Abstract
Keywords
Introduction
Breast cancer is the second leading cause of cancer deaths among women. 1 Breast density (BD), which is the “relative amount of radiopaque epithelial and stromal tissue elements compared with the amount of radiolucent fatty elements seen at mammography,” 2 is an established breast cancer risk factor.2-7 Besides increasing cancer risk, high BD may mask lesions on mammography, decreasing its sensitivity as a screening tool.8,9 BD is classified according to the Breast Imaging Reporting and Data System (BI-RADS) developed by the American College of Radiology. BI-RADS has 4 BD categories—from least to most dense: (a) the breasts are almost entirely fatty, (b) there are scattered areas of fibroglandular density, (c) the breasts are heterogeneously dense, which may obscure small masses, and (d) the breasts are extremely dense, which lowers the sensitivity of mammography. 2 The categories are often dichotomized: a and b considered “nondense,” and c and d considered “dense.” 2
In 2009, Connecticut became the first state to pass legislation requiring patients with dense breasts on mammograms be notified. The goal was to increase awareness and improve decision making regarding supplemental breast ultrasound and magnetic resonance imaging (MRI). 10 However, while BD legislation has been passed in at least 25 other US states as of April 2016 (California in April 2013), it is unclear how notification affects breast cancer detection and patient morbidity. Since 43% of US women 40 to 74 years old have dense breasts, such legislation could have substantial public health impact. 11
Only a few studies have examined changing clinical practices after BD legislation.12,13 Such information may influence guidelines and determine whether California legislation will continue beyond 2019, the date for its repeal unless it is extended. Thus, this study’s purpose was to examine the impact of the California BD notification legislation on rates of screening mammography and MRI, focusing on the 2 years before and 2 years after BD legislation. The authors hypothesized that the postlegislation screening MRI rate would increase from the prelegislation rate.
Methods
Study Setting and Population
This retrospective cohort study analyzed women aged 40 to 74 years enrolled in Kaiser Permanente Northern California (KPNC) in 2011-2015. KPNC is an integrated health care system serving 3.9 million enrollees that reflects the region’s underlying population, although it slightly underrepresents socioeconomic extremes. Study eligibility criteria included 2 years of continuous KPNC enrollment without more than two 45-day gaps in membership. Women with a double mastectomy before the screening mammogram or MRI were excluded. These criteria were chosen because of the recommended breast cancer screening age range at KPNC, and are similar to criteria for Healthcare Effectiveness Data and Information Set (HEDIS) measures. The study was approved by the KPNC Institutional Review Board in December 2015 (approval number CN-15-2492-H). Informed consent and Privacy Rule authorization requirements were waived.
Databases
Information was collected from The Permanente Medical Group (TPMG) Breast Cancer Tracking System (BCTS) and patient medical records. Collected information included KPNC facility where the screening mammogram (hereafter referred to as mammogram) or screening MRI (hereafter referred to as MRI) was performed, patient age at end of each 2-year period, body mass index (BMI) closest to end of each 2-year period, race/ethnicity, neighborhood median family income (using census block address) at end of each 2-year period, double mastectomy and breast cancer history prior to mammogram or MRI, and BD (BI-RADS fifth edition). Screening mammograms were designated with Current Procedural Terminology (CPT) code 77057. Screening MRIs utilized codes 77058 and 77059, and were classified as “screening” by BCTS clinicians. For mastectomy history, International Classification of Diseases, 9th revision (ICD-9) codes for bilateral mastectomy procedure (85.42, 85.44, 85.46, 85.48) and 2 unilateral mastectomy procedures done on different days (85.41, 85.43, 85.45, 85.47) as well as CPT codes (19180, 19182, 19200, 19220, 19240, 19303-7) were used.
Screening Rates
For most of 2011-2015, screening mammography in KPNC was recommended every 1 to 2 years for women aged 40 to 74 years, while screening MRI was recommended as an adjunct for those at high genetic risk. After August 2014, KPNC guidelines were modified to mammography every 1 to 2 years for women aged 50 to 74 years, while decision making between the patient and physician was recommended for women aged 40 to 49 years. In these guidelines, BD category did not affect screening recommendations. To calculate changes in screening practices, a 2-year prelegislation period from April 2011 to March 2013 was compared with the 2-year postlegislation period from April 2013 to March 2015. Women were only counted once for each 2-year period.
