Abstract
There is a lack of knowledge about healthcare professionals’ perspectives on rehabilitation in relation to heart failure. Still, collaboration between different professionals can impact patients. The purpose of this study was to describe healthcare professionals’ perceptions of their work with patients of working age with heart failure. The sample population consisted of six nurses, one physiotherapist and one cardiologist. One individual interview and two focus-group interviews were conducted. The interviews were analyzed using qualitative content analysis. Three descriptive categories were constructed: ‘the impact of heart failure on patients’ life situations’, ‘heart failure service’, and ‘patients’ process of returning to work’. To support patients, healthcare professionals need to find ways to combine patients’ personal needs with protocol-driven care.
Introduction
Worldwide, heart failure is a prevalent condition and an illness which has an impact on public health. Approximately 10% of patients with heart failure are of working age. The condition is characterized by shortness of breath and fatigue. Patients are treated in hospital during acute exacerbations. After hospital discharge, they usually become sick listed for a period of time. Additionally, they are appointed to multidisciplinary teams at heart failure clinics, either in the hospital or in a primary care setting, during rehabilitation. 1 These teams incorporate interprofessional collaboration between specialized heart failure nurses and cardiologists/physicians. 1 Patients are also encouraged to participate in exercise programs led by physiotherapists. 2 Accordingly, physiotherapists are often part of the interprofessional teams.
Collaboration between different healthcare professionals is considered a prerequisite for optimal heart failure care. 3 The relationship between healthcare professionals and patients forms a foundation in the management of heart failure. However, there is a lack of knowledge about professionals’ perspectives on rehabilitation in relation to heart failure. There is some previous knowledge but, to an extent, it is contradictory. Healthcare professionals can have divergent and sometimes conflicting views of one another. For example, both physicians and physiotherapists attribute significance to psychosocial matters in patients with back pain, but the views of general practitioners and physiotherapists can differ concerning work discussions with patients and concerning ways to manage patients’ pain. 4 In turn, nurses and physiotherapists claim that they have more time to spend with patients than do general practitioners, and nurses claim that they offer greater accessibility to patients than do general practitioners. 5 Conversely, general practitioners can perceive that they are better placed to manage patients with complex health problems and have a more holistic view of patients than do other professional groups. 5 Conversely, general practitioners can perceive their cooperation with other professionals concerning medical certification as being positive. 6 Then again, not all physicians welcome specialized heart failure nurses. 7 At the same time, specialized heart failure nurses are well equipped to facilitate communication within multidisciplinary teams and they can perceive themselves to be more efficient than cardiologists in addressing the needs of patients. 8 Obviously, these contradictory findings can be caused by different research perspectives or by different undertakings to accomplish research protocols. However, they can also reflect contradictory realities.
If healthcare professionals have divergent perceptions of each other or of their own roles, it can have consequences for the interprofessional collaboration surrounding the rehabilitation of patients. This can eventually have consequences on the life situations of patients. It has been reported that patients with heart failure struggle to manage their illness and daily lives. But it has also been reported that people of working age with heart failure perceive that they are abandoned by healthcare professionals, which implies that they are left to handle a complicated life situation on their own. 9 In addition, a lack of coordinated care exists, which leads to vicious cycles of unplanned hospital readmissions. 10 Hence, it is not unreasonable to assume that unclear roles or inadequate collaboration can be one of several reasons for such experiences. The aim of this study was to investigate how healthcare professionals perceive collaboration and their work with patients of working age with heart failure.
Methods
A qualitative descriptive research design with an inductive approach was chosen for this study. The data were collected in 2012 in two focus-group interviews and one individual interview. The interview content was analyzed with openness and with a bridled understanding in accordance with the principles of reflective lifeworld research. 11 Bridling means that the researchers take on a self-critical attitude that involves systematic reflection and discussion within the research team on any pre-understanding and understanding, and also that the evolving analysis and findings is unceasingly questioned by the researchers. The study was approved by the regional Ethical Review Board in Uppsala, Sweden (2011/074). Purposive sampling was used. The head nurses of different cardiac clinics at three hospitals identified healthcare professionals who were interested in participating in the study. The hospitals were located in different urban communities in Sweden. The first author and the head nurses had telephone contact with one another.
