mentioned 3 “silver linings” for themselves that they associated with this experience: (1) remote care delivery was feasible; (2) patients expressed gratitude; and (3) payers adapted insurance coverage to fully reimburse for telehealth. We describe these themes in further detail next, and present additional verbatim quotations in Table 2.
“Silver Linings” of Telehealth for Primary Care Physicians.
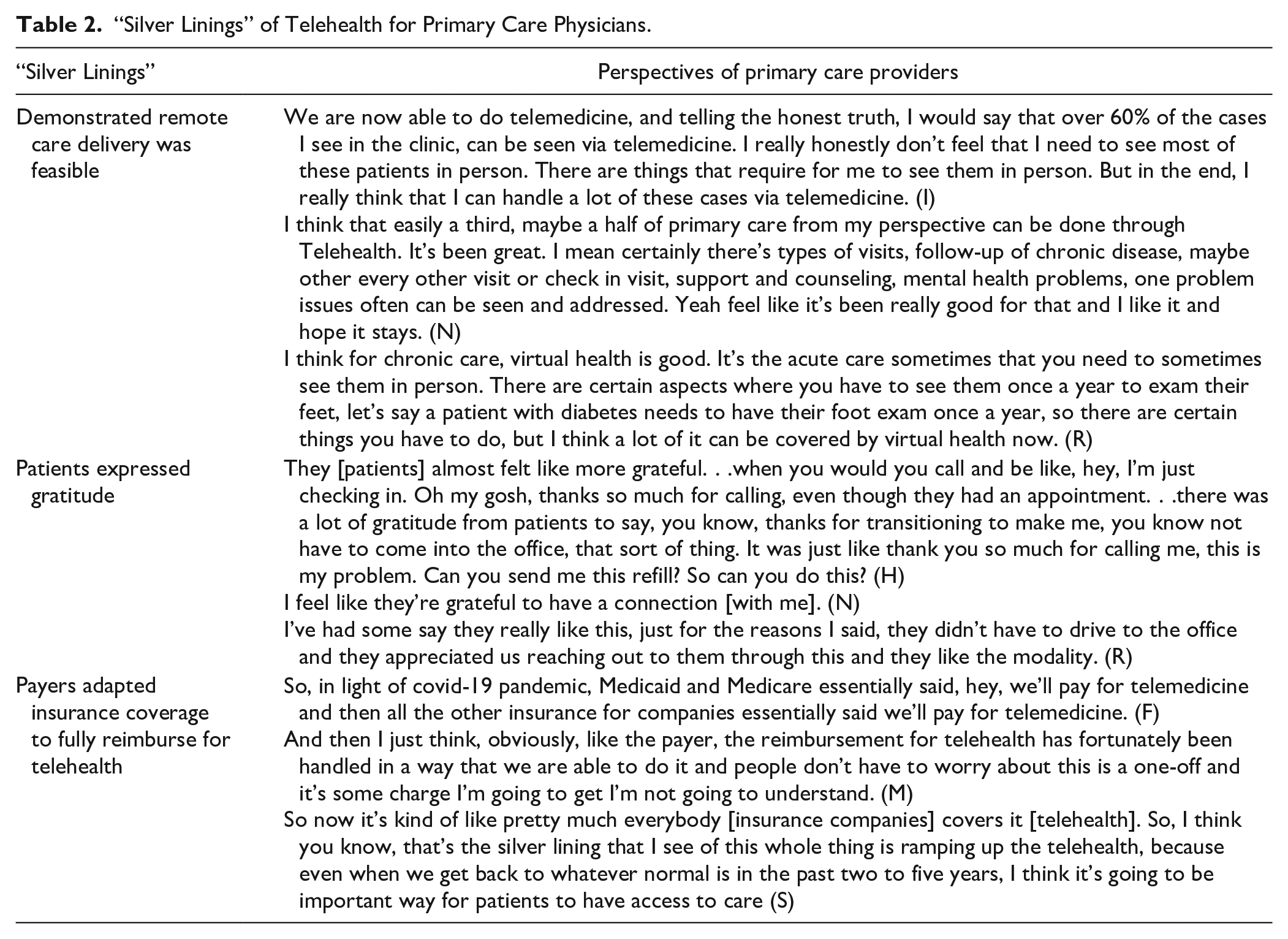
First, interviewees emphasized that their experience during the pandemic convinced them and others that delivering medical care remotely was feasible. A physician noted, “As much as patients demand and want to be seen in person, as much as we need to see them in person, just as much, if not more of the time, at least in what work I do as a family medicine physician [it] can be done virtually.” This perspective about feasibility was particularly evident when interviewees described providing care for existing patients. As another physician explained, “If you have a patient who you see on a regular basis and you’re adjusting medications or things like that, I think phone check in. I think trying to help them understand what is safe and reasonable to be managed via telephone versus what is to be managed with a face-to-face, even if it’s be [sic] a video. Because I think a lot [of] chronic care can be provided via video.”
