Abstract
Background
Each year in the United States approximately three million individuals sustain sport or recreation-related concussion which may occur in the setting of orthopedic trauma requiring surgical intervention under general anesthesia. The effects of surgery and general anesthesia on brain recovery are currently unknown. The objective of this study was to determine the prevalence of recent sport concussion, recognized or not, in a preoperative, pediatric, surgical population.
Methods
The study involved administering a questionnaire to all eligible, consented patients in one of the following settings: Preoperative Clinic, Day Surgery Unit, Trauma Clinic, or inpatient floor. The questionnaire was designed to determine the occurrence and symptoms of a concussion. This study was conducted at an urban 395-bed comprehensive center for pediatric health, between May 2014 and April 2015. Inclusion criteria for study were age 5–21 years, presentation for surgical repair of orthopedic traumatic injury or nasal fracture, and precipitating injurious event occurring within four weeks of surgery.
Results
The prevalence of concussion in the setting of orthopedic trauma, either known or unknown at the time of presentation for surgery was 6%. The interval between surgery and injury was between three and 13 days. Prior education for recognition of concussion was present in 66% of patients.
Conclusions
The impact of surgery with general anesthesia in pediatric patients with a recent concussion is unknown. No changes in post-op disposition were noted in this patient population. However, our findings support the need to measure neurocognitive function before and after administration of operative procedures in a larger population with a recent concussion compared with controls.
Keywords
Introduction
Each year in the United States approximately three million individuals sustain sport or recreation-related concussion, but many more incidents may go unrecognized or unreported.1,2 There is also a notable rise in the incidence of concussion in the United States, with the highest incidence occurring in patients ages 15–19 years of age. 3 A concussion is a neurologic insult induced by traumatic biomechanical forces resulting in complex pathophysiologic injury with transient functional and biochemical changes in the brain and may progress to varying degree of diffuse axonal injury. 4 A concussion results in a temporary alteration in brain function and mental status which manifests as a loss of consciousness, amnesia, or disorientation with an absence of any abnormalities on neuroimaging (i.e. CT, MRI). 4 In addition to the mild cognitive impairments, symptoms include headaches, fatigue, and impaired concentration. 5 These symptoms typically last for 7–10 days; however, the duration of neurophysiological derangement caused by the concussive injury has not been defined. 6 Standard clinical practice has been to restrict patient activity following a concussion in order to prevent a second insult or secondary injury. Anesthesiologists and surgeons often encounter concerns regarding the safety and timing of operative procedures and general anesthesia in the postacute setting of concussion. There are no data or literature to guide this decision.
At present, there is no evidence-based clinical pathway describing the optimal timing of surgery and anesthesia for semielective surgical procedures following a concussion. Since the impact of general anesthesia on a patient with a recent concussion is unknown, the decision to proceed with surgery in patients with known concussion is based on individual clinician judgment. In our experience, clinicians will often delay elective surgery in patients with known concussion until the patient is cleared to “return to play” or “free of symptoms.” In this regard, physicians recognize that rest and avoidance of second or recurrent cerebral insults are essential in the patient’s recovery.
In view of the above, and the uncertainly in how to manage the semielective orthopedic pediatric patient who has suffered recent concussion, we decided upon a pilot study to assess the magnitude of the problem, first, locally in our own practice and, second, provide an estimate of this problem nationally. Therefore, in this study we have assessed the prevalence of recent sport concussion, recognized or not, in a preoperative, pediatric, surgical population scheduled to undergo semielective surgery for orthopedic trauma or nasal fracture. In addition, we describe in more detail cases with preoperative concussion in which semielective, orthopedic surgery was performed.
Methods
This study was approved by the Institutional Review Board for clinical research studies and was carried out in the 12 months between May 2014 and April 2015. Boston Children’s Hospital (BCH) is a 395-bed comprehensive center for pediatric health that services a surrounding population of over four million.
Inclusion criteria for study were age 5–21 years, presentation for surgical repair of orthopedic traumatic injury or nasal fracture, and precipitating injurious event occurring within four weeks of surgery. We defined orthopedic traumatic injury as any injury resulting from a fall, collision (struck by or struck against), vehicle accident, assault, or bike-related injury or fracture. Exclusion criteria were English language not the first language or inability to respond to survey questions.
Concussion questionnaire for presurgical orthopedic injury patients ages 5–21 directions: please circle your answer.
