Abstract
Background
Technology for concussion identification and management is rapidly expanding across the continuum of care. Although many technologies offer a range of services around concussion, there is an absence of a non-commercial online location for medical providers to access regarding the functionality of the various technologies used in concussion identification and management.
Objective
The purpose of this review is to present research findings on technology for concussion identification and management.
Methods
Searches for eligible studies were conducted using the PubMed, EMBASE, and Scopus databases with specific search criteria. Through a stepwise process, full-text articles were selected for inclusion if they described clinically useful electronic technologies (i.e. electronics able to be used in standard clinical environments including telehealth) by healthcare providers or end users (i.e. parents or athletes).
Results
A total of 29 articles were included in this review and described technology used to measure symptoms (3), neurocognitive performance (7), the visual system (4), and balance or dual task performance (18). Within the results, various technologies demonstrated increased utility for concussion identification, often detecting subtle deficits not possible with current low-tech clinical methods, differentiating those with concussion from those without concussion, with strong reliability and validity.
Conclusion
Innovative technologies included in this review demonstrate enhanced ability to identify and manage symptoms of concussion, neurocognitive deficits, visual deficits, and balance and dual-task deficits.
Introduction
Among civilians, athletes, and service members, concussion has gained attention as a concerning diagnosis with potential to impact health status for a prolonged period of time. Interestingly, although millions of research dollars have been spent to better understand concussion, there still seem to be more questions than answers. In fact, to date there is still no “gold standard” for diagnosis of concussion. 1 No routinely available biomarker or imaging technique has been identified to definitively diagnose concussion. Rather, concussion emerges as a clinical determination by coupling a reported traumatic biomechanical event with common signs and symptoms.1,2 Because concussion can potentially impact multiple brain functions, but does not always impact any one brain function, it can be a difficult diagnosis to make. Similarly, because concussion presents differently across the populations affected, treatment (or management) does not include one formal or typical path.2,3 This makes concussion one of the most difficult diagnoses to identify and treat, especially when associated with sports and military environments. 1
Technology use for concussion identification and management is a burgeoning avenue for research and development. As an adjunct to traditional clinical tests and patient report, technological advances could serve to increase the accuracy of diagnosis and aid clinical decision making by providing enhanced objective measurements. Technology may also assist clinicians in managing concussion symptoms by treating resultant functional disturbances. From the use of phone-based applications for education, 4 to computerized testing for baseline assessment (pre-concussion), to eye movement video tracking and analysis for diagnosis of concussion, the use of technology is rapidly expanding across the continuum of concussion care. 5
At this time, although there are many technologies and start-up companies offering a range of services around concussion, 6 there is an absence of a non-commercial online location for medical providers to access regarding the functionality of the various technologies used in concussion management. This makes it difficult for medical providers to navigate between biased claims versus research evidence supporting the best technologies to enhance concussion care. Therefore, the purpose of this review is to present research findings on technology for concussion identification and management. This will include a description of the technology, its purpose, how it is used, and the research findings. Following the description of current technologies, future directions and opportunities for technological development in this area will be discussed.
Methods
This project was completed as a scoping review of existing literature. A systematic search was used to identify relevant publications within the aim of this project.
Data sources and search strategy
Searches for eligible studies were conducted using the PubMed, EMBASE, and Scopus databases. The search was developed with assistance from a medical reference librarian at the University of Mississippi Medical Center using the search string ((“electronic technology” or “wearable electronic devices” or technology or telemedicine)) AND (“brain concussion” or concussion).
Selection criteria
Studies included in the review met the following inclusion criteria: a full text article written in English describing clinically useful electronic technologies (i.e. electronics able to be used in standard clinical environments including telehealth) by healthcare providers (i.e. physicians, neuropsychologists, physical therapists, athletic trainers, etc.) or end users (i.e. parents or athletes) in affiliation with a concussion diagnosis (for our purposes, concussion was synonymous with mild traumatic brain injury or mTBI). Diagnostic accuracy, psychometrics (validity, reliability, etc.), user interaction/feelings/etc., and intervention designs were also included in this review in order to search for all evidence on electronic technology and its usefulness in diagnosing and managing/treating concussion. Studies were excluded if the technology consisted of on-field sensors to detect head acceleration or impacts only (where diagnostic accuracy for concussion is not reported), or if data was obtained via instrumented lab-based biometric measurements that would not be available for a typical clinician to use in an environment where concussions are typically diagnosed, managed, or treated.
