Abstract
Introduction
The prevalence of Autism spectrum disorders (ASDs) has increased substantially, and the overall prevalence estimates vary from 0.5% to 2.24%.1-3 With this increasing prevalence, the onus of supporting families managing challenging behaviors associated with ASDs often falls on general practitioners (GPs), who are required to develop health care plans using a multimodal approaches such as behavior management strategies and psychopharmacology.4-7 This has resulted in an increase in the use of psychotropic medications in children with ASDs globally.8-10
Longitudinal population study for a period of 4 years from 2009 to 2012, based on dispensing data for Australian government–subsidized antidepressant, antipsychotic, and attention deficit/hyperactivity disorder medications, showed an overall increase of 16.1%, 22.7%, and 26.1%, respectively, from the baseline. 11 This assumes importance because GPs are the primary pediatric providers in Australia, and their workload for children with emotional problems has increased 3-fold over the past decade. 12 Studies have also demonstrated that primary care physicians contribute to the increase in psychotropic prescriptions. 13
It is also argued that some children receive inappropriate prescriptions of these medications, particularly in the younger age group. 14 Since little published literature exist on understanding of Australian GPs regarding psychopharmacology use in children with ASDs, we report a qualitative analysis of comments on the perceptions of GPs regarding psychopharmacology use in children in the state of New South Wales, Australia.
Methods
An exploratory cross-sectional postal survey was conducted with GPs in New South Wales after ethical approval from the Northern Sydney Central Coast Area Health Service Human Research Ethics Committee (HREC-1102-076 M). A concurrent mixed methods embedded approach was used to design the questionnaire (supplementary file, available online at http://jpc.sagepub.com/content/by/supplemental-data), which included both close- and open-ended questions to gather qualitative and quantitative data. 15 The 3 sections of the questionnaire included the following: Section A collected demographic information. Section B was designed to measure the “relevance” (how often do GPs see children with ASDs?) and “perceptions” regarding services, psychopharmacology, educational needs, and referral choices. Section C contained 14 true/false type knowledge questions. A total of 1185 questionnaires were posted using a simple random strategy from a statewide directory of GPs. We have reported the questionnaire development and findings of relevance, knowledge, and broad educational needs of GPs regarding ASDs previously.16,17 In this report, we elaborate the analysis of descriptive responses to 3 questions asked in the questionnaire:
Data Analysis
All the qualitative responses were analyzed using thematic coding by the first author, after exploration of word frequencies helped in emergence of themes using NVIVO qualitative software. 18 Data were coded reading “line by line,” and exploration of the data was done to visualize if there were any pattern of themes according to the demographic characteristics. Quantifying of qualitative data was done; first, by converting the themes into numbers by “dichotomizing” or “categorizing” (eg, by converting GP responses into binary variables “0” and “1,” ie, those who expressed the theme vs those who did not), and second, by counting the number of participants expressing a particular theme. The quantified qualitative data were analyzed using chi-square analysis for trend. These strategies are well used with mixed method research designs.19,20 Statistical analyses were performed using MedCalc for Windows, version 15.11.4 (MedCalc Software, Ostend, Belgium).
Results
The demographic characteristics of respondents are shown in Table 1. Female GPs and Australian medical graduates, with an interest in child and/or mental health were overrepresented (Table 1). A total of 191 (16.1%) questionnaires were returned and 177 responded to the question on prescribing medications; 123 (72%) reported prescribing these medications for children, even when a similar proportion raised concerns regarding these medications in children. Risperidone (n = 18) and selective serotonin reuptake inhibitors (SSRIs; n = 13) were most often prescribed. GPs reporting more children with ASDs in their care, more new diagnosis of ASDs every year, and those with greater confidence in developmental disorders, prescribed more medications (χ2 =13.8, 15.4, and 28.1 with P = .03, .0001, and .0001, respectively). GPs reporting more concerns about psychotropic medications prescribed less (χ2 = 6.05, P = .01; Table 2).
Characteristics of Respondents as Compared With Characteristics of General Practitioners in New South Wales and Australia.