PCPs also commented about how it was a “silver lining” to hear and see how grateful their patients were to receive virtual care during the pandemic. One physician reflected, “I think patients generally have been very thankful that we’re able to offer any kind of care in any modality through this whole thing. And, I feel like a lot of our patients worry a lot about our safety and making sure that we’re healthy. Some of them have expressed a lot of relief that I can still see them.” Another physician echoed this sentiment, noting, “Everyone’s been grateful I’m saying and some had actual needs that they weren’t addressing or didn’t think to address.”
Third, interviewees reported being pleased that the rapid increase in the use of telehealth in response to the COVID-19 pandemic had resulted in improved insurance coverage for virtual visits. As 1 physician explained: “I think that actually forcing payers to come up with solutions that kind of adapt to our real world and our technologies probably wouldn’t have happened without the pandemic. And so as a result like we have these novel tools and we are more able to use them. I think that the telehealth visits are our silver linings because we have had all these tools available to us but we didn’t use them because there wasn’t an impetus and then we didn’t use them because there was no billing strategy.” Another PCP similarly commented, “One thing that’s good is like at least temporarily, Medicare and other insurers are covering video visits better now. So, my hope is that they’ll just continue to do that and recognize that it’s really a valuable tool for patients and providers.”
Perceived “Silver Linings” for Patients
PCPs also provided examples of the “silver linings” they perceived patients experienced that resulted from the delivery of care via telehealth: (1) it was easier for patients with certain medical conditions to receive care; (2) it provided patients with a convenient follow-up care modality; and (3) it enabled patients to get quick specialty referrals and visits. Below we describe these themes in greater detail, and additional verbatim quotations are presented in Table 3.
Physicians’ Perceptions of “Silver Linings” of Telehealth for Primary Care Patients.

Physicians’ responses suggested they perceived a benefit for patients around the ability for patients with certain medical conditions to receive care via telehealth instead of needing to come in person to the office. As 1 physician reflected, this could be perceived as a “silver lining” for a number of different types of patients:
Patients who, you know, let’s say they simply have medical comorbidities that make it much more challenging for them to come to the clinic. So, we’re talking about patients with you know, agoraphobia, patients with PTSD [Posttraumatic stress disorder], patients with depression, whatever the case maybe. Or even patients who are you know, morbidly obese where just getting up and out of bed is too painful for them. Now we can at least deliver some care to those patients.
Another physician described additional types of patients who seemed to benefit: “I think it has improved access for some people, mobility issues, folks that just like really are, can’t stand going to the doctor’s office, folks that live really far away.”