Study selection and management
A stepwise process was used to select articles for inclusion. Title and abstracts were screened by two authors, with discrepancies decided by a third author. Two authors reviewed the full text articles with discrepancies decided by a third author. After selection, the included studies were grouped into categories based on the type of neurological function being studied or described. Furthermore, within each category, studies were classified based on what type of evidence was presented on the usefulness of the technology for a given purpose.
Data extraction
Data extraction was performed by all authors, with articles separated into categories. A second author checked the accuracy of the original author’s data extraction. The extracted items included the description of participants, the technology, the technology’s purpose, and how the technology is used. The results of each study were extracted based on the study type and purpose.
Results
Study selection
From the database search, 818 titles were identified and screened (after removal of duplicates); 201 abstracts were screened, 27 of which were abstracts only from conference proceedings and were discarded, leaving 75 full text articles. After review, a total of 29 articles were included in this review.
Study characteristics
Upon review of the 29 included studies, the following primary categories of function emerged: balance/dual task; neurocognition; symptoms; and vision. Studies that described results in more than one category were included in both categories. Within these categories, the studies presented evidence on specific technology and its usefulness for differentiation of concussion from healthy; normative values of performance as measured by the technology; reliability and validity of the technology; and usefulness of the technology in the management of a concussion. Results for each category are presented in Tables 1 to 4.
Technology for balance and dual-task performance.

Balance Accelerometer Measure (BAM); Balance Error Scoring System (BESS); Inertial Measurement Units (IMU); Intra-class Correlation Coefficients (ICC); modified BESS (mBESS); Range of Motion (ROM); Root Mean Square Error (RMSE); Sensory Organization Test (SOT); Virtual Environment TBI Screen (VETS); Virtual Reality (VR); virtual time-to-contact (VTC); years old (y/o);
Results of individual studies
Balance and dual-task
Eighteen studies examined how concussion adversely influences balance and the performance of dual tasks (Table 1). Three of these studies established normative values for technologies that measure postural sway and balance errors after a suspected concussion. These technologies included the Sway Balance System for children and adolescents, 6 BTracts Balance Test Concussion Measurement Tool, 7 and the Tekscan Mobile Mat. 8
Seven studies investigated reliability and/or validity for new technologies used for identification or management of concussion. Five of these studies investigated specific technology compared to the Balance Error Scoring System (BESS) or modified BESS (mBESS). The Wii Balance Board displayed good reliability and excellent validity. 9 Kinect V2 sensors exhibited good test-retest reliability and excellent validity with total BESS score. The total mBESS scores were also compared in this study and found to exhibit good reliability and excellent validity. 10 The effectiveness of the Automated Assessment of Postural Stability (AAPS) system was evaluated for sideline identification of concussion. Good correlation was found with the AAPS algorithm and human scoring of the BESS. The AAPS also measured multiple balance errors with high resolution providing additional consistency and accuracy. 11 Another study examined the validity of the Glass Explorer Edition smart glasses compared to the well-described smartphone waist accelerometer using the National Institute of Health’s Balance Accelerometer Measure (BAM). The smart glasses were highly correlated with the waist accelerometer, and reliability was high. When all three axes were used in the normalized path magnitude, the correlation improved even further. 12 Validation of the OptoGait motion analysis technology was attempted by comparing it to the BESS and the Immediate Post-Concussion Assessment and Cognitive Testing (ImPACT). Thirty of the 64 OptoGait mean scores were correlated with the double-leg foam BESS scores. Seventeen of the 64 OptoGait standard deviation scores were correlated with the balance tandem hard surface BESS scores, but none of the OptoGait variables correlated with the ImPACT. 13