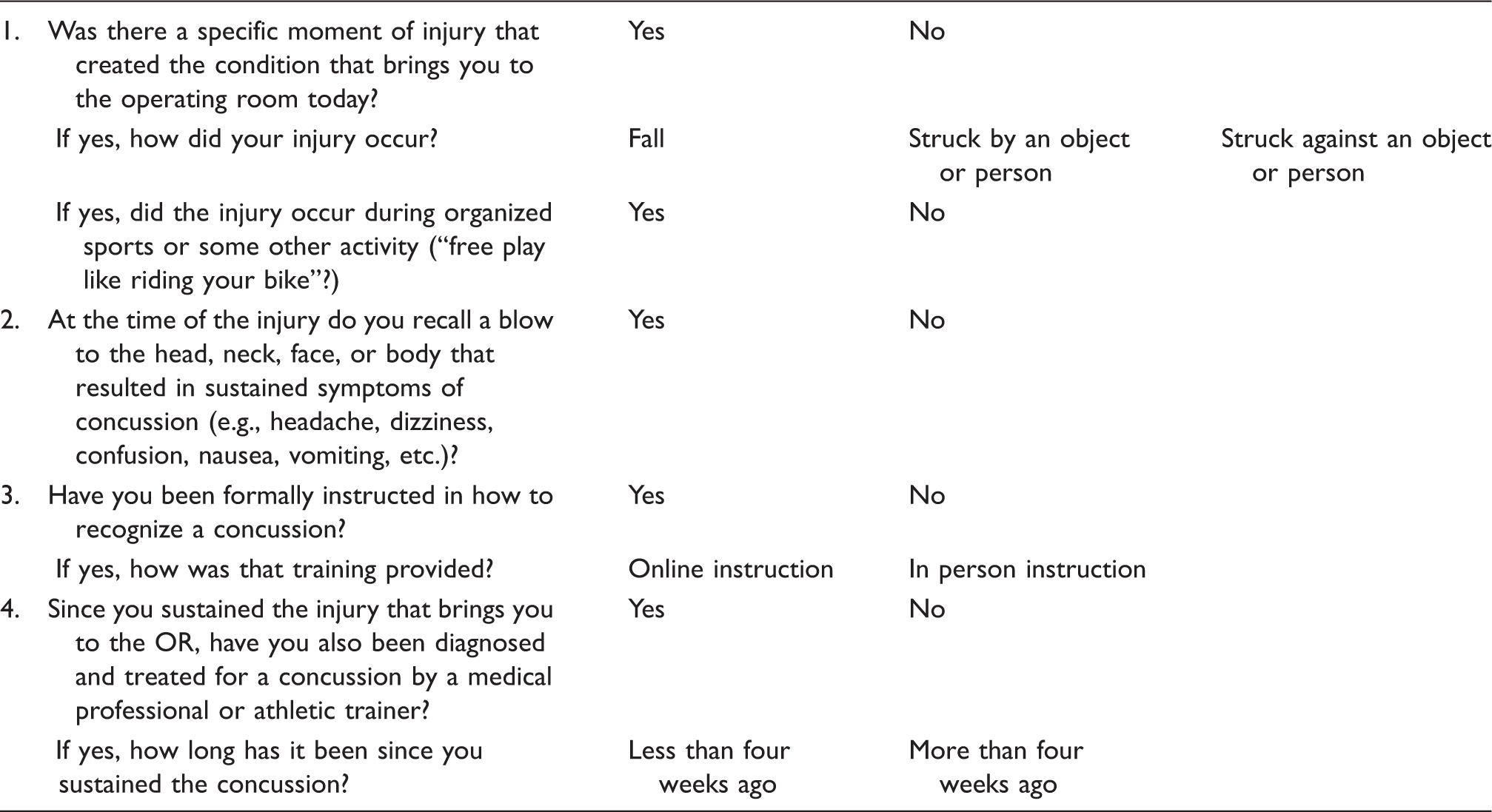
Responses obtained from the questionnaire were used to determine the prevalence of symptomatic concussions, either known or previously unrecognized. Information was entered into the Research Electronic Data Capture (REDcap™) database under a deidentified subject number. 9 A copy of the completed SCAT3™ or Child SCAT3™ was placed in the medical record. If the participant scored higher than 0 in any of the SCAT3™ or the domains, the results were conveyed to the scheduling surgeon prior to the start of the scheduled surgical procedure. The decision to continue with surgery or refer the patient to the BCH Sports Concussion Clinic was made by the surgeon.
Intraoperative records and postoperative clinic visit notes were reviewed after the study was completed for patients with a positive finding of concussion symptoms.
Statistical analysis
The prevalence of concussion in our sample is defined as the proportion of patients enrolled who had symptoms of concussion and reported with a 95% confidence interval using Wilson’s method. 10 Among the 382 patients screened, comparison between enrolled (N = 125) and nonenrolled (N = 257) groups was performed using the Student’s t-test for age, Pearson chi-square test for race, and Fisher’s exact test for gender and type of surgical procedure. Multivariable logistic regression analysis was applied to assess whether age, gender, and race were associated with concussion among the patients who were screened. 11 Statistical analysis was conducted using IBM SPSS Statistics Version 23.0 (Armonk, NY). Two-tailed values of P < 0.05 were considered statistically significant.
Results
Demographic characteristics of screened patients according to enrollment status.
