Abstract
Background:
The aim was to examine the predictability of stage of disease (FEV1) and measures of strength (arm and leg) to arm and leg ergometry capacity of patients with chronic respiratory diseases.
Methods:
A total of 44 chronic respiratory disease patients, 16 males and 28 females (mean age = 59.8 ± 11.9 years), with an FEV1 of 22%–89% predicted (mean FEV1% predicted = 54.6 ± 18.3) participated. All participants completed spirometry, Medical Research Council grade, anthropometric assessment, submaximal arm and leg ergometry testing, grip strength, and isokinetic quadriceps and hamstrings strength and endurance testing.
Results:
To determine contributing and predictor variables of arm and leg ergometry capacity, multiple linear and binary regression analyses were performed. Multiple regression analysis demonstrated that quadriceps strength (N m), FEV1% and grip strength (kg) predicted 64% of peak wattage during submaximal leg ergometry testing (adjusted R2 = 64%, F = 26.387 and p = 0.00). Quadriceps strength showed the highest predictability of peak leg ergometry wattage (p = 0.00, β = 0.844 and t = 6.238), followed by grip strength and FEV1% (p = 0.038, β = −0.270 and t = −2.143 and p = 0.028, β = −0.230 and t = 2.279, respectively). A second regression analysis determined that quadriceps strength (N m), FEV1% and grip strength (kg) predicted 53% of peak wattage during submaximal arm ergometry testing (adjusted R2 = 0.53, F = 17.018 and p = 0.00). Quadriceps strength was the only independent variable that showed predictability of peak arm ergometry wattage (p = 0.00, β = 0.793 and t = 5.125). The odds ratio analysis indicated that chronic respiratory disease patients with high quadriceps strength have 13.76 times higher odds of having high peak arm ergometry wattage. This odds ratio equated to an 85% probability of having high arm ergometry peak wattage if quadriceps strength is high.
Conclusions:
In summary, the main factors predicting leg ergometry capacity were quadriceps strength, FEV1 and grip strength. Quadriceps strength was the only statistically significant predictor of peak arm ergometry wattage, suggesting a relationship between arm and leg functionality in chronic obstructive pulmonary disease patients.
Introduction
Chronic respiratory disease (CRD) is a common medical term used to describe chronic conditions of the lungs and airways that cause progressive airflow limitation which is not fully reversible. 1 CRD most commonly includes chronic bronchitis, emphysema, chronic obstructive pulmonary disease (COPD), bronchiectasis, asthma, interstitial lung disease, pulmonary hypertension and obstructive sleep apnoea syndrome. In New Zealand, CRD is a significant cause of morbidity and mortality, which places a major burden on the healthcare system of New Zealand. 2
As CRD severity progresses, exercise capacity becomes limited, which is largely due to increasing symptoms and systemic complications. 3 Exercise-based rehabilitation is an important component in the management of CRD, with the focus to improve physical function largely via an increase in exercise tolerance. 4 The decreased ability to exercise limits the physical rehabilitation of patients with CRD, as symptom limitations such as dyspnoea and leg fatigue prevent patients from exercising at an intensity or duration that provides sufficient overload to elicit physiological adaptations. 1
Exercise limitations of CRD patients are largely determined by lower limb dysfunction, specifically fatigability, muscle atrophy and structural muscle fibre changes, which impacts lower body strength.2,3 Quadriceps strength in particular can impact dramatically on quality of life and physical independence 5 and has been found to be a significant predictor of healthcare utilisation in COPD patients. 6 Lower limb muscle strength contributes significantly to the intensity of leg effort and dyspnoea at a given power output of cardiorespiratory patients, and individuals with reduced leg strength are associated with having a reduced peak exercise capacity. 7 Hamilton et al. 7 found that improving leg strength improves exercise limiting symptoms of respiratory disease patients, quantifying that a doubling of strength is associated with a decrease in leg effort by 25% and dyspnoea by 30%.
The frequency of muscle recruitment and activation in CRD patients largely determines the degree of dysfunction in a given muscle. In this regard, researchers have demonstrated that upper body exercise capacity might be better preserved as CRD severity progresses. Higher skeletal muscle dysfunction in CRD, when compared to healthy individuals, has been reported for the lower limbs compared to the upper limbs in terms of exercise tolerance and strength.8,9 More insight into whether CRD patients demonstrate better exercise training potential with arm ergometry as compared to leg ergometry is needed. The aim was to examine the contributions of stage of disease (FEV1) and measures of strength (arm and leg) to arm and leg ergometry capacity of patients with CRD.
Method
Study design and participants
A cross-sectional research design was used to investigate the within-group relationships of respiratory, strength and physiological measures of patients with mild to very severe airflow obstruction. All participants completed three 1-h assessments, with 24 h minimum between. Appointment 1 consisted of informed consent, health screening, respiratory function testing and the Medical Research Council (MRC) dyspnoea scale. Appointment 2 included anthropometric assessment, submaximal leg ergometry testing and grip strength testing. Appointment 3 included submaximal arm ergometry testing and isokinetic quadriceps/hamstrings strength and endurance testing. The study protocol had prior approval of research ethics from the central lower North Island ethic committee of New Zealand.
