Abstract
Background
In Ethiopian traditional medicine,
Aim of the study
To evaluate the wound healing activity of crude extract of the leaves of
Methods
Results
Treatment of wounds with ointments containing 5% and 10% crude extract showed significantly increased wound contraction rate, shorter epithelialization period, and higher skin-breaking strength (P < 0.05) compared with the negative control. Both 5% and 10% formulations of the aqueous and ethyl acetate fractions significantly increased wound contraction and decreased the period of epithelialization in the excision wound model (p < 0.05), however, the chloroform fraction showed no significant wound healing effect compared with the negative control.
Conclusion
The 80% methanol crude extract as well as the aqueous and ethyl acetate fractions of
Plain language summary
Background
A wound is defined as the disruption or damage to the structural and functional integrity of living tissues. This disturbance leads to an alteration in the typical anatomy and functioning of the skin.1–3 Wounds result from a rupture in skin epithelial integrity and can be open or closed. Open wounds, the most common type, involve a break in the skin, exposing underlying tissue to infection.
4
Wounds can occur as part of a disease process or have an accidental or intentional etiology.2,5 Additionally, wounds can be classified as acute or chronic.
6
Wound healing occurs through a coordinated physiological response of four overlapping but well-defined phases which include hemostasis, inflammation, proliferation, and remodeling.
7
In various regions of Ethiopia such as Gubalafto,
11
Tara Gedam,
12
Dega Damot,
9
Debark Woreda,
13
Fiche
14
and Kunama,
15
A previous in vitro study was conducted with supportive results to the medicinal claim of the plant for wound treatment. The ethanolic extract of
Materials and methods
Drugs and chemicals used in the study
Drugs, chemicals, and reagents of analytical grade were used. Methanol absolute (AppliChem, Darmstadt, Germany), chloroform (Nice Chemicals Pvt. Ltd, Kochi, Kerala, India), ethyl acetate (Carlo Erba Reagent S.A.S., Val-de-Reuil, France), nitrofurazone skin ointment 0.2% (Shanghai, General Pharmaceutical CO., LTD, Shanghai, China), wool fat (Uni-Chem chemical reagents, Mumbai, Maharashtra, India), hard paraffin (University of Gondar, Pharmaceutics Laboratory, Gondar, Ethiopia), white soft paraffin (Ethiopian Pharmaceuticals Manufacturing, SH.CO, Addis Ababa, Ethiopia), cecostearyl alcohol (Blulux Laboratories (P) Ltd, Hyderabad, Telangana India), silver sulfadiazine cream USP 1% (Galentic Pharm Pvt. Ltd, Baddi, Himachal Pradesh, India), ketamine hydrochloride injection (Neon Laboratories Limited, Mumbai, Maharashtra, India), diazepam injection (Gland Pharma Limited, Hyderabad, Telangana, India), halothane inhalation (Piramal Enterprises Limited, Mumbai, Maharashtra, India), distilled water (University of Gondar, Pharmaceutics Laboratory, Gondar, Ethiopia) and bees wax (Golla Bee Products PLC, Addis Ababa, Ethiopia) were used during the experiment.