The head nurses made arrangements for the interviews and verbally informed the eligible informants about the study. The information included the study’s aim, that participation was voluntarily and that data would be handled in confidence. Participants were informed that they could withdraw at any time. Prior to the interviews, the participants signed a written consent form.
Data collection
Two focus-group interviews were conducted (Interviews 1 and 3). The focus groups included a total of six registered nurses (five females and one male) and one physiotherapist (female). There was also one individual interview conducted with a male physician (Interview 2). The length of participants’ experience of working in specialized heart failure care ranged from 3 years to 21 years (mean 12 years). The second and the third authors conducted the focus-group interviews. The first author conducted the individual interview. The interviews took place at the participants’ workplaces. Prior to the interviews, the participants were again provided with written and verbal information about the study. During the focus-group interviews, the first author acted as a moderator to guide the discussion and to help participants reflect on their experiences. The third author took notes and ensured that all of the participants participated in the discussions. Consequently, both researchers posed questions, listened, and completed the process with follow-up questions.
Open and unstructured questions were used so that participants could reflect on their experiences. 11 The researchers asked the same initial question in all of the interviews, which was, ‘Could you please tell us about your work with patients of working age with heart failure?’ The follow-up questions varied depending on the interview’s progress. These included questions such as, ‘How do you mean?’, ‘In what way?’, and ‘Can you expand on that?’ All three of the interviews lasted for approximately one hour and were digitally recorded and transcribed.
Data analysis
The initial part of the analysis was conducted by the second and last authors. In the later phases of the analysis, all of the authors participated. A manifest qualitative content analysis was conducted in accordance with Graneheim and Lundman. 12 The categories of the qualitative content analysis refer to a descriptive level of content. Thus, the categories describe the manifest content in text. 12
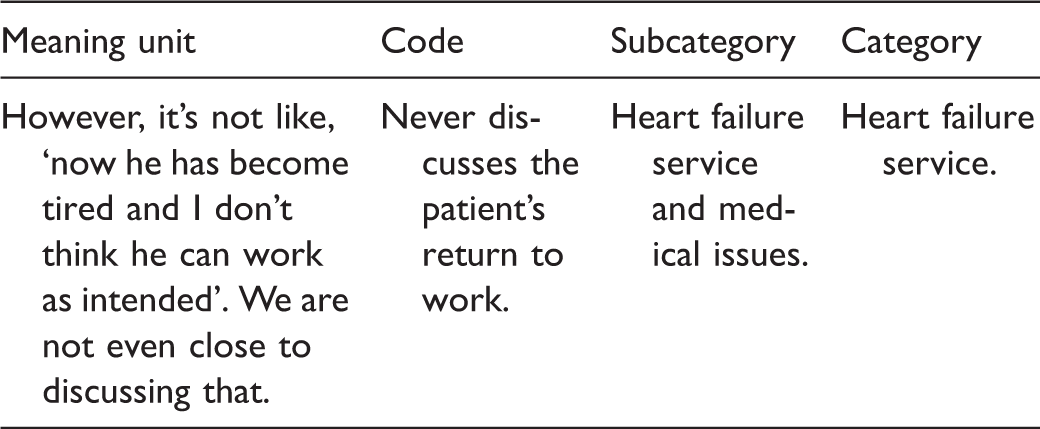
Examples of the analysis process.
Findings
The content analysis resulted in three descriptive categories: ‘The impact of heart failure on patients’ life situations’, ‘heart failure service’, and ‘patients’ process of returning to work’. Each category contained subcategories. Quotations from the interviews were used to illustrate the content. ‘Younger patients’ refers to patients of working age.
The impact of heart failure on patients’ life situations
The participants acknowledged that patients diagnosed with heart failure were challenged by their new and difficult life situation, which was signified by vulnerability. The participants also believed that patients’ subjective experiences could conflict with external demands for measurable objective data.