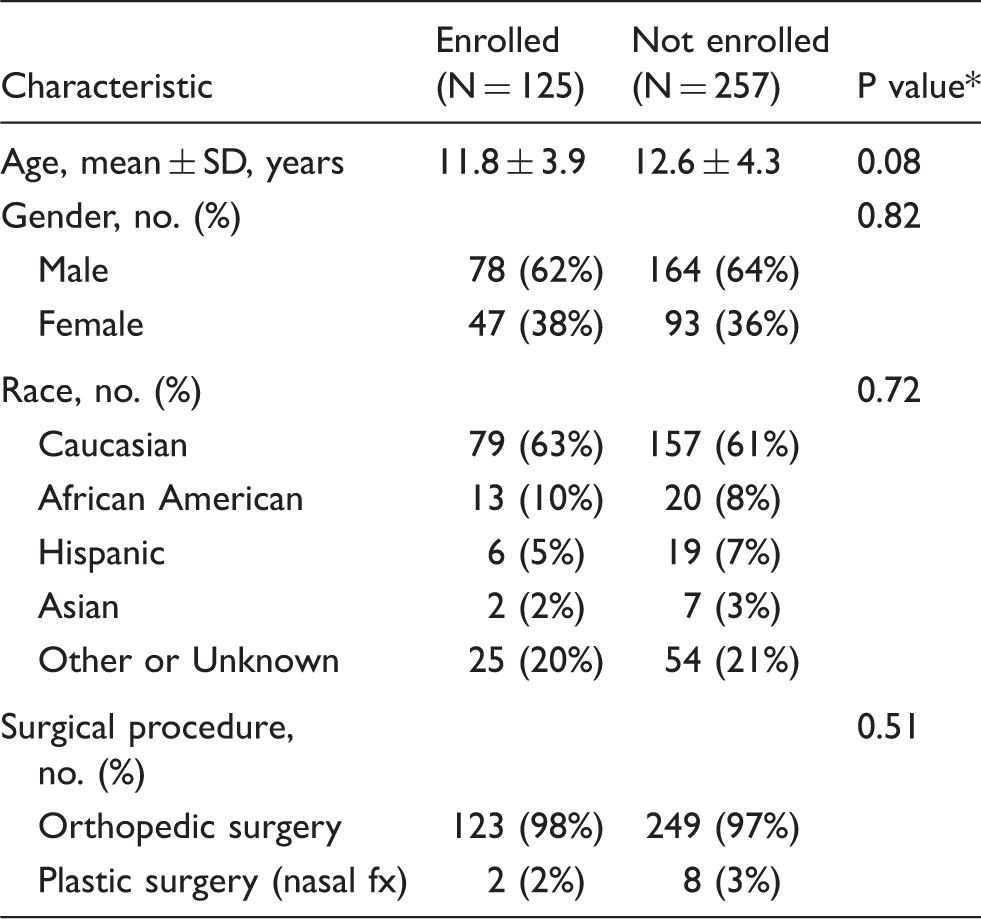
No significant group differences, confirming no selection bias. P-values were determined by Student t-test for age and Pearson chi-square for the categorical variables.
Comparison of patients with and without concussion.
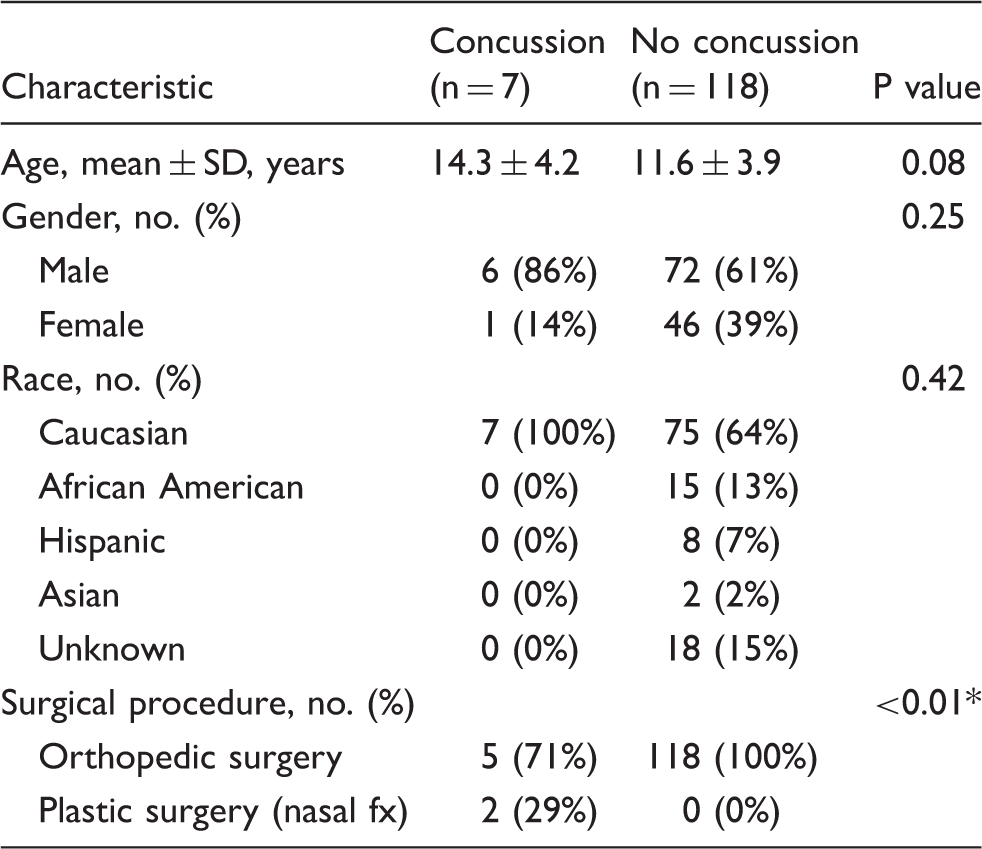
Statistically significant.