Further, in the diagnosis of concussion, two studies described new virtual reality (VR) technologies. One of these used an inertial tracking technology attached to the head to detect position while watching VR animations through liquid crystal shutter glasses and then performed balance testing with different virtually projected scenarios. VR balance module was found to have high sensitivity and specificity. 14 Another study examined the Virtual Environment TBI scan (VETS) which uses a Wii Balance Board, compared to the Neurocom Sensory Organization Test (SOT). The VETS was found to have high sensitivity and specificity. The overall accuracy through all six VETS conditions was 91.0%. 15
Three additional studies described sensor technology in the measurement of balance for diagnosis of concussion. One of these compared the ability of the BESS to the ability of the BAM to detect the differences in postural sway between concussed and healthy individuals. The BAM was not able to delineate between them. However, the BESS, especially tandem stance, was able to discriminate between adolescents with acute concussion and healthy individuals with a low sensitivity and high specificity. 16 Another study examined which portions of the mBESS and postural sway measurements obtained with an Opal inertial sensor placed at L5 could detect acute concussion. The measures taken with the inertial sensor successfully discriminated acutely concussed individuals, and the double leg stance portion of the mBESS best discriminated those with acute concussion. Clinical mBESS measures were not able to discriminate between acutely concussed and healthy adolescents. 17 The third study examined the ability of the Wii Balance Board to assess balance in the pediatric population to identify concussion. Only the double limb eyes open test successfully identified concussion. 18
Three studies were identified which described technology in the management of concussion. One study examined postural sway in standing using the virtual time-to-contact (VTC) measures through a force-plate. The only significant differences seen from prior to and 30 days post-concussion in the VTC were at the deflection points and mode at 30-days post injury. 19 A case study examined treatment of an individual who had delayed concussion recovery using the virtual Computer Assisted Rehabilitation Environment (CAREN) system. At the conclusion of 6 treatments, the patient improved in postural and gait balance with almost complete resolution of concussion symptoms. Improvement was also seen in the executive function and dual tasks tests. 20 The third study determined the responsiveness of the C3 App in detecting postural sway while performing the BESS protocol by comparing scores of concussed individuals who had typical recovery with those who had prolonged recovery. There were significant differences in two of the six BESS stances as measured by the C3 App including double limb stance on foam and tandem stance on foam. 21
Finally, one additional study explored the use of a wearable inertial measurement unit (IMU) to quantify head movements in response to vestibular rehabilitation. Here, it was found that this technolology had good agreement with a room-based motion capture system. 22 One study developed a dual-task model to evaluate cognitive-motor function using the inertial sensors in an iPad to measure postural sway. The optimal dual-task model was found to be the model where 60 stimuli/min was delivered in tandem stance with eyes closed. 23
Neurocognition
Seven studies described the use of technology for identifying, managing, or developing normative data in relation to neurocognitive symptoms commonly seen with concussion (Table 2). A variety of technology was used including the C3 App,21,24 the Display Enhanced Testing for Concussions mTBI(DETECT System), 25 the CogSport, 26 the ImPACT, 27 the Cambridge Neuropsychological Test Automated Battery (CANTAB), 28 and the BrainScope Ahead 300. 29 The C3 App was successful at detecting significant differences for simple reaction time, choice reaction time, and Trail Making Test B when comparing individuals who recovered within three weeks of a concussion to individuals who remained symptomatic after three weeks. 21 When the C3 App was combined with a dual task activity, a significant difference was found in simple reaction time, choice reaction time, gait speed, and stride length when comparing concussed and healthy individuals. 23 One study evaluated the effectiveness of a portable neuropsychological assessment device with a distraction-free, immersive visual and auditory environment, the DETECT system, in eliminating external audio and visual stimuli in healthy college students. No significant difference was found in performance in a noisy versus quiet environment. 24
Technology for neurocognitive performance.