Plant materials
The fresh leaves of
Experimental animals
Healthy, adult Swiss albino mice of both sexes (25 ± 10 g, and 6–8 weeks of age) and adult healthy female Wistar rats weighing 150–200 g and 3–4 months of age were purchased from the Ethiopian Public Health Institute. Mice were used for the evaluation of wound healing activity, and rats were used for acute dermal toxicity tests. Female rats were used for toxicity studies due to their larger size and advanced skin structure, which facilitates the observation of dermal reactions. Conversely, mice were used in wound healing studies due to their ease of handling compared with rats. The animals were housed in cages under standard conditions with 12 h light and dark cycles. They were provided with a standard pellet diet and water ad libitum and acclimatized to the laboratory condition for a week before the start of the experiment. Animals were handled according to international laboratory animal use and care guidelines throughout the experiment. 18 At the end of the experiment, the animals were sacrificed with an overdose of anesthetics. 19
Crude extract preparation
The leaves of
Solvent fractionation
Ninety grams of the 80% hydro-methanol crude extract underwent successive extraction with chloroform, ethyl acetate, and aqueous solvents with increasing polarity respectively. The dried crude extract (90 g) was suspended in 500 ml of distilled water and transferred to a separator funnel. Chloroform was added, shaken vigorously and the resulting chloroform fraction was collected. This step was repeated twice. The remaining aqueous portion was then treated with ethyl acetate, with the upper ethyl acetate layer separated and collected. This process was also repeated twice. Finally, chloroform and ethyl acetate fractions were concentrated using a rotary evaporator and dried at 40°C to obtain the respective fractions. The remaining aqueous residue was frozen in a freezer overnight and then freeze-dried with a lyophilizer to obtain an aqueous fraction. All fractions were stored in screw cap vials in a refrigerator at −4° C until used for the formulation of ointments. 12
Ointment formulation
Medicated ointments of 80% methanol extract as well as chloroform, ethyl acetate, and aqueous fractions and the simple ointment (non-medicated ointment) were freshly prepared on the day of the experiment for each wound model based on British Pharmacopeia. 21
A hundred grams of simple ointment base was prepared by using the reduced formula from British Pharmacopeia (Table 1). Five grams of hard paraffin and five grams of cecostearyl alcohol were melted in a beaker. 5 g wool fat and 85 g white soft paraffin were melted in another beaker. The mixtures were then combined and stirred until cooled. To prepare the extract ointment, first the extracts were powdered in a mortar and pestle, then 5 g and 10 g of the 80% methanol extract were mixed with 95 g and 90 g simple ointment bases for preparing 5% w/w and 10% w/w crude extract ointment respectively by levigation on the surface of the ointment slab to make an ointment of uniform consistency and smooth texture. In the same manner, the 5% w/w and 10% w/w ointments of each fraction were prepared by incorporating 2.5 g and 5 g of the aqueous, ethyl acetate, and chloroform fraction each into a 47.5 g and 45 g of simple ointment base to get a 50 g medicated ointment of each fraction. Finally, the medicated ointments were transferred to a clean container for topical application during the experiment. 22
Formula used for the preparation of simple and medicated ointments.

MF, Master formula. RF, Reduced formula.
Preliminary phytochemical screening
The hydro-methanol extract and its chloroform, ethyl acetate, and aqueous fractions of the leaves of
Acute dermal toxicity study
Acute oral toxicity study was previously done in rats and up to a dose of 7.1 g/kg was not toxic.
16
Acute dermal toxicity test of 80% methanolic extract of
First, a sighting study was performed to determine the starting dose by applying 2000 mg/kg of the 10% extract ointment. There was no death or skin irritation observed within 24 h, and then four additional rats from each group were used, and the same dose of the crude extract ointment was applied. The 10% ointment formulation of the extract and the control non-medicated ointment were applied uniformly over the shaved area of test and control rats respectively, and observed for 24 h. During the exposure period, rats were caged individually. At the end of the exposure period, the residual test substance was washed out by distilled water and the animals were observed for the development of any adverse skin reactions daily for 14 days. 20 The reactions, defined as erythema and edema, were evaluated and graded according to the OECD 404 grades. 29
Grouping and dosing of experimental animals
For the evaluation of crude extract, animals were grouped into four groups for excision, five groups for incision, and another four groups for burn wounds (six animals per group). For the excision wound model, the first group was treated with simple ointment (served as a negative control), the second and third groups were treated with 5% w/wand 10% w/w crude extract ointment, respectively, and the fourth group was treated with nitrofurazone, 0.2%w/w (served as a positive control). 30
In the linear incision wound model, Group I-IV were treated similarly to the excision wound model, but animals in Group V were left untreated (served as untreated negative control). 31 For evaluation of burn wound healing activity, the animals in Group I-III were treated in a similar fashion with the excision wound model, but animals in Group IV were treated with 1% silver sulfadiazine cream (served as a positive control). 32
To evaluate the activity of the solvent fractions in the circular excision wound model, eight groups of mice (each with six) were used. The excision wound model was selected because it is an ideal method to study physical attributes like wound contraction, epithelization, and scar remodeling. 33 Group I was treated with simple ointment, Group II and III were treated with 5% and 10% of aqueous ointment, respectively, Group IV and V were treated with 5% and 10% of ethyl acetate ointment, respectively, Group VI and VII were treated with 5% and 10% of chloroform ointment, respectively and Group VIII was treated with 0.2% nitrofurazone ointment.