A total of 44 patients referred by the Palmerston North Hospital respiratory clinic to the U-kinetics exercise and wellness clinic for 12 weeks of exercise-based rehabilitation participated. Written informed consent was obtained from all participants of the study. The participants had not been involved in structured exercise training for at least 1 year prior to participation in the study.
All the participants had been diagnosed with a chronic respiratory condition (or a combination) by a general practitioner or respiratory physician including chronic bronchitis, emphysema, COPD, bronchiectasis, asthma and obstructive sleep apnoea syndrome.
For the purpose of this study, disease severity categories were merged to form two groups, due to the low number of respondents in the mild (n = 4) and very severe categories (n = 5). Participants with mild-to-moderate airflow obstruction (Global Initiative for Chronic Obstructive Lung Disease (GOLD) 1–2) were combined to form the ‘Mild-Mod’ group (n = 28), and severe and very severe airflow obstruction (GOLD 3–4) were combined to form the ‘Severe’ group (n = 16). The Mild-Mod group included 10 males (35.7%) and 18 females (64.3%), and the Severe group included 6 males (37.5%) and 10 females (62.5%).
Data collection
Anthropometric measures
Stature was assessed with shoes removed with a wall mounted stadiometer (model 222; Seca, Hamburg, Germany). Body mass was measured on a calibrated electronic scale (Tanita, Cloverdale, WA) with the shoes and as much clothing removed as possible. Body mass index (BMI) was calculated by dividing body mass (kg) by stature (m) squared.
Ergometry testing
All participants completed a modified version of the YMCA submaximal leg ergometer test 10 for estimation of VO2max. Testing was performed on a leg ergometer (ec3000e; Custo-med, Frankfurt, Germany). The test comprised an unloaded 1-min warm-up, followed by three 4-min stages. Participants started on 20–30 W for the first stage and then power output was gradually increased with each stage depending on rating of perceived exertion (RPE), pain and dyspnoea scores, and heart rate and blood pressure responses. Power output was increased at the end of the fourth minute of each stage if the third and fourth minute heart rates were within a steady state (±6 bpm) and no symptom limitations were present. The aim was to reach either 70% of the age-adjusted maximum heart rate using Karvonen’s formula [(220 − age − resting heart rate) × 0.7 + resting heart rate] or any symptom limitation according to the American College of Sports Medicine (ACSM) absolute and relative contra-indications for terminating exercise testing. 10
Electrocardiography (ECG) was used to monitor heart waveform and rhythm during exercise testing using the Mason and Likar 11 modified electrode placement provided by McArdle et al. 12 Arm electrodes were positioned medial to the anterior deltoid 1–2 cm below the right and left clavicles, and foot electrodes were positioned over the lower ribs.
The following equation was used to calculate: VO2max [VO2 = ((10.8 × work rate in watts)/body mass) + 7]. 10
All participants performed an incremental multi-stage submaximal arm ergometry test. 10 Testing was performed on a Technogym Arm Ergometer (Top Excite 700; Tech-nogym, Casena, Italy). Participants sat upright with both feet on the ground and at a distance that their arms were slightly flexed while undertaking the arm ergometry test. Participants performed a 1-min warm-up of unloaded arm cycling, before completing three stages of 3 min. Participants started on 20–30 W for the first stage, and then power output was gradually increased with each stage depending on RPE, pain and dyspnoea scores, and heart rate and blood pressure responses and if the third and fourth minute heart rates were within a steady state (±6 bpm) and no symptom limitations were present. The aim was to reach 70% of age-adjusted maximal heart rates (using Karvonen’s formula as above), an RPE score of higher than 14 or a wattage equal to or greater than 42% as obtained during the last stage on the leg ergometry assessment, according to Carter et al. 13 If peak wattage beyond 42% of leg ergometry wattage were required for subjects to reach the same maximum heart rates as obtained during leg ergometry, the test continued beyond three stages until they reached the required heart rate or the clients requested to stop. Test termination points included the presence of symptom limitation based on ACSM’s 10 guidelines for early termination.
The following equation was used to calculate: VO2max [VO2 = ((18 × work rate in watts)/body mass) + 3.5]. 14
Dyspnoea and RPE
Dyspnoea and RPE were measured at the end of each stage during arm and leg ergometry testing using the Borg dyspnoea scale and the Borg RPE scale. 15
Disease severity
Spirometry was performed in order to verify the degree of airway obstruction, with consideration to the ratio FEV1/forced vital capacity (FVC), so that participants could be classified into mild (FEV1 ⩾ 80% predicted), moderate (predicted 50% ⩽ FEV1 < 80%), severe (predicted 30% ⩽ FEV1 < 50%) and very severe (predicted FEV1 < 30%) obstruction categories. 16 Spirometry was performed using a hand-held spirometer (EasyOne; ndd Medizintechnik AG, Zurich, Switzerland), which was calibrated prior to each test with a 3-L syringe. Participants performed the FEV1 and FVC manoeuvre according to the American Thoracic Society guidelines. 17 The participants sat in an upright position with both feet on the floor wearing a nose peg when performing the test and were instructed to breathe in as deeply as they could, seal their lips around the mouthpiece, and blow out as hard, fast and as long as possible. Subjects performed three attempts, and the best attempt was recorded.
All subjects completed the MRC scale 18 for the purpose of determining the severity of dyspnoea and stage of disease.