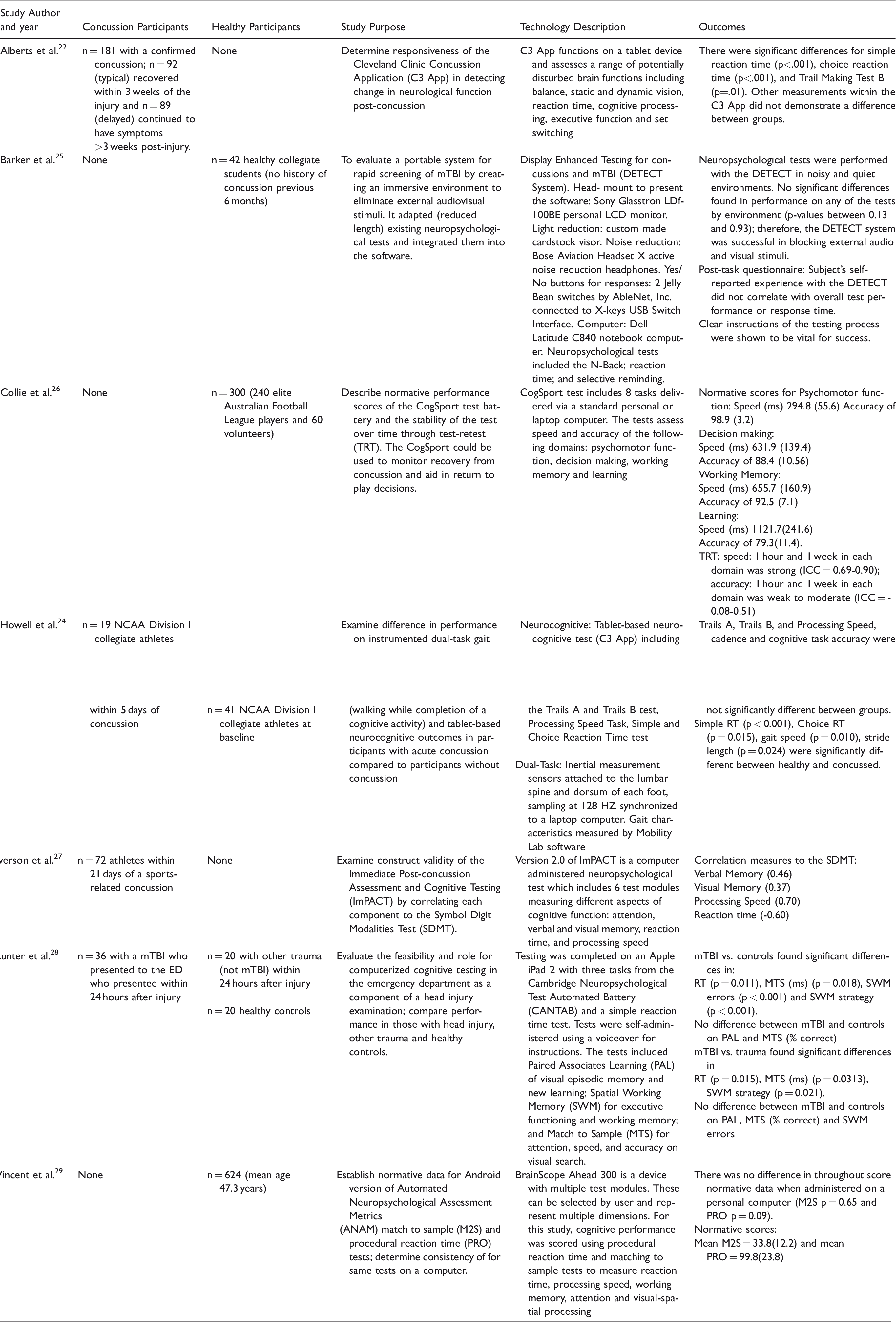
Two studies enrolled only healthy individuals in order to determine normative data. The CogSport’s measure of speed and accuracy for neurocognitive functions was found to be highly reliable in serial testing and ideal for repeated testing of cognition. 26 Normative data for two cognitive performances on the Automated Neuropsychological Assessment Metrics (ANAM) was obtained via The BrainScope Ahead 300 android mobile device with multiple test modules to aid in assessment of mTBI, and then compared to data collected on a personal computer platform. There were no significant differences found between the two, indicating that this mobile device can be used clinically with comparable reliability as a personal computer. 29
Lunter et al., 27 compared individuals with a mTIB to a healthy control group and a trauma group (not mTBI) in order to determine the feasibility and role for computerized cognitive testing (CANTAB) in the emergency department as a component of head injury examination. When comparing mTBI to the control group, there was a significant difference in reaction time, match to sample, spatial working memory errors, and spatial working memory strategies. There was also a significant difference in reaction time, match to sample, and spatial working memory strategy when comparing mTBI to the other trauma group. No significant differences were found on paired associates learning or match to sample percent correct between the mTBI individuals and the healthy or trauma groups. Lastly, one study enrolled only concussed individuals in order to determine construct validity for the ImPACT, which developed correlation measures to the Symbol Digit Modalities Test (SDMT). 26
Symptoms
