Abstract
Background:
The study aimed to assess the influence of the calcification of the ascending aorta on surgical mortality, postoperative stroke, and completeness of coronary revascularization in patients undergoing off-pump coronary artery bypass grafting with graft strategy tailored to its calcification severity.
Methods and results:
We examined the clinical records of 726 patients who underwent off-pump coronary artery bypass grafting. The age at operation was 71 ± 8 years. Calcification of the ascending aorta was graded as none–mild (less than spotty) in 668 (92.0%), moderate (<1/4 of circumference) in 26 (3.6%), and severe (>1/4) in 32 (4.4%) by preoperative non-contrast computed tomography. There were no significant differences in the number of distal anastomoses per patient among the three groups (3.3 ± 1.1, 2.9 ± 1.0, and 3.0 ± 0.9, respectively; p = 0.85). Graft strategy was tailored for each patient. Proximal anastomosis with partial clamp was used in 43.8%, 7.7%, and 3.1%, respectively (p < 0.001), while anastomotic devices were used in 6.8%, 30.1%, and 28.1%, respectively (p < 0.001). Other patients had aortic no-touch technique. There were four hospital deaths in the none–mild group (0.6%, p = 0.85). Stroke occurred in 1 (0.1%) patient, an aortic no-touch technique patient with none–mild calcification. Complete revascularization was not possible in 1 (0.1%) patient in the severe calcification group. Patency of saphenous vein graft of distal anastomosis was not different among groups.
Conclusion:
Influence of the calcification of the ascending aorta was minimized by tailoring graft strategy to calcification severity. It can practically abolish postoperative stroke while maintaining coronary revascularization success rates.
Keywords
Introduction
One of the major disadvantages of coronary artery bypass grafting (CABG) over percutaneous intervention is postoperative stroke. In contrast, the advantage of CABG for multi-vessels disease is completeness of revascularization, as reported by SYNTAX study. 1 Of critical importance for avoiding stroke while achieving complete revascularization is careful management of the ascending aorta for the following reasons. The ascending aorta is the site of cannulation for cardiopulmonary bypass as well as the proximal anastomosis site in aorto-coronary bypass, and these procedures make the ascending aorta a source of emboli.2–5 While there are many studies indicating that calcification of the ascending aorta leads to increased stroke incidence, there are few studies on the effect of calcification in off-pump CABG anastomotic device usage and aortic no-touch technique, on surgical outcomes, both positive and negative.2–8
Our standard procedure was off-pump CABG with graft strategy tailored to the condition of the ascending aorta. Specifically, proximal anastomosis with partial clamp, proximal anastomosis with anastomotic device, or aortic no-touch technique was carefully selected for each patient.
In this study, we retrospectively classified calcification severity of the ascending aorta by preoperative non-contrast computed tomography (CT) and assessed its influence on surgical mortality, postoperative stroke, and completeness of coronary revascularization in patients undergoing off-pump CABG with the tailored graft strategy.
Materials and methods
We retrospectively reviewed clinical records and images of preoperative CT scans of 730 consecutive patients who underwent CABG at Saitama International Medical Center between October 2007 and March 2013. Four patients (0.5%) who underwent on-pump CABG because of preoperative unstable hemodynamics were excluded and remaining 726 were included in this study. This study was approved by the institutional review board. Mean age at operation was 71 ± 8 years. We included 73 patients on chronic hemodialysis, and 67 aged >80 years. Patient characteristics are summarized in Table 1. Postoperative catheter or CT angiography was performed in 427 patients (58.8%).
Clinical characteristics of the study population and three groups of patients classified by degree of calcification of their ascending aorta.
