Abstract
Objectives
This study propose an extended Technology Acceptance Model (TAM) to bridge the gap between technical feasibility and human-centric adoption by incorporating external variables such as regulatory compliance (RC), training and technical support (TTS), peer influence (PEI), information literacy (IL), and technology/digital literacy (TDL) to investigate the factors driving users’ intention to adopt metaverse telehealth services (MVTHS) in the Chinese healthcare context.
Methods
The study uses a cross-sectional survey-based quantitative research design to validate an extended TAM model. Valid data from 739 respondents were collected across China using an online research questionnaire between October 1 and December 31, 2024. Smart PLS Structural Equation Modeling was employed to test the proposed model.
Results
The results indicate that RC and PEI significantly influence perceived usefulness (PU), perceived ease of use (PEOU), and individual attitudes (ATT) toward the use of MVTHS. TTS demonstrated a significant positive influence on both PU and PEOU but did not influence ATT. While PU positively influenced ATT, PEOU did not significantly affect ATT toward adopting MVTHS. IL significantly influences metaverse telehealth adoption intention (MVTHAI) and moderates the relationship between PU and ATT, as well as between ATT and MVTHAI. Similarly, TDL significantly influences both ATT and MVTHAI. TDL also significantly moderates the relationship between PEOU and ATT, and between ATT and MVTHAI.
Conclusion
A clear regulatory framework is essential for healthcare providers and policymakers to leverage PEI through social channels to encourage users’ ATT to adopt MVTHS. While TTS improves PU and PEOU, PEOU does not directly shape ATT—suggesting that resources should be strategically allocated to RC, IL, and TDL to engage users to adopt MVTHS.
Keywords
Introduction
Telehealth uses digital communications technologies to provide health care in distant places.1–3 It is essential for enhancing healthcare accessibility, especially for rural and marginalized communities. It improves operational efficiency, reducing patient travel and wait times, facilitating immediate consultations between individuals receiving medical care and those delivering healthcare services, and enhancing healthcare quality without increasing costs.4,5 In contrast, traditional telehealth services rely on two-dimensional interactions, limiting engagement and immersive experiences.
The rapid advancement of internet technology services has driven innovative developments within the metaverse, enabling users to access a wide range of services through enhanced virtual interactions and immersive digital environments.6,7 The metaverse technology provides a foundation for the evolution of telehealth services, offering a highly interactive and engaging virtual space for advanced healthcare for virtual consultations and transformed patient engagement.8,9 Integrated cutting-edge technologies such as artificial intelligence (AI), virtual reality (VR), augmented reality (AR), blockchain, and digital twins create a realistic, three-dimensional healthcare environment,10,11 empowering the transformation and provision of Metaverse-driven telehealth (MVTH).
This approach enables patients and healthcare providers to participate in realistic virtual sessions, immersive medical training, AI-powered diagnostics, and blockchain-secured health data management. Unlike traditional telehealth, MVTH promotes a more engaging, community-driven, and persistent virtual healthcare environment, revolutionizing remote medical care, patient education, and rehabilitation through immersive, real-time experiences.12–14 Though both MVTH and traditional telehealth incorporate VR or AR immersive tools to enhance healthcare delivery,15,16 MVTH offers a more integrated interactive experience that boosts the efficacy of conventional telehealth solutions.17,18 It establishes a persistent, collaborative virtual space that facilitates continuous engagement, education, and cooperation,19,20 distinguishing it from the more transactional and isolated nature of traditional VR and AR telehealth applications. As the demand for digital healthcare solutions grows, the adoption of MVTH technologies is expected to increase significantly in the coming decade. 21
The integration of metaverse technology within the healthcare sector remains in its nascent phase, even though it holds significant promise for revolutionizing healthcare delivery services.22,23 This capacity revolutionizes the health care system for the benefit of patients. For instance, those patients who have the chance to undergo virtual examinations in an immersive environment feel as if they are engaging with one another in a familiar setting. 22 MVTH also facilitates remote patients’ access to quality healthcare in isolated areas where health facilities and qualified medical professionals are limited. Moreover, the metaverse facilitates remote medical consultations, enhances access to health-related information and resources, and provides training opportunities. 24 This advancement benefits people to take greater control of their health via informed decision-making.