Among the 48 Pediatric Hospital Health System (PHIS) hospitals, during a similar date range to the current study, the number (median (interquartile range)) of patients with orthopedic trauma scheduled for urgent surgery with a concurrent diagnosis of concussion was 287 (200–579) cases. Thus, our study population is representative of pediatric hospitals reporting to the PHIS.
Injury occurred after a fall in 62% of enrolled patients. The remainder of the enrolled patient group demonstrated that 22% were struck by a person or object whereas 16% were struck against a person or object. Sports-related injury was present in 52% of patients and 48% sustained non-sports-related injury. A total of seven patients (5.6%) from the enrolled group had symptoms of concussion and represented the observed prevalence in our study of 2.7–11.1% (95% confidence interval). These subjects recalled a blow to the head.
Group comparisons
In the enrollment group, 83 of 125 (66%) patients indicated that they had prior, formal instruction on how to recognize a concussion. Face-to-face instruction occurred in 77% of patients and 23% obtained instruction through online tools. The group with instruction was significantly older than the group without instruction (average age: 12.0 ± 3.9 years versus 9.9 ± 3.5 years, P = 0.006).
For the enrollment cohort of 125 patients, the mean recovery time in the postanesthesia care unit from admission until discharge criteria were met was 95 min (SD 47 min; range 27–351 min). There was no significant difference in mean recovery time between the seven patients with concussion (84 ± 31 min; range 41–134 min) and the 118 patients without concussion (97 ± 48 min; range 27–351 min) (P = 0.50, Student’s t-test).
Multivariable logistic regression was performed to assess whether age, gender, or race was independently associated with concussive symptoms and none of these were found to be significant (age, P = 0.08; gender, P = 0.28; race, P = 0.70).
Patients with concussion
Details of the enrolled patients who had symptoms of concussion.
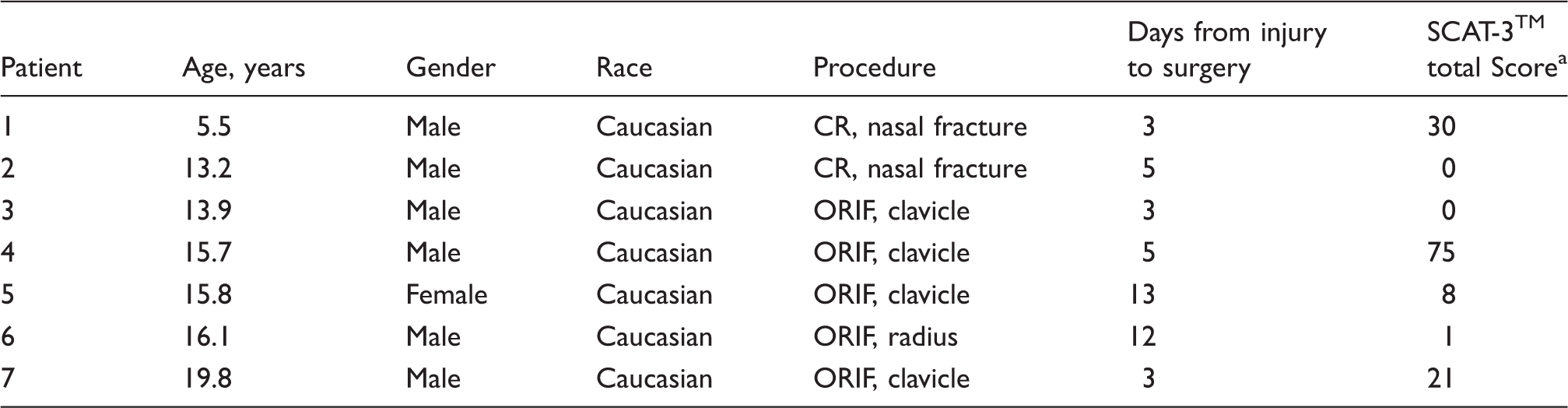
CR: closed reduction; ORIF: open reduction internal fixation; SCAT-3™: Sport Concussion Assessment Tool.
