Abstract
Blood samples were collected serially from 14 women with healthy pregnancies, beginning in gestational week 4 at the time of a positive pregnancy test through to the identification of a foetal heart by ultrasound. Six biomarkers were measured in the serum retrospectively including two reproductive hormones (progesterone and human chorionic gonadotrophin (hCG)) and four additional biomarkers (prostate-specific antigen (PSA), cancer antigen 15-3 (CA15-3), cancer antigen 125 (CA125) and pregnancy-associated plasma protein A (PAPP-A)) measured on a Siemens Centaur XP and a Roche Cobas e411 automated analysers, respectively. The progesterone and hCG results were unremarkable following established patterns, but distinctive patterns of change were seen in the other four biomarkers during this period of early pregnancy. PAPP-A and PSA levels rose steadily as the pregnancies progressed, while CA125 levels rose until week 5.5 and then returned to baseline values. CA15-3 serum concentrations were observed to drop as the pregnancies progressed. These biomarker results suggest further investigation is warranted to allow a non-invasive correlation of the biomarkers with the various stages of embryogenesis, implantation and placentation.
Introduction
The first few weeks of human pregnancy are characterized by rapid and synchronized developments in embryogenesis, implantation and placentation (Norwitz et al., 2001). Unfortunately, non-invasive imaging techniques between 2 and 5 weeks after ovulation are often limited technically to measurements of embryonic size and gestational sac volume (Rousian et al., 2010, 2011) aimed at predicting foetal outcome (Oh et al., 2002). A number of biomarkers are used to monitor physiological processes in reproductive medicine (Palmer and Barnhart, 2013), and these can be used to reveal pathophysiology when used either alone or in combination with other biomarkers.
While most biomarkers have a principal association with a particular disease, some are not always specific for that disease but can be found in unexpected situations or used in the detection and monitoring of apparently unrelated conditions. Serum biomarkers in early pregnancy may prove useful in revealing some of the changes that occur following implantation during embryogenesis and placentation, and the availability of validated reagents for the measurement of a number of novel tumour markers (Wu et al., 2007) and established markers of pregnancy (Pillai et al., 2016) may well provide this opportunity of monitoring non-invasively the different events in early pregnancy. The present study therefore measured, in addition to the recognized reproductive hormones human chorionic gonadotrophin (hCG) and progesterone, four biomarkers (pregnancy-associated plasma protein A (PAPP-A), prostate-specific antigen (PSA), cancer antigen 15-3 (CA15-3) and cancer antigen 125 (CA125)) that have been linked directly or indirectly with female reproduction. PAPP-A is useful in a combined test with free β-hCG and foetal nuchal translucency for the identification of increased risk of Down’s syndrome (Avgidou et al., 2005) and miscarriage (Rissanen et al., 2006), although it is not regarded as being adequate as a screen on its own for pregnancy viability (Brameld et al., 2008). PSA is a usual choice as it is more familiar as a marker for prostate cancer in men (Armbruster, 1993; Schröder et al., 2012) but a peptidase that has curiously been associated with breast tissue and shows temporal changes during the ovarian cycle in women (Diamandis and Yu, 1995). CA125 is principally used as a marker for ovarian cancer (Bast et al., 1981) but it has found a role in the non-invasive detection and monitoring of endometriosis (Pittaway and Fayez, 1986). CA15-3 is mainly used in the monitoring of women with breast cancer (Clinton et al., 2003; Duffy et al., 1999; O’Brien et al., 1994). It is a mucin-like glycoprotein encoded by the MUC1 gene and has a clear association with reproduction as MUC1 is heterogeneously expressed on the surface of epithelial cells, including those in the breast and upper reproductive tract, and is thought to prevent embryo implantation (Al-Azemi et al., 2009).
The present study therefore measured six serum biomarkers of pregnancy, two reproductive hormones (progesterone and hCG) and four additional biomarkers linked with female reproduction (PSA, CA15-3, CA125 and PAPP-A) in healthy women during the early stage of a viable pregnancy from the time of a positive pregnancy test to 7 weeks’ gestation. Results were analysed relative to the last menstrual period in an attempt to identify any longitudinal changes that may provide insight into the physiological processes occurring at this time of the pregnancy.