Peripheral muscle strength testing
Upper limb strength was measured by grip strength using a Baseline Hydraulic Hand Dynamometer (Irvington, New York, USA). Two attempts were performed on each side for familiarisation, and the highest reading was recorded. The grip strength test started with the arm in shoulder abduction of 90°, with the elbow in full extension (0° of flexion). The subject was instructed to grip the hand dynamometer as hard as possible and lower the arm down to the side of the body squeezing the tool with a maximum effort. The dynamometer was reset to 0 prior to each reading.
Lower limb strength and endurance were measured by knee flexion and extension using an Isokinetic muscle dynamometer (HUMAC norm, model 502140; Computer Sports Medicine, Inc., Stoughton, MA, USA). The dynamometer was calibrated according to standard settings outlined by the user manual with the axis of rotation in line with subject’s femoral epicondyles. The dynamometer was corrected for gravity. Range of motion (ROM) was set to at least 90°. Subjects completed one trial set of five repetitions at 60 and 180°s−1 for familiarisation and then one set of five repetitions at 60°s−1 and one set of 15 repetitions as fast as possible at 180°s−1. Each set was separated by a 60-s rest interval, which has been found to be an adequate rest period during isokinetic testing to avoid fatigue. 19 Subjects were instructed to flex and extend their knee as hard and as fast as they could for the full duration of the test. This quadriceps/hamstring strength and endurance testing protocol has been used on healthy, inactive, elderly individuals. 20
Statistical analysis
Statistical analyses were performed using STATISTICA (Version 7.0) and SPSS (Version 22). Descriptive statistics are presented as mean ± standard deviation. The data set presented with normal distribution. Between-group differences regarding anthropometric, aerobic capacity and strength values were analysed using an unpaired t-tests for the two disease severity groups. Two multiple linear regressions were conducted to determine whether peak arm and leg ergometry wattage could be predicted with quadriceps strength, grip strength and FEV1. A check for multicollinearity was completed and variables with r <0.30 and >0.90 were excluded. A binary logistic regression analysis was used to examine the predictability of upper body function (arm ergometry) by quadriceps strength.
For the multiple linear and binary logistical regressions, participants were grouped for each of the variables used into relative ‘high’ and ‘low’ categories. Peak arm and leg ergometry wattage, quadriceps strength and grip strength were split at the 60th percentile, while FEV1% was split at the 50th percentile of the group distribution. Grouping at the 60th percentile is recommended for binary and regression analyses because the aim is to distinguish predictability of either poor or good performers. 21
Results
Participants’ descriptive characteristics
The descriptive and disease severity characteristics of the participants are displayed in Table 1. The study participants included 44 CRD patients, 16 males and 28 females, with a mean age of 59.8 ± 11.9 years. The mean FEV1% predicted was 54.6 ± 18.3, indicating GOLD stage 2 (moderate CRD). Participants’ FEV1% predicted ranged from 89%–22% (mild to very severe airflow obstruction).
Participants’ descriptive and disease severity characteristics.
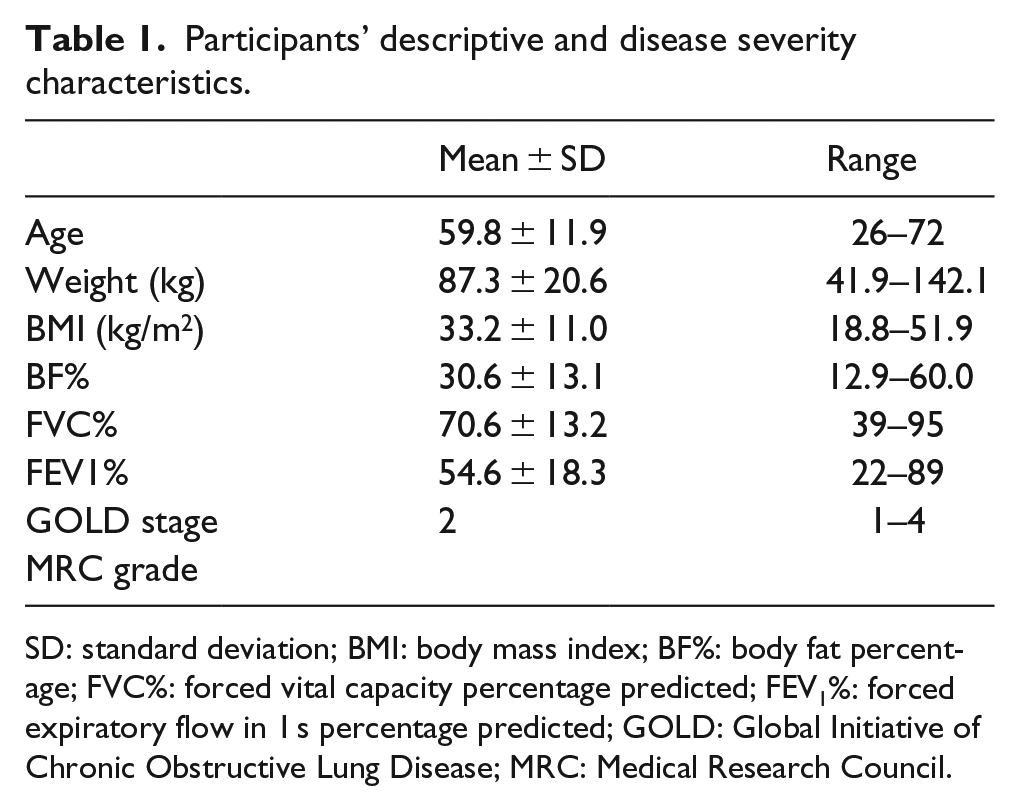
SD: standard deviation; BMI: body mass index; BF%: body fat percentage; FVC%: forced vital capacity percentage predicted; FEV1%: forced expiratory flow in 1 s percentage predicted; GOLD: Global Initiative of Chronic Obstructive Lung Disease; MRC: Medical Research Council.