Evaluation of wound healing activity
Circular excision wound model
The mice were weighed individually and anesthetized with intraperitoneal 50 mg/kg ketamine and 5 mg/kg diazepam before infliction of the wound. Then, the hair from the dorsothoracic area of the animals was shaved using an electrical hair clipper. 32 A circular mark (314mm2) was prepared using a permanent marker. The full thickness of this circular mark was excised carefully using forceps and scissors to form an excision wound which was left undressed. After recovery from anesthesia, mice were returned to their cage. This was considered as day 0. After 24 h of wound creation, all preparations were applied topically to the wound area once per day until the wound was completely healed. For evaluation of wound healing activity of the aqueous, ethyl acetate, and chloroform fractions, the same wound area was created and ointments were applied as described in the grouping and dosing section.
The mice were observed for wound closure and measurement was done every two post wounding days using a transparent sheet and permanent marker. The evaluated surface area was used to calculate the percentage of wound contraction, taking the initial size of the wound as 100%. The wound healing activities of the crude extract were assessed by the period of epithelialization, percentage of wound contraction, and histological studies while the parameters in the case of solvent fractions were period of epithelialization, and percentage of wound contraction.34–36
The percentage of wound contraction was calculated as follows
37
;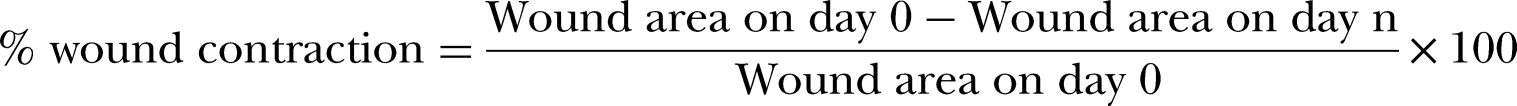
The number of days required for the eschar to fall off from the wound surface exclusive of leaving a raw wound behind was taken as the end point of complete epithelialization, and the days required for this were considered a period of epithelialization. 38
Linear incision wound model
All mice were anesthetized and shaved as in the excision wound model. Then, a 3 cm long, linear and paravertebral incision was made through the full thickness of the skin on either side of the vertebral column at a distance of 1 cm from the midline. The wound edges were apposed and sutured with non-absorbable surgical thread and a curved needle (no. 11) at intervals of 1 cm. The first four groups were treated similarly to the groups in the excision wound model, and the fifth was used as untreated control. The treatments were topically applied once daily for 9 days. The sutures were removed on the 8th day of post-wounding. Tensile strength (the force required to open the healing skin) was assessed to measure the extent of healing.
39
The tensile strength was measured on day ten (Figure 1) through a continuous water flow technique by considering the gram of water required to break the skin
40
and the breaking strength of the groups treated with extracts was compared with the standard, simple ointment and untreated control groups. The tensile strength was calculated as follows.
20


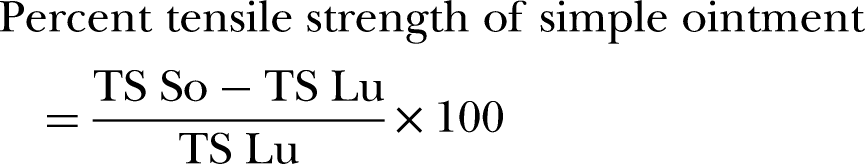

Photograph of incision wound on day 0 (A) and measurement of tensile strength on the 10th day by using water flow technique (B).