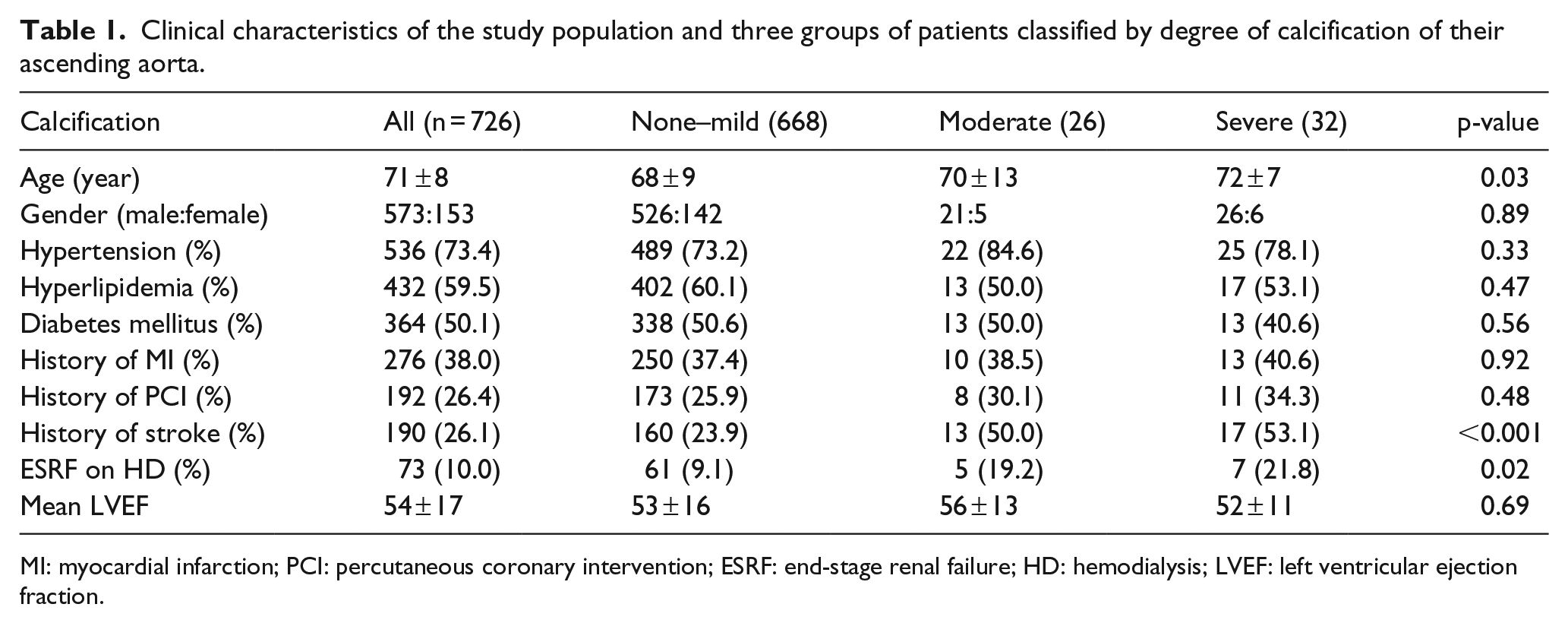
MI: myocardial infarction; PCI: percutaneous coronary intervention; ESRF: end-stage renal failure; HD: hemodialysis; LVEF: left ventricular ejection fraction.
Calcification of the ascending aorta was assessed by non-contrast CT near the level of the right pulmonary artery where proximal anastomoses are usually made. We retrospectively divided the patients into three groups based on maximum severity of calcification. They were None–mild calcification: no calcification or spotty calcification, Moderate: calcification less than 25% of the circumference of the aorta, and Severe: calcification of 25% or more of the circumference of the ascending aorta (Figure 1). We compared the three groups and assessed influence of the calcification severity of the ascending aorta on surgical mortality, postoperative stroke, and completeness of coronary revascularization in patients undergoing off-pump CABG with graft strategy tailored to calcification severity of the ascending aorta (next paragraph). Stroke was defined as any neurological deficit of acute onset confirmed by a neurologist and brain imaging that occurred postoperatively and that did not resolve within 24 h. Incomplete coronary revascularization was defined as when not all stenotic main-branch vessels were revascularized.