Materials and methods
Ethical approval, including approval of patient information sheets and consent forms, was approved by both the Joondalup Health Campus Research Ethics Committee and the Edith Cowan University Human Research Ethics Committee. All blood samples were taken as part of the routine management of the women at Fertility North, but consent was sought for the analysis of additional compounds not indicated medically. The data from this study formed part of a thesis submitted to Edith Cowan University towards a master of science degree which has now been awarded.
Patients
Consecutive women with a positive pregnancy test between 1 February 2012 and 31 July 2012, and with no evidence of cancer (clinical history and examination) or endometriosis (previous laparoscopy in the last 12 months), were approached during their routine clinical management to participate. The 14 pregnant women meeting the above entry criteria and agreeing to give consent for the additional tests had all conceived following fertility treatment, were routinely given progesterone supplements from the mid-luteal phase and were monitored until a foetal heart was seen on ultrasound. All pregnancies progressed uneventfully and resulted in the birth of a healthy singleton baby.
Sample processing and analysis
Blood was collected using syringes and transferred into 5-ml Vacutainer SST™ tubes (Becton Dickinson, UK) before delivery to the laboratory. The blood was allowed to clot at room temperature and then centrifuged at 1300 ×
Statistical analysis
The response variable (PSA, CA125, CA15-3 and PAPP-A) was log transformed before analysis. Gestation was included as a fixed effect factor and ‘Subject’ and ‘Time’ were modelled as random effects. The interaction between Group and Gestation was also modelled. The analyses were done using the R version 3.0.0 computing software (Team, 2013), models built using the ‘nlme’ mixed models package (Pinheiro et al., 2012) and graphics produced using the ‘ggplot2’ package (Wickham, 2009).
Results
Reproductive hormones
Results for progesterone and hCG levels, measured routinely in pregnancy, are shown in Table 1. They followed standard patterns of change, confirming that the modelling and expression of results according to the stage of pregnancy was appropriate.
Reproductive hormone concentrations (mean ± SEM) in early pregnancy.a
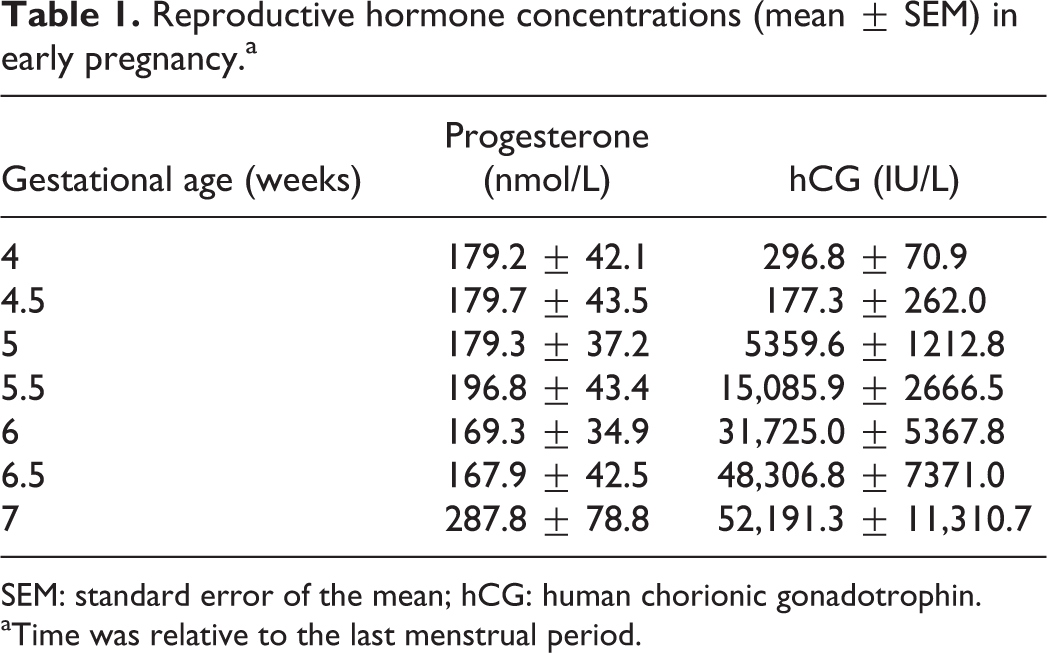
SEM: standard error of the mean; hCG: human chorionic gonadotrophin.
aTime was relative to the last menstrual period.
