Abstract
Introduction
Primary health care (PHC) systems play a crucial role in preventing disease and helping people to better manage their health in many countries. In Australia, PHC is acknowledged in the National Primary Health Care Strategic Framework. 1 Improving PHC and helping people “Better manage their care” are key goals of the Council of Australian Governments National Health Reform Agreement, 2011. 2
One of the aims of a consultation is to help patients better manage their own health. Consultations in the PHC settings differ from consultations in the hospital setting and so patient-reported outcome measures (PROMs) used in hospitals are not always transferrable. Several PROMs are used to assess the quality of PHC consultations one of which, patient enablement (hereafter enablement), has been found to be particularly useful. 3 Enablement can be defined as “an intervention by which the health care provider recognises, promotes and enhances a patient’s ability to manage their own health.”4(p1) Enablement is the result of individual empowerment 5 and involves building on a person’s strengths. 4 In 1997, Howie et al 6 used enablement as an outcome measure in a study designed to determine the quality of consultations in the general practice setting. Enablement is now recognized internationally as a valid measure of the quality of a consultation with a general practitioner (GP).7,8
Howie et al 9 developed and validated the Patient Enablement Instrument (PEI) 6 to better measure consultation quality in PHC. This instrument has been used to study patient enablement in PHC in a number of countries.8,10,11 The PEI is a 6-item instrument that rates patients’ ability to cope with life, to understand their illness, to cope with their illness, to keep themselves healthy, to be confident about their health, and to help themselves. 6
While the PEI has been used internationally to measure enablement, it appears the concept remains poorly understood in PHC. The PEI has only been used to determine enablement following GP consultations, and therefore its performance following consultations with other health professionals such as nurse practitioners is not known. We conducted a narrative, integrative review of the literature to determine what is known about enablement in the PHC setting.
The aim of the review was to summarize and synthesize the existing published literature concerning the concept of enablement and its practice in PHC. The 3 questions to be answered by the review were the following:
How is enablement conceptualized in PHC?
How is enablement practiced in PHC?
Which factors, if any, influence patient enablement in the PHC setting?
Review Design
An integrative review approach was chosen to allow for the incorporation of diverse research methodologies and varied views expressed about enablement by health care workers and patients within PHC. Whittemore and Knafl 12 suggest that, although this method does have limitations such as being open to reviewer bias, an integrative review can inform practice as long as a rigorous, transparent process is followed.
Search Methods
Health literature, published in English between 1997 and 2014, was searched. These dates were chosen to ensure the review encompassed the seminal work of Howie et al. 6
A rapid initial review of articles in CINAHL and Medline led to the development of the search string. This was then used to more comprehensively search Medline, CINAHL, Web of Science, and Informit. These databases were identified as key databases for medical, nursing and allied health research undertaken in the in PHC setting.
Title and abstract reviews were undertaken to determine if the articles appeared to be relevant to the review. Full text copies of relevant reviews were obtained and read, and the reference lists of those identified for inclusion were searched for additional relevant studies.
The search terms were Enablement OR “patient self-efficacy” OR “patient self-efficacy” OR “client self-efficacy” OR “client self-efficacy” OR “patient empowerment”) AND (“primary health care” OR “primary care” OR “general practice” OR “family practice” OR consultations OR appointments).
Articles were excluded if they were duplicates; concerned with the secondary or tertiary health care sectors; did not specifically deal with patient enablement, self-efficacy, or empowerment; or were focused on patients who were engaged with a number of specialist services as well as PHC. As this review forms part of a doctoral study, the initial decision about inclusion and exclusion of studies was done by the lead researcher. However, the studies were then presented to both supervisors (who had read the articles) and a robust discussion led to the final decision to include or exclude studies incorporated in this review.
Search Outcome
The search yielded 692 articles, 24 of which were included in the review (Figure 1). Of these, 3 used qualitative methods, 17 used quantitative methods, and 3 were review articles. Of the 17 quantitative studies, 1 was a randomized controlled trial (RCT) and 15 were observational studies. Of the latter, 7 were cross-sectional studies, 5 were surveys, 2 were observational studies, and 1 was a longitudinal study. Two studies were not described as using a mixed method approach, but claimed both qualitative and quantitative components.
