Abstract
Intussusception refers to invagination of bowel loops into a neighboring, adjacent bowel segment. While it is not an uncommon entity in paediatrics—about 95% of intussusceptions occur in childhood, merely 5% of them affect the adult population. When affecting the later typically the small intestine is engaged rather than the colon. The diagnosis often represents with unspecific symptoms and is rarely considered a possibility in adults. In the past the diagnosis was typically made intraoperatively. As the Multi-Detector Computed Tomography (MDCT) of the abdomen became a referral diagnostic method, recognizing the signs of the condition is very important since some of the cases are transient, while others have an underlying malignant cause and more aggressive treatment is required. Surgical treatment planning is mandatory in those neoplastic complicated cases. The presented case report describes the role of radiology and the surgical treatment of a malignant ileocolic intussusception.
Introduction
Intussusception is a condition in which part of the bowel slides into the next, adjacent and larger part of the bowel. This usually leads to a partial or complete bowel obstruction. It is considered that only 1% of intestinal obstructions in adults are caused by intussusception.1–3 It is a rare condition, especially in adults, where it is considered to affect 2–3 people out of 1000,000 per year. 4 Ileocecal intussusception is the most common type of intussusceptions. 5 Imaging has an important role in identifying the cause and to establish complicated cases, where impaired mesenteric circulation and signs of parietal ischemia are present, since the later are associated with a higher risk of perforation and peritonitis. 3 Abdominal computed tomography appears to be the most sensitive modality in establishing preoperative diagnosis and can even have an important role in estimating the possibility of self-resolution. 6 Ultrasonography is a reliable imaging tool for children at low risk for intussusception; however, in classic diagnosis they need to be investigated by contrast enema, both for diagnostic and therapeutic purposes. 7 Bowel perforation is an absolute contraindication for an enema in any age and in this case surgical treatment is mandatory.
Case presentation
We present a case of a 72-year-old male presenting in the ER with complains of right hemiabdomen pain, diarrheic stool and subfebrile temperature for 3–4 days. No concomitant medical conditions have been observed, except long history of arterial hypertension. On the physical exam tenderness to palpation was noted in the right hypochondrium, where a moving palpable mass was felt. Physiological peristaltic was present. Due to the clinical complains and presence of claustrophobia subsequent i.v. contrast enhanced CT of the abdomen and pelvis CT was overtaken instead of MRI. CT was performed with 256 detector row computed tomography scanner, Brilliance iCT (Philips Healthcare, Best, Netherlands). Arterial and portal venous phases with slice thickness of 2 mm., followed by multiplanar reformation MPR in coronal and sagittal plane of 1 mm slice thickness were performed and images were revied on an IntelliSpace Portal 8.0 (IPS) workstation. Contrast administration by intravenous injection of iopamidol-370 with injection rate 4,5 mL/sec. Using power injector (Medrad Stellant CT Injection System; Bayer Medical Care, Indianola, Pa) was achieved. On arterial and portal venous phases the ileocolic invagination was observed with signs of inflammation and bowel ischemia. Figures 1(a) and (b). There was focally thickened bowel wall with nodular shape that was intensively enhancing in the post-contrast series suggestive of an underlying neoplastic process. Figures 2(a) and (b). Enlarged locoregional lymph nodes were also seen. The diagnosis of ileocecal intussusception secondary to a caecal adenocarcinoma was later confirmed intraoperatively. The ileocecal valve was the leading point of the intussuscepted colon, thus also confirmed on surgery. Figure 3 Contrast enhanced CT scans of the abdomen in porto-venous phase—coronal (a) and sagittal (b) views representing the bowel within bowel configuration ( Computed tomography axial views in arterial phase (a, b) demonstrating the focally thickened bowel wall, suggestive of an underlying neoplastic process ( Computed tomography in porto-venous phase axial view showing the diagnostic bowel within bowel configuration, equivalent of the ultrasound “target” sign (