Furthermore, scholars such as Wang, Zhu 22 and Chengoden, Victor 25 emphasized that the significant adoption of metaverse technologies in the healthcare field requires tackling obstacles related to interoperability issues, data privacy, public trust, information concerns, loss of personal touch, high cost of technology, adoption/acceptance of new technologies, and legal and regulatory compliance Wang, Zhu. 22 Particularly, since the metaverse is still an emerging concept, it is crucial to engage in further promotional and educational activities to boost public awareness and foster acceptance.22,26 While there is growing enthusiasm and hope regarding the metaverse’s potential, a substantial gap remains in understanding its operational mechanisms and real-world applications, 27 particularly in the context of MVTHS. Based on these backgrounds, this study addresses a critical gap in the literature, i.e., the limited research on the adoption of MVTHS from the user perspective. To achieve this, the study extends the TAM framework by combining information literacy, technology literacy, regulatory compliance, training and technical support, and peer influence to examine how these factors collectively explain individuals’ acceptance of MVTHS. Thus, this work bridges this gap by proposing an integrated model that offers a comprehensive framework context for analyzing user acceptance of telehealth services in the metaverse.
The selection and integration of these variables is grounded on well-established technology acceptance theories, digital literacy theory, social cognitive theory, and institutional framework. Thus the adoption of MVTHS will be driven or shaped by three foundational dimensions: First, their intrinsic individual capabilities (IL and TDL grounded in digital literacy theories); Second, the extrinsic social influence from their environment (social/peer influence grounded in social cognitive theory) and; Third, the institutional framework established by the state (RC and TTS grounded in institutional theory). The integrated and extended TAM addresses the complex nature of metaverse telehealth adoption.
Research objectives
This research aims to investigate the factors influencing individuals’ acceptance and utilization of MVTHS from the lens of an extended Technology Acceptance Model (TAM) in China. The specific research questions (objectives) are: 1. How do information literacy and technology literacy impact attitudes and adoption intention of MVTHS? 2. How do information literacy and technology literacy moderate the influence of attitudes on adoption intention and PU and PEOU on attitudes? 3. How do PU and PEOU drive people’s attitudes toward MVTHS? 4. How do regulatory compliance, peer influence, training, and technical support positively impact the PU and PEOU of MVTHS, respectively?
Addressing these research questions equips government officials and stakeholders with critical insights to improve the design of MVTHS by ensuring MVTHS are more accessible, manageable, and receptive to the needs and preferences of prospective users.
Theoretical framework
Technology acceptance model
The Technology Acceptance Model (TAM) Davis 28 has been tested in diverse contexts by numerous researchers to explain the espousal of information systems at the personal level. Although the TAM is based on the fundamental theoretical concept of the Theory of Reasoned Action (TRA), it substantially differs from the TRA in two ways: First, the TAM presents two novel constructs: (1) perceived usefulness (PU), which refers to the belief that utilizing an application will enhance an individual’s performance, and (2) perceived ease of use (PEOU), which signifies the belief that engaging with an application will require minimal effort. Within this model, both PU and PEOU serve as predictors of an individual’s attitude (ATT) toward the application’s usage. 28 Additionally, the TAM does not consider subjective norms as a factor influencing intention. 29
The popularity of TAM is evident in its diverse applications across various fields and contexts, whether through modifications, extensions, or the full utilization of the model. The extensive applications of TAM confirm TAM’s reliability and robustness to adequately account for the use of technology, i.e., demonstrating its robustness as a predictor of technology acceptance. Additionally, TAM is relatively straightforward, consisting of key constructs such as PU and PEOU. This simplicity makes it easier for researchers to operationalize and measure these concepts in studies. Furthermore, TAM versatility allows it to adapt to different technological environments—from information systems to mobile applications, public health, and more.