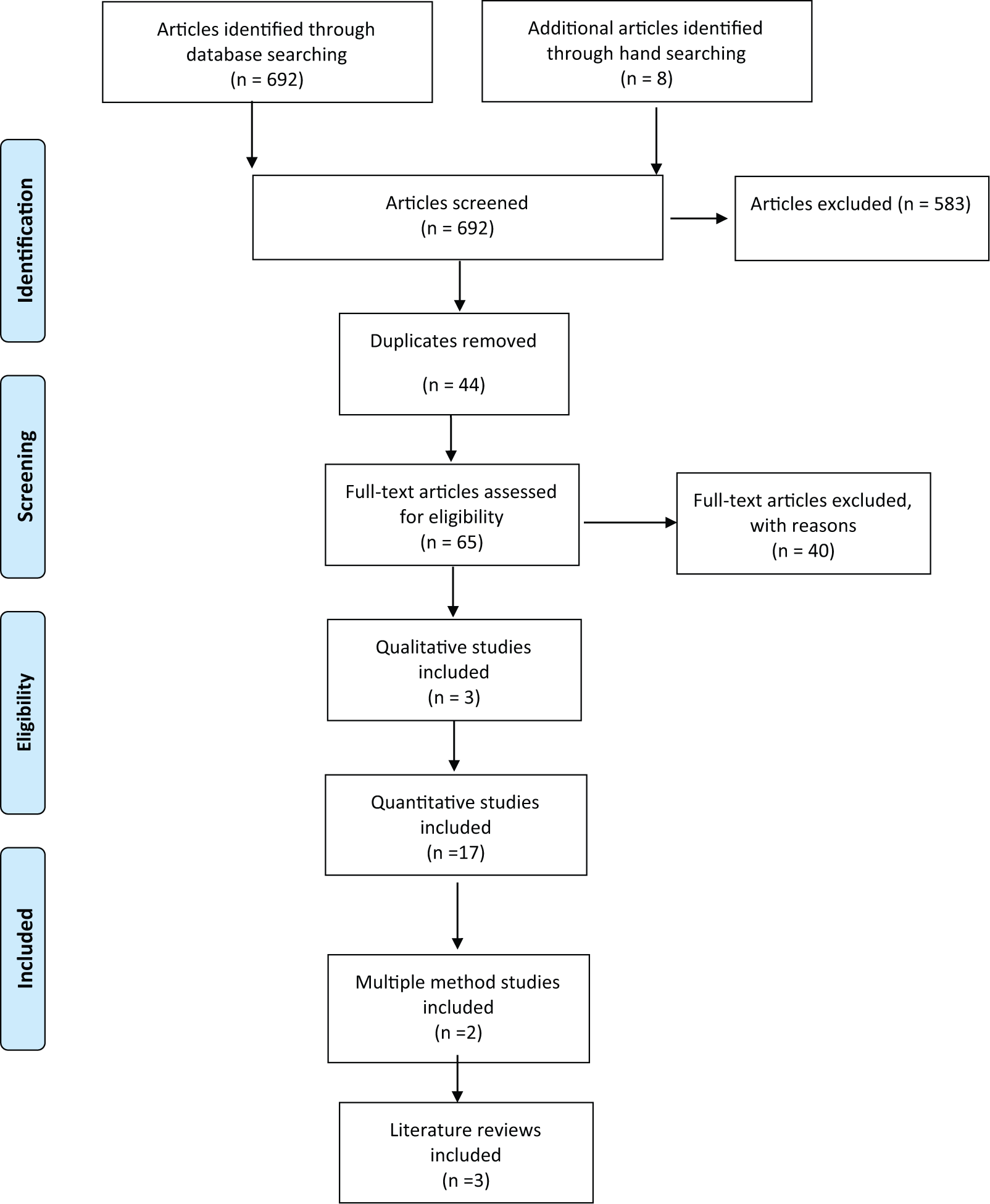
Literature search flow diagram. Based on: PRISMA 2009 flow diagram.
Quality Appraisal
The quality of all articles was assessed using the framework and guidelines devised by Caldwell et al. 13 This framework comprises overarching questions to determine quality in both qualitative and quantitative research, followed by specific questions for quantitative and qualitative studies, respectively.
Data Abstraction and Synthesis
A manual search was used to identify commonalities in the studies and these were categorized. Data reduction, data display, data comparison, and finally conclusion drawing and verification were undertaken as suggested by Whittemore and Knafl. 12
Results
Table 1 demonstrates the breadth of the literature found and the major findings of each study included in the review.
