Abstract
Background
Computed tomography (CT)-guided transthoracic biopsy is essential for diagnosing pulmonary lesions but exposes patients to considerable radiation from repeated image acquisitions. With the growing emphasis on radiation safety, applying validated low-dose CT protocols to interventional procedures has become a key clinical priority.
Purpose
To assess the feasibility, safety, diagnostic yield, and radiation dose of low-dose computed tomography-guided transthoracic biopsies using an 80 kVp protocol compared with standard 120 kVp protocols.
Methods
A retrospective review was performed on 183 consecutive computed tomography-guided transthoracic biopsies of lung nodules or masses, including 143 procedures with the standard 120 kVp protocol and 40 procedures with a low-dose 80 kVp protocol at 30 mAs. Procedural characteristics, image quality, histopathological adequacy, radiation exposure, and complications were analyzed. Both subjective and objective image quality assessments, including signal-to-noise and contrast-to-noise ratios, and cellular analyses of specimens were compared.
Results
The low-dose protocol reduced mean effective radiation dose from 5.89 ± 2.88 millisieverts to 0.19 ± 0.06 millisieverts, a 96.8% reduction. Biopsy specimen adequacy was 85% in the low-dose group versus 79% in the standard-dose group. Complication rates were comparable, 45% versus 43.4%. Subjective image quality was lower in the low-dose group, but objective signal-to-noise and contrast-to-noise ratios remained sufficient for accurate diagnosis.
Conclusion
Computed tomography-guided transthoracic biopsies with an 80 kVp and 30 mAs protocol significantly reduce radiation exposure without compromising diagnostic yield or safety. This low-dose approach is a viable alternative to conventional protocols and can be adopted in routine interventional radiology practice.
Introduction
Several studies have demonstrated the feasibility of reduced tube voltage in diagnostic chest CT; however, evidence regarding the use of low tube voltage protocols (<100 kVp) in CT-guided transthoracic biopsy remains limited. 1 CT-guided transthoracic biopsy, while diagnostically reliable, involves multiple CT acquisitions during patient positioning, needle advancement, and confirmation, increasing radiation exposure for both patients and interventional team. 1 This is particularly relevant in oncology patients, who may undergo repeated CT examinations for staging and follow-up, leading to a considerable cumulative dose over time. 2 Strategies to reduce dose include lowering tube voltage or current, shortening scan time, and employing iterative reconstruction algorithms.1,3 Despite methodological heterogeneity, previous analyses have shown that these approaches can reduce radiation dose by up to 90%.2,3 The purpose of this study was to evaluate the feasibility of an low-dose 80 kVp protocol for CT-guided transthoracic lung biopsy and to compare its safety, diagnostic yield, and radiation dose with the conventional 120 kVp protocol.
Materials and methods
This retrospective study was approved by the Bolu Abant Izzet Baysal University Clinical Research Ethics Committee (Decision No.: 2020/197; Date: 25 August 2020). Written informed consent regarding the biopsy procedure was obtained from all patients prior to the intervention.
Patient selection
We reviewed 183 consecutive CT-guided biopsies of lung nodules or masses: 143 performed with a standard 120 kVp protocol (Nov 2017–Oct 2019, control group) and 40 performed with an 80 kVp low-dose protocol (Nov 2019–July 2020, study group). Patients with pulmonary nodules measuring ≥1 cm on procedural CT or masses identified on prior CT or PET-CT were included in the study. Nodules <1 cm were not biopsied in our institution because such small lesions present significant technical challenges for accurate needle targeting, are associated with a substantially higher risk of non-diagnostic sampling, and may carry an increased complication risk. For this reason, patients with nodules <1 cm are managed in our clinical practice through alternative strategies such as radiological surveillance or less invasive diagnostic modalities rather than CT-guided transthoracic biopsy. 143 patients in the control group and 40 patients in the study group were obtained. Exclusion criteria included missing PACS images or histopathology specimens, resulting in 32 excluded cases. Demographics, smoking history, lesion characteristics, and histopathological data were collected and analyzed.
The mean age of patients was 65.60 ± 8.49 years in the study group and 63.72 ± 12.54 years in the control group, with no statistically significant difference observed between the groups (p = .273). Gender distribution was also similar, with the study group consisting of four women (10%) and 36 men (90%), and the control group including 27 women (18.9%) and 116 men (81.1%) (p = .237). Among all evaluated patients, 137 (74.8%) were smokers. The average smoking history was comparable between the control group (37.87 ± 35.79 pack-years) and the study group (38.65 ± 25.66 pack-years), showing no statistically significant difference (p = .458).