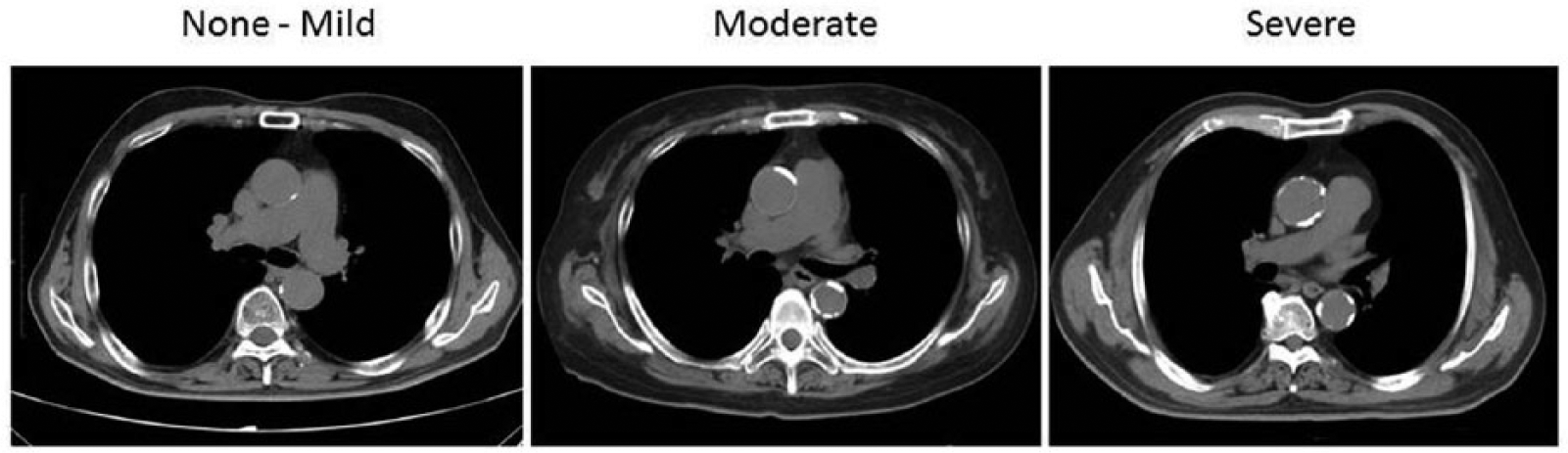
Representative computed tomography (CT) images at the level of the right pulmonary artery on preoperative CT from none–mild, moderate, and severe aortic calcification groups.
Surgical technique and graft strategy
Our standard procedure was complete revascularization with off-pump CABG technique. In general, the vessels used for the bypass procedure were selected based on study of age and affected coronary artery. For revascularization of the left anterior descending artery (LAD), the internal thoracic artery (ITA) was used regardless of age. For left-sided lesions other than the LAD, bilateral ITAs were used as the first line of choice in patients younger than 75 years old, and in patients older than 75 years, we tended to perform aorto-coronary bypass with saphenous vein graft (SVG). For the right coronary artery system, we used the right gastroepiploic artery (GEA) for patients younger than 75 years old, and in older patients, we tended to perform aorto-coronary bypass with SVG. Graft strategy was then tailored according to aortic calcification severity for each patient. When the ascending aorta had no or mild calcification, a partial clamp was considered first. If the calcium-free area did not appear to be large enough for partial clamping, anastomotic devices such as Heartstring (Guidant, Indianapolis, IN, USA), Enclose II (Novare Surgical Systems, Cupertino, CA, USA), or Passport (Cardia Inc., Redwood City, CA, USA) were chosen. When there was no calcium-free area or the risk of embolism related to aortic manipulation was predicted to be high, an aortic no-touch technique was chosen, regardless of patient age. During all CABG procedures, intraoperative transesophageal echo (TEE) was performed periodically to detect protruding or mobile plaque. If there was protruding or mobile plaque in the ascending aorta, all manipulation of the ascending aorta was avoided. During this period, epiaortic echo (epiaortic ultrasound (EAU)) was not systematically performed. Although this was our basic strategy, the principal surgeon made the final decision on which of the grafts to perform after considering preoperative risk.