Peripheral muscle strength
The total group mean for quadriceps strength, as measured by peak torque, was 103.67 ± 34.99 N m and 53.10 ± 19.47 N m for hamstring strength (Table 2). Statistically significant differences were found between the two GOLD groups for quadriceps strength and hamstrings strength (p < 0.05). No differences existed between GOLD groups for grip strength, quadriceps endurance or hamstrings endurance.
Mean arm and leg strength measures and the comparison of GOLD groups.
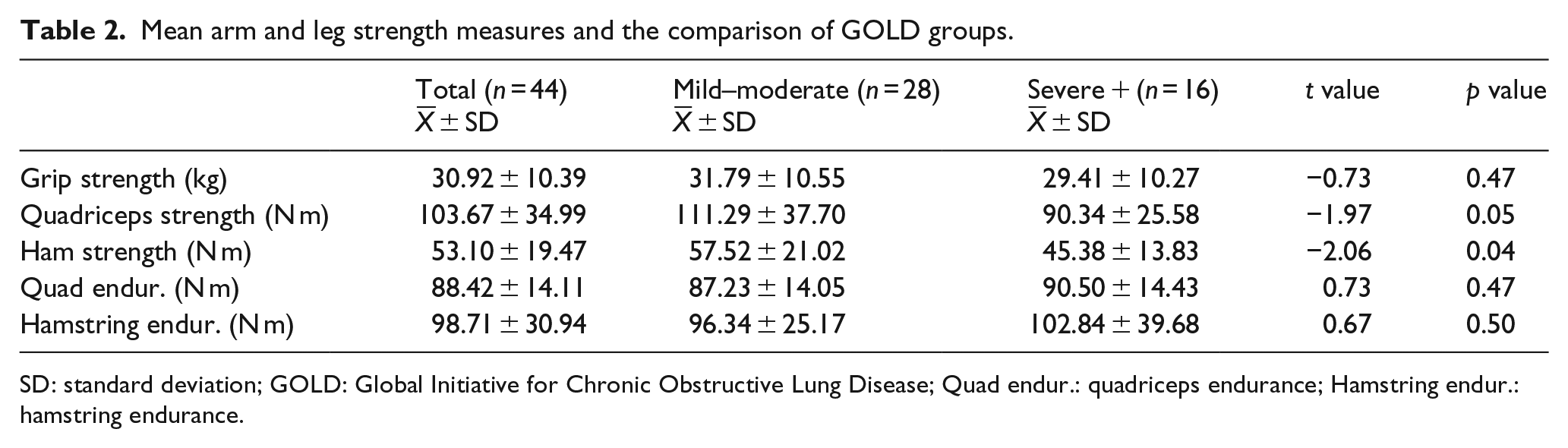
SD: standard deviation; GOLD: Global Initiative for Chronic Obstructive Lung Disease; Quad endur.: quadriceps endurance; Hamstring endur.: hamstring endurance.
Arm and leg ergometry
In Table 3, participants with mild–moderate CRD demonstrated significantly higher (28%) peak leg ergometry wattage compared to the severe CRD group (p = 0.03). The mild–moderate CRD group demonstrated a 16% higher peak arm ergometry wattage, which was close to meeting statistical significance (p = 0.08). In addition, the leg pain scores reported during the ergometry testing were 18% greater for those with mild–moderate disease compared to severe disease; however, the difference was not statistically significant (p < 0.08). Arm pain scores were 20% higher in the mild–moderate CRD group, compared to the severe group (p = 0.13).
Comparison of GOLD groups for arm and leg ergometry outcomes.