CT protocol and biopsy technique
Due to ongoing departmental efforts to reduce radiation dose in diagnostic thoracic imaging, we implemented a low-dose protocol for CT-guided transthoracic biopsies to systematically evaluate its impact on image quality, radiation exposure, and diagnostic yield. All procedures performed after November 2019 followed this low-dose protocol; no selective case inclusion was applied, ensuring that potential selection bias was minimized. CT-guided transthoracic lung biopsies were performed using a 64-detector CT scanner (GE Revolution Evo, June 2017, China). In the control group, the manufacturer’s standard protocol was used, which included a tube voltage of 120 kV, tube current modulation (225–560 mAs), a rotation time of 0.5 seconds, and a slice thickness of 5 mm. In the study group, the low-dose protocol utilized an 80 kV tube voltage, a fixed tube current of 30 mAs, a rotation time of 0.5 seconds, and a slice thickness of 5 mm. Iterative reconstruction techniques were applied to compensate for increased image noise in the low-dose acquisitions. For each patient, the target lesion location was already known from prior diagnostic CT or PET-CT examinations. Therefore, pre-procedural and intra-procedural CT imaging was not performed as a whole-lung acquisition. Instead, an initial limited, non-contrast scan was obtained over the anatomical region containing the lesion, ensuring inclusion of the entire lesion margins without unnecessarily extending the scan range. The biopsy was then performed with intermittent, focused CT acquisitions restricted to the lesion-containing volume to guide needle advancement while minimizing radiation exposure.
CT protocol and biopsy technique details.

Abbreviations: CT = computed tomography, kVp = kilovolt peak, mAs = milliampere-seconds, mm = millimeter, s = seconds, G = gauge, PET = positron emission tomography.
Data collection
Procedural data were collected, including procedure duration, number of scans performed during and after the procedure, lesion size (Group 1: 1–2 cm, Group 2: 2.1–5 cm, and Group 3:
Subjective image quality evaluation
Subjective image quality was evaluated using a 5-point Likert scale with predefined anchors to ensure reproducibility: 1 = non-diagnostic image quality with insufficient visualization of both the lesion and needle track; 2 = poor image quality that allows limited visualization of the lesion but inadequate visualization of the needle track; 3 = marginal but diagnostically usable image quality for both the lesion and needle track; 4 = adequate-to-good diagnostic image quality for both the lesion and needle track; and 5 = excellent and fully diagnostic image quality with clear delineation of both the lesion and needle track.
Subjective imaging scoring criteria are presented.


A 56-year-old patient undergoing CT-guided transthoracic biopsy with the low-dose protocol. Biopsy images obtained without and with iterative reconstruction (IR) are presented. (a) Mediastinal window image acquired without IR. (b) Mediastinal window image acquired with IR. (c) Lung parenchyma window image acquired without IR. (d) Lung parenchyma window image acquired with IR.
Objective image quality evaluation
Objective image quality was assessed by measuring mean attenuation (HU) and noise (SD) in 1-cm ROIs placed in standardized anatomical locations (lung parenchyma, vertebral body, pectoral muscle, and axillary fat). SNR and CNR were calculated according to established formulas used in previous CT image quality studies.4,5 Figure 2 shows ROIs drawn in the lung parenchyma, pectoral muscle, axillary adipose tissue, and vertebral body for obtaining average and SD values used in objective image analysis. Mean and standard deviation values derived from regions of interest (ROIs) placed in representative anatomical areas: (a) Lung parenchyma. (b) Pectoral muscle. (c) Axillary adipose tissue. (d) Vertebral body.
Pathological specimen evaluation
Scoring based on the cellular percentage in the histopathological specimen is presented.


Pathological specimen images and cellular analysis of four patients from the study group using HEX100. (a) Small cell carcinoma with a tumor score of 3 and fibrosis score of 2 (arrow: tumor; arrowhead: fibrosis). (b) Small cell carcinoma with a tumor score of 2 (arrow: tumor). (c) Hepatocellular carcinoma metastasis with a tumor score of 4 (arrow: tumor). (d) Squamous cell carcinoma with a tumor score of 3, fibrosis score of 3, and inflammation score of 1 (arrow: tumor).