A new and difficult life situation
The participants perceived that it was shocking for patients to be diagnosed with heart failure in the middle of their lives. They also perceived that patients could associate their diagnosis with death. ‘Because the heart, it’s loaded with anxiety. It’s actually about death’ (Interview 3, registered nurse [RN] 1). Although patients of working age were not considered to be as ill as older patients, they believed that patients needed time to ‘land’ and to come to terms with their new and difficult life situation. The participants perceived that patients had an excessive need for support. If patients had concerns regarding family, work or finances, the situation was even more complicated. All at once, the participants said that patients were responsible for their own situation.
Patients’ vulnerability
The participants believed that patients had a particular vulnerability in relation to social insurance. They said that patients could feel insignificant and wanted to be listened to but that social insurance administrators did not listen. The participants perceived this as being a possible cause of conflicts between the administrators and patients. They also described patients’ vulnerability in relation to healthcare professionals and that patients were at risk of not being seen or heard. As a consequence, patients could be poorly treated by both the social insurance and the healthcare system.
Conflicts between subjective experiences and objective data
The participants described heart failure as a condition with no outward signs, meaning that other people such as employers or social insurance administrators could have difficulties in understanding and assessing patients’ work abilities. ‘You’re not sick if it’s not visible on the outside’ (Interview 1, RN 1). Subsequently, when patients were unable to work, they could be treated with disbelief. The participants also perceived that social insurance was assigned to get patients back to work. However, to make objective assessments, social insurance administrators had to distance themselves from patients. In addition, the participating physician perceived that social insurance administrators could have difficulties in assessing and interpreting medical data. He perceived that it was difficult to convey a patient’s story in a medical sick leave certificate. ‘I think these certificates do not always convey the whole picture’ (Interview 2, Physician). The physician also perceived it as more problematic to assess the work ability of patients with heart failure than of those with other serious illnesses.
Heart failure service
The participants believed that younger patients with heart failure were rarely referred to primary care. Instead, they were seen annually by interprofessional teams at hospital-based heart failure clinics, which the participants perceived created continuity. They considered physical activity to be particularly beneficial for patients. However, at the same time, the organizational structure surrounding heart failure patients of working age was perceived as being partially unsatisfactory.
Supportive interventions
The availability of heart failure services was perceived as being important for patients. The participants perceived that each patient’s unique needs formed the basis for supportive interventions. ‘And I usually consider the patient in front of me. What would be interesting to bring up and so on’ (Interview 1, RN 2). The participants described encouragement and listening as supportive measures that could strengthen patients’ self-confidence. They also said that the heart failure service offered the possibility to provide patients with different supportive activities, such as medical treatment, information and knowledge, which they believed created security and reduced anxiety. They also perceived helping patients relax and instructing them to listen to their bodies as being supportive.
Physical activity as a supportive measure
The participants thought that physical activity was beneficial for patients. The physiotherapist in particular acknowledged this, but the nurses and the physician acknowledged it as well. They believed that physical activity was available to all patients with heart failure and that patients became more confident about their physical capabilities if they received information and performed physical activities, in a group or individually, under the guidance of a physiotherapist. They also believed that patients could support each other in group activities because that allowed them to meet other patients who were in the same situation, which meant that experiences of being alone could be reduced. ‘And this interaction, they sit and talk and support each other. You hear the way they talk. I think it’s very important for the younger patients, to know there are other people in the same situation’ (Interview 3, Physiotherapist). The patients were generally motivated to engage in physical activity, and the participants believed that patients were more capable than they believed they were. In addition, the motivation of patients increased when they were encouraged to trust their own bodies. The participants believed that this reduced patients’ fear and also increased their security and self-reliance. They also perceived it as being important that patients did not see physical activity as a compulsion. If patients were not motivated to exercise, the physiotherapist thought that medical professionals could not take over patients’ own responsibility.