Statistical Methods
Crude rates of mammography and MRI were compared in pre- and post-legislation periods using chi-square tests. To determine screening trends after adjusting for race, age, BMI, neighborhood median income, medical facility, and cancer history, Poisson regression estimates were used to calculate relative risk comparing mammography and MRI rates in both periods. A separate Poisson model with an interaction term for legislation period and age was included to determine age group–specific rate change from pre- to postlegislation period. Nesting of patients within medical facilities was accounted for using a generalized estimating equation with a robust sandwich covariance estimator. Bivariate comparisons of BD frequencies by demographic characteristics were analyzed using chi-square tests. To isolate the effect of legislation on the likelihood of supplemental MRI, multivariable logistic regression was used to estimate an odds ratio of MRI within 9 months of mammogram in the prelegislation period versus the postlegislation period. When BD data became available during the post-legislation period, multivariable logistic regression was used to estimate an odds ratio of MRI within 9 months of mammogram among each BI-RADS BD category. The logistic regression model similarly adjusted for race, age, BMI, neighborhood median income, medical facility, and cancer history, and used a robust sandwich covariance estimator to allow for repeated subjects within medical facilities. Statistical analyses were done using SAS 9.3 (SAS Institute, Cary, NC). An alpha of 0.05 was considered statistically significant.
Results
Mammogram and MRI Screening Rates
The number of eligible women increased from the prelegislation period (April 2011 to March 2013) to the postlegislation period (April 2013 to March 2015), from 614 663 to 631 478. The number of women with a mammogram who met inclusion criteria decreased in the postlegislation period, from 506 400 to 487 365 while the number of women with an MRI increased from 743 to 872.
Table 1 shows total and demographic-specific counts and crude rates of mammograms and MRIs. There was a decrease in mammogram rate from 82.4% (95% CI 82.3%-82.5%) prelegislation to 77.2% (95% CI 77.1%-77.3%) postlegislation (P < 0.001). This decreasing trend was statistically significant for all race, age, BMI, and neighborhood median income–specific rates, except women aged 70 to 74 years (significant increase, P < 0.001). During the same period, the rate of MRI increased from 12.1 per 10 000 women (95% CI 11.2-13.0) to 13.8 per 10 000 women (95% CI 12.9-14.7) (P = 0.008). There were statistically significant increases in MRI rates for Asian and white women, women aged 42 to 44 years, women with normal BMI, and women living in neighborhoods with a median family income of $60 000 to <$90 000 or more than $120 000.
Total and demographic-specific counts and crude rates of screening mammograms and MRIs.

Abbreviations: MRI, magnetic resonance imaging; Pre, prelegislation (April 2011 to March 2013); Post, postlegislation (April 2013 to March 2015); BMI, body mass index.
Chi-square test to compare pre- and post-legislation rates. Values in boldface indicate statistical significance.
Median income = census block median family income.
Table 2 lists relative risks (RRs) comparing mammogram and MRI rates in the postlegislation period relative to the prelegislation period. After adjustment for race/ethnicity, age, BMI, neighborhood median income, medical facility, and cancer history, there was a relative 6.6% decrease (RR 0.934, CI 0.92-0.95) in the mammogram rate and a relative 16% increase (RR 1.16, CI 1.07-1.25) in the MRI rate (Ps < 0.001). Age group specific change in mammography rates, determined using an interaction term between legislative period and age, varied substantially; there was a modest, if any, reduction in rates among women aged 55 years and older. In contrast, the increase in MRI screening rates postlegislation appeared to be greatest among women in their early 40s.
Multivariable Relative Risks Comparing Postlegislation With Prelegislation Screening Mammogram and MRI a Rates.
