Abstract
Temporality, i.e. the concept of lived time, is important for understanding and encountering older individuals with dementia. Lived time is, however, sparsely studied among nurses when it comes to caring for people with dementia. This also seems to be the case with nursing students. We are not aware of any studies on the topic that have been conducted with nursing students. Thus, the aim of the present study was to answer the research question of what lived time is about when nursing students are caring for older persons with dementia in a nursing home. A phenomenological design inspired by van Manen's hermeneutical phenomenological approach was employed to analyse 11 interviews with seven nursing students. The study was reported in accordance with the COREQ checklist. Three themes were obtained: ‘the meaning of the older person's past in the present’, ‘moments of connectedness’ and ‘living in different temporalities – when time dimensions collide’. This study has practical implications for the care of older individuals with dementia. The findings suggest seeing older people with dementia living their time in the past and the present. The future, however, requires more attention in nursing. The meaning of the various moments illuminating lived time between the students and the older individuals with dementia is further discussed.
Introduction
Time constraints are common barriers to providing quality nursing care, and the reasons for nurses’ lack of time in healthcare settings are innumerable, affecting how they perceive nursing and themselves as nursing professionals.1–4 Realising time as equal for everybody, but perceiving time as different, remains pivotal in nursing. 5 Therefore, clock time and experienced time may disrupt the nursing care delivered. In this study, time as temporality in nursing is explored in the context of caring for older individuals with dementia.
Temporality refers to ‘the nature or structure of time, in terms of its objective existence, its subjective experience or both, particularly, with respect to the relationships among its dimensions (past, present and future) and the way in which it passes’. 6 , pp. 1351–1352
Caldas and Berterö 5 suggest that temporality in nursing appears as an unmeasurable nursing presence when the nurse is ‘being with’ the patient or is physically present (i.e. a measurable presence). Temporality in nursing is demonstrated when the nurse acknowledges the patient's thoughts about their life (past), their disease or daily welfare (present) or their future. Temporality is about trying to understand another human being and trying to find connections between different temporalities, preferably with tolerance and patience.
Lillekroken et al.'s 7 concept of ‘slow nursing’ is closely related to temporality in nursing. The authors define the core elements of ‘slow nursing’ as reflected moments of caring, a way of delivering good care, doing one thing at a time, and creating joy and contentment. Lillekroken 8 suggests slow nursing opens care through quality time, where time is treated as a resource through slow nursing. Hence, slow nursing is about nurses’ presence and draws nurses and people with dementia into a ‘moment’. 9 Thus, temporality in nursing manifests itself through being present and aware of the past, present and future.
Therefore, the theoretical framework of our study was inspired by van Manen's existential life world of temporality as lived time 10 , pp. 214–215; van Manen 11 divides time into clock time (objective time) and ‘phenomenological time’ (subjective time). He further encourages us to explore time in the phenomena we investigate and connect the past, present and future. Hence, a phenomenological understanding of time may occur in an individual's experience of lived time. Baars 12 emphasises that the experience of time should be shared with others in the form of narratives; human actions take and constitute time. According to van Manen, 11 , p. 815 ‘time is life, time is who we are’.
From a temporality point of view, individuals with dementia constitute a vulnerable group. 13 The stages of dementia are irreversible and the capacity for verbal communication during the later stages of dementia declines significantly. 14 According to the Clinical Dementia Rating (CDR) Scale, dementia develops in five stages. The fifth stage includes severe dementia accompanied by severe memory loss and disorientation of time and place. The person with dementia requires help with personal care and tasks of daily living. The patient no longer has problem-solving abilities, which significantly affects their daily lives. 15
However, it is important to bear in mind that Alzheimer's dementia is the most common form of dementia among the different types of dementia. Therefore, ‘dementia’ is the suggested term to use when referring to dementia in general. 16
The results of studies show contradictions related to the extent to which individuals with dementia experience the past, present and future.5,13,17,18 Caldas and Berterö 5 suggest that when this disease has progressed, the person's temporality might also be in a state of change as the person who is living her own time. However, in a study with 32 participants with mild Alzheimer's disease (AD), El Haj et al. 18 observed that individuals with AD rated their temporality toward the past more frequently, compared with participants who served as controls. Eriksen et al.'s 13 systematic meta-synthesis of 61 qualitative studies, in turn, described the experience of time for 762 individuals with dementia as important for managing their disease and their seeming involvement with time dimensions, for most of their daily lives. Thus, persons with dementia are not living in the past only. Lived time as past and present appeared more often, while the future seemed more precarious.