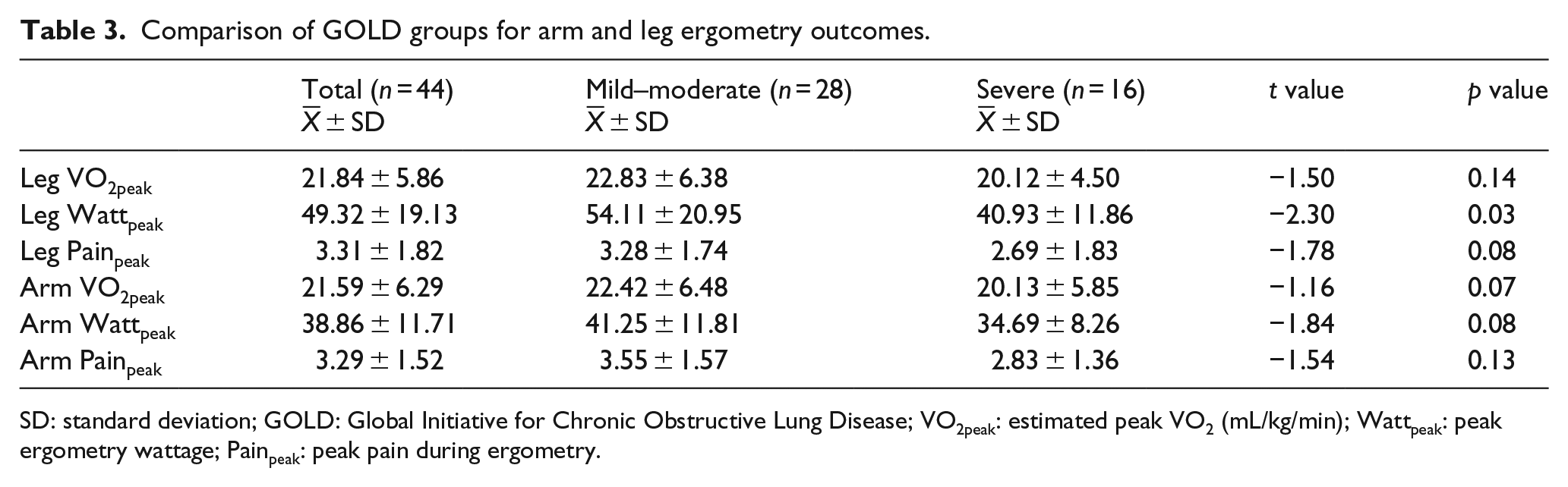
SD: standard deviation; GOLD: Global Initiative for Chronic Obstructive Lung Disease; VO2peak: estimated peak VO2 (mL/kg/min); Wattpeak: peak ergometry wattage; Painpeak: peak pain during ergometry.
Prediction of arm and leg ergometry wattage
A regression analysis (Table 4) was conducted to determine whether quadriceps strength (N m), grip strength (kg) and FEV1% were predictive of peak wattage during submaximal leg ergometry testing. The adjusted R2 indicated that 69% of the variability in peak leg ergometry wattage was explained by the independent variables. The F-statistic was 26.387 with a significance level of p = 0.00, indicating that we can reject the null hypothesis.
Regression analysis to determine whether peak wattage during submaximal leg ergometry testing could be predicted by quadriceps strength (N m), grip strength (kg) and FEV1%.
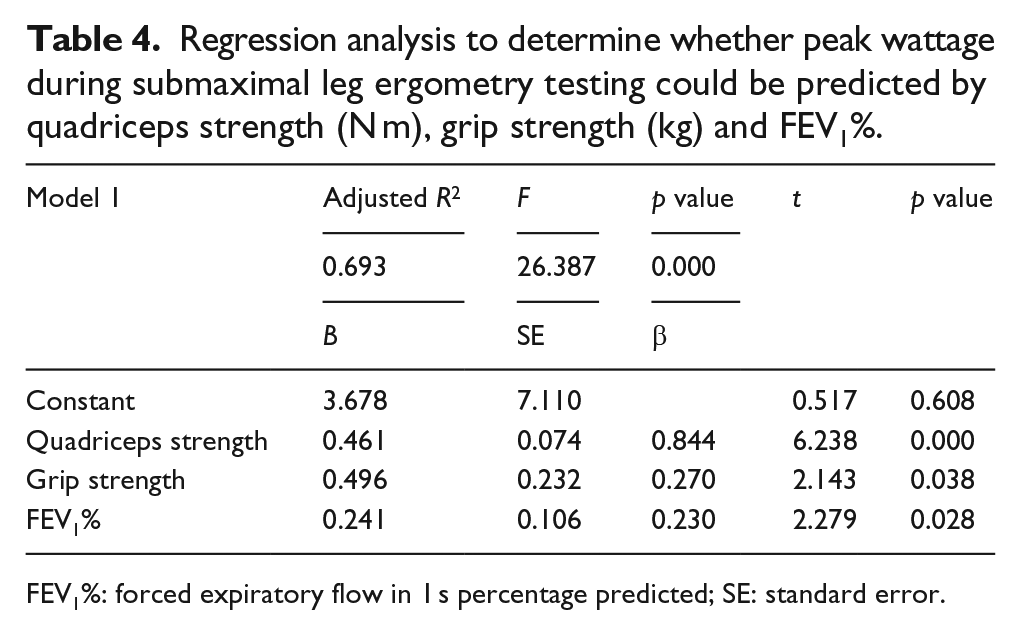
FEV1%: forced expiratory flow in 1 s percentage predicted; SE: standard error.
Quadriceps strength showed the highest predictability of peak leg ergometry wattage (p = 0.00, β = 0.844 and t = 6.238). The model predicts that for a 1 N m increase in quadriceps strength (peak torque), peak leg ergometry wattage would increase by 0.5 W, holding grip strength and FEV1% fixed. Furthermore, grip strength and FEV1% were significant predictors of peak leg ergometry wattage (p = 0.038, β = −0.270 and t = −2.143 and p = 0.028, β = −0.230 and t = 2.279, respectively). The model predicts that a 1-kg increase in grip strength would proliferate with a 0.5 W increase in peak leg ergometry wattage, and a 1% higher in FEV1 predicted value would increase peak leg ergometry wattage by 0.2 W.
