Abstract
Knee osteoarthritis (KOA) is a common chronic disease in the elderly and leads to a high rate of disability. Du Huo Ji Sheng Tang (DHJST), a Chinese traditional medicinal formula, is a classic prescription for the treatment of KOA. Here, we investigated whether DHJST could inhibit inflammation and treat KOA through suppressing NLRP3/nuclear factor (NF)-κB inflammatory signals in rats. The serum levels of interleukin (IL)-1β, IL-6, IL-10, tumor necrosis factor (TNF)-α, NLRP3, ASC, Caspase-1, p-NF-κB-P65, and p-IκBa were detected in healthy adults and patients with KOA before and after treatment. Sprague Dawley (SD) rats were divided into normal group, model group, diclofenac sodium group (5 mg/kg), DHJST high-dose group (1 g/kg), and DHJST low-dose group (0.5 g/kg). The right hind knee joint of the rats, except normal group, was injected with 4% papain (0.25 mL/kg) once every 7 days for three times. All rats were treated for 3 weeks. The swelling volume of right hind paw; five classification of inflammatory cells in synovial fluid; pathological changes of the knee-joint synovial membrane and cartilage; levels of IL-1β, IL-6, and TNF-α in serum and knee-joint synovial fluid; and the expressions of NLRP3/NF-κB inflammatory signals in the knee-joint synovial membrane were detected. The serum levels of IL-1β, IL-6, IL-10, TNF-α, NLRP3, ASC, Caspase-1, p-NF-κB-P65, and p-IκBa in KOA patients treated with DHJST were significantly decreased. The KOA rats treated with DHJST showed significant decreases in swelling volume of right hind paws; the percentage of leukocyte, lymphocyte, neutrophil, and eosinophils in synovial fluid; the levels of IL-1β, IL-6, and TNF-α in serum and knee-joint synovial fluid; and the expressions of NLRP3 ASC, Caspase-1, IL-1β, p-NF-κB-P65, and p-IκBa in the knee-joint synovial membrane, and showed an alleviation in pathological changes of the knee-joint synovial membrane and cartilage. Our data provide the first evidence that DHJST relieves KOA via suppressing NLRP3/NF-κB inflammatory signals in rats
Introduction
As a chronic joint disease, osteoarthritis (OA) affects articular cartilage, synovium, joint capsules, and muscles around the joints and causes local joint pain, swelling, and deformities that seriously affect daily work and life. 1 More than 400 million people suffer from OA, placing a heavy financial burden on families and society. 2 Inflammation plays a key role in the pathogenesis of OA. The upregulation of inflammatory genes that promote cartilage damage may lead to OA; 3 the study found that the expression levels of interleukin (IL)-1β and tumor necrosis factor (TNF)-α in the joint fluid of patients with OA were significantly increased and were positively correlated with articular cartilage injury. 4
Nucleotide-binding oligomerization domain, leucine-rich repeat, and pyrin domain containing 3 (NLRP3) inflammasome plays an important role in arthritis. 5 NLRP3 inflammasome is a polyprotein complex mainly composed of NLRP3 protein, cysteine aspartic acid–specific protease-1 (Caspase-1), and apoptosis-associated speck-like protein containing a CARD (ASC) composition. 6 Activation of NLRP3 activates Caspase-1, which induces the production and secretion of IL-1β and IL-18, and further causes an inflammatory response. 5 Activation of NLRP3 inflammasome also promotes NF-κB activation. 7 The NLRP3/NF-κB signaling pathway has been shown to be closely associated with rheumatoid arthritis, gouty arthritis, and knee osteoarthritis (KOA).8–10
Clinically, Du Huo Ji Sheng Tang (DHJST) is used to treat KOA.11,12 Although we know that DHJST can regulate inflammatory factors, 13 however, whether DHJST can inhibit these inflammatory factors and treat KOA via NLRP3/NF-κB signaling pathway has not been proven.
Materials and methods
Serum samples from human
The sample size of this project was calculated according to the following formula: N = Z2 × (
The serum of 30 healthy adults aged 40–70 years was collected as normal group. Sixty patients aged 40–70 years with KOA were randomly divided into DHJST group and diclofenac sodium group—30 cases in each group. Ninety human subjects were included in our study. The serum of the patients was collected before and after treatment with DHJST or diclofenac sodium for 3 weeks. The patients in this study had long-term pain (less than 6 months) in the knee joint and did not have significant cartilage damage. The pain of KOA in patients can be undertaken by patients without anti-inflammatory drugs. This study was approved by the Wuxi Traditional Chinese Medicine Hospital Ethics Committee. The clinical trial registration number was 2017050301. Patients all signed the informed consent for these treatments.