Where So = simple ointment and Lu = left untreated
Burn wound model
Initially, the mice were divided randomly into four groups of six mice, then anesthetized through intraperitoneal injections of ketamine (50 mg/kg) plus diazepam (5 mg/kg). 41 The hair on the dorsum of each mouse was shaved off to ensure even burn wounding. Then, a molten bees’ wax (2gm) at 80◦C poured into a metal cylinder with 314mm2 circular opening was placed on the back of the animal to inflict a partial thickness burn wound. On solidification of wax after 8 to 10 min, the metal cylinder with wax adhered to the skin was removed and left a markedly circular burn wound (Figure 2). Wound contraction rate and epithelialization period were used as parameters for the evaluation of burn wound healing activity. 32

Circular burn wound on day 0.
Animal dissection, tissue collection, and histological processing
For histological studies, a skin specimen from each group in the excision wound model was collected on the 13th day of post-wounding after the mice were sacrificed with an overdose of diazepam and ketamine (four times the anesthetic dose intraperitoneal). 42 The examination was blindly done and a vertical midline incision at the wound site from superior to inferior was performed. Samples were fixed in 10% buffered formalin, processed, and blocked with paraffin and then were sectioned into 5-micrometer sections and stained with hematoxylin and eosin (HE) stains, then the slides of the skin tissues were examined by light microscope for epidermal or dermal remodeling. 43
Statistical analysis
The data were expressed as mean ± SEM. The result was statistically analyzed using one-way ANOVA followed by post hoc Tukey-tests with SPSS version 23 software, and a P value < 0.05 was considered as statistically significant.
Results
Screening of phytochemicals
The percentage yield of the crude methanol extract was 19%, and the solvent fractionation produced 57.8%, 28.3%, and 13.9% yield of aqueous, ethyl acetate, and chloroform fractions, respectively. Phytochemical screening of the crude extract and solvent fractions showed the presence of different secondary metabolites as shown in Table 2.
Phytochemical screening of the crude extract and solvent fractions of

(+ = Present, - = absent).
Acute dermal toxicity
Topical application of the maximum concentration (10%) ointment formulation of the crude extract using a limit dose of 2000 mg/kg did not show any sign of edema and erythema in rats. Additionally, no signs of toxicity and no mortality were observed during the 14 days of observation.
Wound healing activity of the crude extract on excision wound
Contraction of wound and period of epithelization
As shown in Table 3, treatment with 10% crude extract and nitrofurazone 0.2% ointment significantly enhanced wound contraction by the second day compared to the control group. Mice treated with 5% crude extract ointment exhibited significant wound contraction from the fourth day onward. Both 5% and 10% plant extract ointments, along with nitrofurazone 0.2% ointment, significantly facilitated wound contraction from the sixth to the sixteenth day compared to the control group. There was no significant difference in wound healing activity between the standard drugs, 10%, and 5% crude extracts. Animals treated with 5%, 10% (w/w) extract, and nitrofurazone ointments showed a significant reduction in epithelization period compared against the negative control (23.39%, 33.91%, and 27.96%, respectively, p < 0.05).
Effect of topical application of 80% methanolic crude extract of the leaves of

Each value denotes the mean ± SEM (n = 6 mice in each group) and is analyzed by one-way ANOVA followed by post hoc Tukey test; * p < 0.05, **p < 0.01, ***p < 0.001 when compared with the negative control group. SO = simple ointment base; MLE = methanol leaf extract; NFO = nitrofurazone ointment; EP = epithelization period.
Histopathological Analysis
Granulation tissue of healed wounds in standard and 10% w/w extract treated groups showed more organized collagen fiber and fewer concentrations of inflammatory cells compared with the negative control group. Negative control groups had fewer collagen fibers, and more inflammatory cells, and thus showed delayed wound healing processes (Figure 3).

Photomicrograph of hematoxylin and eosin staining of tissues from excision wound model in mice. (A) Mice treated with negative control (HE ×40). (B) Mice were treated with the standard treatment of nitrofurazone (HE X 40). (C) Mice treated with 5% methanolic leaf extract ointment (HE ×40). (D) Mice treated with 10% methanolic leaf extract ointment (HE ×40) C = Collagen fiber, D = Dermis, E = Epidermis, HF = Hair follicle, BV = Blood vessels, F = Fibrocytes.