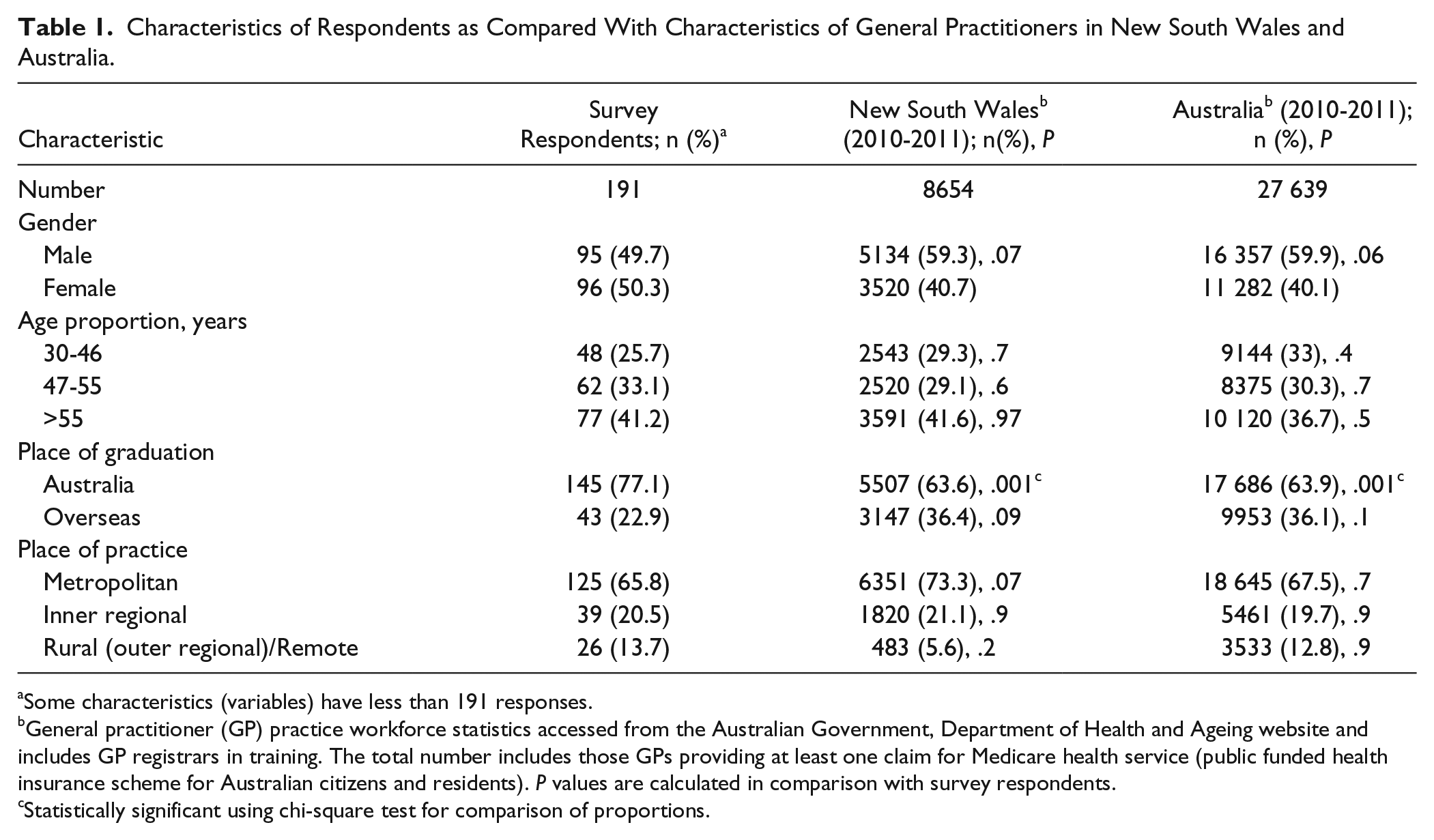
Some characteristics (variables) have less than 191 responses.
General practitioner (GP) practice workforce statistics accessed from the Australian Government, Department of Health and Ageing website and includes GP registrars in training. The total number includes those GPs providing at least one claim for Medicare health service (public funded health insurance scheme for Australian citizens and residents). P values are calculated in comparison with survey respondents.
Statistically significant using chi-square test for comparison of proportions.