Interestingly, the results suggest that people with dementia often live in their own time. For instance, de Witt et al. 17 found that among 14 older women with dementia, holding back time represented the temporal meaning of living alone. However, the futures of the older women were about their fear that the illness might force them to leave their homes, as well as their forthcoming deaths. Hence, the perspective we take, as a premise in our view of individuals with dementia and temporality, is a person who is still experiencing life as the past, present and future. The above reported studies focused on people with dementia and suggested a need for further research on individuals with a severe form of this disease.5,13,17,18
Eriksen et al. 13 claims that people with dementia are disadvantaged by their lack of a temporal norm for communication. Therefore, past-, present- and future-oriented dementia care needs to be strengthened when supporting older individuals with dementia.
Furthermore, how temporal norms are valued in nursing is an important issue because nurses’ perceptions of time may impact on how they relate to older people with dementia. Thus, lived time raises both practical and ethical challenges in nursing.
Nursing students are trained to care for older people with dementia, but studies about nursing students’ as well as nurses’ experiences of the phenomenon of temporality seemed to be scarce. Nursing students are generally young, and it can be assumed that their time orientation is towards the future rather than the past. This makes it interesting to explore their reflections of lived time when encountering older individuals with dementia. Thus, the aim of the present study was to explore temporality in nursing by answering the following phenomenological research question: What is lived time about when nursing students care for older persons with dementia in a nursing home?
Material and methods
The design
This study used a qualitative inductive, phenomenological design and a hermeneutic phenomenological approach. Individual interviews were conducted with nursing students exemplifying the phenomenon through lived experiences as experiential examples and stories. 11 This study was reported in accordance with the Consolidated Criteria for Reporting Qualitative Research (COREQ) checklist. 19
The setting
This study was conducted at a municipal nursing home, with six dementia care units, located in the northern region of Norway. The facility delivered professional care to approximately 50 people with dementia, of whom the majority (we were told) were in stage 5 of the disease. 15 It employed approximately 100 professionals, including specialised nurses, specialised nurses in geriatric care, auxiliary nurses and healthcare workers. The nursing management consisted of three people, of whom all were nurses. The nursing home had a reputation as a good learning placement20,21; therefore, it was expected to be a suitable setting for collecting data on experiences related to the research topic. The nurse managers and mentor nurses were informed about the project and gave the researchers permission to conduct this study.
The participants
Eight nursing students (four in their first year of studies and four in their third year) who enrolled in a clinical placement in the nursing home during spring 2019 were selected as a convenience sample. The students were chosen by the university's administration. They had varied backgrounds: all of them were women aged 20–35 years; two had a bachelor's degree (in other fields) and six had higher secondary degrees. All except two of the first-year students had gained experience at other nursing homes, but not necessarily with dementia care. All of the students’ placements were in dementia care units. The third-year students’ placements were mainly in nursing administration, which included supporting first-year students. Appointments were scheduled with the nursing students by two supervising lecturers who were not involved in the study. The first author was invited by the supervising lecturers to inform the eight students about the study's topic: the past and present and the future of the persons with dementia. The students were informed about the possibility of participating in a follow-up interview.
Data collection
The first author conducted 12 individual audiotaped interviews, at the beginning and end of the eight-week clinical placement in the nursing home. All eight students participated in the first interview, but the third-year students stated they did not have ‘more’ to add to the topic or did not want to participate twice. One third-year student's statements did not contribute to the topic, so the student was excluded; thus, 11 interviews remained. Most of the interviews were conducted without interruptions; however, nursing staff tried to enter the room on a few occasions to retrieve something. Notes were written after each interview to support the subsequent interview. The first author created verbatim transcripts out of 9.5 h of recordings, and the duration of the interviews was in the range of 22–71 min., with a mean duration of 46.5 min. The shortest interview was a follow-up, and the longest was a single interview.