Three studies described the use of technology for symptom management or reporting post-concussion (Table 3). The technology used in each of these studies include the following: Self-Management Activity Restriction and Relaxation Training (SMART), 30 Ecological Momentary Assessment (EMA), 31 and SuperBetter. 32 These applications monitor symptoms, provide education in managing current symptoms, and provide reminders to track occurrence and intensity of symptoms. Babcock et al., 30 established that using a web-based intervention such as the SMART program soon after injury is safe because there were no worsening symptoms or disability observed with its use. Significant improvements were reported in functional disability and executive functioning by the parents, but not the adolescents. In another study, participants demonstrated high utilization and satisfaction of the SuperBetter mobile app to track and self-report symptoms following concussion. Greater improvement in symptoms and optimism were reported with the app use; however, no significant differences were found with app use for depression. 32 The EMA methodology using the Palm Pilot device was found to be easy to train adolescents to use, feasible for a school setting, and had a high compliance rate. 31
Technology for symptom measurement.
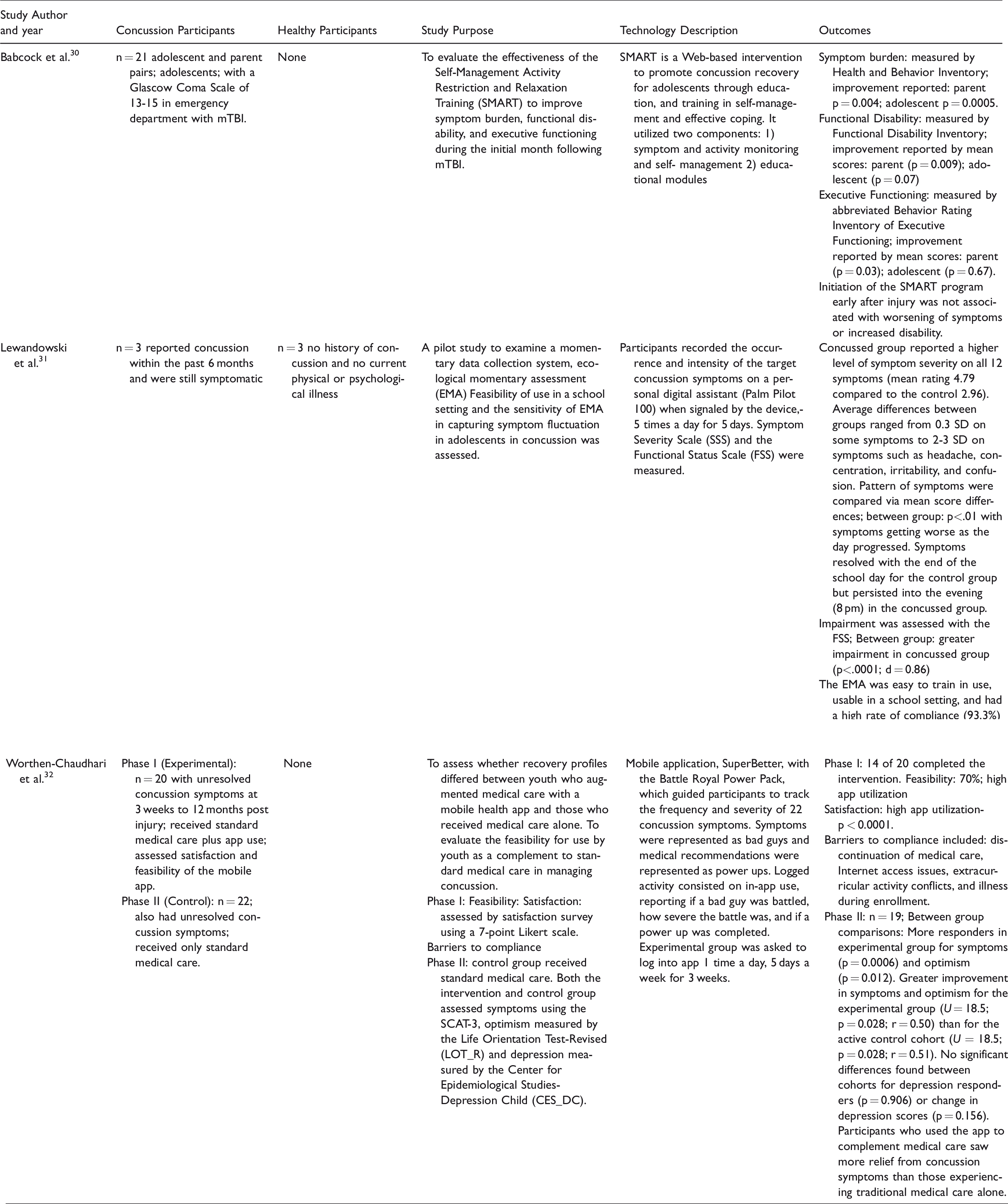

Technology for visual system performance.
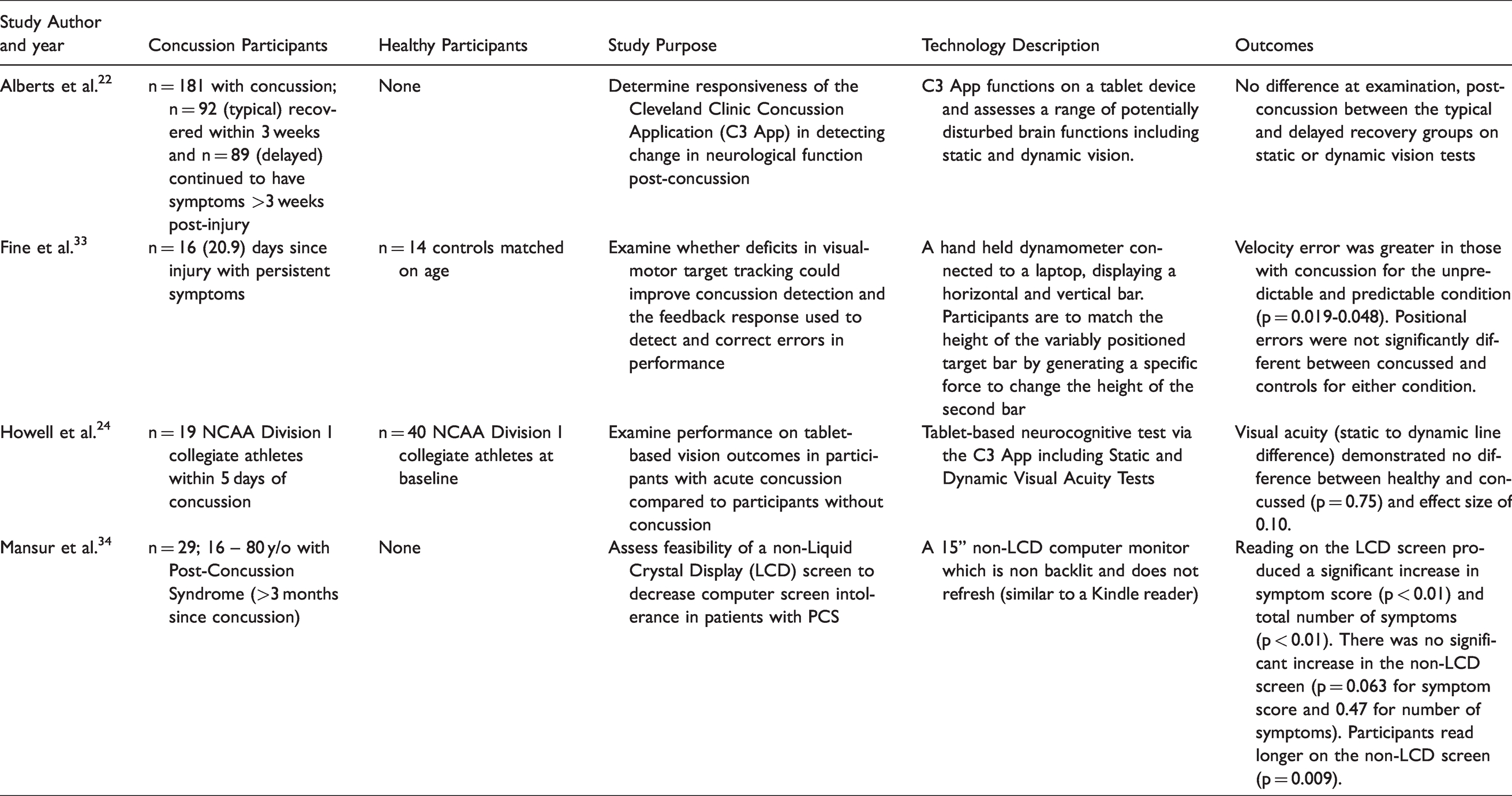
Visual system
Four studies described the use of technology for components of the visual system related to concussion (Table 4). Three of these explored technology in identification of visual deficits post-concussion.21,24,33 Within these studies, the technology described included the C3 App; a computer based program to examine deficits in visuomotor target tracking; and the use of a non-Liquid Crystal Display to decrease visual sensitivity. Across the three studies, one found that the technology was useful to detect velocity error, which was greater for the concussion group when compared to healthy controls. 