Radiation dose evaluation
The radiation dose evaluation was based on dose-length product (DLP) and CT dose index volume (CTDIvol) values, which were automatically calculated by the CT machine during the procedures and archived alongside the images in the PACS. The effective radiation dose was calculated by converting the DLP records using dose conversion factors as recommended in the European guidelines. Specifically, for 80 kVp, the conversion factors were 0.0107 mSv/mGy-cm for men and 0.0188 mSv/mGy-cm for women, while for 120 kVp, they were 0.0105 mSv/mGy-cm for men and 0.0185 mSv/mGy-cm for women. 7
Complication evaluation
Presents the categorization of complications that may be encountered during the procedure.

Statistical analysis
Quantitative variables were summarized as mean ± standard deviation or median (minimum–maximum), while categorical data were presented as frequencies (percentages). The Shapiro–Wilk test and histogram graphs were employed to evaluate the normality of data distribution. Variables following a normal distribution were compared using one-way analysis of variance (ANOVA) or independent t-tests, whereas non-normally distributed variables were analyzed using Kruskal–Wallis and Mann–Whitney U tests. Categorical variables were assessed using Pearson’s chi-square test or Fisher’s exact test, depending on the expected frequencies. Relationships between variables were analyzed using Spearman’s correlation coefficient. Statistical analysis was performed using SPSS version 25.0 (SPSS Inc., Chicago, Illinois, USA), with p-values less than 0.05 considered statistically significant.
Results
Demographics and baseline characteristics of patients undergoing CT-guided p ercutaneous transthoracic core needle biopsy using 120 kVp versus 80 kVp.

Data are presented as mean ± standard deviation (SD).
Mean ± SD or n (% of column).
aIndependent samples t-test
bPearson’s chi-square test
cMann–Whitney U test and Fisher’s exact test.
Spearman’s correlation analysis between selected variables and subjective and objective image quality.

Data are presented as Spearman’s correlation coefficients (ρ) with corresponding p-values. SNR: signal-to-noise ratio, CNR: contrast-to-noise ratio, BMI: body mass index.
Subjective and objective image quality evaluation
Subjective image quality evaluations revealed notable differences, with all control group patients scoring five, while the study group had a mean score of 3.75 ± 0.54 (median: 4, range: 2–5), indicating significantly lower scores (p < .001). Objective image quality assessments demonstrated significantly higher SNR and CNR values in the control group for some lung regions (p < .05). However, the study group exhibited superior values in measurements from the pectoral muscle and axillary regions (p < .05).
Radiation dose exposure
Radiation exposure was substantially reduced in the study group, with mean DLP and effective radiation dose values of 17.48 ± 5.49 mGy/cm and 0.19 ± 0.06 mSv, respectively, compared to 487.90 ± 192.85 mGy/cm and 5.89 ± 2.88 mSv in the control group, reflecting reductions of 96.2% and 96.8% (p < .05).
Histopathological evaluation