Characteristics of General Practitioners Associated With Their Self- Reported Prescribing Practices
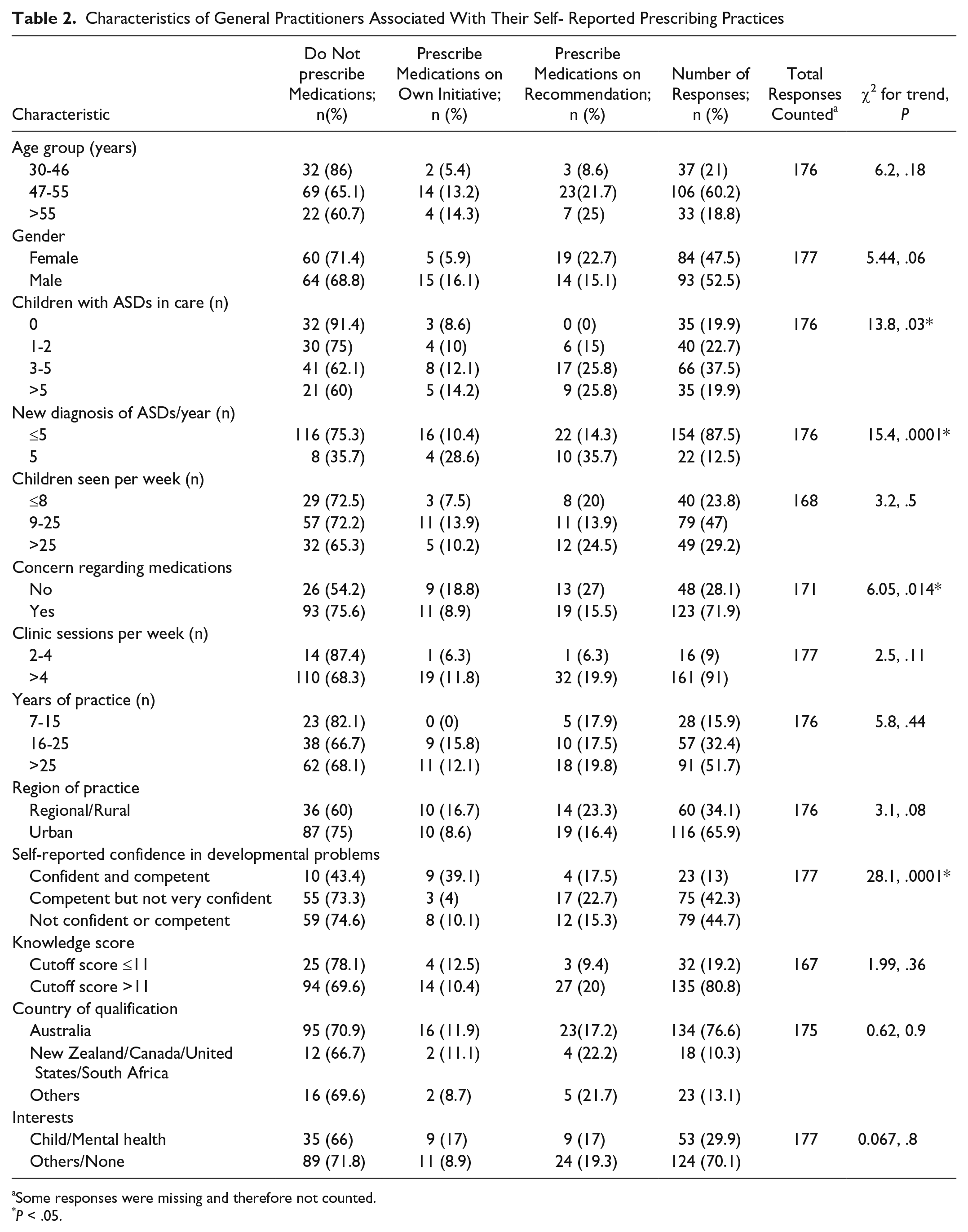
Some responses were missing and therefore not counted.
P < .05.
The main themes that emerged consistently irrespective of demographic or other variables such as exposure to children with ASDs are highlighted below (italicized sentences or words below are GPs’ written comments on the questionnaires).
Concern Regarding Safety
This was the most common theme reported by 82 (47%) GPs. GPs reported refraining from a broad brush approach to using medications in children with ASDs by stating each patient has to be assessed on an individual basis using a risk benefit analysis. They raised concerns that metabolic & weight effects and long term problems like diabetes result in side effects outweighing benefits. They expressed worry about drug effects on immature brain, overprescribing for children with behavioural disorders, compliance issues, experimenting by older adolescents, dependency on the medications to keep them [patients] manageable by carers, sedative effects impair[ing] academic function, and off-label prescribing.
GPs also expressed practical and logistic concerns such as [the] patient did not want to have regular review by specialists if scripts were given by GP. They also raised concerns about inappropriate prescriptions and safety under age 10.
They highlighted the need [for] updates regarding evidence and were happy to prescribe as long as there was good evidence of effectiveness.
The proportion of GPs who reported the subthemes of “side effects” and “evidence for effectiveness” were 66(37.3%), and 16(9%) respectively.
Lack of Experience and Knowledge
Twenty-five (14.1%) GPs raised this theme. This theme acknowledged GPs own limitations of expertise and judgement required for using these major drugs. GPs recognized that these medications for children need specialised knowledge and were explicit to acknowledge that they have little experience of prescribing these medications for autism, because they are not familiar with effects of these drugs in kids.