33 The C3 App did not detect significant differences in static or dynamic visual acuity between concussion and healthy participants. 24 The second study using the C3 App found that the vision tests were unable to discriminate between the typical and delayed recovery groups at examination. 21 One of the included studies described technology in concussion management. 34 This study found that a non-LCD display produced less screen intolerance in participants with post-concussion syndrome.
Discussion
The 29 articles included in this review described technology to measure balance, neurocognition, vision/oculomotor function, and symptoms associated with concussion. An interesting point is that 27 articles were unable to be included in this review because they were only available as an abstract, having no corresponding manuscript. Typically, this occurs when research is presented as a poster or platform at a scientific conference or meeting but does not go on to become a published, peer-reviewed, full-length manuscript. It is not known why so many studies describing technology and concussion are not being published, but it is disappointing because the results of these additional 27 studies could have been very informative to this review and to the general research base supporting technology development. We would like to encourage those researching in this area to bring their research findings to publication so that it is able to be incorporated more completely into the evidence base.
A majority of the studies included in this review reported on balance and within this, most focused on technology’s ability to identify concussed individuals from non-concussed individuals. Several studies explored technology’s measurement of balance in comparison to the BESS or mBESS (no-tech clinically based outcome measures), or used sensor measurement to provide enhanced measurement of balance during BESS/mBESS performance.8,10,11,13,16,17,21 Overall, the additional information provided through sensor measurement increased the usefulness of the BESS/mBESS for concussion identification. A second finding within the research on balance is that quantification of postural sway with VR technologies provided sensitivities and specificities of >80% to differentiate concussed from non-concussed individuals.14,15 Other sensor based technologies of postural sway identified specific postures that were the most discriminant for concussion diagnosis, two of which showed double leg stance, eyes open, 18 and closed, 19 were the most discriminant positions for concussion identification.
It is understandable why technology in concussion has an abundance of research exploring balance. Standing balance is quick and easy to assess, can be examined almost anywhere, and if advanced sensor measurements can demonstrate high diagnostic utility, balance could be an ideal biologic marker of concussion. According to the results presented here, although technology’s ability to measure balance is superior to human measurement, produces good to excellent validity and reliability, and provides an enhanced ability to identify balance impairments, there are still 13–19% false positives and false negatives in differentiating concussed from non-concussed,14,15 making these technologies very useful, but not stand-alone tools in concussion identification.