SCAT-3™ total severity score out of a maximum of 132 points, except patient 1 (a Child SCAT-3™; out of 60 possible points).
Characteristics of patients with symptoms suggestive of concussion.
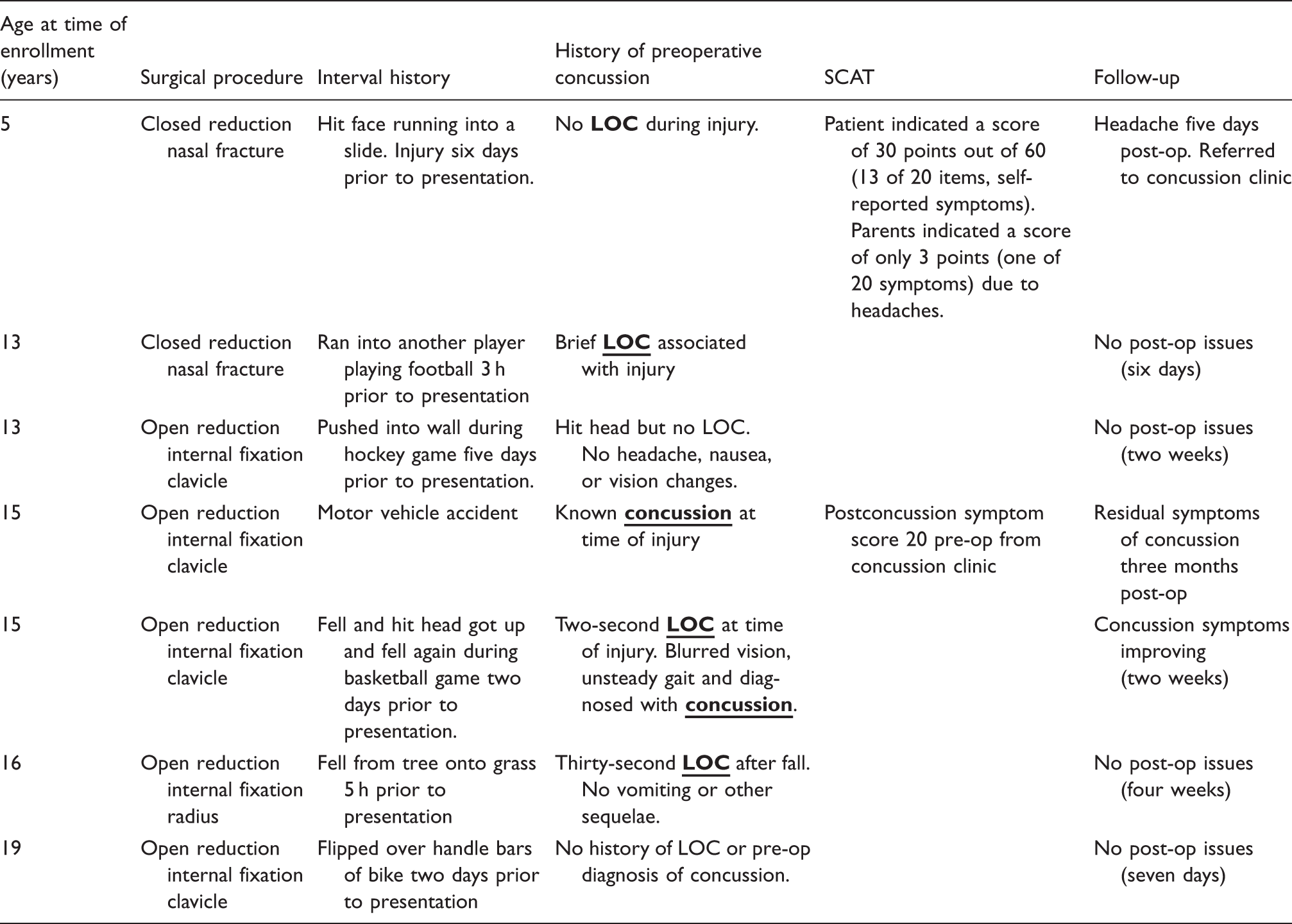
LOC: Loss of consciousness; SCAT-3™: Sport Concussion Assessment Tool.