The interviews began with the open question, ‘When you think about the older people with dementia at the nursing home, what experiences do you have about their past, present and future? Could you please tell me?’ The students were encouraged to speak openly about the topic. Only in cases of short pauses did the researcher interrupt with questions, such as ‘Could you tell more?’ or the researcher continued with a follow-up question related to the student's last answer. The questions in the follow-up interviews were based on the students’ answers in the first interview. The nursing students reflected on their encounters with the older individuals with dementia and their dementia condition. Whenever possible, the researcher listened to their reflections in silence.
Analysis
This study used a hermeneutic phenomenological approach inspired by van Manen.10,11 Three researchers, of whom two were authors, participated in the analysis. The first author read the text of the transcriptions several times and tried to capture its meanings. Each individual student's transcript was read as a whole and written as a ‘story’. A total of seven ‘stories’ were written and named (see ‘Results’ with students’ pseudonyms). The stories of the students who shared them in depth were retained but shortened throughout the analysis. Thus, experiential material/meanings were highlighted in the ‘story’ text. 11 Thereafter, the meaning contents describing the phenomenon of lived time were grouped, revealing eight ‘sub-themes’ and three ‘themes’, 11 which the researchers discussed, revised and finally agreed upon. 22 The researchers’ pre-understanding of the phenomenon under study, both theoretically and practically, raised their awareness during the analysis. We all had experiences from nursing education and aged care. Therefore, our intention was to read the material before asking ‘What it is really telling us?’ Thus, the adoption of a phenomenological attitude was actualised, but not far from our pre-understanding. 23 For instance, the various ‘moments’ as the sub-themes of lived time made us wonder about our understanding of time. An example from the analysis is presented in Table 1.
An example of a thematic analysis.
Selected text from Berit's story with marked experiential material/meanings:
Berit said that dementia was not unknown to her, as a female family member had the disease. She felt she was unable to communicate and connect with her. Therefore, she felt unsure when all the patients would be the ‘same kind of persons’. She spoke about a female patient who mostly did not speak, and if so, it was meaningless sentences. She found it distressing to help an adult with personal hygiene in the shower. Surprisingly, she states: ‘
She continued:
‘

Ethical Considerations
The Norwegian Centre for Research Data No.49229 approved the data collection, storage and handling of the study's materials. This study was exempted from the approval requirement by a regional research ethics committee according to Norwegian legislation because it did not include research questions related to health or the patient's personal information. The ethical principles of the World Declaration of Helsinki were followed during all phases of the study. 24 Students gave their informed consent to participate after receiving oral and written information about the project. The authors informed the participants that the interviews were voluntary and independent of their clinical practice and studies, and that they could withdraw from the study at any time. Beyond this, none of the authors was involved in the students' studies. The patients were not identified in any of the study's materials; thus, informed consent was not required from the patients or their next-of-kin.
Results
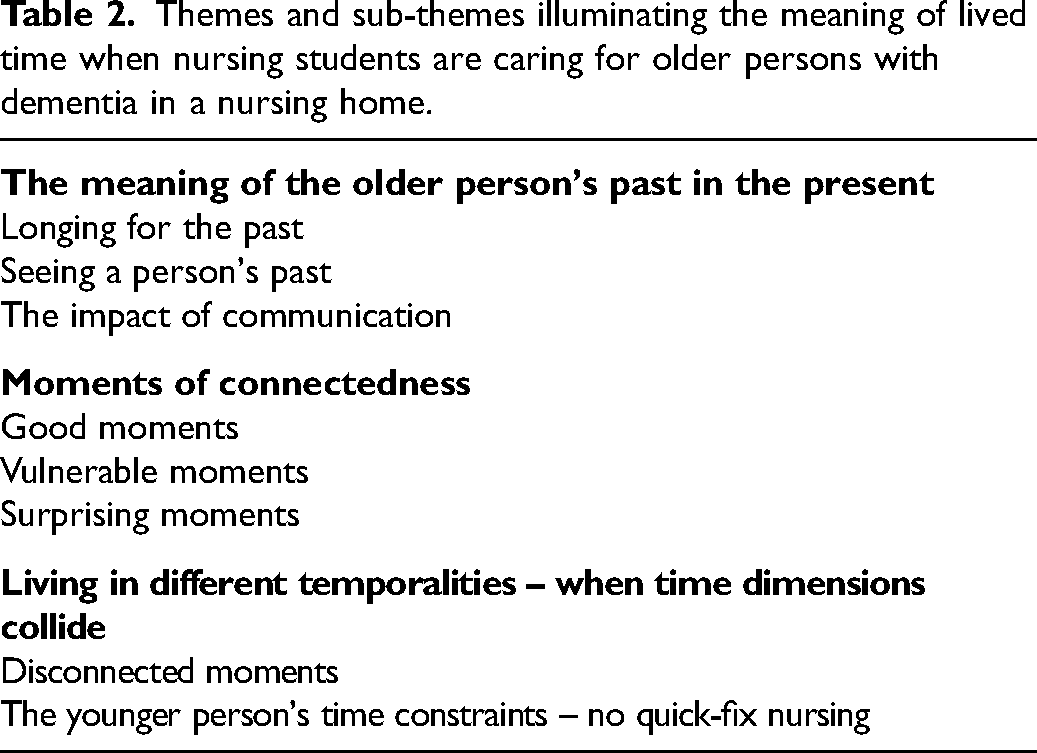
Seven first-year (Anna, Berit, Caroline and Diana) and third-year (Eva, Frida and Gro) nursing students shared their experiences of lived time as reflected in the following themes and sub-themes (Table 2).
Themes and sub-themes illuminating the meaning of lived time when nursing students are caring for older persons with dementia in a nursing home.
Theme 1: the meaning of the older person's past in the present
Longing for the past