Tests of neurocognition have been widely used to screen for concussion. Initially, these tests were completed with paper and pencil but have moved to computer-based platforms. Of the seven studies included in this review, various types of tests on tablets, other mobile devices, and immersive environments produced significant differences in performance between those with and those without a concussion.21,24,25,29 The sensitivity and specificity of these tests was not described in any of these studies. We believe that new technologies to administer valid tests of neurocognition hold much promise, particularly as they are moved in to emergency departments and are able to obtain reliable results in non-optimal (noisy) environments,25,28 these technologies hold promise for more immediate concussion identification. Future directions should continue to work towards technology-enabling tests of neurocognition with measurement capacities that do not require baseline testing for optimal usefulness.
The experience of symptoms by individuals with concussion is variable based on provocation of movement, 35 environment, and cognitive load. The studies included in this review explored technology for symptom monitoring, enabled enhanced methods of tracking daily symptom reports, and provided medically based suggestions for self-management.30,32 We see these tools as being very useful as mobile applications, accessible from a smart-phone, for monitoring response to increased mental and physical demands, including gradual return to learn, and providing real-time solutions to de-escalate increased symptoms. We suggest that further advances in this area would include the use of these types of tools for collection of symptom metrics each day post-concussion to present to medical providers through a telehealth platform for asynchronous remote patient monitoring. This would permit directed management, including change of management strategies. For example, remote symptom monitoring would enable a provider to assess if symptomatic recovery is progressing faster than anticipated. This may enable a progressive resumption of typical activities. Conversely, if unanticipated spikes in symptoms occur, this could indicate neurological overload and warrant an in-person visit or scaling back of activities.
Within the recent past, vision, oculomotor function, visual attention, and perception have all become areas of intense interest in the study of concussion.36–38 In the absence of concussion, research on oculomotor function has been conducted using instrumented laboratories with eye tracking capabilities, specialized computer software, data filters, and advanced statistical analyses. These are difficult things to translate from a lab-based environment to a mobile platform. The studies included here did not utilize instrumented labs but rather laptop computers and iPads. From the results provided, there is limited evidence that static and dynamic vision, as measured on an iPad, can differentiate concussions from non-concussed or those with typical or delayed recovery.21,24 There was some evidence that visuomotor target tracking could improve concussion detection using a hand-held dynamometer and a laptop. 33 One study also demonstrated that visual sensitivity could be decreased with a non-LCD computer screen, 34 which is helpful as a management strategy as student athletes try to return to the learning environment. Given that eye-related metrics have gained considerable ground as biomarkers for concussion,38 we believe that research to detect eye-related impairments with mobile technology is just beginning. We expect advances in this area to accelerate in the near future.
Technological advances offer the opportunity to enhance concussion identification by detecting minute impairments undetectable with regular clinical measurement capacities, thereby increasing the objectivity of examination. Most of the studies included here explored technologies for concussion identification. We believe that technologies also hold promise for the provision of unique opportunities for rehabilitative treatment of functional impairments. Unfortunately, only one case study was identified in this review describing high-end technology (a fully immersive virtual reality system) as a treatment modality. 20
We hope that innovative ideas using advanced technologies continue to be studied and are able to add enhanced diagnostic accuracy for concussion as well as effective treatment mechanisms.
It is likely that many of the commercially available technologies for concussion are not represented in the literature included in this review. Some of these may be represented in the 27 abstracts which were unable to be included. However, it is also possible that these were not identified by the search strategy utilized. Because this review sought to include all available technologies which are able to be used in a clinical environment for concussion, many research designs and study objectives were included, making strong generalizations across studies difficult.
Conclusion
There are many technologies which have been and are being investigated to assist with concussion care. To date, these technologies have predominantly focused on the ability to identify those with concussion from those without concussion. While the research included in this review demonstrates some enhancement over clinical tests and measures, the ability to definitively detect concussion remains obscure. Additionally, there are many unexplored opportunities where technology could be investigated as an intervention modality. It is likely that this broad and diverse area of research will continue to evolve as new sensors and software are developed, exposing new tools to enable greater accuracy in identification and usefulness in management.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project is/was supported by the Federal Office of Rural Health Policy (FORHP), Health resources and Services Administration (HRSA), U.S. Department of Health and Human Services (HHS) under cooperative agreement award no. 6 U66RH31459-02–03.