Summary of reviewed articles

Abbreviations: CARE Measure, Consultation and Relational Empathy Measure; CSQ, Consultation Satisfaction Questionnaire; GHQ, General Health Questionnaire; GP, general practitioner; PEI, Patient Enablement Instrument; PHC, primary health care.
The Concept of Enablement
In the quantitative literature enablement was conceptualized as a PROM used to indicate the quality of a consultation.3,5,8 The primary focus of the quantitative literature was on how to facilitate enablement rather than defining the concept. The 3 literature reviews4,29,30 linked enablement and empowerment. These reviews extrapolated the properties of empowerment to define the concept of enablement on the premise that enablement is the result of individual empowerment. 4
Findings of the 3 qualitative studies26-28 were similar to those of the quantitative studies. For example, Hudon et al 27 explored the enablement experience of patients with chronic illnesses and determined that enablement resulted from the process of developing a partnership; promoting interest in health care; starting from the patient’s situation; legitimizing the illness experience; acknowledging and promoting patient’s expertise and maintaining hope. The concept analysis literature review by Hudon et al 29 found that 67% of the articles included were derived from the nursing literature. Interestingly, the review failed to identify any of the work on enablement conducted in PHC. 29
As expected in patient-centered concepts one size does not fit all. The whole ethos of patient centeredness is one of uniqueness and diversity. 31 Enablement will be an individual experience; however, there are several elements of the PHC consultation that the research proposes directly influence enablement. Both the qualitative and quantitative studies used in this review explored the relationship between factors potentially associated with enablement, including communication, patient centeredness, consultation length, patient expectations/satisfaction, and other factors that affect patient enablement.
How Enablement Is Practiced
Empowerment was considered to be intrinsically linked with enablement with some authors suggesting the terms are interchangeable. 4 Four of the articles (2 quantitative studies,6,20 the concept analysis, 29 the systematic review of enablement measurement tools 4 ) focused specifically on the relationship between enablement and empowerment. The 2 qualitative studies surrounding patients’ perspectives of empowerment and enablement show that the patient behaviors required to achieve both empowerment and enablement were similar.15,27 These 2 studies identified attributes such as listening, explanations, and involvement in decisions.15,27
The literature focuses on empowerment through education, whereas some authors suggest that enablement is more comprehensive and also incorporates coping and managing illness. 6 The term self-efficacy is also used interchangeably with enablement, and is defined as the belief in one’s ability to act. 32 No qualitative research could be found that described patient’s perspectives of self-efficacy.
Factors Influencing Enablement
Communication and Patient-Centeredness
Twelve studies (7 quantitative5,10,11,16,19,20,24 2 qualitative,25,27 and 3 literature reviews4,29,30 examined enablement and communication, or patient-centered behaviors, including empathy 5 and involvement. 19 Overall, these behaviors improved enablement, but findings were not consistent across all studies. An early study of enablement 25 in general practice found no correlation between GPs’ patient-centered behaviors and enablement.
Empowerment and self-efficacy were, however, linked with communication15,33. Pawlikowska et al 24 attributed 33% of enablement scores to practitioners’ patient centeredness, but were unable to account for the source of the remaining 67% of the enablement score. This study also found that nonverbal communication and verbal dominance in consultations did not directly affect enablement. All 3 literature reviews linked communication and patient centeredness to both enablement and empowerment.4,29,30 Mercer at al 5 found a positive association between GP empathy and enablement. This study was limited by the fact that the GP practices studied may not have been representative due to the recruitment strategy used. A randomized controlled trial that examined enablement in asthma management reported that patients felt that flexibility and autonomy were positively correlated to enablement. 20 This is reiterated by Kurosawa et al, 11 who related coping and independence to enablement. 10
Length of Consultation
Length of consultation was positively correlated with enablement in 5 of 6 studies using the PEI.9-11,21,34 Mercer et al 14 tested whether facilitating GPs to increase the length of their consultations on an ad hoc basis by employing an additional part time GP and allowing 10 minutes in each hour as “free time” would increase in patient enablement. Results from this study showed an increase in PEI scores was achieved with a mean increase in consultation length of 2.5 minutes for the posttest group. 14 Overall, there was a 0.75 point increase in the enablement score in the complex consultations from baseline. However, enablement scores increased significantly with all consultations, not only the complex consultations. 14 Interestingly, while an increase in enablement scores was found, the increase was not uniform across the 6 scale items. Differences were demonstrated in patients’ ability to understand their condition (P = .004), cope with their illness (P < .001), and keep themselves healthier (P < .001). 14 The patients’ ability to cope with life, confidence about health and ability to help themselves, the other items on the PEI scale, 9 were not increased by the longer consultations offered as the intervention in this study. GPs reported less stress following introduction of the “free time” initiative. 14
Longer patient interactions yielded higher enablement scores in some studies; however, this finding was not consistent across the literature. Studies conducted in the PHC sector in the United Kingdom,9,14 Poland, 10 and Japan 11 report positive associations between longer clinician-patient interactions and enablement. However, an Australian study 18 found no relationship between time and enablement. The financial implications of a longer consultation may also be a factor in the relationship between consultation length and enablement. The implications for patients will depend on the way the individual PHC service operates. 18 Rohrer et al 15 suggest it might be better to outsource education aimed at empowerment in cases where the need was not urgent or overly complex, but cautioned that outsourcing could affect the clinician-patient relationship.