Statistical analysis
Continuous variables are reported as mean ± standard deviation. Continuous variables were compared between the groups using the Kruskal–Wallis test. Categorical variables were compared between groups with chi-square test. Statistical significance was accepted at p < 0.05 and performed with SPSS statistical software (SPSS version 11.0, SPSS Japan, Tokyo, Japan).
Results
Prevalence and severity of calcification of the aorta and graft strategy
A total of 668 (92.0%) patients had none–mild calcification, 26 patients (3.6%) had moderate calcification, and 32 (4.4%) patients had severe calcification. Between these three groups, there was a significant difference in age, history of stroke, and prevalence of end stage renal dysfunction (patients on hemodialysis) (Table 1).
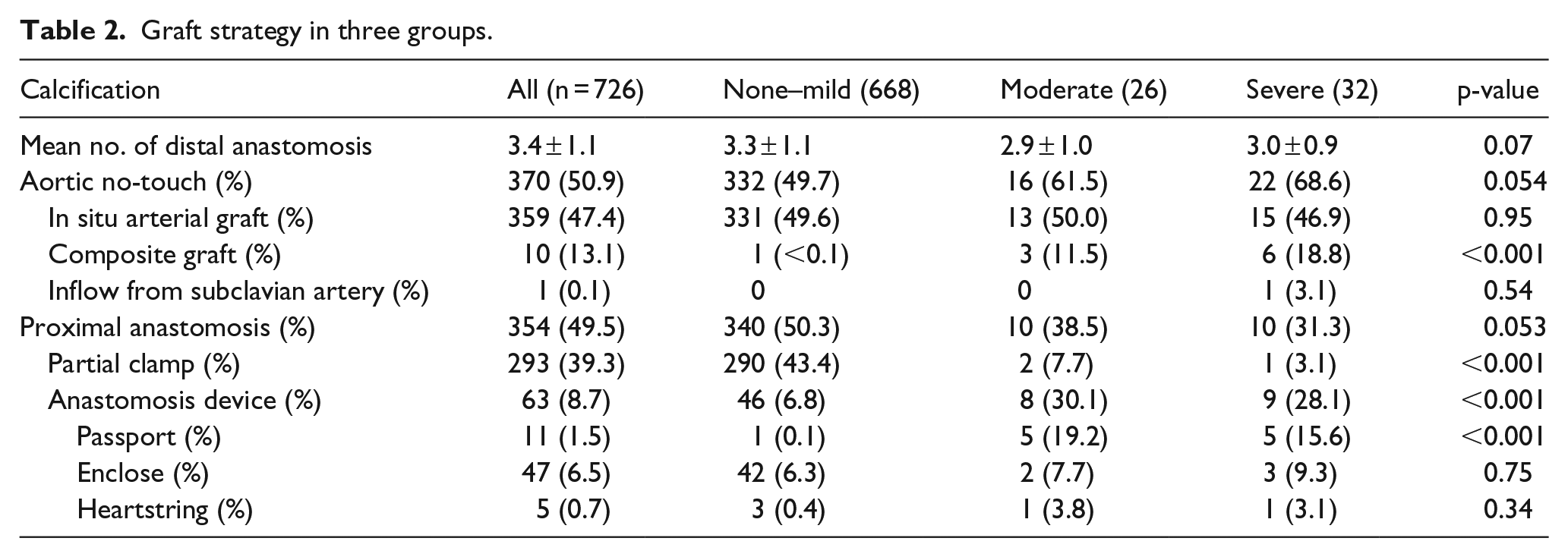
Graft strategy of CABG is summarized in Table 2. There were no significant differences in the number of distal anastomoses per patient between the three groups (none–mild: 3.3 ± 1.1, moderate: 2.9 ± 1.0, severe group: 3.0 ± 0.9, p = 0.85). Use of aortic no-touch technique in the severe group was performed for 22/32 (69%) patients, a rate higher than in other groups, but the difference did not reach statistical significance. For proximal anastomoses, partial clamps were used in 290/668 (43%) as opposed to anastomosis devices in 46/668 (7%) in the none–mild group, while anastomosis devices were used more in moderate 8/26 (30%) and severe 9/32 (28%) groups as opposed to partial clamp in 2 (8%) and 1 (3%) patient, respectively (p < 0.001). In particular, Passport was used more frequently in the moderate and severe groups (p < 0.001).