A second regression analysis was conducted to determine whether quadriceps strength (N m), grip strength (kg) and FEV1% were predictive of peak wattage during submaximal arm ergometry testing (Table 5). The adjusted R2 indicates that 53% of the variability in peak leg ergometry wattage is explained by the independent variables. The F-statistic was 17.018 with a significance level of p = 0.00, indicating that we can reject the null hypothesis.
Regression analysis to determine whether peak wattage during submaximal arm ergometry testing could be predicted by quadriceps strength (N m), grip strength (kg) and FEV1%.
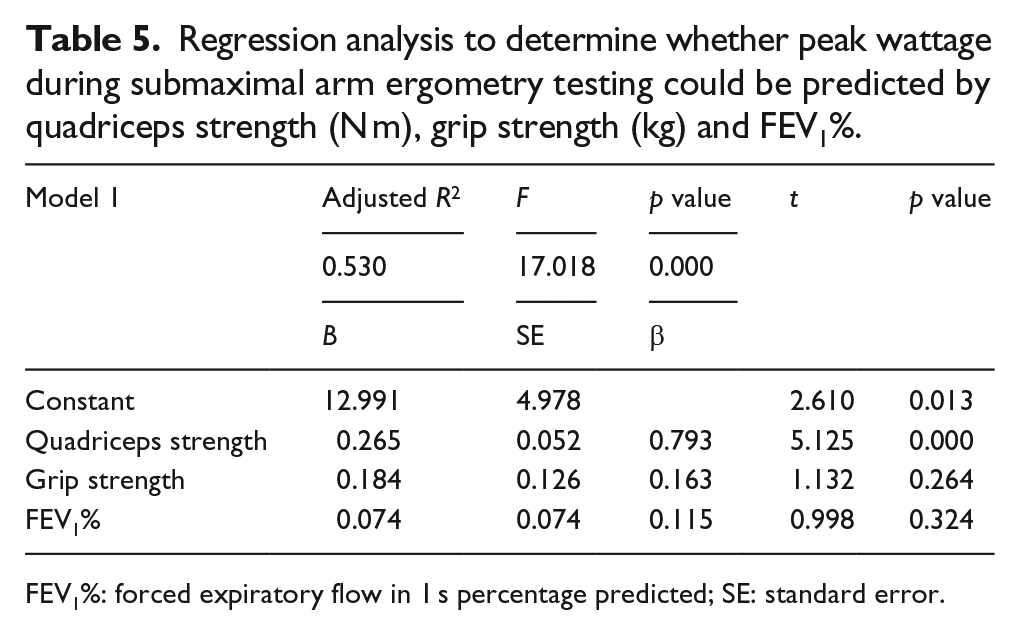
FEV1%: forced expiratory flow in 1 s percentage predicted; SE: standard error.
Quadriceps strength was the only independent variable that showed predictability of peak arm ergometry wattage (p = 0.00, β = 0.793 and t = 5.125). The model predicts that if you hold grip strength and FEV1% fixed, a 1 N m increase in quadriceps strength (peak torque) would equate into 0.3 W higher peak arm ergometry wattage.
Quadriceps strength was a statistically significant contributor to leg wattage and arm wattage in the two regression analyses (Tables 4 and 5). The results of the two standard regression analyses raised the question of how important leg strength is and whether it could be used as a predictor of arm ergometer capacity. Is arm wattage dependent on the maintenance of leg strength?
Prediction of arm ergometry wattage from quadriceps strength
A binary logistic regression analysis was therefore conducted to examine the predictability of peak arm ergometry wattage with quadriceps strength (Table 6, Model 1). A test of the full model against the constant only model was statistically significant, indicating that quadriceps strength distinguishes with statistical significance between low and high arm ergometry wattage (χ2 = 14.75, p = 0.001). The Nagelkerke R2 value indicates that quadriceps strength contributes 38.1% to the variance of peak arm ergometry wattage.
Binary logistic regression analysis to predict arm ergometry wattage with quadriceps strength while controlling for stage of respiratory disease, dyspnoea during physical activity and grip strength.
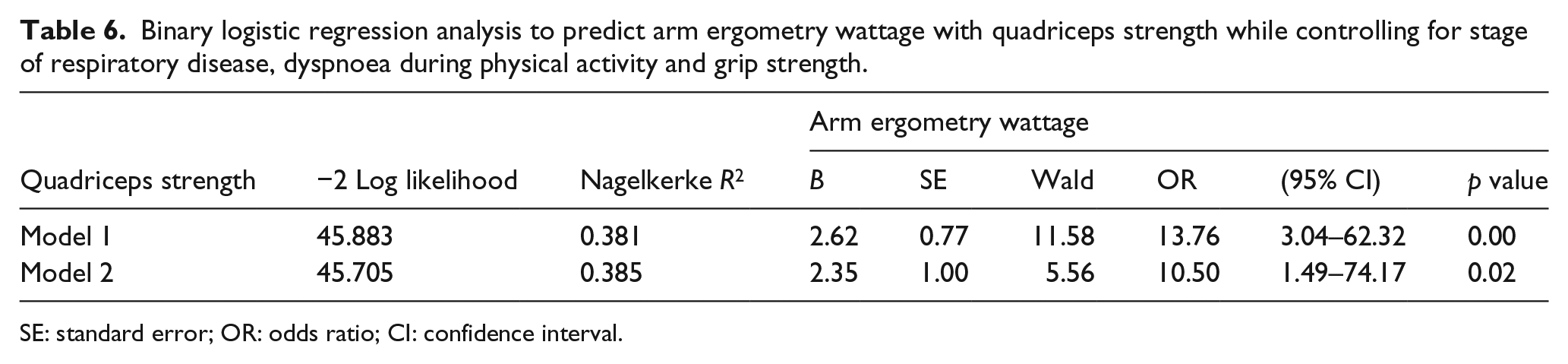
SE: standard error; OR: odds ratio; CI: confidence interval.