Reagents
Diclofenac sodium enteric-coated tablets were provided by Beijing Novartis Pharmaceutical Co., Ltd. The enzyme-linked immunosorbent assay (ELISA) kits for IL-1β, IL-6, IL-10, TNF-α, NLRP3, ASC, Caspase-1, p-NF-κB-P65, and p-IκBa were purchased from Wuhan Yibo Biotechnology Co., Ltd. Antibodies against GAPDH, NLRP3, ASC, Caspase-1, IL-1β, p-NF-κB-P65, NF-κB-P65, p-IκBa, and IκBa were bought from CST. Other reagents were purchased from Sinopharm Chemical Reagent Co., Ltd.
Preparation and composition analysis of DHJST
The medicinal materials of DHJST were weighed according to the proportion of the prescriptions. The medicinal materials were mixed with distilled water and soaked overnight. The materials were boiled for 1 h. The dregs were filtered and the liquid supernatant was concentrated into a high concentration of decoction. The decoction was diluted according to the administered dose to prepare a solution.
UFLC/Q-TOF MS-based chemical analysis
14
was used to analyze and identify the chemical constituents of DHJST. According to chromatographic retention time (tR) mass spectrometry, fragment ion (

Chemical composition analysis map of (a) DHJST and (b–e) standard control by UPLC-QTO-MS method. Four main components of DHJST were determined, including a, glycyrrhizic acid; b, citric acid; c, paeoniflorin; and d, gentianine.
Animal grouping and KOA model preparation
Fifty Sprague Dawley rats, 8–12 weeks old, were randomly divided into five groups, including normal group (without treatment), model group (with papain injection treatment), diclofenac sodium group (5 mg/kg), DHJST high-dose group (1 g/kg), and DHJST low-dose group (0.5 g/kg). Except the normal group, the right knee-joint cavity of the rats in other groups were injected with 4% papain (0.25 mL/kg) once every 7 days for three times. Then, the diclofenac sodium group (5 mg/kg), DHJST high-dose group (1 g/kg), and DHJST low-dose group (0.5 g/kg) were treated with intragastric administration once a day for 3 weeks. The normal group and the control group were given saline. The number of animal ethic review is SCZON1719, which was approved by Ethics committee of WuXi Hospital of Traditional Chinese Medicine. This work was a preclinical pharmacological research.
Paw volume measurement
The paw volume of the rats in each group was determined by the drainage method on the 7th, 14th, and 21st days after treatment. 15 In brief, paw volume was measured by YLS-7C paw swelling meter (Shanghai Bio-will Co., Ltd, China). Appropriate amount of water was added to the sink of the instrument. The top of the water was higher than the lowest mark and below the highest mark of the sink. After holding the rat, the paw was placed in the sink. The instrument measured the paw volume and displayed the values on the screen. The values were recorded.
Joint fluid cytology
The joint fluid of the right knee joint of the rats was drawn out by a syringe after 3 weeks of administration with DHJST, and then the joint fluid was centrifuged at 1000 r/min for 10 min at room temperature. The supernatant was cryopreserved for other tests. The precipitate was fixed in glass slide and then stained by Reggie’s dye; 200 white blood cells were counted under the microscope and the percentage of various types of white blood cells was calculated.
Arthritis pathology
Three rats in each group were randomly selected and sacrificed after anesthesia with 2% pentobarbital (0.3 mL/100 g). The right knee was taken and immersed in 4% paraformaldehyde solution for over 72 h. The knee-joint cavity was dissected, and synovial membrane was taken for hematoxylin–eosin (HE) staining. The HE staining was performed according to Fischer et al. 16
ELISA
The steps of detecting IL-1β, IL-6, IL-10, TNF-α, NLRP3, ASC, Caspase-1, p-NF-κB-P65, and p-IκBa were carried out in accordance with the instructions provided in the kit.
Western blot
The synovial membranes of the knee joints of each group were taken and mixed with lysis buffer to prepare protein samples. A sample containing an equal amount of protein was added to the well of a sodium dodecyl sulfate–polyacrylamide gel electrophoresis (SDS-PAGE), and after electrophoresis, the protein in gel was transferred to PVDF (polyvinylidene difluoride) membrane. The membrane was blocked with 5% bovine serum albumin (BSA) for 1 h at room temperature and incubated with primary antibody at 4 C overnight, and then incubated for 1 h at room temperature with the secondary antibody. After cleaning the membrane, the image was scanned using Bio-Rad SYSTEM GelDoc XR+.