Thus, focusing on TAM, the study can build on existing literature and also incorporate the context-specific factors (information literacy, technology literacy, regulatory compliance, training and technical support, and peer influence) that influence user acceptance in this novel environment. This adaptability offers a balance between theoretical rigor and practical relevance. Those aforementioned reasons and advantages empowered its application in this paper to study the adoption intention of MVTHS.
Research model
The proposed research model and the summary of the research hypotheses, their paths, and relationships are illustrated in Figure 1 and Table 1. Research model. Summary of proposed research hypotheses, paths, and relationships. Note. ATT=Attitude Toward Using, IL =Information Literacy, MVTHAI = Metaverse Telehealth Adoption Intention, PEI =Peer Influence, PEOU =Perceived Ease of Use, PU =Perceived Usefulness, RC = Regulatory compliance, TDL =Technology/Digital Literacy, TTS =Training and Technical Support.

Research hypotheses development
Regulatory compliance (RC)
Regulatory compliance by service providers is a fundamental element in guaranteeing users’ safety and confidence in any technology-driven healthcare system. Particularly, the strong legislation and regulation are vital for governance, accountability, and the assurance of safety and security for healthcare professionals and technologies. 30 Regulatory compliance measures to guide telemedicine services, such as remote physiologic monitoring, check-ins, therapeutic monitoring, and the disclosure of service location, 31 can boost user adoption of telehealth technology systems. Gajarawala and Pelkowski 32 argue that various regulatory, legal, and repayment issues have obstructed the broader usage of telehealth services. Therefore, MVTHS providers who ensure compliance with government regulations regarding state-specific physicians and practice measures will encourage users’ positive attitudes towards MVTHS. MVTHS providers should comply with applicable state and federal privacy laws, as well as strict regulations related to advertising and marketing of health-related products and services. It is essential to implement regulations and compliance measures for “remote clinical healthcare, health-related education for patients and professionals, public health, and health administration, utilizing electronic information and telecommunication technologies”, 33 along with metaverse technologies. Additionally, the nature of the government regulatory framework and the MVTH system design reflect on the perceived ease of use and usefulness of such a technology. Furthermore, government support has been confirmed to influence technology adoption. 34 Based on this, we proposed that RC towards MVTHS would influence the PU, attitudes, and PEOU toward MVTHS. Accordingly, H1, H2 and H3 were proposed.
RC has a positive impact on the PU of MVTHS.
RC has a positive influence on ATT toward using MVTHS.
RC has a positive influence on the PEOU of MVTHS.
Training and technical support (TTS)
Adequate training and technical support are vital for users to achieve maximum benefits from the use of technology-driven healthcare services. Better training and technical support have been the key enablers for efficient delivery of important telehealth services.35,36 Particularly, the provision of adequate training and technical support through health coaching mechanisms (education, encouragement, feedback, etc.) can drive users’ behavior towards adoption of telehealth services. 37 Furthermore, some argue that providing adequate training and technical support can better address the barriers patients face in using telemedicine services, healthcare systems, and telemedicine portals, and at the policy level, thereby achieving equity in the field of telemedicine. 38 In the context of MVTHS, adequate training is required to understand metaverse healthcare services and how they differ from traditional telehealth services for their usage. Also, teaching users how to operate MVTH systems, such as movement, communication tools, and access to virtual health spots, boosts their confidence and attitude in metaverse health systems. Training that provides information regarding the essential hardware and software prerequisites, such as VR headsets, mobile devices, and computers, along with detailed instructions on their setup, would be helpful to users. This includes a comprehensive guide on utilizing MVTH applications to schedule appointments, engage with healthcare professionals, and obtain health-related resources. Moreover, a help desk that offers multiple communication channels, such as phone calls, chat, and email, will provide users with round-the-clock support for their technical difficulties. Additionally, developing an extensive online repository of information that encompasses commonly asked questions, troubleshooting manuals, and resource articles addressing prevalent issues and their resolutions would serve as an effective method of technical assistance for users. Studies have shown that technical support drives both PU and PEOU of technology. 39 Based on this, we assert that these training and technical support services provided to MVTH users would shape their perceptions of PU, attitudes, as well as PEOU associated with MVTHS. Consequently, H4, H5 and H6 were proposed.