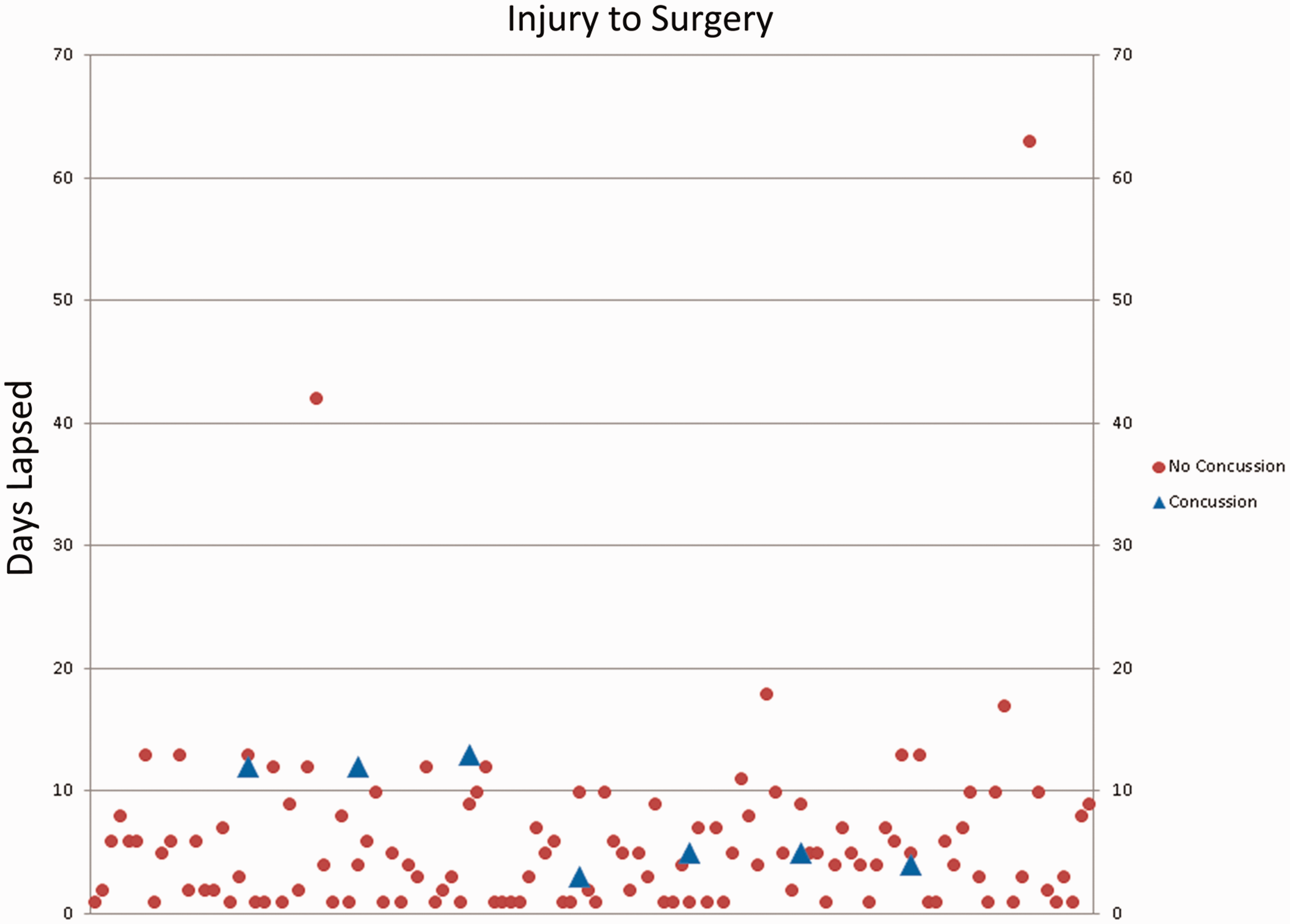
Total number of days from injury to surgery.
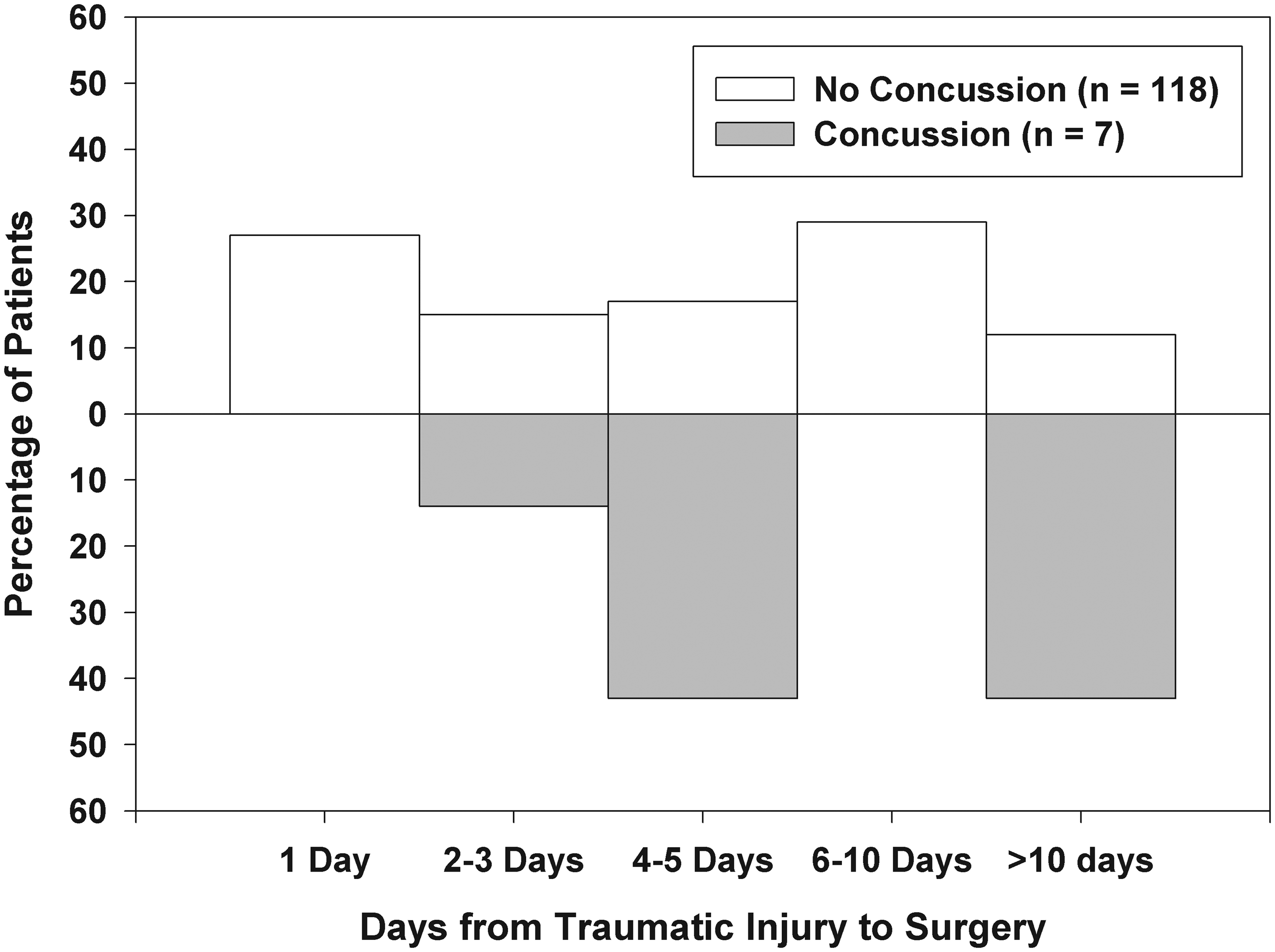
Percentage of enrolled patients with and without concussion.
The number of days from injury to surgery ranged from three to 13 (Figure 1). Figure 2 shows the percentage of enrolled patients with and without concussion with respect to time from injury to surgery. The group of patients with concussion had significantly longer waiting times (Pearson chi-square = 10.99, four degrees of freedom, P = 0.027) than the group without concussion, particularly in the category longer than 10 days from injury.
Among the seven patients with concussion the interval between injury and surgery was as follows: one patient (14%) was 2–3 days from injury, three (43%) patients were 4–5 days from injury, and three (43%) were seen >10 days after injury. In comparison, among those without concussion, the interval between injury and surgery was as follows: 27% within one day from injury to surgery, 15% between two and three days, 17% between four and five days, 29% between six and 10 days, and 12% >10 days.
The anesthetic records of patients with concussions revealed no adverse intraoperative hemodynamic or respiratory events. Neither phase-one (discontinuation of anesthetic agents to recovery of protective reflexes) nor phase-two (intermediate recovery to discharge) recovery periods were prolonged. The planned postoperative disposition was not altered in any patient after general anesthesia nor was any patient readmitted after hospital discharge. On follow-up, only one patient had concussion symptoms that persisted beyond four weeks, but this patient was subsequently noted to be positive for Lyme disease and posttraumatic stress disorder related to a motor vehicle accident, so the etiology of ongoing symptoms was unclear.
Discussion
In this study, we found that the prevalence of recent concussion diagnosed during the preoperative period for children undergoing semielective orthopedic surgery was approximately 6%. We did not observe an adverse impact of surgery with general anesthesia in these patients. However, we did identify two important contemporary aspects of this population: only two-thirds of the at-risk population had received instruction on sports-related concussion and, as a group, all injured subjects when questioned recalled a blow to the head that resulted in the symptoms that occurred.
