Abstract
Introduction
Over the past few decades, the dramatic increase in the use of medical imaging tests that employ ionizing radiation in the United States has led to growing sensitization to patient safety, which has resulted in efforts to reduce radiation exposure during these tests, and consideration of alternatives to their use whenever possible.
1
There is substantial uncertainty concerning the actual risks associated with medical imaging radiation (MIR).2-8 In this context, the mass media has devoted increasing coverage to patient safety in the context of tests that use MIR. For example, in January 2014, the Op-Ed section of
While the media focus on MIR has been predominantly negative, 10 it is not clear how this dialogue has affected the general population. Patients’ concerns about the health risks of MIR could increase patient anxiety and impede quality of life, and could impede imaging adherence, given that high cancer worries are related to general distress and can lead to avoidance of imaging, such as cancer screening. 11 An accurate assessment of population worry about the harms of MIR will assist in efforts to anticipate and understand patients’ attitudes toward medical imaging, and improve risk communication and shared decision making regarding medical imaging among referring primary care physicians, radiologists as well as patients. Furthermore, understanding patient characteristics associated with high levels of worry about MIR will help referring physicians anticipate and address such concerns in specific patient subpopulations.
Accordingly, Aim I is to determine rates of worry about MIR in the US general population and to compare these with rates of worry about other common environmental hazards. Aim II is to determine significant correlates of MIR worry, including demographics, medical and psychological factors, health information-seeking and physician trust, as well as cancer fatalism—the belief that cancer is inevitable.
Methods
Study Design and Participants
The Health Information National Trends Survey 12 (HINTS, 2013) version 4, cycle 2 is a nationally representative survey that was conducted by the National Cancer Institute (NCI) via mail between October 2012 and January 2013. Of 12 057 invitees, 3630 participants returned completed surveys. The total sample consisted of 3532 individuals for whom complete data on the outcome of interest (worry about MIR) was available.
Measures
Worry About MIR
The study dependent variable was a self-report item measuring the amount of worry about the health harms of MIR. Other items assessed worry regarding the health harms of chemicals in water, chemicals in food, outdoor air pollution, chemicals in household products, indoor air contaminants, chemicals in personal products, and radiation from cell phones.
Demographic Factors
Gender, age, race/ethnicity, educational attainment, annual income, whether the participant was born in the United States, subjective health status, health insurance status, as well as personal cancer history, and general anxiety 13 were assessed.
Health Information-Seeking and Physician Trust
Participants were asked whether they sought health information, how much trust they would have in cancer information from a doctor, and finally, the level of attention paid to information about cancer from 7 different media sources (eg, print newspapers, the Internet, radio, and local television news; all 7 combined into a summary score, 0-100 range).
Cancer Fatalism
Consistent with prior work, 3 questions (eg, “There’s not much you can do to lower your chances of getting cancer”) were combined to create a continuous summary score (0-100) measure of cancer fatalism. 14
The specific wording of all measures reported in this study appears at: http://hints.cancer.gov/docs/HINTS_4_Cycle_2_English.pdf.
Analytic Strategy
All analyses were conducted in R version 3.1.015 using the “survey” package,16,17 version 3.29-5 to account for the HINTS complex sampling design. The HINTS full-sample weight was applied to all analyses to yield nationally representative point estimates. Standard errors were calculated using jackknife repeated replications with the set of replicate weights included with the HINTS data.
First, covariates of interest were examined using descriptive statistics (unweighted frequencies, weighted percentages, means with 95% confidence intervals [CIs]). Next, logistic regression analysis was conducted and presented as unadjusted (univariable) and adjusted (multivariable) odds ratios with 95% CIs. For the logistic regression analysis, the dependent variable (MIR worry) was dichotomized (not at all/a little vs some/a lot) and elevated MIR worry was modeled. Omnibus
Results
Characteristics of the Sample
Table 1 reports the descriptive characteristics of the analyzed HINTS sample. The sample was balanced in terms of gender, predominantly aged 18 to 64 years, 33% non-white, and highly diverse in educational attainment and income. Most were US born (86%), had health insurance (82%), and reported subjective health that was good or better than good (84%).