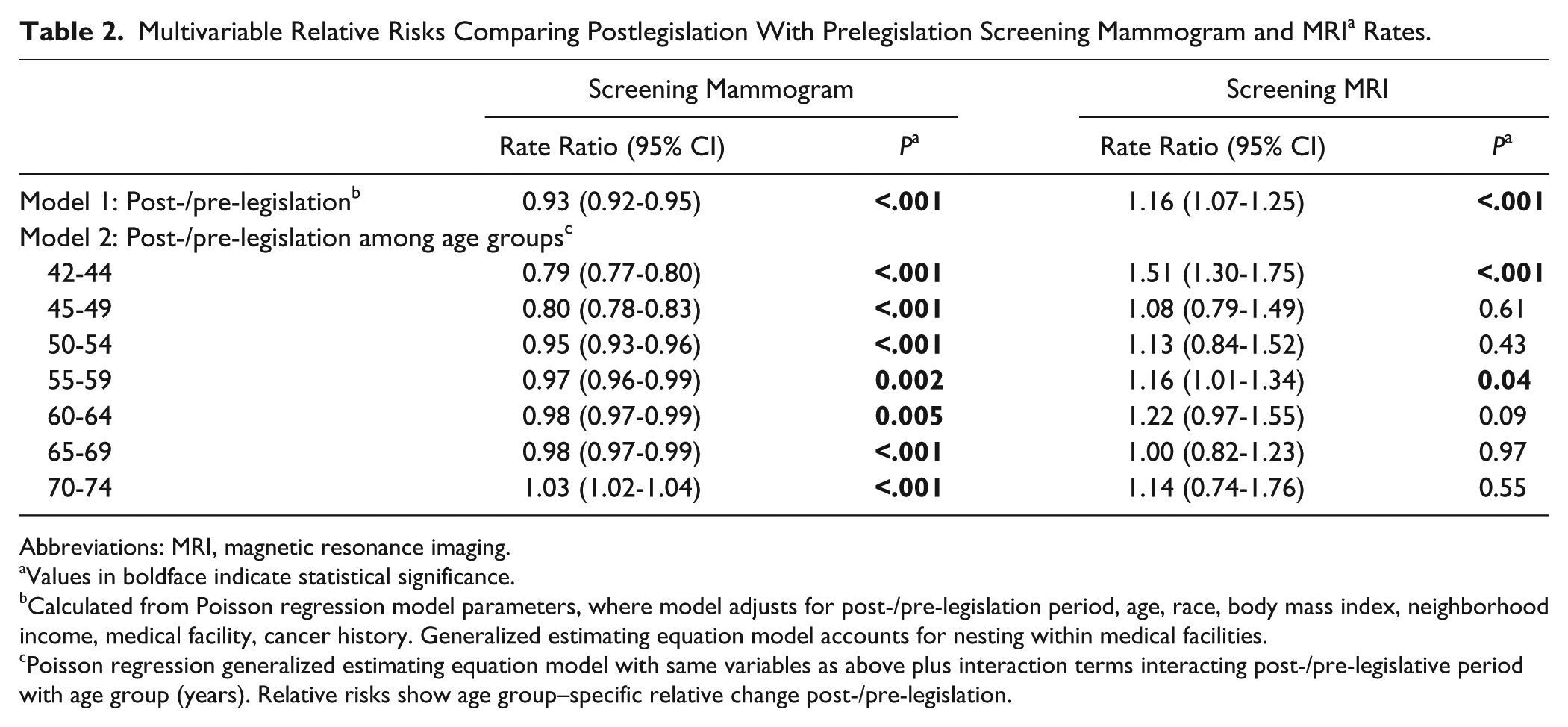
Abbreviations: MRI, magnetic resonance imaging.
Values in boldface indicate statistical significance.
Calculated from Poisson regression model parameters, where model adjusts for post-/pre-legislation period, age, race, body mass index, neighborhood income, medical facility, cancer history. Generalized estimating equation model accounts for nesting within medical facilities.
Poisson regression generalized estimating equation model with same variables as above plus interaction terms interacting post-/pre-legislative period with age group (years). Relative risks show age group–specific relative change post-/pre-legislation.
Breast Density Patterns
Figure 1a-d shows, respectively, frequencies of BD categories overall, by race/ethnicity, by age, and by neighborhood median income. When BD categories were collapsed into 2 groups, the overall distribution became 58% not dense and 42% dense. Categorical frequencies stratified by age and BMI (not shown) revealed inverse relationships between each variable with BD, whereas BD frequencies stratified by neighborhood median income revealed a direct relationship. BD patterns were significantly different across race, age, BMI, and neighborhood median income (Ps < 0.001).

Distribution of breast density categories (April 2013 to March 2015): (a) overall; (b) by race/ethnicity; (c) by age; and (d) Neighborhood median income. Heterogen. dense, heterogenously dense; Native Am, Native American.
MRI Within 9 Months of Screening Mammogram
Table 3 shows select adjusted odds ratios (ORs) for having MRI within 9 months of mammogram. There was a 46% increase (OR 1.46, CI 1.30-1.64) in the odds of MRI within 9 months of mammogram pre- to postlegislation. ORs decreased with increasing age and BMI, increased with increasing neighborhood median income, and were lower in non-white women. In the postlegislation period, women who had dense breasts had 2.08 times (CI 1.769-2.46) or 2.77 times (CI 1.93-3.97) (category c or d, respectively) the odds of having a MRI within 9 months of a mammogram compared with women in category b (also shown in Figure 2).