Concussions account for 8.9% of high school athletic injuries with an incidence of 0.23 per 1000 exposures and 5.8% of collegiate athletic injuries with an incidence of 0.43 per 1000 exposures. 12 The prevalence of 6% in our preoperative population, and the wider PHIS population, is entirely consistent with these data. The clinical implication is clear: perioperative clinicians should be aware of patients at risk in their practice. In particular, individuals with a concussion are at risk of significant deterioration in the event of a “second collision,” and if elective anesthesia were to represent such an event, it is significant in that greater than 50% of our cases underwent surgery within five days of injury. 13
A second finding in our study is the pediatric concussions are difficult to diagnose as signs and symptoms may be vague and identification of the condition often relies on self-reporting in a population where many neglect to disclose their head injury to a medical professional. 12 The diagnosis of a concussion is therefore generally based on the clinical assessment by a healthcare professional evaluating symptoms, activity at time of injury, and physical examination. Disturbance in brain function caused by a direct or indirect force to the head resulting in a variety of nonspecific signs or symptoms may not always involve loss of consciousness but may result in presence of headache, gait unsteadiness, impaired brain function (e.g. confusion), or abnormal behaviors (e.g. change in personality). 14 In our study, we found that two-thirds of the children and adolescents questioned had been trained in the recognition of concussion, and all those experiencing concussion at the time of injury stated this on direct questioning. This finding likely reflects recent Massachusetts legislation requiring any school athlete or marching band member to participate in an annual head injury safety training program. 15 Studies from outside Massachusetts show that more than 30% of athletes do not recognize their symptoms as concussion.16,17–19 Our observation therefore has relevance to public health. In addition, for the practicing clinician the message is clear: be direct and ask the patient or caregiver about concussion symptoms at the time of injury or prior to scheduling a surgical procedure.
Avoidance of a secondary injury is essential in the management of patients with concussions. The initial concussive insult causes a cascade of pathological events leading to cerebral dysfunction without significant cell death. Injury to cells causes an ionic imbalance and excessive neurotransmitter release, which is further compromised aberrant cerebral blood flow (CBF) due to altered cerebral autoregulation and vasospasm.4,20 There is an inflammatory response with an influx of neutrophils, monocytes, and lymphocytes traveling across the blood–brain barrier and releasing inflammatory cytokines which can exacerbate cell injury.
Although the impact of surgery and general anesthesia on the progression of injury in patients with concussion is unknown, preclinical data reveal activation of inflammation and disruption of the blood–brain barrier.21,22 Volatile anesthetics also suppress cerebral metabolism in a dose-related manner, but these agents also possess intrinsic cerebral vasodilatory activity as a result of direct effects on vascular smooth muscle. 23 General anesthesia is also frequently associated with alterations of blood pressure and arterial partial pressure of carbon dioxide, and large volumes of intravenous fluids may be administered in response to surgical blood loss, hypotension, and anesthesia-induced vasodilation. In this context, little is known about the safety of anesthesia and surgery in the early period following a concussion.
In a prospective controlled cohort study of children with mild TBI to examine CBF in association with the various clinical recovery patterns both symptomatic and asymptomatic patients underwent arterial spin labeling MRI to quantify CBF 40 days after their concussive injury. Altered CBF patterns were seen in the mTBI groups; specifically, symptomatic children had higher CBF while asymptomatic patients had decreased CBF. This reduction of CBF in this study subgroup possibly suggests that clinical recovery can precede cerebral recovery. 3 Additional studies have reported a significant decrease in CBF at both 24 h and eight days. These perfusion disturbances can increase neurologic vulnerability to secondary injury whether from another physical injury or from a physiologic derangement that can occur during surgery or general anesthesia. Furthermore, while these and other studies demonstrate a change in CBF with concussion injuries, the duration, correlation with symptoms, and the clinical implications of these CBF changes are uncertain.
Given these concerns in preclinical models of concussion, there is now an extensive literature about “return to play” criteria after sport-related concussion and “return to learn” instructions in school-aged children.5,24 However, the ideal process of dealing with recovery from concussion may be complicated by the need for a surgical procedure under general anesthesia. For example, some individuals may have also sustained an orthopedic injury that requires semielective surgery.25,26 In these circumstances the best clinical course of action for optimizing the potential for brain repair and recovery is unknown.5,24 It is possible that effects of surgery and general anesthesia at such a vulnerable time may be detrimental. Hence, the clinical dilemma is balancing perceived risks and benefits.
There are three main limitations to our pilot study. The population is small and the prevalence of concussion is low. The absence of postoperative SCAT3™ or Child SCAT3™ in patients with a positive finding of preoperative concussion is also a limitation since it prevents us from making any conclusions about the effects of surgery and anesthetic agents. Last, we have relied on self-reporting when assessing symptoms.
In summary, the prevalence of recent concussion diagnosed during the preoperative period for children undergoing semielective orthopedic surgery was approximately 6%. The impact of surgery with general anesthesia, either favorable or unfavorable, in this population is unknown. Using this prevalence as a reference, the next step in assessing the impact of surgery and general anesthesia on the trajectory of recovery following concussion would be to measure neurocognitive function before and after administration of operative procedures in a larger population with a recent concussion compared with controls.
What is known on this subject
Patients who sustain simultaneous orthopedic injury and concussion in a recreation-related event may require semielective surgical treatment. The optimal time for scheduling such a procedure and the effects of general anesthesia are unknown.
What this study adds
Concussion without loss of consciousness may go unrecognized. This report assesses the prevalence of recent sport concussion, identified or not preoperatively, in a pediatric surgical population scheduled to undergo semi-elective surgical treatment of orthopedic trauma.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