Descriptive Characteristics of the Sample (N = 3532). a
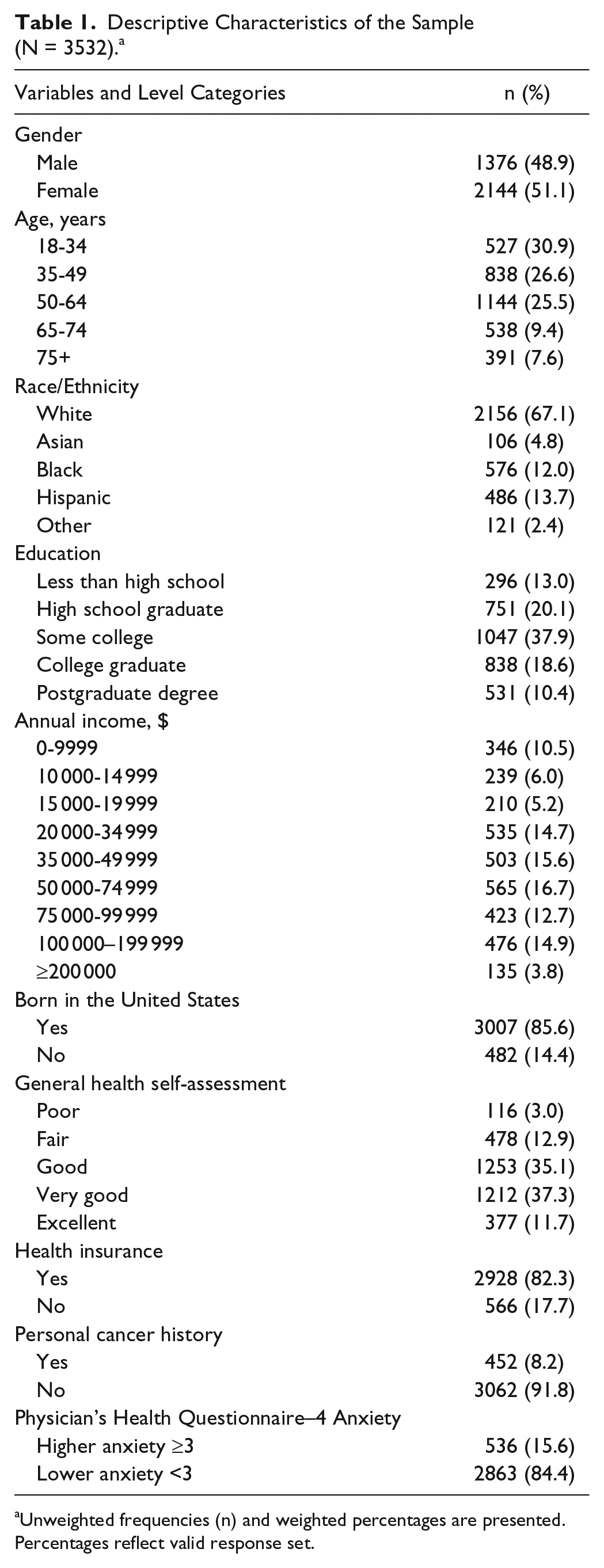
Unweighted frequencies (n) and weighted percentages are presented. Percentages reflect valid response set.
Aim I: Rates and Levels of Worry About MIR in the General Population
About two-thirds of the sample (65.5%, 95% CI = 62.9% to 68.1%) reported worry regarding the health effects of radiation from medical imaging. Specifically, 31.1% (95% CI = 28.6% to 34.0%) reported a little worry, 21.9% (95% CI = 19.1% to 24.7%) reported some worry, and 12.3% (95% CI = 10.6% to 14.0%) reported a lot of worry (see Figure 1). Rates of worry about the health effects for other hazards were higher than for MIR.

Self-reported worry about harm to health from medical imaging radiation compared with other hazards (N = 3532). Participants’ estimates of worry for a series of hazards. Responses represent portion of sample who reported no worry or any other degree of worry (a little worry, some worry, or a lot of worry).
Aim II: Correlates of MIR Worry
Univariable and multivariable logistic regressions examining associations between elevated MIR worry and demographics, health information-seeking, and cancer fatalism variables are presented in Table 2. At the univariable level, higher worry about MIR was significantly associated with female gender, racial/ethnic minority status, having an annual income <$50 000, lower education, and being foreign born. Additionally, higher worry about MIR was significantly associated with poorer subjective health, having a personal history of cancer, and elevated general anxiety. Worry about MIR was not associated with age or health insurance status. In terms of health information-seeking, MIR worry was not associated with seeking health information in the past year but was significantly associated with being less trusting of cancer information communicated by doctors, and with paying more attention to cancer information from popular media. The univariable relation between MIR worry and cancer fatalism was not statistically significant.
Univariable and Multivariable Logistic Regressions Examining Correlates of Worry a About Harm From MIR (N = 3532).

Abbreviations: MIR, medical imaging radiation; OR, odds ratio; CI, confidence interval; PHQ, Physician’s Health Questionnaire.
Worry item was dichotomized as
In the first multivariable model, the adjusted odds ratios for each demographic variable are adjusted for all of the other demographic variables.
In the second multivariable model, the adjusted odds ratios for each information-seeking behavior variable are adjusted for all of the demographic variables and for the other information-seeking behavior variables.