Graft strategy in three groups.
Severity of calcification and surgical outcomes
There were four hospital deaths in the none–mild group (0.6%, p = 0.85). Causes of death included two respiratory failures, one sepsis, and one low cardiac output. Only one patient of the none–mild group who underwent aortic no-touch technique had stroke during the follow-up period (0.1%, p = 0.98). It was associated with atrial fibrillation and occurred on postoperative day 5. One patient belonging to the severe group ended with incomplete revascularization (3.1%, p = 0.54), because there was no appropriate site for proximal anastomosis in his porcelain ascending aorta. In his case, the aortic no-touch technique was not feasible for his coronary pathology either. There was no statistical difference among the groups in incidence of death, postoperative stroke, incomplete revascularization, and other postoperative outcomes (Table 3).
Surgical outcomes.
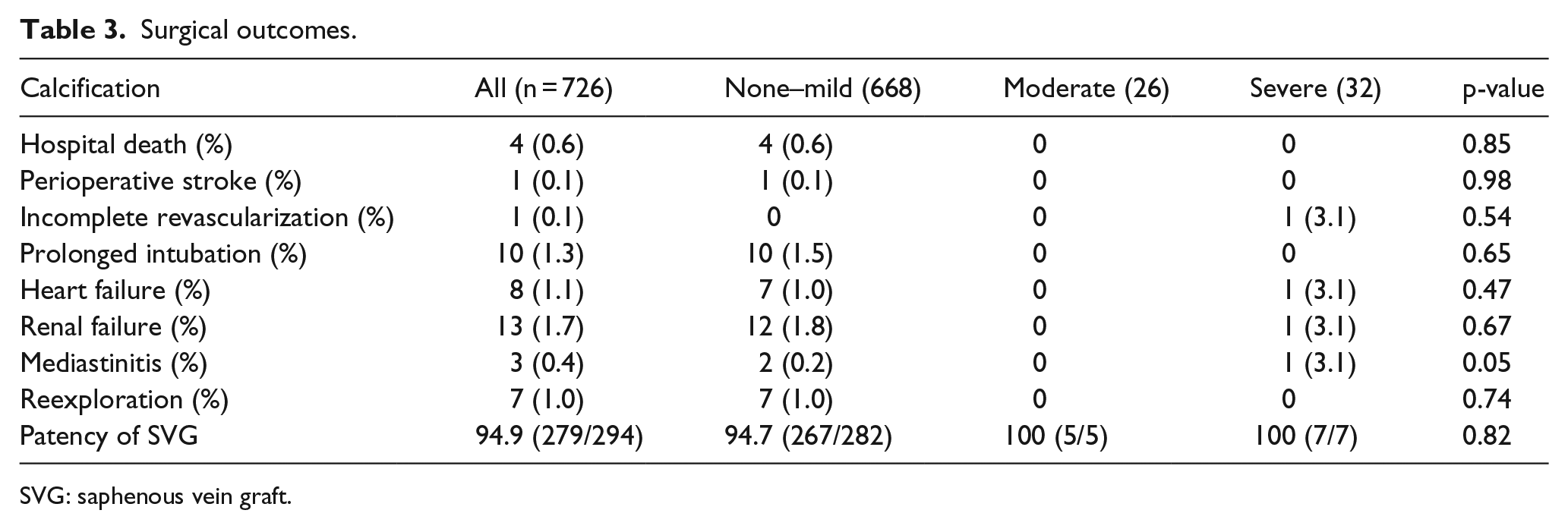
SVG: saphenous vein graft.