Statistical analysis
Statistical analysis was carried out using Student’s two-tailed
Results
DHJST decreased the serum levels of related cytokines in NLRP3/NF-κB signaling pathway in KOA patients
First, we used ELISA to detect serum levels of IL-1β, IL-6, IL-10, TNF-α, NLRP3, ASC, Caspase-1, p-NF-κB-P65, and p-IκBa in healthy volunteers and patients with KOA. The results showed that, except for IL-10, the levels of the other factors in the serum of patients with KOA were significantly higher than those of healthy volunteers (

Serum levels of related cytokines in NLRP3/NF-κB signaling pathways in volunteers. Changes of serum levels of (a) IL-1β, IL-6, IL-10, TNF-α, (b) NLRP3, ASC, Caspase-1, p-NF-κB-P65, and p-IκBa in healthy adults (n = 30) and patients with KOA (n = 60). Changes of serum levels of (c) IL-1β, IL-6, IL-10, (d) TNF-α, ASC, (e) NLRP3, Caspase-1, (f) p-NF-κB-P65, and p-IκBa in patients with KOA (n = 60), patients treated with DHJST (n = 30) (300 mL/10 g/day), and patients treated with diclofenac sodium (n = 30) (100 mg/day) for 3 weeks.
Subsequently, we tested these factors before and after treatment in patients with KOA. We found that except for IL-10, the levels of other factors in the serum of patients with KOA were significantly lower after DHJST and diclofenac sodium treatment, compared with before treatment (KOA group) (
DHJST reduced the swelling volume of the right hind paws of the KOA rats
The morphological characteristics of right hind paw of rats showed that paw swelling was reduced by DHJST and diclofenac sodium treatment (Figure 3(c)). After 1-, 2-, and 3-week treatment of DHJST and diclofenac sodium, the swelling volume of the right hind paw was significantly decreased (

DHJST reduced swelling volume of the paws of the rats with KOA (n = 10 in each group). (A) Left hind paw volume and (B) Right hind paw volume in the various rat groups. Data represent mean ± SD in each group. ##
DHJST reduced the inflammatory cells in synovial fluid of the KOA rats
Compared with the normal group, the percentage of leukocytes (
Inflammatory cells in synovial fluid of different groups (mean± SD, n = 10).

KOA: knee osteoarthritis; DHJST: Du Huo Ji Sheng Tang.
#
DHJST alleviated pathological changes of the knee-joint synovial membrane and the cartilage of the KOA rats