TTS has a positive influence on the PU of MVTHS.
TTS has a positive influence on the ATT towards using MVTHS.
TTS has a positive influence on the PEOU of MVTHS.
Peer Influence (PEI)
Peer Influence (PEI) is one of the significant social factor that facilitate the diffusion and adoption of technology.40,41 Individuals usually recognize and value the power of their peers to influence their actions and work-related activities due to the implicit trust mechanism it generates. 42 With the ongoing expansion of the metaverse, which integrates virtual environments and interactions into sectors such as healthcare. It is essential to comprehend the influence of peer dynamics on the utilization of these services. The likelihood of individuals trusting MVTHS increases when they receive endorsements from their peers. Positive feedback and recommendations from friends or family can serve as social validation, prompting others to consider utilizing these services. People tend to adopt the behaviors of those around them in their social circles. When individuals witness their peers engaging with MVTHS, they may be more likely to participate as well. Various studies have confirmed that peer influence is a positive indicator of a positive attitude toward technology adoption.43,44 Consequently, we propose that peers will influence individual knowledge regarding the PU, attitudes, and PEOU of MVTHS. Accordingly, H7, H8 and H9 were proposed.
PEI positively influences the PU of MVTHS.
PEI positively influences an individual’s attitude towards using MVTHS.
PEI positively influences the PEOU of MVTHS.
Perceived usefulness (PU)
The PU pertains to the degree to which an individual holds a belief that the application of a particular technology will enhance his/her performance.28,45 Perceived usefulness encapsulates the expected benefits a technology provides to its users. Telehealth represents an auspicious approach to enhancing access to behavioral healthcare for both uninsured communities and the general population. 46 Metaverse technology facilitates patients’ access to healthcare conveniently via telehealth services without a physical visit. Access to healthcare in remote or deprived regions would not only encourage more users to use it but also drive their positive attitudes toward MVTHS. Consequently, MVTHS that provide tangible benefits for users to access health services would influence users’ attitudes toward them. Empirical studies have confirmed that the PU of technology, such as telehealth, positively drives attitudes toward it.47,48 Accordingly, H10 was advanced.
PU has a positive influence on attitudes toward using MVTHS.
Perceived ease of use (PEOU)
PEOU denotes the level of confidence a person has in the belief that a particular technology will require minimal effort and be straightforward to utilize.28,49 The potential of telehealth technology to integrate with existing IT systems and user-friendly designs, accompanied by adequate technical support, is one of the issues concerning the user-friendliness of telehealth services. 50 The ease of use associated with telehealth services that make it easier for users to operate and learn is a top priority for users. 51 Also, information and communication technology skills have been determined to be key antecedents of the perceived ease of telehealth service. 51 PEOU in the context of MVTH is the extent to which individuals believe that utilizing telehealth services is free of effort. A straightforward, intuitive interface of MVTHS that enhances users’ comfort and reduces the cognitive load required to navigate the platform would increase users’ PEOU. Easy-to-use features like straightforward appointment scheduling, clear video calls, or accessible medical records can contribute positively to PEOU. Additional features like appointment reminders, simple billing processes, and integration with other health tools (like wearable health apps) can enhance the overall user experience towards MVTHS, making the platform feel easier to use. These easy-to-use features of MVTHS would significantly impact users’ attitudes towards it. Research indicates that the PEOU is positively correlated with users’ attitudes.52,53 Subsequently, H11 was proposed.
