Abstract
Health care services that increase costs but fail to improve health are of low value. Limiting low-value services has potential to decrease health care expenditures by eliminating waste. We examined the opinions of Continuing Medical Education attendees about the “Choosing Wisely” campaign and decreasing use of potentially unnecessary services of low value. We compared our attendees’ responses to those of participants who completed a survey a year earlier. Respondents acknowledged waste of resources as a common and serious problem and noted frequent opportunities to address low-value services with their patients. They also reported limited ability to successfully reduce unnecessary services in daily clinical care. Lack of familiarity with “Choosing Wisely” may be related.
Introduction
The Choosing Wisely campaign seeks to “promote conversations” between physicians and patients so choices about testing and treatment are “1) supported by evidence, 2) not duplicative of other tests and procedures already received, 3) free from harm and 4) truly necessary.” 1 Limiting low-value services should decrease health care expenditures but also improve quality and, potentially, prevent harm.2-4 These concepts are gaining favor as more than 70 medical societies and organizations have now proposed their own “Top 5” lists. 1 Altogether, more than 300 tests and services have been identified as potential targets for practice improvement. As providers are key stakeholders in efforts to avoid low value services, we studied perceptions among clinicians attending a national Continuing Medical Education (CME) meeting.
Method
Subjects were the attendees at the “Meet the Preceptor” luncheon sessions occurring on 2 consecutive days at a March, 2015 medical education course in Scottsdale, Arizona. 5 We engaged “Choosing Wisely” session attendees by using an Audience Response System (ARS) and polled responses to questions during the presentation. Participation was voluntary and anonymous. This project was deemed exempt by our institutional review board.
During the presentation, we used items from the 2014 survey, “Unnecessary Tests and Procedures in the Health Care System: What Physicians Say about the Problem, the Causes, and the Solutions.” 6 That opinion poll was sponsored by the American Board of Internal Medicine (ABIM), through their Robert Woods Johnson Foundation (RWJF) grant. It had been conducted by telephone and collected responses of 600 physicians, both primary care providers and specialists. Its purpose was to “gauge physicians’ attitudes toward the problem of unnecessary tests and procedures in the health care system, views on the causes of the problem, and their perspectives on various solutions.” 6
The ARS units collected attendees’ responses to questions posed during the presentation. Individual characteristics of respondents could not be captured for comparison. Data from responses were stored and aggregated. These were transferred for analyses performed using R version 3.1.2. We describe the data and compare them to the ABIM poll responses where applicable with Fisher’s exact test. An alpha of <.05 was set as the cutoff for significance.
Results
In all, 104 of 379 registered CME attendees selected “Choosing Wisely” as one of their sessions (27%). The majority of these providers were physicians (80/104; 77%) while the remainder were advance practice nurses. Most of these registered participants (75/104; 72%) identified themselves as providing primary care. Seventy-one of the registered participants (68%) came to their scheduled session and used the ARS (43 on Wednesday March 25, 2015 and 28 on Thursday March 26, 2015).
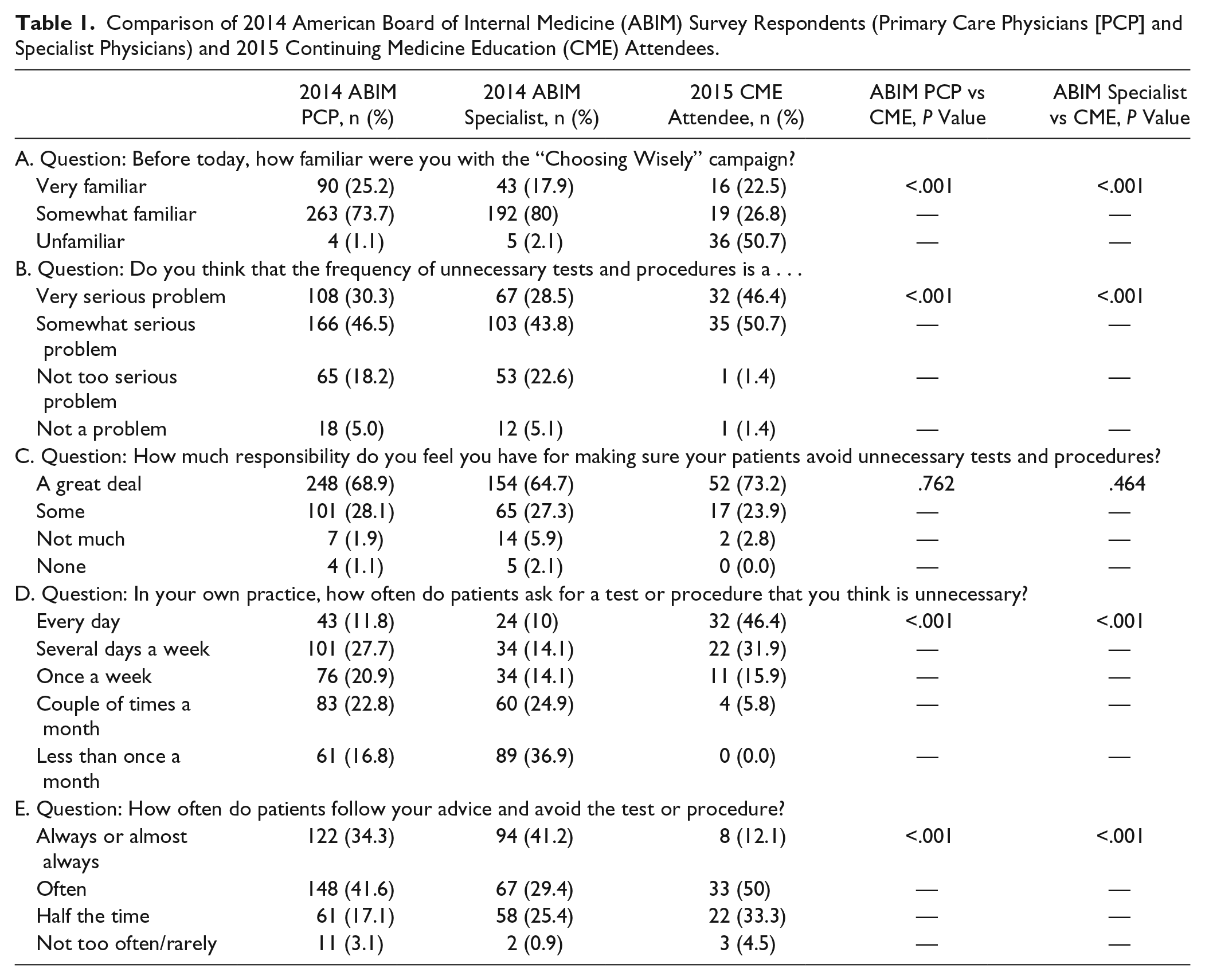