At laparoscopic exploration, a loaded cecum and right hemicolon was found Figure 4. Because of the difficult exploration of the lower abdominal cavity requiring colonic manipulation, the procedure was continued by a hand-assisted approach. During manual reduction maneuver a massive ileocolic intussusception with invagination of the cecum and the ascending colon with underlying neoplastic formation. The latter was resected followed by end-to-end anastomosis. The patient had a full recovery and was discharged three days after surgery. The patient recovered and was discharged four days after surgery. Histological examination revealed dissemination with colon carcinoma in the intussuscepted bowel and standard chemotherapy was prescribed to the patient. Operative specimen of the right hemicolectomy and the resected colon segment showing the presence of the intussusceptum with underlying neoplasm.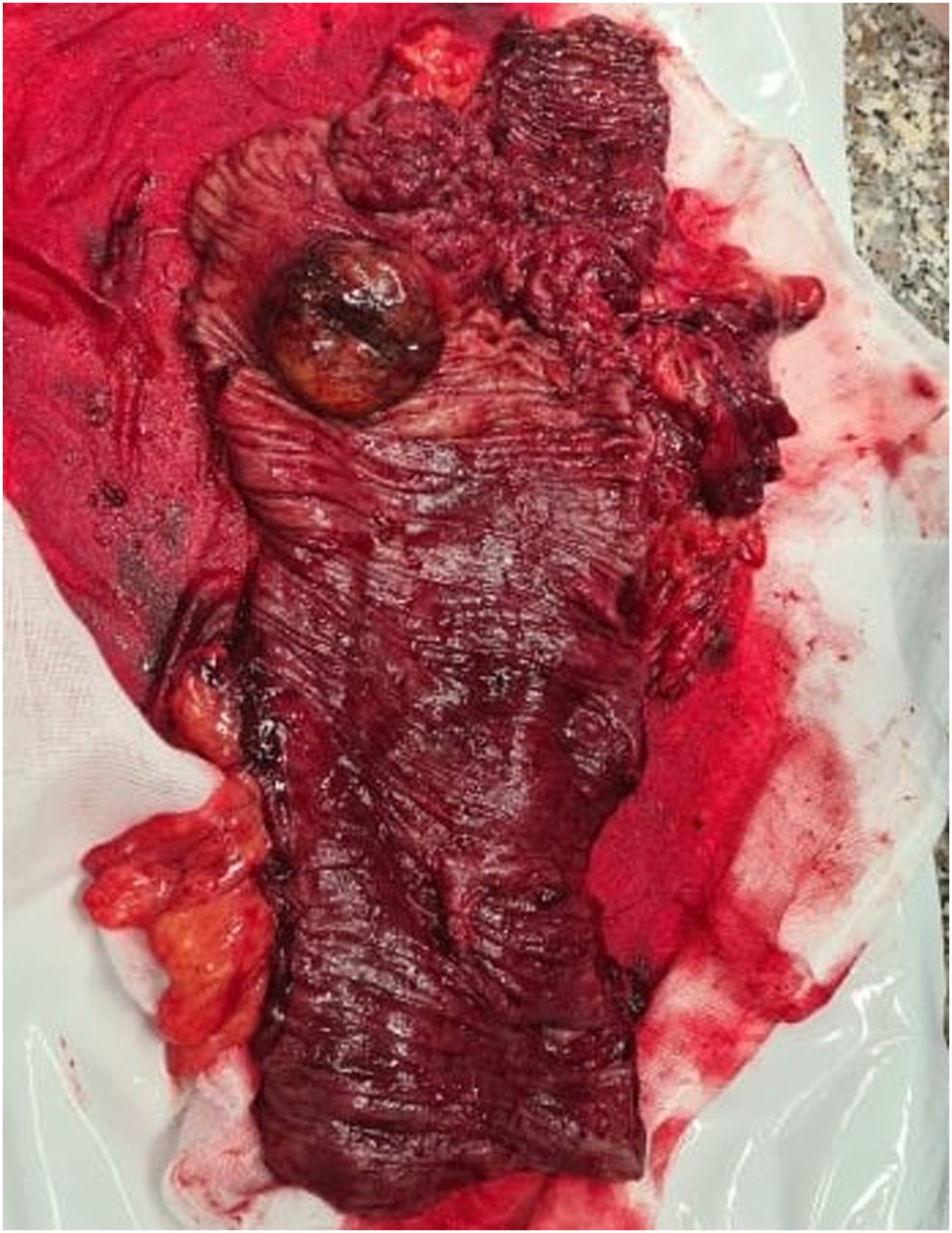
Discussion
Ileocolic intussusception in adults is a rare pathology presenting with nonspecific
The most common type of intussusception in the adult population is enteric and the majority of the lesions in this location are benign. 11
A frequently encountered benign lesion as an etiologic factor is a lipoma in the colon. If a lipoma is confirmed an intussusception reduction is the treatment method of choice. Unfortunately, it is considered that more than two thirds of the cases are caused by an underlying malignant tumor—more often in the colon. This leads to operative intervention being the method of choice in treating those patients. Primary resection is the usual approach and best treatment option, resp. Segmental colonic resection.
About 14% from all intussusceptions are ileocolic. 12 Colonic intussusceptions have most likely a malignant origin as in our case. As a consensus the resection should comply with the principles of surgical oncology, when large bowel is involved due to the higher incidence of underlining malignancy. In the majority of cases of ileocolic intussusception, a conventional right hemicolectomy is mandatory.13–15 A relationship with previous or ongoing chemotherapy is interesting to be assessed.
Surgical resection is the treatment of choice since in most cases the etiology involves an underling neoplastic process acting as a lead point. Prior reduction should be performed in patients with suspicion of benign origin and mainly in cases of small bowel intussusception without ischemia, while especially in malignant colonic intussusception this procedure must be avoid due to potential risk of embolization and dissemination of malignant cells.8,13,14,16 In our patient, manual reduction was unnecessary due to the already planned right hemicolectomy based on CT examination findings; however, an attempt has been tried without success. The recovery of our patient was beneficial and successful due to the laparoscopic hand–assisted mini-invasive surgical procedure.
In conclusion, intussusception in adults is a rare pathology and should be taken into consideration in patients with neoplastic bowel disease. Consideration of the condition and appropriate imaging modalities like MDCT can help achieve the right diagnosis and make the proper treatment plan and short-term surgical planning. As in adults a malignant lesion is often the reason for intussusception, colonic resection and anastomosis are necessary for curative or palliative results with better outcome in laparoscopic hand-assisted surgery and in regard of the oncological principles.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