Patients’ Expectations and Satisfaction
Some studies viewed enablement and satisfaction as distinct concepts, others found they were linked. Three studies4,19,30 included in 1 review, 4 claimed that enablement and satisfaction are linked, but Howie et al 9 while testing the PEI against 2 satisfaction scales (the Consultation Satisfaction Questionnaire [CSQ] and Medical Interview Satisfaction Scale [MISS]), suggested that they are different concepts. A further 2 studies,3,23 which examined the outcomes separately, found that while the relationship between enablement and satisfaction was not linear, 3 they were linked.
While satisfaction appears to be linked to patient expectations, 35 one Australian study found no relationship between the 2 outcomes. 18 Simmons and Winefield 18 suggest that patient satisfaction is poorly reported. The Australian study found that patients were, however, more likely to admit to experiencing no health benefit and this could be expressed in terms of enablement. 18 The findings suggest that the latter was not seen to be a personal reflection on the practitioner. 18
Other Factors That Influence Enablement
The relationship between enablement and any single modifiable factor is confounded by intrinsic factors that are not modifiable and are decidedly heterogeneous. Some authors suggest that the degree to which a patient is enabled is influenced by factors such as presenting issue, 5 general state of health, 5 ethnicity, 16 own coping strategies, 11 degree of independence, 11 and socioeconomic status. 14 In addition, the degree of enablement was influenced by the paradigm in which the general practitioner was trained. A 2002 study in Poland looked at the different ways GPs were trained. 10 It found that those who had been trained to take a patient focused approach to care, as opposed to traditional training, gained higher enablement scores among their patients. 10 Traditional training was seen to have less focus on holistic care and more on the medical model of illness. Studies concerning GPs’ empathy 21 and help-giving styles 18 suggest these are also linked to GP education or preparation. Two studies17,22 examined whether GPs could predict enablement scores in patients. Both studies found the link between the GP’s prediction of enablement and the patient’s actual enablement score, was weak. This indicates that GPs require a stronger understanding of the concept of enablement in order to fully incorporate it into their practices.
Discussion
Medicine clearly defines patient enablement in PHC and recognizes that it is a more valid measure of the quality of a consultation than satisfaction. Enablement does not correspond purely to the patient’s expectations, but rather to how the consultation assists them to cope with life and health issues. 5 Articles included in the content analysis came primarily from nursing and the tertiary sector. They failed to include Howie’s work conducted in the PHC setting. In this analysis, the attributes of enablement were defined as “the therapeutic relationship, the consideration of the person as a whole, the facilitation of learning, the valorization of the person’s strengths, the implication and support to decision making and the broadening of possibilities.”29(p147) The study by Hudon et al 27 is the only comprehensive study found in this review that combined the 2 aspects of enablement by investigating patients’ perspectives of enablement.
Studies included in this review, show that ethnicity,16,35 reason for consultation, 14 socioeconomic situation, 34 and general state of health 5 can limit enablement. These findings are important to explain regional and international differences in enablement and to tailor practices accordingly. Ethnicity was found to affect enablement16,35, but no explanation for this has been put forward in the literature. In broader research, a study of empowerment in the United Kingdom that focused on people of South Asian origin suggested that existing attitudes of a community needed to be explored in order to enhance empowerment. 36 The value placed on education in this study, had a positive influence on attitudes to empowerment through knowledge but conversely led to low motivation in becoming a partner in their own care. 36 The relationship of these factors needs to be explored and incorporated into the practice of enablement to promote enablement as a fair measure of the quality of a consultation,
The RCTs that examined enablement 20 and self efficacy 33 are perhaps the best evidence of the practice of enablement in the PHC setting. Although the trials examine specific illnesses, they show positive outcomes for the adopted approaches. Haughney et al, 20 in their RCT conducted among patients with asthma, found that having greater control of their medication doses enabled patients. Stone et al, 36 in a study among patients with diabetes found that a program that promoted self-efficacy and patient involvement enhanced enablement. 33 Both trials showed a significant improvement in enablement and self-efficacy.