Selected Odds Ratios Indicating Odds of Having Screening MRI Within 9 Months of Screening Mammogram.

Abbreviations: MRI, magnetic resonance imaging; BMI, body mass index.
Logistic regression model adjusting for age, race, BMI, neighborhood median income, medical facility, and cancer history. Odds ratio estimates for medical facility and cancer history not shown.
Logistic regression model adjusting for breast density, age, race, BMI, neighborhood median income, medical facility, cancer history. Generalized estimating equation model allowed for nesting of individuals within medical facility. Odds ratio estimates for medical facility and cancer history not shown.
Values in boldface indicate statistical significance.
Median income = census block median family income.

Adjusted odds ratiosa and confidence bounds for having screening magnetic resonance imaging (MRI) within 9 months of screening mammogram in the postlegislative period. Ref, reference.
Discussion
To our knowledge, this is the first study to quantitatively examine how breast cancer screening practices have changed since the California BD notification legislation went into effect. KPNC screening mammography rates were consistently higher than average commercial, Medicaid, and Medicare screening rates reported to HEDIS. 14 The study’s distribution of BD categories stratified by demographic variables resemble what has been reported for the US female population.11,15,16 In the 2 years after BD notification legislation went into effect, screening mammography decreased slightly, although this was largely limited to women younger than 50 years. In contrast, rates of MRIs appeared to increase for most age groups, but was greatest among the youngest women. Higher BD was associated with supplemental MRI, suggesting that observed increases in MRI screening rates could have been associated with BD legislation. Because we did not have prelegislation BD, we could not examine whether increases in screening MRIs from the pre- to post-legislation period were limited to women with dense breasts.
Other studies found increased supplementary screening subsequent to BD legislation. At a single community hospital in New Jersey, Sobotka and Hinrichs 12 found follow-up breast ultrasound utilization increased 176% to 336% over 1 year. Meanwhile, Mason et al 13 at Baylor University in Texas found a 23-fold increase in supplementary MRIs in the 2-year period after BD legislation went into effect. In contrast to these 2 facility-specific studies, our study encompassed an entire region of California served by a single health plan.
Our study had additional limitations. It was conducted in an insured population, and results may not be generalizable to other settings. The study was limited to a 4-year period based on available data, but this may have been too short a time period to expect substantial behavior change, especially since studies have demonstrated low awareness of BD legislation among both physicians and patients.4,17 Information on other predictors of screening (such as individual-level socioeconomic status, MRI access, and physician training) was unavailable. Technology updates and increased acceptability of screening MRI among physicians could contribute to increased screening MRI rates. There may have been misclassification of screening versus diagnostic imaging, which depends on the radiologist’s interpretation of provided clinical information. Lastly, while BI-RADS for BD is used routinely in clinical care, it relies on radiologists’ visual estimation and can be subjective. 18
An unexpected result was the decrease in KPNC screening mammography rates. While the age at initiation of breast cancer screening began shifting from age 40 to 50 years due to US Preventive Services Task Force (USPSTF) recommendations in 2009, 19 KPNC guidelines continued to recommend screening for women in their 40s until 2014. These recommendation changes may explain reduced screening mammography among women aged 40 to 49 years, but little if any decrease among women 50 years and older.
In their latest guidelines, the USPSTF and the National Comprehensive Cancer Network state there is insufficient evidence to establish screening recommendations for women with dense breasts.15,20 Although some studies have examined BD awareness and legislation,4,12,21 research about effects on clinical practice is limited. More studies based on clinical algorithms and cost-effectiveness analyses of supplemental screening methods are needed, so that evidence-based policies and recommendations can guide health providers as they counsel patients with dense breasts.
Footnotes
Acknowledgements
The authors would like to acknowledge the Kaiser Permanente Oakland Medical Center Internal Medicine Residency Program, University of California Berkeley School of Public Health Interdisciplinary Program, Kaiser Permanente’s Division of Research, TPMG BCTS, and specifically Dr Joan Lo, Dr Thomas Baudendistel, Dr Anke Hemmerling, Dr Phuoc Le, Debbie Postlethwaite, Mary Anne Armstrong, Mary Callahan, Jane Bethard-Tracy, Dr Sherry Butler, and Dr Veronica Shim.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the KPNC Community Benefit Program and its KPNC Graduate Medical Education Research funds.