Specific issues raised by GPs regarding knowledge of medications included when to cease medications, various drug interactions, length of time of use, unsure of doses, how to assess effectiveness, not comfortable prescribing such medications in children. GPs laid importance on whether [a] comprehensive assessment has occurred [or not]. Some GPs expressed their personal beliefs such as most [children with ASD] don’t need medications except fish oil.
Taking Responsibility for the Medications
Eighteen (10.2%) GPs reported this theme. GPs reported that they (didn’t) feel confident and will prescribe only when the [child is] under [a] paediatrician. They don’t want to be responsible for prescribing those [psychotropic medications] and prefer to leave to [a] specialist, particularly if I [the GP] trusted the specialist. They preferred to provide only follow up scripts.
Adjuvant to Behavior Management
Ten (5.6%) GPs reported this theme. GPs highlighted that they prefer[ed] behavioural modification methods in first instance. They acknowledged that there may be other conditions [comorbidities] present with autism which may make their use helpful. GPs expressed that medications if well supervised, and the correct diagnosis (indication) is made the benefit of these drugs is great.
Discussion
We have highlighted that respondent GPs in New South Wales have awareness of the contemporary issues for psychotropic medications in children with ASDs, but lack experience and knowledge regarding these medications. This is an important finding, as in near future GPs in Australia are more likely to be involved in managing medications in children with ASDs due to increased workload of children with emotional problems. 12
In the current study, GPs were comfortable to prescribe when the child was managed by a trusted specialist. This finding is supported by an earlier qualitative study of 35 GPs, where the local specialists were highly valued as a source of authoritative and unbiased information. 21
The finding of unwillingness of GPs to be responsible for managing medications in children with ASDs in our study is supported by a study of 28 GPs in Queensland regarding their attitudes for management of attention deficit/hyperactivity disorder. They expressed a largely supportive role for themselves, working in close liaison with the specialist services. 22
The concern of GPs regarding “overprescribing,” particularly in the context of diagnostic uncertainty is debated in the literature.23-25 As raised by GPs the potential of abuse of psychotropic medications is a well-known and has been shown in a large population study with adolescents done in Missouri, North America. 26 The issue of prescribing of psychotropic agents by GPs despite being “not comfortable” and concern regarding side-effects of medications such as extrapyramidal symptoms and metabolic abnormalities particularly in children are also well known.8,27,28
Implications of the Study
The implication of this study is that although GPs have a good understanding of these medications, they are in general uncomfortable managing these medications in children with ASDs. Thus, “integrated models of care” are needed to improve coordination between and access to services. 29 In North America, medical homes provide access to family-centered primary care needs of children with ASDs. 30 The applicability of this model in Australian context remains an open question due to differences in population and its distribution, manpower resources, health care systems, funding mechanisms and organization of allied health services. 31 The current study suggests that a proportion of GPs in New South Wales have an interest in autism, and there could be merit in formalized training courses for them. These GPs could potentially provide a “beacon” practice with an expanded clinical capacity to deliver health care for children with ASDs, and provide partnerships links with other general practices, community services, and tertiary autism units. A similar model has been developed for providing primary health care services to refugee populations in Australia. 32 Further qualitative study with GPs using focus groups or interviews should explore the reasons of reluctance to prescribe despite appearing to have a good understanding of psychotropic prescribing, and the possibilities of beacon GP practices for children with ASDs. Further research should also focus on the multidisciplinary design and evaluation of collaborative models of service delivery for GPs.
Strengths and Limitations
We acknowledge the limited generalisability of findings due to response rate biases. We have attempted to offset this by focusing on qualitative analysis of GP responses. The respondent GPs were from rural, regional, and metropolitan areas, which increase the transferability of qualitative findings.As the characteristics of non-respondents were not available it was not possible to compare them with respondents. The low response rates for GPs remain a major challenge for conducting primary health care research in Australia. 33 The findings from the current study, although limited in scope, make an argument for larger funded studies.
Since this was an analysis of written comments on questionnaires, the responses were brief, and more elaborate qualitative data is achieved by in-depth-interviews and focus groups. The data on characteristics of GPs are based on self-report and not measured objectively.
Conclusions
Respondent GPs in New South Wales, Australia, demonstrated good understanding of the issues surrounding use of psychopharmacology in children with ASDs. This pilot study argues for large scale studies for greater understanding in collaborative approaches for supporting GPs in psychotropic prescribing for children with ASD’s, as well as further exploration of possibility of “beacon” general practices for children with ASDs.
Footnotes
Acknowledgements
The authors acknowledge the help of Dr. Carolyn Kefford, Prof. Simon Willcock, and Dr. Helen Wilkinson for setting up the GP survey, and all GPs for responding to the survey.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