Histopathological evaluation revealed diagnostically adequate specimens in 85% of the study group and 79% of the control group, favoring the study group (p < .05). Cellular analyses showed no significant differences between groups in tumor cell ratios or other histological components, except for inflammatory cells, which were more prominent in the control group (p = .013).
Complications
Distribution of complications by group.
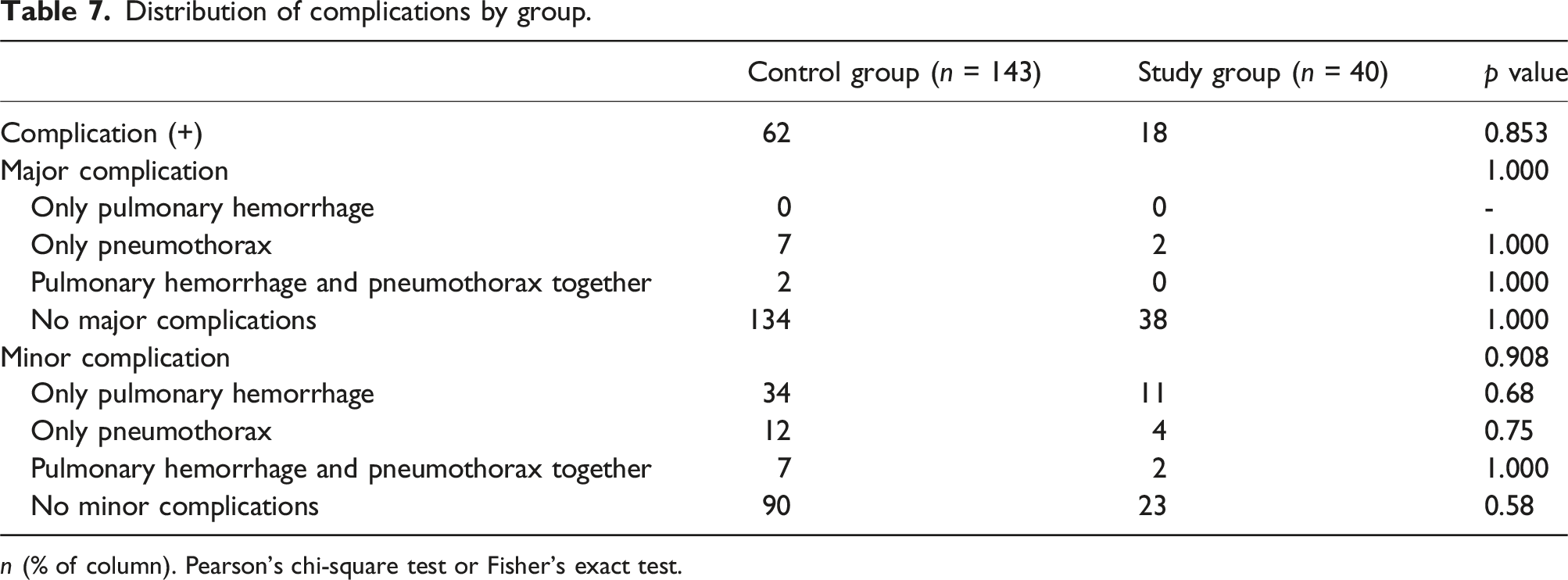
n (% of column). Pearson’s chi-square test or Fisher’s exact test.
Discussion
Our study demonstrates that an ultra-low-dose protocol can be used for CT-guided transthoracic lung biopsy of pulmonary nodules and masses with a very substantial reduction in radiation exposure, while preserving diagnostic performance. Notably, this dose reduction did not result in significant differences in complication rates, cellular analyses, tumor cell ratios, or other histological components between the two groups. To our knowledge, this study represents one of the first investigations into the safety and diagnostic efficacy of CT-guided transthoracic biopsies of lung nodules and/or masses procedures utilizing radiation doses below 100 kVp, while maintaining diagnostic yield and procedural success.
Subjective image quality scores were, as expected, lower in the low-dose group than in the standard-dose group. However, histopathological assessment demonstrated diagnostically adequate specimens in 85% of the study group and 79% of the control group (p < .05). This difference may be attributed to the operators spending more time targeting areas with higher cellular tissue representation in the study group, potentially as a precaution to mitigate the risk of diagnostic failure.
Procedure duration was modestly longer in the low-dose group, whereas the number of CT acquisitions during the procedure was similar between protocols. This extended duration may be attributed to the additional time required for iterative reconstruction, and operators required more time for needle trajectory planning and confirmation due to reduced confidence in visualizing the needle track and lesion borders. It is plausible that the lower image quality in the low-dose group, resulting in reduced confidence in visualizing the needle track and lesion borders, necessitated slower needle advancement and ultimately prolonged the overall procedure time.
Objective image quality analysis further clarified the impact of the low-dose protocol. Signal-to-noise and contrast-to-noise ratios were lower in several lung regions with the 80 kVp protocol, consistent with increased image noise at lower tube settings. Nevertheless, these reductions did not impair diagnostic yield, indicating that SNR and CNR remained within an acceptable range for safe needle guidance. Interestingly, SNR and CNR measurements obtained from the pectoral muscle and axillary fat were higher in the low-dose group, suggesting that iterative reconstruction combined with lower kVp may enhance contrast perception for certain soft-tissue structures in the mediastinal window. In our review of the literature, we were unable to find studies on CT-guided transthoracic biopsies of lung nodules and/or masses using low-dose protocols that employed similar methods for objective image quality analysis. As a result, we were unable to directly compare our SNR and CNR measurement results with those in the existing literature.