PEOU has a positive influence on attitudes toward using MVTHS.
Attitude (ATT)
Attitude is characterized as a predetermined mental state that reflects one’s views on the advantages of a system in optimizing job efficiency, improving effective management of time for carrying out tasks, and its role in elevating the quality of the work performed. 54 A notable segment of the population faces considerable healthcare demands and seeks enhanced healthcare access for themselves and their families, making extensive utilization of information and communication technology (ICT). 48 At the same time, there is a generally positive perception of telehealth, with socio-demographic variables, including age, location, education level, and family size, significantly impacting attitudes toward telehealth services. 48 The perspective (attitude) on the utilization of MVTH is impacted by a variety of issues, such as technological progress, cultural viewpoints, user interactions, and accessibility to healthcare services. MVTH can serve an essential function in increasing accessibility for individuals located in remote areas with inadequate services. For those who encounter difficulties in traveling to physical appointments, metaverse solutions may present a more convenient alternative, consequently promoting a positive attitude towards their utilization. However, access to the necessary technology, such as virtual reality headsets and high-speed internet, is not universally available. As a result, individuals who possess these essential systems are likely to exhibit a more favorable attitude towards utilizing MVTHS. A variety of research findings suggest that the attitudes held by users are a vital determinant in both the acceptance and the efficiency of technology implementation in real-world scenarios.55–57 Studies have confirmed explicitly that attitudes positively influence the intent to use telehealth. 53 Based on the foregoing, H12 was proposed.
ATT toward using MVTHS has a positive influence on the adoption intention of MVTH.
Information literacy (IL)
IL is defined as the skill to identify the need for information, undertake specific tasks or resolve issues, search for information in a cost-efficient manner, organize or reorganize information sources, interpret and analyze the required information, and evaluate the trustworthiness, reliability, and dependability of the information. 58 The concept of IL includes a range of abilities that equip individuals to proficiently search for and analyze different information sources, while also evaluating the authenticity and reliability of the information presented. 59 It entails a process of introspective inquiry, grasping, and valuing the formation and relevance of information, as well as its proficient use in generating novel insights. 59 To function effectively within society, an individual must prioritize the advancement of information literacy. 60 In the current era characterized by an abundance of information, individuals need to develop the skills necessary to assess the authenticity and reliability of the information they encounter, 59 particularly concerning digital health services such as telehealth. Individuals’ capacity to access health-related information is crucial to their effective management of well-being, 59 particularly when using MVTHS. Consequently, the degree to which individuals can obtain, interpret, and understand critical MVTH information and services is essential for making informed health decisions. These abilities may influence their perceptions of the PU, attitudes, and PEOU, which might lead to MVTH service use. Studies have confirmed that information literacy failed to influence the PU of technology directly but exhibited an indirect effect on the intention to adopt technology through positive attitude. 52 Another study showed that the technology adoption behavior was moderated by information literacy. 61 However, in this study, we assert that IL can directly influence both attitudes and adoption intention of MVTHS as well as moderate the impact of PU on attitudes and MVTH adoption intention. According, H12, H13, H14, H15 and H16 were advanced.
IL positively influences the individual’s attitude toward MVTHS.
IL positively influences the individual’s intention of adopting MVTHS.
IL positively moderates the PU influence on an individual’s attitudes toward using MVTHS.
IL positively moderates the influence of the individual’s attitude on the adoption intention of MVTHS.