Medical issues
The participants perceived that cooperation between different professionals at the heart failure clinic primarily concerned medical issues. It’s all about medical matters, patients should reach certain doses. We discuss with the doctor about what to do now (…) However, it’s not like, ‘now he has become tired and I don’t think he can work as intended’. We are never even close to discussing that. (Interview 3, RN 4) I’ve been contacted by patients concerned about their sick leave running out but it’s not within my field, I cannot help them with the sick leave certificate (…) I refer them to the doctor, ‘If you think you’re not ready, you should talk to the doctor’. I don’t know what else to do. (Interview 3, RN 5)
A lack of structure
The participants described a lack of structure regarding the age of patients with heart failure. This lack of structure was particularly described in relation to physical activity. The physiotherapist said that physiotherapists rarely received referrals from the heart failure services regarding younger patients. The participants believed patients of working age had other needs than those of older patients. The participants also believed that patients of working age risked feeling unappreciated or could lose confidence in their own ability when they were forced to exercise with older patients. ‘With those who are young, you can really feel they don’t get to decide for themselves’ (Interview 3, Physiotherapist). Thus, to motivate the younger patients, the physiotherapist would occasionally construct individualized exercise programs. In addition, the participants perceived the written patient information as being directed toward older patients, which signifies that the content did not focus on relevant lifestyle changes from the perspective of patients of working age. They also said that physicians rarely monitored the physical activity of patients even though nurses and physiotherapists cooperated well. The physiotherapist could raise questions at so-called training rounds, but individual patients were never discussed in these rounds.
Patients’ process of returning to work
The participants believed that there was a need for a clear structure for establishing long-term rehabilitation plans for younger patients who could possibly return to work. They recognized the patients’ situations as being complex and believed that rehabilitation plans tended to be overlooked and forgotten about, particularly for patients of working age.
The ability of patients to return to work
The participants believed that many patients wanted to return to work but that different patients had different abilities to do so. ‘I think many patients want to return to work’ (Interview 2, Physician). Because of restrictions brought on by heart failure, they believed that most patients could not return to work or that it would often take a long time before they could return to work. Also perceived as a limitation were the patients’ own fears regarding any consequences of returning to work. Thus, in relation to patients’ return to work process, the participants considered sick leave as a part of the whole process.
Establishing rehabilitation plans
To establish rehabilitation plans for patients, the participants believed that well-functioning cooperation between different actors, such as the healthcare organization, social insurance, counselors, employers and/or employment services, was needed. They perceived that the dialogue between different actors was generally sufficient. Social insurance administrators in particular were perceived as being informative. None of the participants perceived physiotherapists or nurses to be part of this cooperation. The physician, though, described it as being desirable that nurses in particular should be more involved because they were more knowledgeable than physicians about patients. I often think it would be good for patients with heart failure if nurses participated because they have important supplementary information medically and maybe a little better knowledge about the patients’ social dimensions than I have as a physician (…) I think we complement each other. (Interview 2, Physician)
Barriers for implementing rehabilitation plans
The participants described heart failure as a complicated condition with an unpredictable course, which meant that it could be difficult to assemble and follow specific rehabilitation plans. In some cases, rehabilitation plans were completely dismissed. As a consequence, the plans tended to be individualized yet randomly developed; that is, the rehabilitation plans depended on whom patients met or had contact with. The participants also believed that healthcare professionals were responsible for building networks around patients but that such a commitment was too resource intensive. They perceived that there were difficulties in obtaining an overview of available community resources and felt that accessibility to heart failure services was insufficient. If it was difficult to contact people, if actors failed to talk to each other, or if motivation, the structure of planning and/or clear goals were deficient or inexplicit, then cooperation could fail. In addition, meetings could be forgotten or cancelled because of a lack of time, which implied that the vulnerability of patients would be further increased. Additionally, the collaboration between primary care and cardiac clinics needed to be further developed.