A second “silver lining” PCPs perceived for patients involved the convenience and flexibility of telehealth and how it appeared to improve patients’ abilities to adhere to follow-up appointment schedules. One physician shared, “Some patients are more likely. . . so if I’m doing some medication changes and I say hey, you know, I’d like to talk to you in two weeks. Maybe I hear from them maybe not. With televideo, they’re like, ‘Sure, I can do it.’ I can do a 5- to 10-minute quick call to just review and make sure everything is okay.” Another physician explained, “Patients are more likely to actually make the appointment, and more frequently, because they don’t waste an hour of their time traveling to wherever and taking the time to find parking, making arrangements to have babysitters.” A third PCP reflected how this flexibility seemed appreciated by patients: “Patients are like getting a little bit more choice in how they can communicate. Like being able to say to a patient, ‘Do you want to see me? I want to see you back in three months. You want to do it by video or phone, or do you want to come to the office?’ Like that’s a choice we’ve never given them. The fact that they feel like they have some say in how they experience their care.”
Finally, PCPs suggested that telehealth provided a “silver lining” for patients when it enabled quick referrals for specialty care, timely consults, and less time to get appointments. One physician explained, “Patients love it [fast e-consults]. So, I’m talking to a patient and I would say hey, we need an appointment for this. They don’t have to wait for six months for a dermatologist to see them or a nephrologist. I’ll just say e-consult this case within two days. We are probably going to get an answer actually 24 hours, not even two days.” Another physician reflected: “Doing a quick telemedicine visit is now more accepted from everybody. If I need to squeeze someone in, adding a video visit is easier.”
Discussion
Our study of the experiences of PCPs using telehealth during the first 4 months of the COVID-19 pandemic (i.e., when restrictions on in-person visits were in effect and then lifted), suggested that physicians perceived multiple “silver linings” related to the increased use of telehealth. Specifically, they highlighted benefits for their own practices such as learning that telehealth was feasible, hearing appreciation from their patients for telehealth visits, and receiving appropriate reimbursement for those visits. They also perceived benefits for their patients and reported that telehealth appeared to enhance care access for patients with chronic conditions and disabilities, made it easier for patients to have virtual follow-up visits with care team members, and enabled expedited patient referrals to specialists. With respect to the broader literature on telehealth expansion during the pandemic, 11 our findings document the unforeseen advantages of utilizing telehealth in routine primary care. Further, our study answers the call for more research examining the contextual factors surrounding telehealth applications. 12 Specifically, our qualitative findings demonstrate how the rapid transition to telehealth enabled PCPs to engage with their patients to address their clinical and non-clinical needs during the pandemic. However, despite these benefits, adaptations to existing workflows are likely necessary to sustain telehealth as an equitable primary care modality.13,14
Given the time frame of our study, telehealth usage was rapidly increasing, and during the declared public health emergency, government agencies and payers allowed video and audio-only visits to be covered at equal parity to in-person visits.15,16 PCPs in our study indicated that reimbursement parity was important in promoting telehealth use, similar to what has been reported in previous research, 17 and also noted that sustaining this parity could allow for the continued use of telehealth modalities. PCPs commented that they were hopeful that payers would continue with this reimbursement approach so that telehealth options could remain available to patients who preferred to receive care remotely as well as supporting ongoing efforts to reduce the spread of COVID-19. Furthermore, establishing reimbursement mechanisms that allow for video and audio-only visit parity both now and in the future can help to address certain aspects of the “digital divide”13,17,18 that exists between patients who do and do not have access to broadband internet.