Technology/Digital literacy (TDL)
The idea of technology or digital literacy is regarded as a crucial element in achieving digital transformation, 62 particularly in the integration of information technology in healthcare delivery systems. Digital literacy encompasses the skills and attitudes individuals need to efficiently use digital technologies by enabling them to access, manage, evaluate, and integrate digital resources, as well as create and communicate digital content. 63 This concept is relevant to personal contexts and aims to foster positive social actions and self-reflection. 63 Digital literacy plays a crucial role in improving health literacy in contemporary society. The capacity to access, comprehend, and effectively use health information has relied on one’s digital skills and knowledge.64,65 TDL encompasses the ability to navigate online health resources, interpret digital health records, and effectively use health-related applications 65 such as MVTH systems. Higher levels of digital literacy significantly influence health literacy. Therefore, inadequate literacy can directly impact individuals’ health by restricting their personal, social, and cultural growth, thereby obstructing the advancement of digital health literacy. 66 In this research, digital literacy and MVTHS refer to an individual’s ability to navigate virtual environments effectively and efficiently for healthcare purposes. Individuals’ poor technology literacy is identified as a barrier to access to telehealth care. 67 Researchers argue that digital literacy positively influences the ease of use of technology and, indirectly, the intention to use it, through one’s attitude toward its use. 52 Digital literacy also showed a direct impact on effort expectancy, as well as indirectly affected intention to use via effort expectancy. 62 In our study, we posit that technology literacy may influence individuals’ perceptions of MVTHS attitudes and adoption intentions. Additionally, we assert that the TDL moderates the influence of PEOU on attitudes as well as the influence of attitudes on the adoption intention of MVTHS. Consequently, H17, H18, H19 and H20 were advanced.
TDL positively influences the individual’s attitude toward MVTHS.
TDL positively influences the individual’s intention of adopting MVTHS.
TDL positively moderates the PEOU influence on an individual’s attitudes toward using MVTHS.
TDL positively moderates the influence of the individual’s attitude towards using MVTHS on the adoption intention.
Methods
Research design and questionnaire development
The study uses a cross-sectional survey design based on a quantitative approach and developed a comprehensive research questionnaire for data collection to analyze the proposed model depicted in Figure 1. The questionnaire instrument was based on items adopted from past literature works, but was adjusted to the context and content of this study. The variable items were adapted as follows: PU, 68 PEOU, 68 attitudes,69,70 PEI,71,72 adoption intention,73,74 RC, 75 TTS, 76 IL, 52 and TDL. 77 The first component of the questionnaire consists of these main variable items, which were measured on five (5) points Likert scales ranging from 1 = strongly disagree to 5 = strongly agree. The second component consists of basic demographic information about respondents, such as age, gender, education, and professional type.
Study settings
We hired two Chinese teachers who were both fluent in English and Chinese and understood the subject matter (experts in public health) to translate the English questionnaire into Chinese. This approach was implemented to ensure that Chinese respondents (Chinese-speaking audience) could relate to the questionnaire, thus promoting active engagement and high-quality responses. Back-translation (from Chinese into English) was conducted to verify the accuracy of the earlier version. It also helped assess the reliability and validity of the translated survey instruments. We ensured that the questionnaire was free from any ambiguity and did not pose any challenge to respondents to get quality responses. Therefore, the questionnaire was pre-tested and piloted among 60 respondents. This was an important step to ensure the effectiveness and validity of the instrument before a full-scale data collection was undertaken.78,79 The pre-testing and piloting study improved the overall clarity of the questions and thus enhanced the likelihood of obtaining high-quality responses and data.
Sampling strategy and data collection
We employed convenience sampling to collect the data. The convenience sampling technique provides researchers with straightforward access to readily available respondents, decreasing the costs associated with data collection by lessening the need for extensive planning or travel.80,81 Moreover, it enables the rapid collection of data, ensuring broad coverage. The questionnaire was hosted on the WJX online survey platform (https://www.wjx.cn/) between October 1 and December 31, 2024. The questionnaire link, including a QR Code, was then shared with respondents residing in Wuhan, Hubei Province, China, via social media platforms such as WeChat (a popular social media platform in China) to collect data. People were also requested to share the questionnaire link/QR code with their friends, family, and others within their communities, work units, and organizations. This method allows us to disseminate the questionnaire quickly and enables participants to complete the survey at their convenience. Additionally, using WeChat offers the advantage of reaching a large audience given its extensive user base. This method can significantly reduce the biases that may arise from collecting data exclusively through convenience sampling.