Participants were knowledgeable about health care spending in the United States. A majority could correctly identify the amount of overall spending and estimate the degree of wasteful services (35/67 [52%] and 43/70 [61%], respectively.) They were significantly less likely to report familiarity with the Choosing Wisely campaign, however, in comparison with the 2014 opinion poll participants. 50% of our attendees were “unfamiliar” with Choosing Wisely in comparison to 1% in the previous study 7 (Table 1) Our 2015 CME attendees were also significantly more likely to think that the frequency of unnecessary tests and procedures was a “very serious problem” than those from the ABIM survey. Most in each cohort felt a great deal of responsibility to make sure patients avoid unnecessary tests and procedures. Our providers reported substantially more frequent patient requests for testing that they believed to be unnecessary, with 46% noting this as a daily occurrence. Unfortunately, they felt that patients were less likely to follow their advice and avoid the test than had their 2014 survey counterparts. Twelve percent of our respondents felt that their patients “always or almost always” followed their advice in comparison with 34% of primary care physicians in the 2014 poll (P < .001). 6
Comparison of 2014 American Board of Internal Medicine (ABIM) Survey Respondents (Primary Care Physicians [PCP] and Specialist Physicians) and 2015 Continuing Medicine Education (CME) Attendees.
Discussion
Waste and its consequences threaten the stability of the US health care system and overall public health. More than quarter of health care spending—about $750 billion a year—is wasted by ordering tests and providing services that do not improve health outcomes for our patients. 7 Reducing waste is a substantial policy priority—the Choosing Wisely campaign is a well-known example demonstrating the widespread acknowledgement of this concern. 1
Providers at a 2015 CME course recognized overuse as a considerable problem in their practices and were knowledgeable about the unsustainable spending behaviors found in the US health care system. They perceived the issue of stewardship of resources as a serious one and felt patients requested these unnecessary services frequently. In many providers’ experiences, this occurs on a daily basis. Our participants were, overall, unfamiliar with the Choosing Wisely campaign, however. This may be a potential reason why they reported difficulty in convincing patients to follow their advice and avoid unnecessary services. The ABIM opinion poll reported that “physicians with exposure to the Choosing Wisely Campaign were 17 points more likely to have reduced the number of tests or procedures they have done in the last 12 months.” 6
Three primary care specialty societies were among the first to provide recommendations about services of low value (see Box 1). 1 It has been estimated that by limiting these nonrecommended activities in outpatient primary care practice, $5 billion in wasteful health care spending could be avoided annually. 8 The American Academy of Family Physicians, whose list has now grown to 15, reports that their members supported the initial “List of 5” for Family Medicine because of the “potential positive impact on quality and cost, and the ease with which the recommendations could be implemented.” 9
Primary Care “Top 5” Lists of Things Physicians and Patients Should Question

Change, unfortunately, may not come easily. A goal of the Choosing Wisely campaign’s was to simply “change the conversation,” 10 but now many of the included low value service items are transforming into measures of quality, using primarily claims data.11-13 For instance, the avoidance of imaging for patients with acute low back pain without alarm features is a well-establish metric of physician performance with the National Committee for Quality Assurance. 14 These measures will be of great importance as physician report cards and public reporting become common in value based contracting systems. 15
Health care spending rates could be substantially affected by limiting low-value services. There are ethical, professional, quality, and economic imperatives creating momentum toward practice improvement. 4 Physicians are frequently recognizing opportunities to address this issue with patients. Our participants report needing help implementing these ideals successfully, however. Future studies should illuminate barriers and facilitators of limiting low-value services in everyday clinical practice.
Footnotes
Acknowledgements
The authors appreciate the editorial comments provided by Dr Matthew Rank in preparation of this article. Data analyses were supported by Mayo Clinic Arizona.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