The odds ratio was 13.76, indicating that if CRD patients have high quadriceps strength, they have 13.76 times higher odds of having high peak arm ergometry wattage. This odds ratio equates to an 85.0% probability of having high arm ergometry peak wattage if quadriceps strength is high. The probability of having low peak arm ergometry wattage in the presence of high quadriceps strength is 29.2%.
In Model 2, FEV1% and grip strength were then added to the prediction model, which had a negative impact on the model’s ability to predict arm ergometry, as the odd ratio decreased from 13.76 to 10.49. The chi-square value was non-significant (p = 0.915) which indicated that adding FEV1% and grip strength does not improve the model’s ability to predict arm ergometry wattage during the third stage of the arm ergometry test.
Discussion
The regression analyses revealed that stage of disease, handgrip strength and leg strength contributed significantly (p < 0.05) to leg ergometry capacity (peak wattage), independent of body composition and gender. Grip strength did not contribute statistically significantly to arm ergometry capacity (peak wattage). The odds ratio of the binary logistic regression, to predict peak arm ergometry wattage with quadriceps strength, demonstrated that CRD patients were 13.8 times more likely to have high peak arm ergometry wattage if their quadriceps strength was high. The hypothesis that arm and leg strength measures would predict arm and leg ergometry capacity independently from body composition and gender can consequently be accepted. Leg strength measures had better predictability (with regard to both arm and leg ergometry capacity) than handgrip strength.
The standard regression analysis to predict peak leg ergometry wattage revealed that quadriceps strength, FEV1% predicted and grip strength explained 69% of the variability in peak leg ergometry wattage (Table 4). Quadriceps strength and FEV1 showed the highest predictability of peak leg ergometry wattage (p = 0.00, β = 0.844 and t = 6.238 and p = 0.028, β = −0.230 and t = 2.279, respectively). These findings support previous studies in which leg strength has emerged as a contributing factor to lower body exercise capacity and disease severity. 22 Peripheral muscle strength and FEV1% have an impact on lower limb aerobic capacity. Indeed, multivariate modelling has shown that 76% of the variance in 6-min walk distance (6MWD) could be explained by lung function, quadriceps strength and lean leg mass. 23 Furthermore, in this study, grip strength was the third significant predictor of peak leg ergometry wattage (Table 4; p = 0.038, β = −0.270 and t = −2.143), indicating that upper body strength and lower body exercise capacity are interrelated. In support, strong associations have been reported between handgrip strength and leg ergometry capacity in COPD, namely, VO2peak (r = 0.73), VO2max (r = 0.53) 22 and maximum wattage (r = 0.76). 24 In addition, grip strength has been associated with the 6MWT (r = 0.58), 25 and lat pulldown one-repetition maximum (1RM; as a measure of upper body strength) was found to be a predictive factor of 6MWD (R2 = 0.589). 26 Although Marino et al. 25 and Dourando et al. 26 used different aerobic capacity and/or strength measures compared to this study, their findings support that upper body strength and lower body exercise capacity are related in CRD patients.
The second standard regression analysis to predict peak arm ergometry wattage revealed that quadriceps strength, FEV1% predicted and grip strength explained 53% of the variability in peak arm ergometry wattage (Table 5). Quadriceps strength was the only significant predictor of peak arm ergometry wattage. No supporting evidence could be found in the literature on the relationship between leg strength and arm exercise capacity; however, previous studies have compared upper body strength with lower body strength and upper body aerobic capacity with lower body aerobic capacity in CRD. Recently, Miranda et al. 27 compared middle deltoid and quadriceps femoris strength and endurance of 21 CRD patients with a mean FEV1 of 46.1 ± 10.3% predicted. The researchers found deltoid and quadriceps to be similar with regard to absolute strength (similar differences when compared to healthy controls), but quadriceps had higher fatigability, indicating better upper body muscle (deltoid) fatigue resistance. Likewise, Franssen et al. 9 reported that quadriceps and biceps muscle functions are equally affected (reduced strength compared to healthy controls) in severe COPD.
The binary logistical regression analysis revealed that respondents with high quadriceps strength scores were 13.8 times more likely to have a higher wattage during submaximal arm ergometry testing. This equates to an 85.0% probability of having higher peak arm ergometry wattage if participants have stronger quadriceps. In support, stepwise regression analysis revealed leg strength to be the only significant contributor to performance during Physical Activity of Daily Living (PADL) (β = 0.547, t(22) = 2.92 and p = 0.008). 28 In this study, quadriceps strength contributed to arm and leg exercise capacity in patients with CRD. For the purpose of the binary regression, ‘high’ and ‘low’ peak wattage and quadriceps strength were split at the 60th percentile (114 N m). Clinically, this indicated that individuals with quadriceps strength testing scores below 114 N m have an 85% probability of not reaching 35 W during the third stage of arm ergometry testing.