PAPP-A, CA125, PSA and CA15-3 during early pregnancy
The biomarker concentrations are shown in Table 2. Concentrations of PAPP-A increased steadily from 6.51 ± 0.56 mIU/L at 4 weeks to 125.38 ± 22.11 mIU/L at 7 weeks, and the changes seen were highly significant (
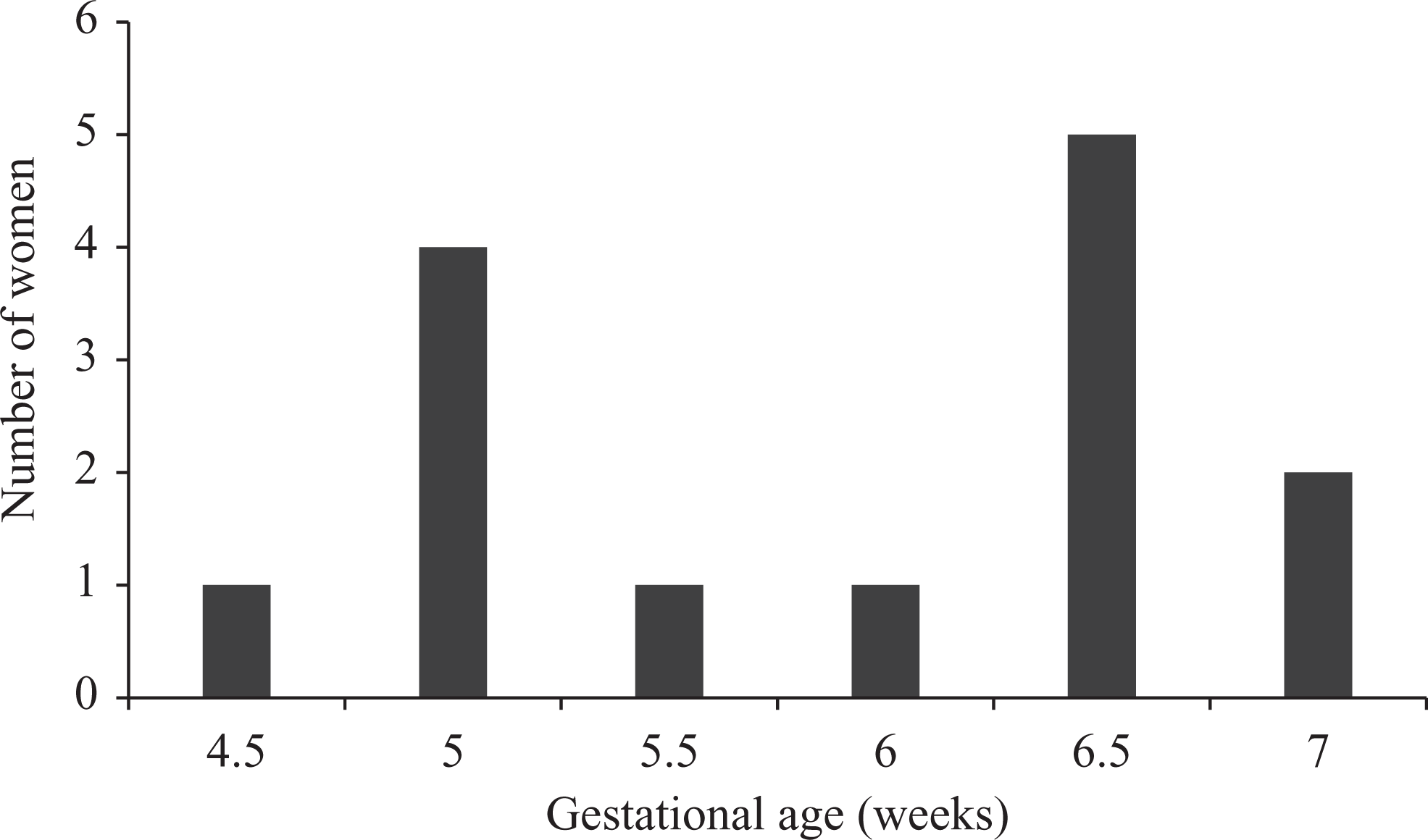
The frequency distribution of the time of the peak CA125 concentration identified in 14 pregnant women. The time was the gestational age relative to the last menstrual period. CA125: cancer antigen 125.