A total of 900 questionnaires were collected between October 1 and December 31, 2024. After careful screening, 161 invalid responses were deleted based on inclusion/exclusion criteria. The remaining 739 valid responses were retained and utilized for the analysis. The primary criterion for determining the inclusion or exclusion of participants was the stipulation that they must be at least 18 years old. Additionally, the identification of response patterns, where participants select the same response option across multiple items, served as a basis for including or excluding specific responses. Following data collection, a screening process was implemented to assess the dataset for missing values, outliers, and response patterns. Other measures, such as Cronbach’s alpha and factor loadings, were also employed to identify and eliminate responses that did not meet the established thresholds.
The adequacy of the sample was determined using a common rule of thumb that recommends that the sample size should be at least 10 times the number of items. 82 This is commonly used in the context of structural equation modeling (SEM) or other multivariate analyses to ensure adequate statistical power. The current study has 37 construct items, implying that the minimum required sample should be 370 (37*10). Our sample size exceeds the recommended minimum sample size, indicating the robustness of the analysis and the sample’s representativeness. The data were analyzed using SPSS and SmartPLS, employing structural equation modeling. Smart PLS is an effective tool designed for researchers interested in applying PLS-SEM to analyze path models.83,84
Ethical statement and informed consent
This study was granted ethical approval (No. NTU-IRB24-SML05) by the Institutional Review Board (IRB) of NingboTech University, Ningbo, China. Additionally, written informed consent was obtained from all the participants. The participants were informed of their right to withdraw or voluntarily participate in this study at any point in time. They were assured that the information collected through this questionnaire would be used only for scientific research and would not be shared with any third party. Additionally, we strictly follow the standardized academic and institutional guidelines along with the 2024 Declaration of Helsinki Ethical standards to ensure data privacy, anonymity, and safety during the data processing and analysis stage.