This article contributed to current knowledge by conducting a binary regression analysis to provide odds ratios and probabilities to predict arm and leg exercise capacity. The findings complemented those of both Miranda et al. 27 and Franssen et al. 9 which indicated that there is an association between upper and lower body function in terms of strength in CRD patients. In addition to the association between upper and lower body strength in CRD, the findings of the regression analyses demonstrated that quadriceps strength is not only associated with upper body strength but also predicts upper body aerobic capacity. Leg strength measures had better predictability (with regard to both arm and leg ergometry capacity) than handgrip strength.
Based on the above findings of the regression analyses, the hypothesis that leg and arm strength measures would predict arm and leg ergometry capacity independently from body composition and gender can be accepted. The results of the standard and binary logistical regression procedures conducted in this study suggest that upper body functional decline might be highly related to lower body decline. Quadriceps strength was predictive of both leg and arm ergometry capacity. A potential explanation for this may be that commonly performed upper body activities of daily living also include leg involvement. Therefore, if there is a reduction in lower limb function, this could cross over to upper body activities that require leg involvement.
Limitations
While the findings of this article provide novel insights into the contributions of upper and lower body strength to upper and lower body exercise capacity, it is acknowledged that there are some limitations to this study that may impact the reliability of the results and their interpretations. These primarily include limitations to physiological measurements and the sample size/study population.
In this study, an indirect submaximal arm and leg ergometry method was used to estimate VO2max. Direct gas exchange measures were not used in this study due to inaccessibility and safety of the participants, but it is acknowledged that cardiopulmonary exercise testing would have improved the accuracy of peak oxygen uptake measurement. In defence, the extrapolation method used to predict VO2peak from the YMCA submaximal leg ergometer test has been shown to provide accurate predictions values. 29 However, Garatachea et al. 30 reported that predicted VO2max was overestimated in healthy adults by 5.4% for men and 11.8% for women for the YMCA protocol. Taking this overestimation into consideration and acknowledging the fact that the participants in this study were not healthy adults, peak intensity used in this study was based on symptom limits (i.e. the actual intensity where exercise needed to be terminated due to symptom limitation).
A convenience sample (n = 44) of CRD patients was used for the study, which was limited by the number of referrals to U-kinetics. It was not possible to control the number of participants or the number of participants in the various GOLD stages. Accordingly, participants with severe and very severe CRD were grouped together, as were participants with mild and moderate CRD. The limitation with this approach was that the impact of disease severity could not be tracked as effectively as was intended. It may be useful to complete a study with a larger sample size and enough participants in the separate GOLD stage groups to compare outcomes.
Diagnostic/classification guidelines for COPD are that airway obstruction is evident with a post-bronchodilator FEV1/FVC of <0.7, and disease severity can be classed from mild to very severe, which increases with a decrease in FEV1 16 This study included participants with COPD, chronic asthma, bronchiectasis and obstructive sleep apnoea. In all, 12 subjects (27%) had a reduced FEV1 but did not meet the <0.7 ratio criteria and were categorised as having restrictive lung disease. However, since there were no differences seen between any outcome measures when FVC and FEV1% predicted were compared, and the fact that all the study population showed some reduction in FEV1% predicted, the GOLD classification system based on FEV1% predicted was used to determine severity of disease.
Implications
The importance of leg strength in CRD is well known, and current exercise training guidelines include leg strength training as a part of rehabilitation of CRD patients. This article demonstrates that there is a high association of leg strength with both arm and leg aerobic capacity, emphasising the need for improving and maintaining leg strength. Attention needs to be given to gaining maximum improvements in leg strength during exercise training interventions.
In addition, the inclusion of leg strength testing before an exercise training intervention is justified in this study, to identify those who have reduced leg strength. A goal of amending this will be a key objective of the individual’s specific exercise programme. It also justifies the need to test leg strength after rehabilitation interventions to monitor the effectiveness of exercise programmes on improving leg strength.
Conclusion
In attempt to enhance the exercise training of CRD patients, it is important to identify specific exercise limitations in this population and how much impact each limitation has on the overall functioning of these individuals. Effective exercise rehabilitation programmes are important to maximise the physical improvements gained by individuals with CRD so that they can maintain an improved quality of life for longer. As a result, this will reduce the healthcare burden and the morbidity and mortality rates of patients with CRD.
It is well established that lower limb muscle function is an important predictor of exercise capacity and mortality in CRD. This study adds to the current literature by proposing that lower limb muscle strength is an important contributor to arm exercise capacity in addition to leg exercise capacity, as measured by arm and leg ergometry.
Leg strength and leg ergometry capacity were directly related to arm ergometry capacity in this study. These findings suggest that a reduction in leg function could lead to a reduction in arm function. Commonly performed activities of daily living often involve legs as well as arms. Therefore, if lower limb function is reduced and individuals with CRD begin to avoid activities involving the legs, it might impact negatively on arm activities.
The findings of this study highlight the importance of assessing upper and lower limb strength in patients with CRD. Additionally, it endorses the incorporation of specified lower limb strength training in respiratory exercise rehabilitation, especially for those with reduced strength and physical activity levels. Respiratory exercise rehabilitation programmes should incorporate both aerobic exercise and lower limb strength training components.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