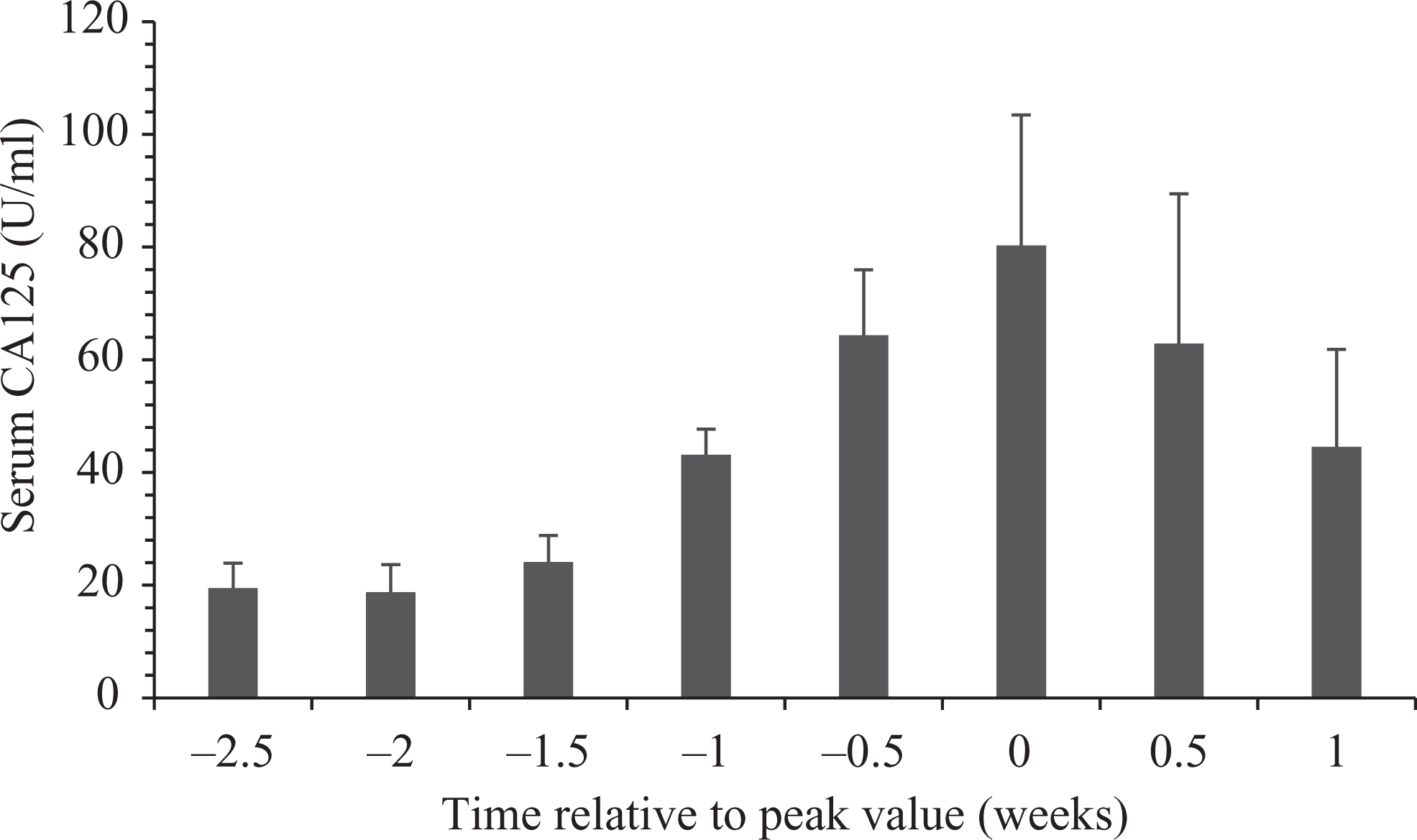
The CA125 concentrations (mean ± SEM) determined in the serum of 14 pregnant women. Time was relative to the maximum value for each woman. CA125: cancer antigen 125; SEM: standard error of the mean.