The literature that discusses the attributes of enablement is also important in determining specific practices that are enabling. The attributes of enablement given by Hudon et al 29 include consideration of the person as a whole, support to make decisions, facilitation of learning, broadening of possibilities, and valorization of strengths. These proposed attributes can be seen to reflect in the quantitative literature that links enablement to empathy, 5 communication, 11 and patient-centered behaviors. 16
A focus of enablement is legitimizing illness and the importance of trust and hope. 27 This reflects the concept of coping emulated in the work of Howie et al 9 and is reinforced by Japanese research, which identified independence and coping as key factors in enablement. 11 Patients in the reviewed studies, appear to value patient centeredness in terms of partnership and trust. However, it does not appear to be a linear correlation. Partnership is linked in the literature with nonverbal behaviors and verbal dominance and these elements have been shown to have different effects on enablement.
It is clear that more research into the other factors that influence enablement. Further qualitative analysis of how and why people feel enabled, is needed. Literature reviews on enablement are sparse, with only 3 studies found: a concept analysis 29 that relies heavily on the concept of empowerment, a review of instruments used to assess enablement, 4 and a study of outcome measures in PHC. 30
The nursing literature about enablement uses a range of research methods, while the medical literature is predominantly quantitative in nature (using PEI). It is important to amalgamate views of the concept gained from both quantitative and qualitative research to fully understand how enablement can be developed within all consultations in PHC.
While the majority of the studies into enablement in PHC focus on GPs, the Patient Enablement and Satisfaction Survey, a variation of the PEI, has been developed for practice nurses. 26 This scale, however, did not investigate properties of enablement. While it is important that the PEI has been adapted for other health care professionals, without further understanding it will not address the gap in knowledge. Therefore, further study is required into both the practice and the factors affecting enablement.
There are a plethora of definitions pertaining to empowerment, which is recognized as a key component of general practice. It is clear that the concept of enablement needs further definition. Recognizing and formalizing the attributes of enablement particularly in relation to PHC is important for both quality improvement and for education of the PHC workforce. Enablement has been recognized as a valid measure of quality in PHC and has been incorporated into more comprehensive consultation assessment tools.37,38 The literature goes some way to describe some of the specific attributes needed to enable a patient, but more research is required. Qualitative data around enablement are particularly lacking and are pivotal to truly understand the concept.
Strengths and Limitations
This study has identified the disparate nature of the current literature into enablement. However, it is acknowledged that this study, while replicable, is limited by the small sample of studies found on this topic.
Implications for Practice
Enabling patients has several important outcomes for the PHC sector. These include reducing patients’ dependence on health care services already under stress; enhancing the quality of consultations and promoting a sense of power among those often rendered powerless by illness or incapacity. The findings of this review may assist practitioners to recognize the importance of incorporating enabling behaviors to improve the quality of their consultations. This review has identified that practitioners have limited success in predicting how enabled their patients feel following a consultation. Implementing the PEI is a validated way to inform the practice of enablement, and for health care providers to reflect on how their current practice affects their patients.
Conclusion
The concept of enablement is well defined as a quality outcome measure in PHC. Enablement is conceptualized as a quality outcome measure that is recognized as the gold standard of care. There is strong but limited evidence concerning the practice of enablement. It is recognized that consultation features such as length of consultation, communication style, and empathy of the practitioner are related to patient enablement. However, there is sparse research into the practices that influence enablement. Qualitative research into enablement is particularly sparse, and studies are needed to explore enablement from the patients’ perspective. The influence that culture and ethnicity have on enablement is an area that also needs to be researched. The focus of studies examining enablement has to date concentrated on GPs; however, this concept could be used to examine the quality of consultations of other health care practitioners in PHC. More research is needed to explore nurse practitioners’ capacity to enable patients in the PHC setting.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