Discussion
The findings of this study reveal important aspects of healthcare professionals’ perceptions of their work with patients of working age with heart failure. The participants understood the vulnerability of patients and were aware of the suffering that patients were experiencing. They recognized that younger patients could have a different life situation than older patients. In a sense, they even perceived patients of working age as being more vulnerable than older patients. It is well known that younger patients with heart failure frequently rate their quality of life as being worse and suffer more from a low mood and/or depression than older patients.13–16 This is assumed to be caused by a loss of social networks or by not being able to work. 17 The participants also emphasized that patients required individualized support and needed to feel secure. When patients perceive healthcare professionals as being available or supportive, they gain a sense of security.7,9,18 The participants recognized heart failure services as important and supportive to patients. In Sweden, as in other countries, there are well-developed routines and programs for patients with heart failure. 1 The programs usually aim to support patients with handling issues such as self-care, medications and/or physical activity after they are discharged from hospital. Common interventions include educational and/or counseling sessions and/or telephone follow-up, as well as a variety of cognitive–behavioral approaches to modify or alleviate patient-related factors. 19 There is a risk, though, that well-defined programs stimulate standardization or objectification, which implies that patients’ unique life situations are at risk of being overlooked by healthcare professionals. Healthcare professionals can feel restricted and have a need to balance between patients’ health statuses, laws, regulations, time and financial resources. 20 Moreover, nurses might aim to improve patient outcomes through patients’ medical compliance. 21 In the present study, though, the participants were aware that the individuals’ needs should take precedence over the diagnosis. Still, they repeatedly referred to routines or regulations or focused on medical treatment or standardized information, which meant that the individual needs were concealed behind the medical condition, that is, behind the diagnosis.
The participants perceived that there was a lack of structural and organizational resources that caused difficulties in handling younger patients’ needs. Yet, they expressed a sincere wish to support patients, but their intentions were constrained by not having sufficient tools or by existing rules and routines. Additionally, Hancock et al. [22] reported that heart failure nurses and cardiologists highlight the importance of rehabilitation but become frustrated over the limitations on the service provision in this area for patients with heart failure. To personalize clinical protocols, healthcare professionals can emphasize available support to patients. 21 In this study, the participants looked for strategies and solutions that were ‘outside of the box’ (Interview 3, Physiotherapist), which implies that they sometimes set the routines aside. For example, because working-age patients’ needs for physical exercise were not equal to older patients’ needs, the younger patients were provided with individually adjusted exercise programs.
Another important finding was that the participants encountered patients from their specific professional point of view but were unable to comprehend the complete rehabilitation process of patients. Accordingly, even though they were aware of their own role, they had little or no insight into the roles of other professionals. Johannessen and Steihaug define uniprofessional collaboration as ‘different professionals working side by side without integrating their activities’.23(p.365) Additionally, they define interprofessional collaboration as ‘two or more members of different healthcare professions working together to solve problems or to provide services’.23(p.365) Accordingly, the participants in the present study worked uniprofessionally rather than interprofessionally. The collaboration concerning only medical aspects was more or less non-existent. At the same time, all of the participants, irrespective of their occupation, explained that they wanted to collaborate more often. Fragmented services and unintentionally co-created structures and systems can create barriers to care for patients. 24 Factors that can affect collaboration include hierarchal systems, professionals’ views about caring, context and organization of care, professional culture, interpersonal knowledge, awareness of one’s own professional identity, and information and knowledge transfer. 20 In turn, interprofessional collaboration is assumed to build on communication and good relations. 20 However, even though the participants claimed that collaboration worked, discussions between professionals were dominated by patients’ medical treatment, whereas patients’ life situations were rarely addressed. This indicates that more efforts are needed to transform the existing uniprofessional collaboration into interprofessional collaboration and teamwork.
The present findings also revealed issues related to patients’ return to work processes. The participants perceived that many patients wanted to return to work but that there were obstacles, and the possibility for returning to work varied between individuals. One obvious obstacle was the condition of heart failure itself, and another obstacle was the work itself. Patients can have heavy and demanding work tasks or there can be a lack of flexibility regarding work tasks or work hours. 25 In another study on healthcare professionals’ experiences of patients’ sick leave processes, insufficient interprofessional collaboration was observed to affect both content and consequences relating to challenges in patients’ sick leave processes. 26 Work is important for people’s perception of their quality of life. Work entails financial security, independence and access to social networks. 25 Thus, work can be considered a central component for people’s identity and self-image. However, the participants in the present study did not clearly acknowledge this, which means that it is reasonable to assume that they had not reflected on what it meant to lose their networks or jobs. Like many other types of patients, patients with heart failure also want to stay active in work, if possible. 25 The participants believed that long-term rehabilitation plans were required if patients were to return to work, but they perceived that rehabilitation plans tended to be overlooked or forgotten. Healthcare professionals may abandon patients with heart failure during rehabilitation, and in this case, the healthcare professionals hand responsibility over to the patients themselves. 9 However, people with a chronic progressive condition such as heart failure are fully occupied by handling their health status and their daily life. To make plans for rehabilitation and the forthcoming working life under those circumstances is a heavy burden that they cannot handle without sufficient support from healthcare professionals or other stakeholders. In order for healthcare professionals to support patients as they return work, they need to show patients that they believe in their ability to return.