The nursing students showed an understanding of the lived time of the older individuals, who were longing for the past in the present and not fulfilling their roles as mothers, which may have connected with the student's own understanding of motherhood. Motherhood was experienced in the life worlds of the younger and older people. Gro, who revealed that she had children herself, seemed to acquire an understanding of the older women's sorrow and despair. Their urgent concern about returning home with their children, who were sitting in the waiting room at the nursing home, was apparent. Gro said, ‘In the event it was me and I was told “you have to stay because you live here” and I knew my children were waiting outside, but I wase locked in, how terrible would that be (loud)?’
Older individuals may experience living the past in the present when they are outside of the nursing home. For example, Berit seemed to acquire an understanding of why individuals with dementia wanted to return home: ‘The older individuals are unique people with the same needs as us and they don’t feel sick (with dementia)’. They might assume responsibilities outside of the nursing home. Gro emphasised the importance of learning about the lived time of one of the older people. She said: ‘It is necessary to know the older person's history because they might either experience peace or become restless when they are connected to their history’. Therefore, the older individuals showed students the meaning of their past, as described by the students.
Seeing a person's past
The students experienced their roles as connectors of the older person's past and present. Furthermore, the students experienced the lived time of the older individuals as a resource from which they could learn. Eva pointed out how important it was to be aware of lived time despite dementia. She emphasised the students’ potential contributions: ‘We can support the older persons’ focus on the persons they have been and the persons they are today, by understanding their life experiences’. Despite one's own limitations, it was important to acquire this knowledge. Caroline was committed to learning from older individuals by listening to their life histories about how their lives have been, such as their childhood, adolescence and adulthood, family, relationships and war experiences, to mention a few’.
Humour and personality awareness may enhance connecting with the past and supporting students’ understanding of an older person's present. Caroline thought humour was useful for helping older individuals with dementia connect with the past, which occasionally evoked smiling and relief: ‘Well, it makes the day for the older people, and I have learned to be aware of their personalities’. She felt her understanding of the older individuals with dementia present improved.
The impact of communication
The nursing students, who were living their time and focusing on the future, enjoyed communicating and connecting with the older individuals. Communication about the people’s past and their histories and memories during daily chats were important connectors to the present. Berit explained that she only wanted to complete the Age Care course in order to become a nurse, but then she said: ‘it surprised me when it was possible to communicate with the older individuals with dementia’. Diana, in turn, emphasised the meaning of communication: ‘When older persons make contact, I find it interesting to ask them about the old days, and to listen to their past life experiences and memories, which seem to brighten them up and make their day’. Eva emphasised moving to a nursing home, when one would no longer be able to engage in everyday chatting:
Theme 2: moments of connectedness
Good moments
A good moment for the older person with dementia seemed to be a good moment for the nursing students as well. Berit said, ‘I lived on the feeling the entire day. I connected to her in a moment. I will remember the moment she [the patient] had for the rest of my life, I think. I get emotional (tearful). It is exhausting, but beautiful. It is a nice moment when you give a lot of yourself; it makes me want to look the older persons in the eye and be there for them.’ Sharing good moments contributed to the development of the student, herself. Anna said, ‘It is a good feeling to experience moments’. Diana said she felt connected with the older individuals. Smiling people made her happy and touched her: ‘They show they are in a good mood and have a zest for life. I think it is rewarding to share experiences and nice moments with them. You feel you have developed as human being yourself.’ The experience was about shared moments confirming humanity and dignity.