Wound healing activity of the crude extract on incision wound
Tensile strength
As shown in Table 4, both 5% and 10% ointment preparations of crude extract significantly increased tensile strength compared to negative controls (p < 0.001). The 10% extract group exhibited the highest percentage of tensile strength among all treatments.
Effect of topical application of 80% methanolic crude extract ointment of

Note: Values are expressed as mean ± SEM (n = 6 mice in each group) and analyzed by one-way ANOVA followed by post hoc Tukey test; a, compared to the untreated group, b, compared to the simple ointment treated group; *p < 0.001.
Wound healing activity of the crude extract on burn wound
Contraction of wound and period of epithelization
The 10% (w/w) extract ointment-treated group showed significant (p < 0.01) wound contraction starting from the 2nd day to 18th day, whereas the 5% (w/w) extract showed significant (p < 0.05) wound contraction effect starting from the 4th day to 18th day in comparison with the negative control group (Table 5). A higher rate of wound closure was observed with the standard drug (100% at day 18) followed by 10% (w/w) ointment (99.34% at day 18). Wound healing with complete wound closure was observed in standard drug and 10% (w/w) extract ointment treated groups within 18 and 19 days, respectively. However, the period of wound closure in the negative control group was beyond 19 days.
Percentage of wound contraction of partial-thickness burn wounds treated with extracts of
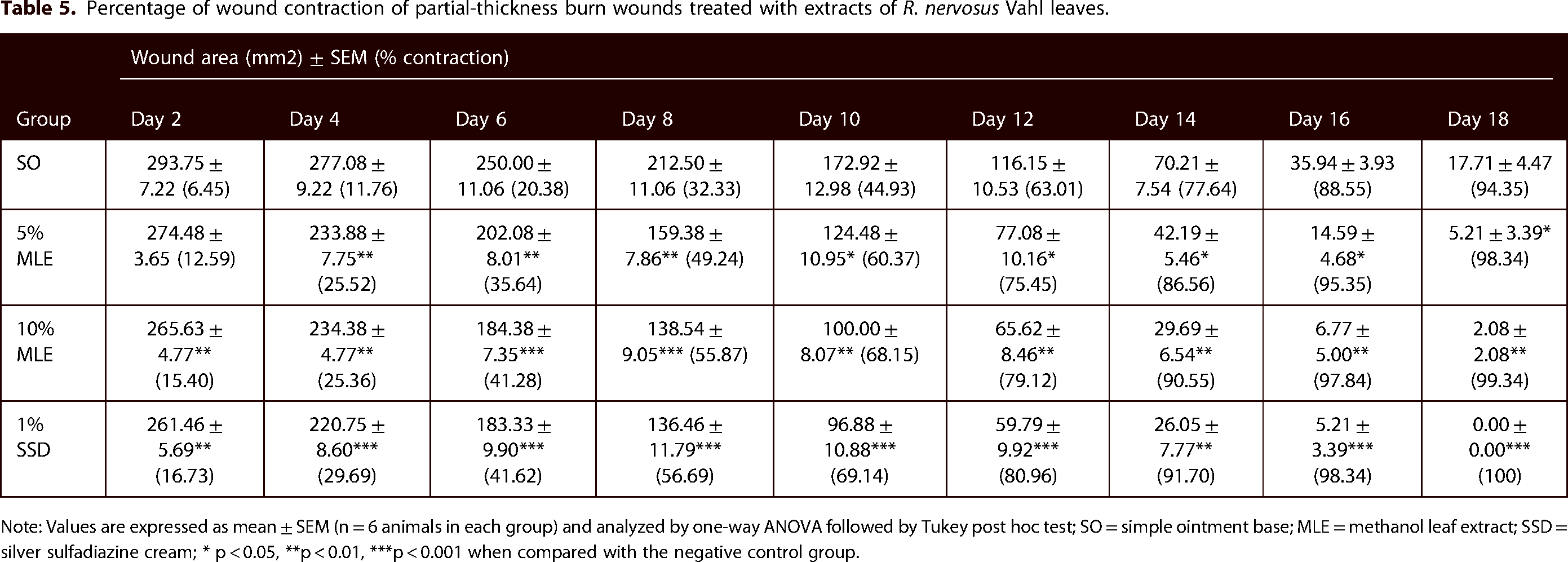
Note: Values are expressed as mean ± SEM (n = 6 animals in each group) and analyzed by one-way ANOVA followed by Tukey post hoc test; SO = simple ointment base; MLE = methanol leaf extract; SSD = silver sulfadiazine cream; * p < 0.05, **p < 0.01, ***p < 0.001 when compared with the negative control group.