Our findings also suggest that telehealth provides a convenient alternative to in-person visits, consistent with the results of other studies. 19 Previously identified clinical 20 and non-clinical factors that can prevent patients from adhering to in-person visits such as not having transportation, childcare, or the ability to take time off from work21-23 were identified by our study participants as having been reduced by the increased availability of telehealth after the emergence of COVID-19. To the extent that telehealth may be able to address some of these personal and social barriers to care, PCPs can reasonably expect to see decreases in no-show rates and in patient cancelations of scheduled appointments.24,25 Moreover, PCPs in our study indicated they were accepting of telehealth and would consider using virtual modalities to provide ongoing follow-up care for patients who either preferred to use telehealth or had conditions that limited their ability to have an in-person visit. This is consistent with previous studies that found physicians and patients had favorable attitudes toward telehealth, 26 and that patients were satisfied with the quality of telehealth they received. 27
Our research may also have important implications for designing telehealth options in primary care that better support patient-centered care. By removing some of the burdens to accessing in-person care (e.g., transportation), telehealth reportedly enabled PCPs in our study to simplify follow-up care for patients who did not require in-person visits. As the use of telehealth continues, more research will be necessary to understand how PCPs and staff members can effectively integrate telehealth with in-person visits and further characterize the workflows and processes that can facilitate a safe and patient-centered care experience that involves this care modality. 28 For instance, patients may need to better understand how sensitive information can be securely shared with their providers, as well as any potential risks of using video platforms to receive primary care. It will also be important to understand explicitly how telehealth can expedite e-consults and specialty referrals without compromising patient safety. This information may shed light on the specific needs of those PCPs who will continue to use telehealth to conduct e-consults as well as refer patients needing follow-up care.
These study findings may have important practical implications for PCPs who are currently using or planning to use telehealth both during this COVID-19 pandemic and into the future. Given that the physicians in our study reported positive impacts of their use of telehealth, primary care practices may benefit from conducting hybrid video and in-person visits to reduce barriers to patient follow-up and to accommodate patients’ preferences for specific visit modalities. However, future protocols for telehealth use will also need to take into consideration the technology access and capabilities of patients as not all individuals have the option to have a video visit with their doctor.29,30 Providers and practices may be able to implement simple screening questions to ensure patients have access to the technology and connectivity that they need and reduce the inequities that could result. As the pandemic continues, it will clearly be important continue to monitor and study the use and impacts of telehealth as we build evidence about this care modality and its integration into primary care practice.
Limitations
Our study has several limitations. First, this study was conducted at a single healthcare system in which physicians had access to a shared electronic medical record (EMR). It is possible that some of the benefits noted in this study, including feasibly scheduling follow-up visits and specialty care, may not generalize to free-standing primary care clinics that do not share a common EMR with neighboring healthcare organizations nor have existing partnerships with clinical specialties (e.g., oncology). Nonetheless, given our saturation with respect to the themes we present and the consistency of our findings in the context of previous research, we are confident that the results we report can be applied to help facilitate the use of telehealth for both patients and providers. Second, given the challenges of the COVID-19 pandemic, we were unable to conduct interviews with patients to understand their experiences with telehealth and to see if their perspectives corroborated with those reported by the PCPs who participated. Of note, a recent nationally representative survey study of U.S. adults (n = 2080) found that two-thirds of respondents preferred at least some video visits in the future, 31 suggesting our findings may indeed align with patient perspectives. Third, all of the PCPs we interviewed reported very little prior experience with telehealth prior to the emergence of COVID-19. It is possible that the perspectives of providers with previous experience may have contributed additional information and insights to this study. Finally, in the context of the ongoing pandemic, it is likely that physicians’ perspectives about telehealth will evolve, highlighting the importance of ongoing research in this area.
Conclusions
We found that in spite of the rapidity with which physicians had to embrace and increase the use of telehealth with the emergence of COVID-19, the impacts of this experience also included “silver linings” for the providers who participated in our study. These PCPs noted benefits to both themselves and their patients that included convenience, responsiveness, and new options for follow-up care. From a policy standpoint, ongoing reimbursement parity for telehealth will be essential to support primary care’s capacity to deliver preventive and follow-up services via telehealth and ensure equitable enhance access to this care.
Footnotes
Acknowledgements
The authors would like to thank the physicians who participated in this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Publication of this article was funded by Rush University’s College of Health Science Open Access Fund.
Research Ethics and Patient Consent
All interviewees provided verbal informed consent prior to their participation. The study was reviewed by the Ohio State University Behavioral Sciences Institutional Review Board and approved as exempt.