In the normal group, the synovial cells of the knee joint were arranged neatly and intact. There were no inflammatory cell infiltration, congestion, and edema. In the model group, the superficial cells of the synovial membrane of the knee joint showed significant inflammatory cell infiltration, proliferation, congestion, and edema. The vascular proliferation and granulation tissue formation could be observed in the synovium. After treatment with DHJST or diclofenac sodium, all the pathological changes were alleviated in the synovium of the knee joint (Figure 4(a)).
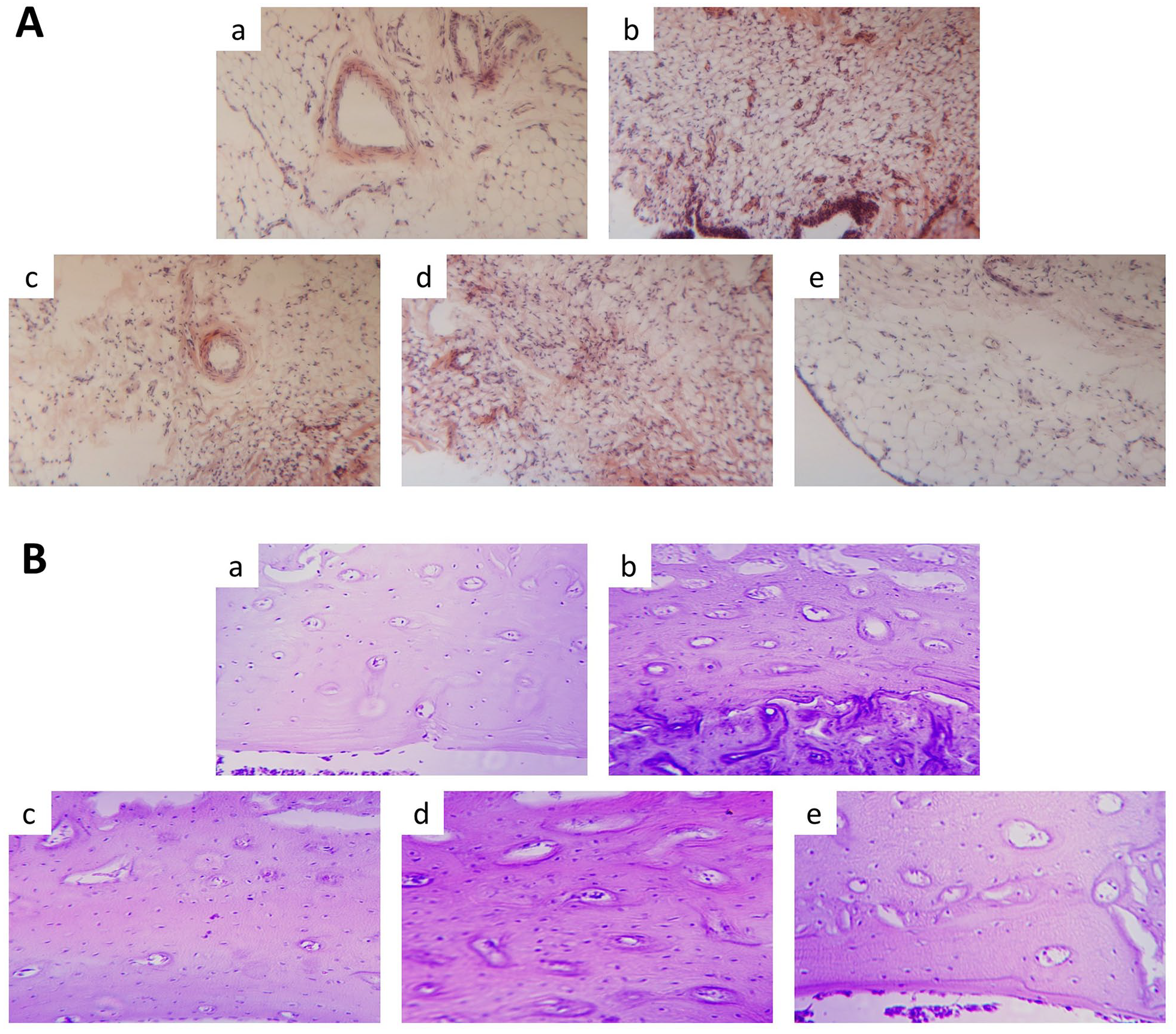
The pathological changes of the (A) knee-joint synovial membrane and the (B) cartilage of rats in a, normal; b, KOA group; c, diclofenac sodium (5 mg/kg); d, DHJST (0.5 g/kg); and e, DHJST (1 g/kg) (n = 3 in each group).
In the normal group, the cartilage matrix, perichondrium, and cartilage sac have normal structure, and no cartilage osteophyte formation and chondrocyte necrosis was observed. In the model group, the cartilage osteophytes were presented, and degeneration and necrosis of chondrocytes could be observed. After treatment with DHJST or diclofenac sodium, the pathological changes of cartilage tissue were reversed (Figure 4(b)).
DHJST reduced the levels of IL-1β, IL-6, and TNF-α in serum and knee-joint synovial fluid in KOA rats
The ELISA kit was used to detect the levels of IL-6, IL-1β, and TNF-α in serum (Figure 5(a)) and synovial fluid (Figure 5(b)) of rats in different groups. While treated with DHJST and diclofenac sodium, the levels of IL-6, IL-1β, and TNF-α were significantly decreased than those in the KOA group (

DHJST reduced the levels of IL-1β, IL-6, and TNF-α in (a) serum and (b) knee-joint synovial fluid of KOA rats.
DHJST decreased the activation of NLRP3/NF-κB inflammatory signals in KOA rats
Western blot analysis confirmed the presence of NLRP3, ASC, Caspase-1, IL-1β, p-NF-κB-P65, NF-κB-P65, p-IκBa, and p-IκBa protein expressions in different groups, and a marked increase of NLRP3, ASC, Caspase-1, IL-1β, p-NF-κB-P65/NF-κB-P65, and p-IκBa/IκBa in KOA rats with significant decrease in DHJST and diclofenac sodium–treated rats (Figure 6(a)–(e)).

Western blot analyzed (A) the expressions of NLRP3/NF-κB inflammatory signals in the knee-joint synovial membrane of the various rat groups. Semi-quantitative results of (B) NLRP3, (C) ASC, (D) Caspase-1, (E) IL-1β, (F) p-NF-κB-P65/NF-κB-P65, and (G) p-IκBa/IκBa in a, normal; b, KOA group; c, diclofenac sodium (5 mg/kg); d, DHJST (0.5 g/kg); and e, DHJST (1 g/kg).