Vulnerable moments
Vulnerable moments challenged the nursing students and were shared in those moments. Berit talked about an encounter with a male patient who cried easily and experienced despair when he was forgetful, and it was noticed. He broke down crying when the staff told him that his loved one had visited him and he could not remember her attendance. ‘I sat with him in silence holding his hand. I tried not to help him by using words. It was about presence, not letting him sit alone with despair (sigh). It must be a very scary experience for him. I visited him several times that day.’
Gro stated that ‘it feels devastating when you are unable to help. As a student, you may feel neglected many times, which hurts because you are a human being. Don’t try to cheat with them [the patients] because they are vulnerable.’ It was about shared moments that confirmed the vulnerability of life itself.
Surprising moments
The nursing students’ initial understanding of connecting with individuals with dementia changed. Communication about children connected the life worlds of the younger and older people. The lived time was sometimes about moments and minutes. Berit stated that she was familiar with dementia because a female member of her family had the disease. Berit felt unable to connect with her. Therefore, she had unpleasant feelings at the beginning, when all the older individuals at the nursing home seemed like they would be the ‘same’. At the nursing home, she met a woman who rarely spoke, and when she did speak, her sentences were meaningless. She found it distressing to help an older person with showering. Surprisingly, she stated: ‘It was so natural to help her and when she asked if I could wash her hair, I answered, “Sure”. I felt it was the most natural thing, almost like helping my own children. I thought about dignity as we were talking about our children. Afterwards, I was sure she would forget our talk, but after 5 minutes she surprisingly asked, “What about your 5-month-old son? Is he with his father now?”’ Berit ended her description by reporting that her supervising nurse confirmed that she really had connected with the older person.
Theme 3: living in different temporalities when time dimensions collide
Disconnected moments
Living in different temporalities when time dimensions collide is characteristic of disconnected moments. Lived time was experienced as lack of time, and encountering older individuals with dementia from a younger person's life world could hinder the younger person's understanding of the older person's lived time. Frida talked about experiences with inadequate time to socialise with older people because nursing procedures took up all their nursing time. She also found it difficult to communicate with older individuals who lacked skills. She was curious about whether older people felt lonely because many of them were forced to be alone. She thought younger people were more social. She said she would feel alone in their position, but she never encountered those feelings herself. Frida also thought it would be difficult to ask older individuals about this topic. There was hesitance to engage in mutual communication.
Disconnected moments of lived time in the present surprised the nursing students and could have caused misunderstandings. However, the students learnt how important it was to try to understand the person in her/his life world. Anna said that she met a man who needed to visit his sister. The patient had good memory and manageability, combined with disorientation. When she recalled his life story, she knew he had a wife, but could not remember staff talking about a sister. The student thought the older person was having a moment of disorientation and said to him, ‘You are at the nursing home now. We did not hear about your sister, so you will stay with us.’ The person became distressed and refused to communicate with her afterwards. Later, she was informed that his sister called him now and then. She said, ‘You learn you have to listen better’. Anna did not expect the older individuals with dementia to provide accurate descriptions of themselves and their health situation. There was resistance to communicating on an equal level.
Time constraints of the younger people with ‘no quick-fix nursing’
The nursing students felt frustrated because they could not manage the incurable disease. Eva and Berit said they were accustomed to fixing things but could not fix dementia. Gro added: ‘They will never recover; this disease is brutal’. Therefore, students’ views of dementia could be an obstacle to seeing the futures of older individuals with the condition. However, the students emphasised that being present with an older person was pivotal. It was necessary to accept time constraints and setbacks. Diana said, ‘You cannot give the level of care you wish due to planning and prioritisation, but care must come from the heart’. Lack of time to spend with older persons was distressing. Eva appreciated ‘having the time to sit down with older persons and not have to rush all the time with a schedule so busy the person is left alone’. Caring for older individuals with dementia requires time and patience to show respect for their vulnerabilities.