Of the 726 patients, 427 patients (58.8%) had postoperative catheter or CT angiography. Among them, angiographic results of 294 anastomoses of SVG showed a patency rate of distal anastomosis of 279/294 (94.9%) (Table 3). There was no significant difference in the patency rate among groups (none–mild: 267/282 (94.4%), moderate: 5/5 (100%), severe: 7/7 (100%), p = 0.82).
Discussion
In our patients, 92.0% had none–mild calcification, 3.6% had moderate calcification, and 4.4% patients had severe calcification. Between these groups, there were significant differences in age, history of stroke, and prevalence of end stage renal dysfunction, suggesting that increased ascending aorta calcification was associated with poor preoperative conditions for CABG. Several reports have found a correlation between calcification of the ascending aorta and increased cardiovascular risk factors.9–11 Takasu reported that the prevalence of aortic wall calcification of the ascending aorta was 1% in 6814 participants without known cardiovascular disease. They found that current smoking, hypertension, dyslipidemia, and aging were associated with the calcification of the ascending aorta. 9 Nishi et al. 10 reported that prevalence of severe calcification of the ascending aorta was 4.3% in patients undergoing cardiac surgery, and they found chronic renal failure, hemodialysis, and aortic stenosis were its predictors. Although correlation between calcification of the ascending aorta and the incidence of postoperative stroke in CABG has been reported previously, the definition of severity and management of ascending aorta are highly variable.2–4 Filsoufi et al. 2 reported that 4.7% of patients before CABG had severe calcification of the ascending aorta. Of their patients, 14% underwent off-pump CABG. The incidence of stroke was 6.3% in patients with aortic calcification. Leyh et al. 3 reported that 23 of 1861 (1.2%) patients undergoing CABG had porcelain aorta. With minimal manipulation of ascending aorta with hypothermic circulatory arrest, no major stroke occurred in their patients. Mills and Everson 5 reported that the incidence of perioperative stroke was 45% for patients with porcelain aorta who underwent CABG with aortic clamping. Van der Linden et al. 12 reported that 36.2% of CABG candidates had significant atherosclerosis, identified by epiaortic ultrasonography. Their patients underwent conventional CABG with cardiopulmonary bypass and aortic clamping with modification of position of cannulation, cross-clamping, and proximal anastomosis of aorto-coronary bypass. The rate of stroke was 6.4% for patients with atherosclerotic disease.