Discussion
KOA is a common degenerative chronic disease in the elderly, and its disease process is closely related to inflammation. 17 Here, we report the therapeutic effect of a Chinese traditional medicinal formula (DHJST) on KOA. At first, glycyrrhizic acid, citric acid, paeoniflorin, and gentianine were quantified for quality control of DHJST. Glycyrrhizic acid is one kind of saponin, as an 11β-hydroxysteroid dehydrogenase inhibitor, glycyrrhizic acid has anti-inflammatory activity and mineralocorticoid activity. 18 Citric acid could enhance the anti-inflammatory activity of other substances. 19 Paeoniflorin has been shown to prevent interferon (IFN)-α-induced neuroinflammation. 20 Gentiopicroside also has anti-inflammatory pharmacological effects. 21 These studies indicate that DHJST may have a powerful anti-inflammatory effect.
NF-κB is one of the key regulators regulating and controlling cytokine expression in immune function and inflammation. 22 NF-κB stimulation leads to the expression of TNF-α and IL-1β23,24 and then induced the production of IL-6; 25 the elevated levels of these cytokines may disrupt cartilage 26 and promote the development of arthritis. 1
The activation of NLRP3 followed by Caspase-1 induces the production and secretion of IL-1β and IL-18 and further causes the inflammatory response. 8 Studies have shown that both NLRP3 and NF-κB signaling are involved in the development of arthritis.9,10,27,28 In turn, IL-1β, IL-6, and TNF-α can stimulate NF-κB, activate IκBα, and promote the entry of κB enhancer into the nucleus to regulate inflammation.29,30
Indeed, our study showed that serum IL-1β, IL-6, TNF-α, NLRP3, ASC, Caspase-1, p-NF-κB-P65, and p-IκBa levels in patients with KOA were significantly increased (Figure 2), indicating that the NLRP3/NF-κB signaling pathway was activated. After treatment with DHJST, NLRP3/NF-κB signaling was significantly inhibited and the levels of inflammatory factors were reduced.
Inflammatory cells, especially neutrophils, are one of the major causes of inflammation in bones and joints. 31 Our study also found that the different doses of DHJST significantly reduced the number of inflammatory cells, including leukocytes, lymphocytes, neutrophils, and eosinophils, in the joint fluid of KOA rats (Table 1).
In cartilage degenerative lesions, inflammatory factors are produced into the joint cavity, causing phagocytosis of synovial cells in the joint cavity, which leads to inflammation and exudation of the synovial membrane. 32 The inflammatory factors will further act on the articular cartilage, aggravating the destruction of the cartilage, thus forming a vicious circle, which will lead to a decrease in repair ability and destroy of the chondrocytes. 33 In vitro, we observed a reduction of IL-1β, IL-6, and TNF-α in serum and synovial fluid in KOA rats (Figure 5) and demonstrated that DHJST treatment significantly reduces the swelling volume of the right hind foot (Figure 3) and alleviated pathological changes of the knee-joint synovial membrane (Figure 4) of the KOA rats. These results indicated that DHJST could reduce inflammation and had a therapeutic effect in KOA rats.
In addition, we measured the protein expression levels of related factors in NLRP3/NF-κB signaling pathway, including NLRP3, ASC, Caspase-1, IL-1β, p-NF-κB-P65, NF-κB-P65, p-IκBa, and p-IκBa, in the knee synovium of rats. Consistent with the results of serological tests, DHJST administration remarkable lessened the NLRP3, ASC, Caspase-1, IL-1β, p-NF-κB-P65/NF-κB-P65, and p-IκBa/IκBa levels in KOA rats. Our results proved that DHJST reduced the activation of NLRP3/NF-κB signaling pathway in KOA rats.
Limitations of our present study should be explored in further study. The first key limitation of our study is that the chemical constituents of DHJST were not used to investigate the anti-inflammatory effect on KOA. The second major limitation is that the exact mechanism of anti-inflammatory effect of DHJST on KOA was not studied, despite its influence on NLRP3 and NF-κB . Therefore, further studies should be directed toward these objectives.
Conclusion
Our data provided the first evidence that DHJST could significantly reduce the swelling volume, the number of inflammatory cells, and inflammatory factors in joint fluid; relieve synovium pathological changes; and suppress NLRP3/NF-κB signaling pathway to remedy KOA in rats.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval for this study was obtained from Ethics committee of WuXi Hospital of Traditional Chinese Medicine (the number of animal ethic review is SCZON1719. The clinical trial registration number was 2017050301).
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Natural Science Fund of China (No. 81473693).
Informed consent
Written informed consent was obtained from legally authorized representatives before the study.
Trial registration
The clinical trial registration number was 2017050301.