Discussion
This study explored temporality in nursing by answering the research question: ‘What is lived time about when nursing students are caring for older persons with dementia in a nursing home?’ The findings have illuminated lived time, including the past, present and future, through the students’ care encounters with the older individuals. Thus, lived time appeared to be explicit or implicit during those encounters when the nursing students deepened their understanding of the phenomenon.
The findings consisted of three themes: ‘The meaning of the older person's past in the present’, ‘moments of connectedness’ and ‘living in different temporalities when time dimensions collide’. The results are reflected against van Manen's11,25 phenomenological or subjective and objective clock time to deepen one's understanding of the lived time caring for older individuals with dementia.
Studies5,13,17 have shed light on the importance of understanding older people with dementia living their own time. This was also the case in the present study. The meaning of the older individuals’ past in the present was about understanding how the older person with dementia lived the past, seeing themselves as the person they were at that time. It seems natural for older people to long for the past and to expect another person to be able to see the person's past. van Manen 11 claims that the meaning of lived time is in the humanness of being a unique person. The students showed awareness of the older individuals with dementia in this study, seeking them out for contact and communication. This approach proved to be an essential starting point for understanding older persons’ lived time.
Communication is valued by van Manen, 11 , p. 817 who asked, ‘What is a true conversation?’ He claimed it was ‘a certain mode of togetherness, a way of sharing a world, understanding and trusting another, experiencing a shared sphere and each other's company. We can speak or we can be silent because we feel totally immersed in this shared conversational space.’ A conversation in silence was exemplified by the nursing students as holding the older person's hand. There was no need for words. van Manen 11 emphasises it has to do with thoughtfulness and tact and characteristics of importance when experiencing connecting moments.
The nursing students experienced various moments of connectedness with older individuals with dementia. According to van Manen, 11 being in the moment and in the presence of the now is when time seems to stand still. The meaning of being present with an older person, preferably in an unmeasurable presence, may draw nurses into the moments.5,9 The good moments that connected the nursing students and the older persons with dementia, even if they were living in different temporalities, meant that they met in the present and created something uniquely good for the older individuals who were also important to the students. For instance, the meaning of good and rare moments has been emphasised by Svendsen et al., 26 who described how caregivers in a nursing home experienced ‘magical, fleeting moments’ in which the person with dementia showed contentedness. Performing slow nursing,7–9 as reflected in moments of caring and being aware of quality of the time as a resource of good care, may enhance connecting moments.
Perhaps such moments can occur more easily and be experienced by both nursing students and older individuals with dementia when the students take the time to follow the older person's lived time, and thereby create good encounters. Eriksen et al. 13 stressed that we can learn from older people with dementia about time as living in the moment. In the connectedness between the younger and the older individuals with dementia, the students experienced vulnerable moments when the vulnerability of the older people touched the students’ own vulnerability. To show vulnerability is to show humanness. 11 For caregivers, the humanness of their vulnerability may be both a burden and a resource for care because it involves feelings and pain as well as courage and openness. 27 The vulnerability of older individuals has a deeper sense; it is associated with being harmed and violated easily by others. This opinion was supported by the nursing students in the present study, bearing in mind that the capacity to feel and grow as an older person also requires having the strength to cope with vulnerability. 28 Despite dementia, it is still about the old person.
The surprising moments occurred when nursing students unexpectedly connected with the older individuals with dementia and their insight about the older people’s lived time expanded. Maybe it was about seeing the older individuals with dementia as experts of their life world, when emotions could become overwhelming both for the older people and the students themselves. van Manen 11 claims it is phenomenological time, which speaks to our humanity. The nursing students emphasised developing humanness in oneself.
The nursing students further illuminated the meaning of catching the eye-contact of an older person with dementia. This is supported by van Manen, 11 who described it as ‘the meaningful look in eye-contact’ happening when we feel the eyes ‘catch’ each other in the look. The pupil of the eye touches the essence of the other; it is a pure touch where we encounter the other's infinite otherness or secret. These moments seemed to be about human connectedness in its purity, between the students and the older individuals with dementia.