The biomarker concentrations (mean ± SEM) determined in the serum of 14 pregnant women.a
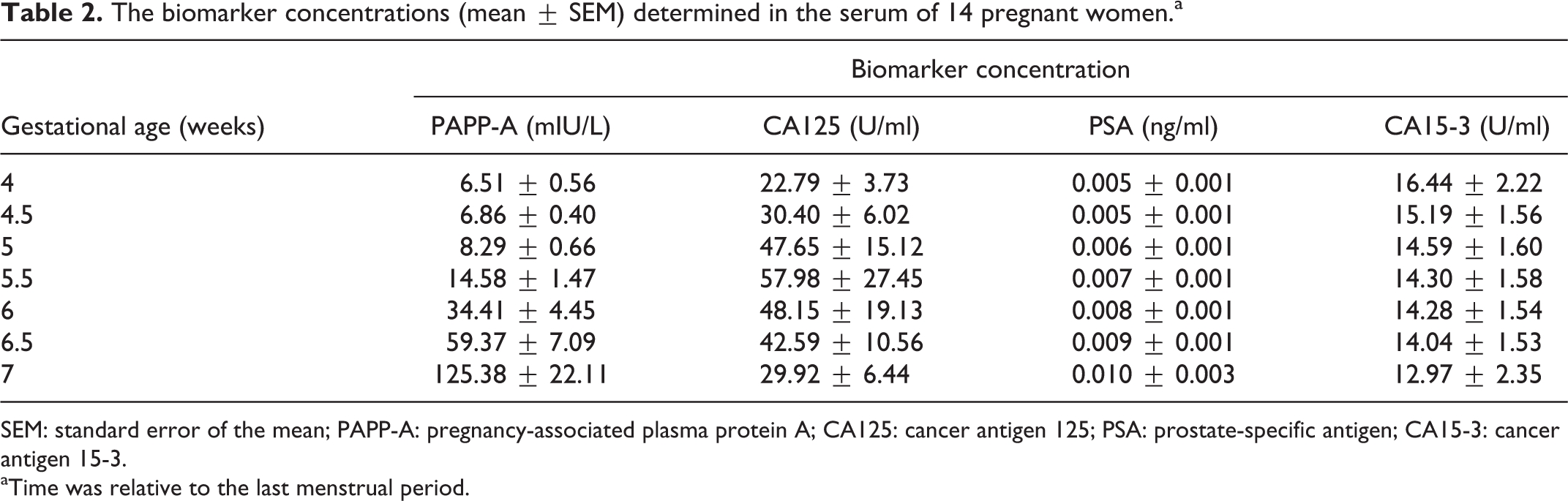
SEM: standard error of the mean; PAPP-A: pregnancy-associated plasma protein A; CA125: cancer antigen 125; PSA: prostate-specific antigen; CA15-3: cancer antigen 15-3.
aTime was relative to the last menstrual period.
Discussion
The use of serum markers requires consideration of both the technical capability of the assays, and the biological relevance of the marker under investigation. While biomarker immunoassays allow precise qualitative measurements to be made when measuring analytes, different assays can result in different numerical values due to differences in choice of reagent or their calibration. This is important when comparing work from different laboratories or over different time frames. For example, the expression of PAPP-A results in milli-international units per millilitre in the present study compared to microgram per litre elsewhere (Sinosich et al., 1982) and reflects the change in methodology and the move to a different standardization. CA125 has varied forms which presents a challenge to assay accuracy, and large differences in results can be seen between the Siemens and Panomics methods (McLemore et al., 2012). Between-method differences can occur with CA15-3 due to differences in calibration rather than specificity (Klee and Schreiber, 2004).
The pattern seen for progesterone and hCG reflects the pattern seen serially in individual women, and this gives confidence that the sampling strategy and data analysis did not have an adverse effect upon the findings. The relatively constant progesterone during early pregnancy was possibly due to the continued administration of exogenous progesterone as a luteal support until a foetal heart was observed. Changes during the ovarian cycles of these patients for the reproductive hormones and other biomarkers have been published previously, with CA125 and CA15-3 both being influenced by the stage of the ovarian cycle (Stemp et al., 2014, 2015). In the present study, different patterns of change were seen between the four biomarkers during early pregnancy, and presumably reflect different processes involved in implantation, embryogenesis and placentation. PAPP-A and PSA rose steadily as the pregnancy progressed, while CA125 rose until week 5.5 before returning to baseline values, while CA15-3 levels decreased during pregnancy.