The burn wound healing effects of 5% and 10% ointments were demonstrated by faster epithelialization. Both ointments significantly reduced epithelialization time compared to the negative control (p < 0.05 for 5% and p < 0.01 for 10%). The reduction in epithelialization time was dose-dependent. The average epithelialization periods were 17.83 days for the 5% extract, 16.5 days for the 10% extract, 16.33 days for the standard drug, and 20.17 days in the negative control group (Figure 4).
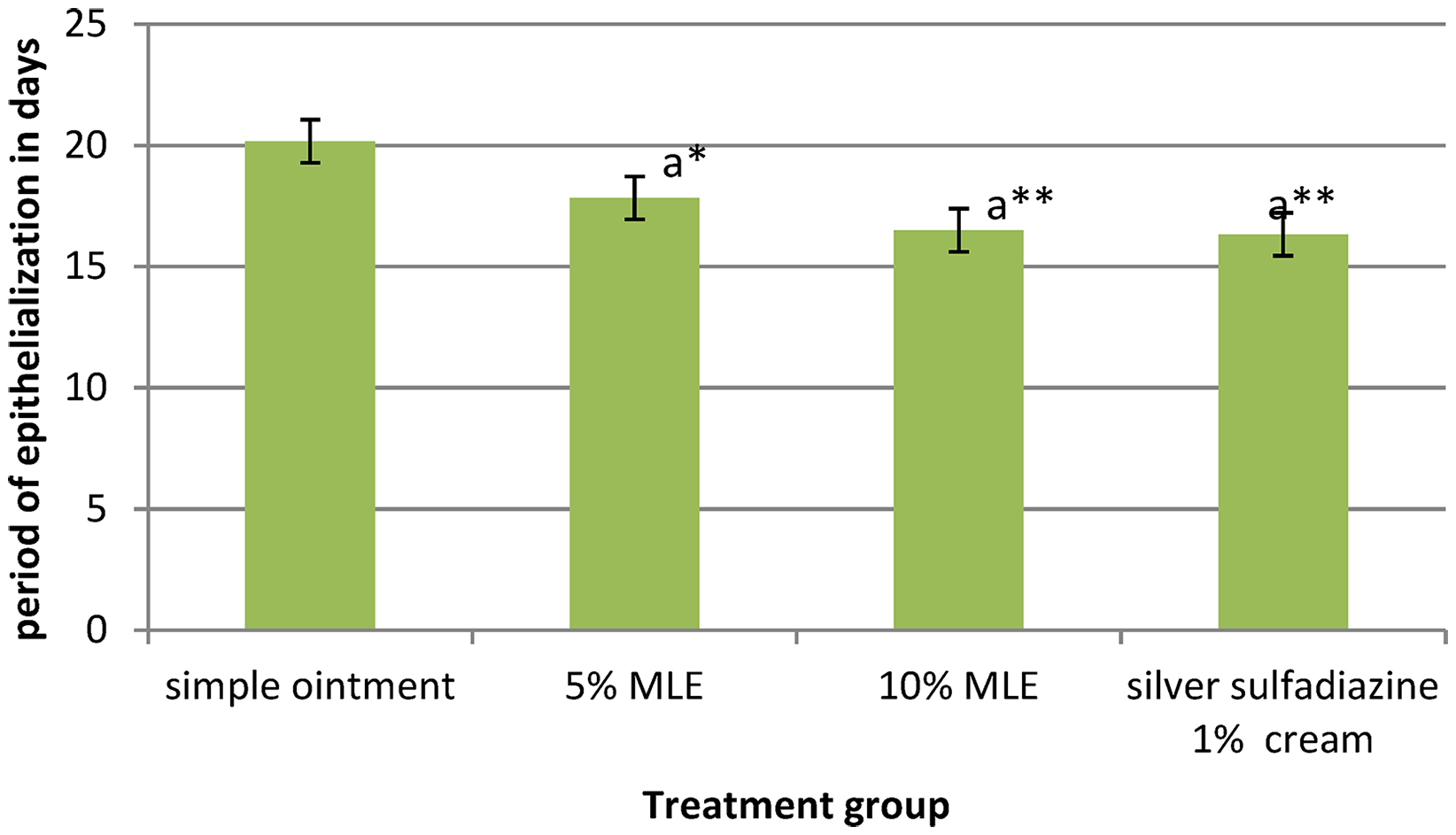
The effect of the crude extract on the period of epithelialization on burn model in mice. Note: values are expressed as mean ± SEM (n = 6 mice in each group) and analyzed by one-way ANOVA followed by post hoc Tukey test; a, compared to the negative control; * p < 0.05, **p < 0.01.
Wound healing activity of solvent fractions
Contraction of wound and period of epithelization
In the excision wound model, both aqueous and ethyl acetate fraction ointments showed wound healing activity. The 5% aqueous fraction ointment significantly improved wound contraction on most post-wounding days (p < 0.01). The 10% aqueous fraction ointment showed significant wound contraction from day 2 onwards (p < 0.01), highly significant from days 6 to 10 (p < 0.001), surpassing the positive control's effect except on day 12. Similarly, the 5% ethyl acetate fraction ointment significantly enhanced wound contraction from day 4 (p < 0.05), becoming highly significant from day 10 to 14 (p < 0.001) compared to the negative control. The 10% ethyl acetate fraction ointment also significantly improved wound contraction on most days (p < 0.01) compared to the negative control. However, ointments of the chloroform fraction did not show significant wound healing activity compared to the negative control. There was no statistically significant difference in the wound contractions between the three fraction ointments as depicted in Table 6.