Connecting was more complicated. The meaning of living in different temporalities, when time dimensions collide, was defined by the nursing students as disconnected moments with older people with dementia. Understanding the older person's lived time was not easy. Furthermore, the time constraints of the younger individuals were obstacles to connecting with the older people. As Caldas and Berterö 5 have emphasised, neither a state of measurable presence nor objective clock time 11 will necessarily connect with the older individuals.
The future was barely mentioned, which raises questions how this may have affected the dementia care given. In fact, some of the nursing students thought it was important to live life despite the disease. Caldas and Berterö 5 stressed the importance of being in the present and understanding how dementia impacts the daily lives of those who are affected. Eriksen et al. 13 confirmed the observation that older individuals with dementia were occupied by living in the present, and not always thinking about the future. As van Manen 11 , p. 104 in turn has claimed, ‘in lived time there is hope and becoming; there is a future. Lived time is also our temporal way of being in the world, as a young person oriented to an open and beckoning future or as an older person recollecting and memorising the past.’
At least the nursing students, as younger individuals, in this study applied their understanding of lived time and illuminated what living in different temporalities means to the care of older people. However, the most important question was whether the nursing students were able to deliver nursing care to older individuals with dementia in the temporality zone where both of them were living.
Temporality in nursing practice
This study adds a component of nursing care, i.e. the meaning of ‘the moments’ to temporality. Connecting in the moments has been suggested to be a component of nursing competence in the care of older individuals with dementia. Time to reflect and wonder about the ‘slow’ temporality in nursing is essential.5,7–9 This could be supported by ‘slow thinking’ and ‘slow wondrous listening’ to develop a wonder-based practice. 29 This type of reflection is expected to support good care.
Strengths and limitations of the study
The use of the same opening interview questions for the participants and offering them the opportunity to participate in a follow-up interview can be seen as strengths of the data-collection process. Further, the individual participants' ‘voices’ throughout the analysis were supported.11,30 Due to the method, the richness of the materials was greater than the number of participants.11,31 The analysis has been described as being as transparent as possible, and it conducted using the COREQ checklist to improve the transferability of the research process. The researchers (with PhDs) had experience for conducting qualitative research. Furthermore, all researchers acknowledged adopting a reflective attitude towards the phenomenon being analysed and studied.
The present study has some limitations. One limitation is that only female students participated. We could not control for this gender imbalance because it reflected the gender distribution among nursing students. Another limitation is that first-year and third-year nursing students were selected for this study, but we did not have control over the sample selection. A third limitation is that the third-year students chose to participate only once, although those students had more nursing experience and were expected to be more prepared to exemplify the topic. On the other hand, a third-year student's material did not qualify for the analysis. The first-year students might have chosen to participate in the follow-up interviews to deepen their reflections. Therefore, a decision was made to cancel the comparison of the material between the first- and third-year students. As the results showed, both the first- and third-year nursing students contributed insightful material to this study. The study was conducted with nursing students in one nursing home; therefore, the results might not be directly transferrable to other clinical placements that provide care for the aged.
Conclusion
This study adds to the knowledge of temporality in nursing. Providing good care to older individuals with dementia needs further attention. First, how time is lived as the past in the present is still of concern. Second, after seeing older people with dementia continuing their lives in the present, despite having dementia, raises the question how nurses could enhance connecting through various moments of the care process. Third, the futures of older individuals with dementia are likely to require more attention in nursing. Fourth, awareness is needed of how different temporality zones and a younger person’s understanding of an older person's ageing experience may hinder connecting moments. This study recommends reflecting upon lived time in healthcare and educational settings to deliver good care to older individuals with dementia.
Footnotes
Acknowledgements
We wish to thank the nursing students who participated in the study. We thank professor Åshild Slettebø, University of Agder, Norway, for supporting discussions and participating in the analysis.
Author contributions
GK formulated the study design, carried out the material collection and analysis, and drafted the paper. AS contributed substantially to the analysis and critically revised the paper draft. Both authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Norges Forskningsråd (grant number 256647).