PAPP-A has been described in normal pregnancy (Bersinger et al., 1986; Westergaard et al., 1983), and the findings in the present study that PAPP-A rises steadily as the healthy pregnancy progressed mirrors these earlier studies. However, it has been shown previously that healthy pregnancies following assisted reproduction have reduced PAPP-A levels in the first trimester compared to naturally conceived pregnancies (Amor et al., 2009). This biomarker is therefore giving information not apparent by other means and may be revealing some impairment of early implantation with some forms of assisted reproduction. Unfortunately, the lower levels found can also increase the risk of receiving a “false-positive” result at the routine first trimester screen and having an unnecessary chorionic villus biopsy or amniocentesis (Amor et al., 2009).
CA125, a high molecular mass mucin-type molecule, is a tumour biomarker that is used extensively to monitor epithelial ovarian cancer (Bast et al., 1981), but it also is found elsewhere such as during the ovarian cycle (Nonogaki et al., 1991), in association with endometriosis (Pittaway and Fayez, 1986), in pregnancies that are destined to miscarry (Azogui et al., 1996), and with pelvic inflammatory disease (Mozas et al., 1994). Consequently, concern has been expressed that this tumour marker can cross the clinical cut-offs for cancerous disease during normal reproductive function (Touitou et al., 1989). Indeed, 5/14 women in the current study had CA125 values that exceeded the recommended clinical cut-off of 35 U/ml. The rise and fall in serum CA 125 seen in the present study is consistent with the changes seen during the first trimester previously (Jacobs et al., 1990).
PSA was thought to be produced exclusively by prostatic tissue and was therefore used to monitor prostate cancer (Armbruster, 1993). However, it is a serine protease also known as kallikrein-3 (Lawrence et al., 2010) and has been associated with a number of tissues and biological events in women (Diamandis and Yu, 1995) such as in the breast (Yu et al., 1996) and during the ovarian cycle (Aksoy, et al., 2002; Zarghami et al., 1997). PSA has also been found in placental tissue during pregnancy and is secreted in vitro by placental cells in culture (Malatesta et al., 2000) thereby being a potentially useful biomarker of pregnancy. The steady rise seen in the present study as the pregnancy progressed is consistent with the increase in serum oestradiol concentrations seen in pregnancies at Fertility North (K Hamilton, personal communication) and a previous report that PSA production and secretion by placental tissue in culture is upregulated by 17β-oestradiol (Malatesta et al., 2000). The main limitation, however, was the lack of sensitivity of the assay used in the current study presumably because it has been optimized for use in the screening of men for prostate disease. This meant that the PSA could not be detected in 36% of the women tested, but subsequent work using a more sensitive assay would seem warranted.
CA15-3, a tumour biomarker, is a mucin-like glycoprotein encoded by the MUC1 gene whose main clinical use of the assay is in the monitoring of women with breast cancer (Duffy et al., 1999). Nevertheless, it has a clear association with reproduction since MUC1 is heterogeneously expressed on the surface of epithelial cells, including those in the breast and upper reproductive tract and is thought to prevent embryo implantation (Al-Azemi et al., 2009). It has been suggested that the human blastocyst can produce certain factors that remove MUC1 from a site to facilitate implantation in the endometrium (Meseguer et al., 2001), and this is consistent with the findings of the present study where the CA15-3 levels decreased as the pregnancies progressed.
Conclusion
A series of six biomarkers have been described that show different patterns of change during early pregnancy. PAPP-A and PSA rose steadily as the pregnancies progressed, CA125 rose until week 5.5 and then returned back to baseline values, while CA15-3 serum concentrations decreased during pregnancy; the two reproductive hormones, progesterone and hCG, followed expected patterns. These biomarker results suggest further investigation is warranted to permit a non-invasive correlation of the biomarker levels with the various stages of embryogenesis, implantation and placentation.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