In the third multivariable model, the adjusted odds ratio for the cancer fatalism variable is adjusted for all of the demographic variables.
Near-significance at
The multivariable analyses yielded similar findings with a few exceptions. The first model, demographics, indicated higher rates of MIR worry among females, racial/ethnic minorities, less educated individuals, foreign-born Americans, those who self-report poorer health, and those with a personal history of cancer. In the second model, information-seeking controlling for demographics, MIR worry was significantly associated with being less trusting of cancer information communicated by doctors and with paying more attention to cancer information from various forms of popular media. Cancer fatalism was still not statistically significant after controlling for demographics (third model).
Discussion
An accurate assessment of public concerns about the harms of MIR will aid referring physicians’ efforts to anticipate and understand patient responses to medical imaging. These data suggest that a large proportion of individuals (65%) in the United States have salient concerns about exposure to radiation from medical tests, a fact that mirrors an expanding dialogue about the delivery of radiation via medical imaging in the medical community and the news media.10,18-20 We found higher levels of MIR worry in this large, nationally representative US sample than in research on smaller samples, which found 12% in those about to undergo imaging in 2011, 18 and 37% in a shopping mall in 2000, were concerned about MIR. 19
Significant correlates of MIR worry indicate 4 population subgroups where MIR worry is most prevalent. These groups include the underserved, those with health challenges, those who are less trusting of cancer information from their physicians, and those more attentive to cancer topics in the media. First, worry about MIR was found to be higher in non-whites, those with lower educational attainment, and Americans who were born outside the United States. Health literacy is lower in underserved populations, 21 and new health innovations are absorbed more slowly in underserved populations. 22 Lower health literacy and poorer access to health innovations could dictate that underserved populations have less access to high-quality information about the benefits as well as the potential harms of medical imaging. Furthermore, lower income was associated with significantly higher MIR worry in the univariable model only, likely due to a high degree of overlap with lower education, which remained significantly linked to MIR worry in both analyses. The analysis also suggests that women endorse higher levels of worry than men.
A second important study finding is that higher MIR worry is associated with both a personal history of cancer and poorer self-reported health. Indeed, those who have serious health issues such as cancer 20 may be imaged more frequently and be aware of potential risks associated with repeated imaging. As such, it is possible that 2 separate subgroups exist—where low socioeconomic status and low knowledge dictate higher MIR worry, and also where those with health concerns (and potentially higher knowledge) may also have higher MIR worry. Additionally, individuals who have been previously diagnosed with cancer may be more likely to worry about cancer in general. In a study examining cancer patient perspectives on MIR, patients felt the need for more information about the rationales for the recommendation of one test over another and for test intervals, and more explicit information about communication between the radiologist and the provider who ordered the test. 20 Primary care patients with poorer health may also be more frequently imaged, and worry more about health, in general. General anxiety was not related to MIR worry in the multivariable analyses, indicating that specific concerns about MIR were distinct from general anxiety. However, worry about MIR would be expected to be high in those with anxious symptoms.
Finally, physician trust and cancer information-seeking patterns were also associated with MIR worry. Those with lower trust in cancer information provided by their doctors reported higher MIR worry. Additionally, participants who reported paying a lot of attention to a variety of common sources of cancer information reported higher levels of MIR worry, suggesting that individuals who are likely to worry about MIR are also likely to be receptive to mass media coverage of cancer issues. 23 There are substantial opportunities for medical imaging experts such as radiologists and medical physics professionals to better communicate with the news media23-25 regarding the actual risks associated with MIR, as well as the social factors that may amplify or minimize perceived risks associated with MIR. 23 Future research should examine whether improved primary care communication about these topics may both increase physician trust and reduce MIR worry.
Study limitations include the modest study response rate, as well as cross-sectional nature of the data, which does not allow for examination of cause and effect relationships between the covariates and worry about MIR. Additionally, our assessment of MIR worry was based on one item, and with this dataset we could not examine specific health concerns such as cancer worry, which is common in the population.11,26,27 Full consideration of myriad public concerns about medical imaging, including both shorter and longer term effects, and other environmental exposures is necessary to fully address their health and policy implications.28-30
Key points and study contributions are as follows. Worry about MIR is relatively high in the US population, and highest in the underserved, those with health challenges, those who are less trusting of cancer information from their physicians, and those more attentive to cancer topics in the media. This study contributes to the literature in that it documents prevalence and patterns of MIR in a large, nationally representative population. Public perspectives regarding the risks and benefits of imaging tests that deliver ionizing radiation can help shape the dialogue regarding shared decision making about recommended tests,31,32 ultimately enhancing patient engagement, and shared decision making, regarding medical imaging among referring physicians and their patients.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