Strengths and limitations
Qualitative interviews have both advantages and disadvantages. One advantage is that the participants get an opportunity to put their experiences into words, which ensures that the researchers are provided with nuanced and rich descriptions of the phenomenon under study. In the present study, focus-group interviews seemed to be an appropriate method for data collection. Focus-group interviews are useful when researchers aim to explore how people think and why they think the way they do. 27 One strength of focus-group interviews is that they include group dynamics, which can help participants explore and clarify perceptions regarding the phenomenon under discussion. 27 To establish credibility, we wanted to ensure that the participants had a variety of experiences and different professions. It was problematic, though, to find participants who could set aside the time required to participate in the focus groups. As a consequence, at one of the clinics, only a cardiologist could participate. Subsequently, instead of the three intended focus-group interviews, we conducted two focus-group interviews and one individual interview, which can be considered a weakness. In addition, only one physiotherapist participated. Thus, the sample consisted mostly of nurses, which is considered another limitation. An equal distribution between different professional categories would have been advantageous thus enriching the results as well as the discussion of interdisciplinary work.
Qualitative content analysis has both strengths and limitations. One strength is that the method is highly flexible. In the present study this was highly advantageous since it included both focus-group interviews and an individual interview. One limitation, though, of qualitative content analysis is that texts can be interpreted in different ways by different people and that coding data always involves some interpretation, even when data are on a manifest level. Another limitation is that the identified meaning units should reflect the phenomenon and not the researchers’ pre-understanding; something which can be difficult to achieve. In the present study, two of the authors conducted both of the focus-group interviews. This can be considered a strength because two different individuals listened to the participants and posed subsequent questions to them. To ensure dependability, the first author was involved in all three of the interviews. In that way, all of the participants discussed the same areas. In addition, reflective dialogue was used, that is, all of the authors jointly reflected on, discussed, and revised the evolving categories until agreements were reached on the descriptions. To confirm the findings, the results are presented with quotations from the interviews. A disadvantage is that the results of qualitative research cannot be generalized (albeit not a major goal). In the present study, this means no firm conclusions can be made about interdisciplinary work nor about healthcare professionals’ perceptions of working with people with heart failure of working age. Thus, to achieve generalizable knowledge the present results ought to be tested and validated in, for example, a national survey of healthcare professionals’ work with this patient group.
Another limitation of this study is that its findings can be considered outdated since the data were collected in 2012. However, according to our experience within the field and also in accordance with, for example, Hancock et al., 22 the management of people with heart failure has changed only a little in the past 10 years. Therefore, under these circumstances, this is not considered a major limitation to this study.
Conclusions
The present findings show that healthcare professionals who are involved in the care of patients of working age with heart failure strive to combine protocol-driven care with an approach that recognizes the individuality of each patient. The findings also indicate that there is a risk that team members end up working side by side instead of working together to solve the problems of each patient. Uniprofessional work, rather than interprofessional work, means that support and rehabilitation plans for patients with heart failure are at risk of being dismissed or overlooked. The current study’s focus was on patients of working age with heart failure, but the findings can be used for discussion and reflection by nurses and other professionals who are concerned with the rehabilitation of patients with other serious chronic conditions. Evaluations of how interprofessional collaboration can be improved in relation to patients of working age with heart failure are needed in future experimental studies.
Footnotes
Funding
This study was funded by grants to Lena Nordgren from the Swedish Social Insurance Agency (grant number 25728/2010).
Conflict of interest
The authors declare that there is no conflict of interest.