Topical effect of solvent fractions of

Note: values are expressed as mean ± SEM (n = 6 mice in each group) and analyzed by one-way ANOVA followed by post hoc Tukey test; * p < 0.05, **p < 0.01, ***p < 0.001 when compared with the negative control; AQF = Aqueous fraction, EAF = Ethyl acetate fraction, CHF = Chloroform fraction.
As depicted in Figure 5, animals treated with the 10% w/w and 5% w/w ointments of each fraction and the standard drug had a shorter period of epithelialization compared to the control (simple ointment base). However, the epithelialization period showed by the chloroform fraction ointments was not statistically significant when compared to the negative control. Groups treated with the standard drug and 10% aqueous fraction ointments showed a faster rate of epithelialization (p < 0.001) compared to the negative control. In addition, mice treated with 5% and 10% ethyl acetate fraction and 5% aqueous fraction ointments showed shorter (p < 0.01) epithelization periods as compared to the control group. There was no significant difference between the treatment doses of the three fractions as well as with the standard drug. Animals treated with the standard drug and 10% w/w aqueous fraction ointment showed a faster rate of epithelialization (16.17 and 16.00 days respectively).

The effect of solvent fractions on the period of epithelialization. Note: Values are expressed as mean ± SEM (n = 6 mice in each group) and analyzed by one-way ANOVA followed by post hoc Tukey test; a, compared to the negative control; ** p < 0.01, ***p < 0.001.