Different graft strategies were selected for the individual patient based on the severity and location of calcification in the ascending aorta by CT and TEE. In addition, poor preoperative condition such as the presence of diabetes and renal failure were also taken into account. In the none–mild calcification group, 44% of patients received partial clamp for proximal anastomosis resulting in no postoperative stroke. Therefore, we believe that use of partial clamp could be rationalized for patients with mild or no calcification, because of its cheaper cost and easier technique without increased risk of embolism. On the other hand, 58 patients (7.9%) had moderate or severe calcification of the ascending aorta making them potentially unsuitable for partial clamp. In these two groups, the aortic no-touch technique would have been ideal for avoiding embolic stroke, and was used for 65% of patients of these groups. However, the aortic no-touch technique is usually more complex, and may carry an increased risk of perioperative complications such as mediastinitis. 13 These considerations led to the aortic no-touch technique being utilized for 65% of the patients in these groups and aorto-coronary bypass with SVG used for the remaining 35% of these high-risk patients. In these groups, an anastomotic device was primarily chosen for proximal anastomosis. In a few patients with moderate calcification, we were able to apply partial clamp carefully during temporarily induced hypotension, exclusively when calcification was located at the posterior portion. Anastomotic devices have been an effective option for minimizing the damage to the ascending aorta. Several studies have reported that devices for proximal SVG were associated with significantly fewer embolic events than partial clamping but with similar graft patency.14–18
By tailoring graft strategy according to severity of calcification, both prevention of stroke and complete revascularization were able to be accomplished in most patients with reasonable operative risks. There were no significant differences in the number of distal anastomoses among the three groups. Stroke occurred in only one patient (0.1%), who had mild calcification and who underwent aorta no-touch CABG, on the fifth postoperative day. Although this patient also had paroxysmal atrial fibrillation, there were no observable thrombi at the time of TEE during the surgery, and it is not clear whether the stroke was due to the atrial fibrillation or to the surgery. Complete revascularization was abandoned in only one patient due to severe calcification and poor preoperative condition. We believe it is crucial to assess embolic risk associated with surgical manipulation and to decide whether proximal anastomoses should be done with partial clamp or device or should be completely avoided for each patient. By avoidance of aortic manipulation, that is, by utilizing the aortic no-touch technique, it is possible to abolish the risk of stroke from the aorta. In particular, off-pump CABG without aortic manipulation definitively facilitates prevention of stroke.6–8 On the other hand, overestimation of embolic risk from the ascending aorta may lead to compromise of the quality of coronary revascularization and increase postoperative complications other than embolism, such as mediastinitis or cardiac events associated with incomplete revascularization. 19
In our experience, the patency rate of SVG was not related to calcification severity. We believe that these highly successful patency rates could also be attributed to the fact that we tailored surgical strategy according to severity and location of calcification detected by preoperative CT. When complete revascularization is not achieved due to extreme calcification of the ascending aorta, hybrid therapy with percutaneous coronary intervention and CABG to the LAD can be a reasonable option. 20
We assessed the calcification of the entire ascending aorta for CABG, but in this study, we classified the calcification by use of CT finding of the ascending aorta near the level of the right pulmonary artery, because this is the part of the aorta most commonly used for proximal anastomosis. Other part was not critically important in off-pump CABG. In addition, intraoperative TEE was performed solely to confirm absence of mobile or protruding plaque in the proximal anastomotic site of aorto-coronary bypass.21–23 During this period, EAU was not systematically performed, because previous studies have shown that results of scanning the proximal aorta by TEE are similar to EAU for detecting atherosclerosis between the annulus and ascending aorta 7 or 8 cm distal to the annulus, where partial clamp or the anastomotic device is usually applied,23,24 corresponding to the level of the right pulmonary artery in many cases.
The limitations of this study are as follows. First, this study was not prospective and randomized, but a retrospective single-arm study without comparison. However, a prospective and randomized comparison would not be ethically feasible regarding this issue. Second, the number of the patients may not have been sufficient. Third, without postoperative brain CT data, we evaluated only clinically evident neurological embolization. Finally, we did not perform EAU systematically. Scanning the aorta by EAU should theoretically detect more thickening and plaques. One concern for EAU is that it might lead to overestimation of quality of the ascending aorta compared to TEE. It may be necessary to reevaluate the benefits and methodology of EAU, from the aspects of not only stroke prevention, but also completeness of revascularization.
Conclusion
Influence of the calcification of the ascending aorta was minimized by tailoring graft strategy to calcification severity. It can practically abolish postoperative stroke while maintaining coronary revascularization success rates.
Footnotes
Authors’ contributions
Y.N. and H.N. analyzed the data and were involved in writing the manuscript. A.I. participated in the study design. M.T. participated in writing the manuscript. A.T., K.H., and K.M. participated in data collection. M.K. participated in the design of the study and performed the statistical analysis. T.A., S.N., and H.N. conceived the study, participated in its design and coordination, and helped draft the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