In the European Curriculum and Syllabus for Interventional Radiology, under the section titled “Recognition and Reduction of Occupational Hazards,” the following directive is emphasized: “Avoid unnecessary patient radiation exposure in Interventional Radiology procedures. 9 Take responsibility for applying the principles of justification (risk/benefit assessment), optimization (including ALARA), and the establishment of reference levels to protect the patient from unnecessary radiation risks” 10 . Considering that a single chest CT scan is estimated to deliver approximately 100 times the radiation dose of a standard chest X-ray, there is ongoing research aimed at reducing radiation doses in diagnostic thoracic CT imaging. As low-dose chest CT becomes more widely adopted in routine clinical practice, it is essential that we also prepare for its use in CT-guided transthoracic biopsies of lung nodules and/or masses.11–13 According to the literature, the highest effective dose reduction rates in CT-guided transthoracic biopsies of lung nodules and/or masses using varying kVp and mAs settings have been reported in studies by Frisch et al. (92%) and Liang et al. (91.5%). In our study, an ultra-low-dose protocol yielded a (96.8%) important reduction in mean effective radiation dose, which, when compared to the existing literature, represents one of the highest dose reduction rates reported to date.14,15 The observed significant reduction in effective radiation dose exceeding 90% can be attributed to the logarithmic influence of tube voltage and the linear influence of tube current on effective radiation dose.
A meta-analysis that reviewed low-dose protocol studies, reported pneumothorax rates of approximately 16.5%–17.2% and pulmonary hemorrhage rates of 13.5%–14.8%. The major complication rates observed in our study are consistent with those reported in the literature. 16
This concordance suggests that dose reduction per se does not substantially alter the risk profile of the procedure. Instead, traditional determinants of complication risk such as pleura-to-lesion distance, lesion size and location, and underlying lung parenchymal changes likely remain the dominant factors. The preservation of a complication profile comparable to the literature supports the feasibility and safety of adopting low-dose protocols in appropriate patients.
Histopathological analysis provided an additional perspective on the impact of low-dose imaging on tissue sampling quality. We observed no significant differences between the groups in tumor cell ratios, necrotic, fibrotic, or lung parenchyma components, or anthracosis, indicating that the low-dose protocol did not adversely affect the quality of tissue cores obtained from malignant lesions. The higher proportion of inflammatory cells in the control group may be related to the small number of benign inflammatory entities overall, rather than a systematic effect of dose level on sampling. To our knowledge, no studies in the existing literature evaluating CT-guided transthoracic biopsies of lung nodules and/or masses with low-dose protocols have performed cellular analysis on histopathological specimens. Therefore, we recommend conducting prospective studies with larger patient populations to assess the effectiveness of the low-dose protocol in diagnosing benign pathologies with a high density of inflammatory cells.
In our study, both subjective and objective image quality assessments demonstrated a reduction that did not compromise the success of the biopsy procedure. However, this decline may serve as an indirect indication that further reductions in dose parameters—particularly below 80 kVp and 30 mAs—could adversely affect image quality and procedural performance in future studies. Lesion characteristics had no measurable impact on subjective or objective image quality. Given that our cohort primarily consisted of solid nodules and masses, the applicability of this protocol to small or ground-glass lesions—where high image quality is critical—remains uncertain. At our institution, this protocol has since been increasingly applied in clinical practice, particularly for large masses and peripherally located solid nodules.
Limitations
The low-dose group included a small number of patients, limiting the generalizability of the results. The retrospective design prevented randomization and may have introduced selection bias. Biopsies were performed by radiologists with different levels of experience, which could lead to procedural heterogeneity. Procedure duration was longer in the low-dose group because the protocol required additional reconstruction and planning steps, which affected workflow. Complete blinding could not be achieved, and a second anonymized randomized reading to assess intra-observer variability could not be performed due to the operator-dependent nature of CT-guided lung biopsy and the absence of a third interventional radiologist in our institution. Additionally, the significantly higher BMI in the control group may have influenced imaging characteristics and procedural parameters, representing a potential confounding factor and limiting the comparability of the two cohorts. Future studies with BMI-balanced groups are needed to address this issue. Finally, the study focused on solid nodules and masses with malignant potential, so the applicability of the low-dose protocol to ground-glass lesions, often associated with early-stage malignancies, remains to be further explored.
Conclusion
Our results indicate that this low-dose protocol can be successfully integrated into interventional radiology practice for solid nodules and masses, offering a viable alternative to conventional high-dose protocols. We believe that our findings provide valuable insights into the development and standardization of optimized low-dose protocols in interventional radiology, paving the way for broader clinical adoption and further refinement.
Footnotes
Ethical considerations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
IRB approval
This study has obtained IRB approval from (BOLU ABANT IZZET BAYSAL UNIVERSITY CLINICAL RESEARCH ETHICS COMMITTEE APPROVAL-Decision No:2020/197 Date:25.08.2020) and the need for informed consent was waived.
Consent to participate
Consent for publication was obtained for every individual person’s data included in the study.
Author contributions
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