Discussion
Wound healing is a complex and dynamic process of tissue repair which initially involves an acute inflammatory phase followed by the synthesis of collagen and other extracellular macromolecules and finally the formation of a scar. Drugs that influence one phase of the wound healing process, may not necessarily affect the other phase. 44 Therefore, the development of an ideal wound healing agent by targeting the different phases of the wound healing process is still a challenge to medical scientists. The ideal agent should meet the criteria such as rapid contraction of the wound area resulting in fast healing, reduction of the wound epithelization period, and achievement of improved tensile strength. 45
In the excision wound model of this study, both 5% and 10% ointments of the plant extract showed significant wound contraction compared to the control group. Although there was no statistically significant difference observed in wound healing activity between the standard drug and the 10% w/w or 5% w/w crude extract ointments, interestingly the 10% w/w extract ointment exhibited a better observable effect in terms of wound contraction and epithelialization compared to the standard drug and the 5% w/w extract ointment. Previous in vitro study reported that methanolic extract of the leaves of
The wound healing activity of the crude extract was evidenced by increased tensile strength in incision wounds of mice. Tensile strength indicates how much the repaired tissue resists opening under tension and may indicate the quality of the repaired tissue.
47
The increased tensile strength can be due to the stimulation of collagen synthesis and its maturation, angiogenesis, and stabilization of fibers.48,49 According to a previous phytochemical study,
The mechanisms of plant-derived compounds in the treatment of burn wounds include anti-inflammatory, antioxidant, antimicrobial, collagen synthesis stimulation, cell proliferative, and angiogenic actions. 52 As described earlier, previous studies indicated that the leaves of this experimental plant have antimicrobial, anti-inflammatory, and antioxidant activities which might contribute to the burn wound healing effect. In addition, burn injury partially suppresses the immune system. Therefore, the use of antioxidants may have a positive effect on the regeneration of the damaged skin tissue and other burn wound complications. 53
In the excision wound model, ointments prepared from aqueous and ethyl acetate fractions enhanced wound contraction. Increased contraction rate accelerates wound healing by reducing wound area, and reduced wound area facilitates re-epithelization by shortening the distance keratinocytes must migrate. 54 Additionally, the epithelization time was significantly reduced in animals treated with aqueous as well as ethyl acetate fraction ointments. Wound re-epithelization occurs due to the proliferation and migration of epithelial cells across the wound bed. 55 Therefore, the shorter epithelization time in the aqueous and ethyl acetate fraction could be due to the facilitated proliferation of epithelial cells. Unlike the aqueous and ethyl acetate fraction ointments, the chloroform fraction did not show a significant wound healing activity. This could be due to the absence of wound healing phytochemicals such as tannins, terpenoids, flavonoids, saponins and glycosides in the chloroform fraction as evidenced by the preliminary phytochemical analysis of this study. Tannins improve wound healing by facilitating tissue regeneration through their antioxidant activity, 56 and the wound-healing effect of flavonoids is related to their antibacterial and antioxidant activities. 57
The wound healing activity of phenolic compounds is due to their antioxidant, anti-inflammatory, and antimicrobial activities. 58 Similarly, terpenoids inhibit inflammatory mediators by inhibiting phospholipase A2 in the metabolism of arachidonic acid, 59 and saponins have membrane stabilizing and anti-inflammatory activity. 60 Glycosides have antimicrobial, anti-inflammatory, antitumor, and antioxidant actions. 61
Conclusion
The crude 80% methanol extract of
Footnotes
Acknowledgement
We are thankful to University of Gondar for funding this study.
Authors’ contributions
All authors made substantial contributions to conception and design, analysis and interpretation of data; took part in drafting the article and revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval and consent to participate
The experiment was conducted in accordance with the Guide for the Care and Use of Laboratory Animals, 41 and the study has been approved by Department of Pharmacology, College of Medicine and Health sciences, University of Gondar with a reference number of SOP4/106/11.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded by University of Gondar. The funder has provided drugs, chemical and laboratory animals required for this study. Additionally, the funder provided financial support to cover per dime costs of investigators.
How to cite this article
Abel A, Kefyalew AG, Bahiru TG, et al. Evaluation of wound healing activity of the crude extract and solvent fractions of Rumex nervosus Vahl (Polygonaceae) leaves in mice. Scars, Burns & Healing, Volume 11, 2025. DOI: 10.1177/20595131251316791.