We used the STROBE reporting guideline to draft this manuscript, and the STROBE reporting checklist is included as supplement material A.
Data analysis and results
Demographic characteristics of the respondents
Sample basic information.
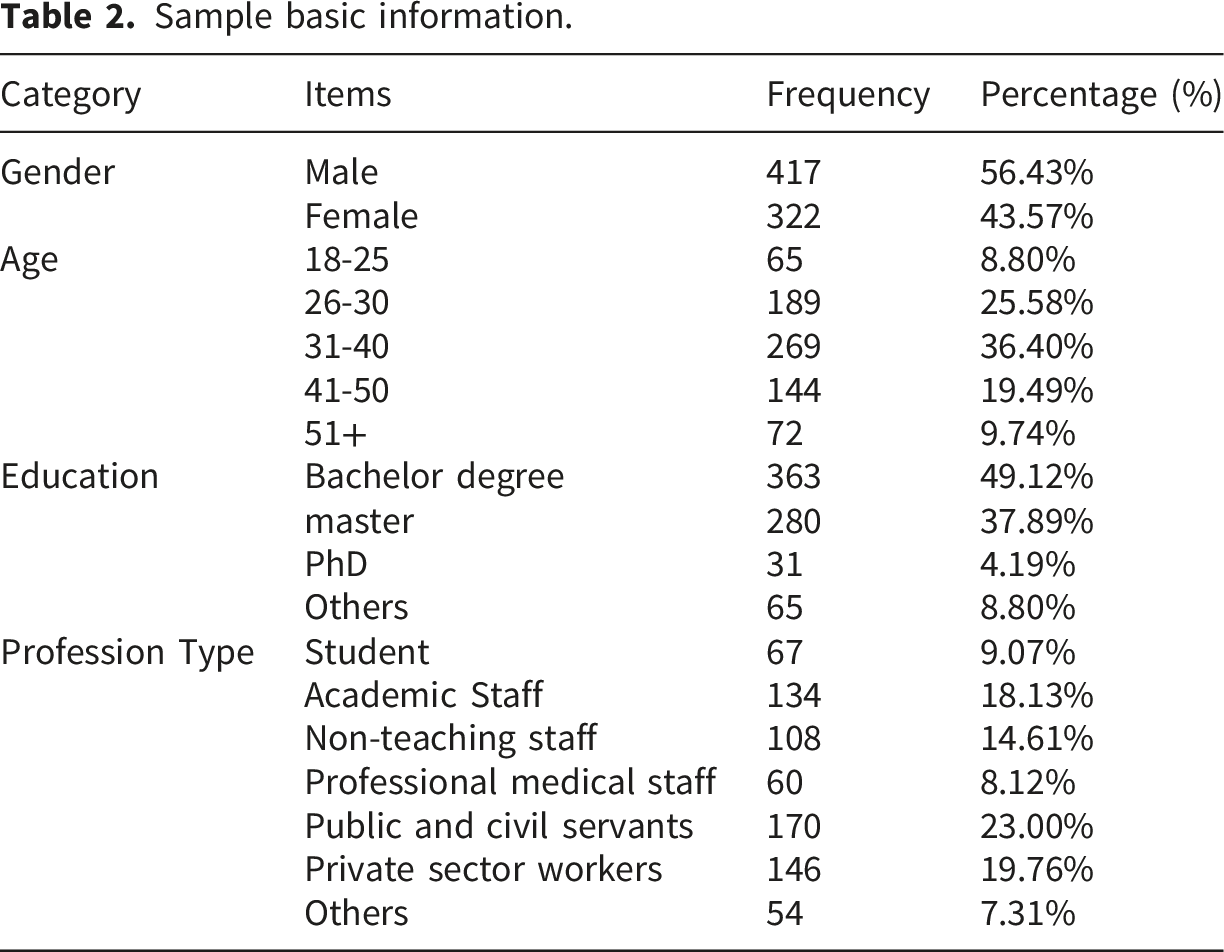
Common method bias (CMB) test
We used Harman’s single-factor analysis to test CMB in our data. Results indicate that a single factor explained 25.617% of the total variance, which is well below the recommended threshold of 50%. Consequently, CMB is not a threat in our study.
Measurement model analysis
Reliability and convergent validity test.

Note. ATT=Attitude Toward Using, IL =Information Literacy, MVTHAI = Metaverse Telehealth Adoption Intention, PEI =Peer Influence, PEOU =Perceived Ease of Use, PU =Perceived Usefulness, RC = Regulatory compliance, TDL =Technology/Digital Literacy, TTS =Training and Technical Support.
Validity testing encompasses both convergent validity and discriminant validity assessments. Convergent validity pertains to the degree of similarity in measurement outcomes when various methods are employed to evaluate a particular scale. According to Fornell, 86 the convergent validity of variables can be determined by the factor loading, composite reliability (CR), and average variance extracted (AVE) of the measurement items. Among them, the factor loading of the measurement items must exceed the minimum limit of 0.6, the composite reliability CR value of the scale must exceed the minimum limit of 0.7, and the average variance extracted AVE value must be greater than the minimum limit of 0.5. As shown in Table 3, the factor loading of the measurement items of the nine scales ranges from 0.782 to 0.870, all greater than 0.6; the composite reliability (CR) of the nine scales ranges from 0.890 to 0.904, all greater than 0.7; the average variance extracted (AVE) ranges from 0.646 to 0.733, all greater than 0.5. It can therefore be concluded that the convergent validity of the seven scales in this study is good.
Fornell-Larcker criterion.

Note. ATT=Attitude Toward Using, IL =Information Literacy, MVTHAI = Metaverse Telehealth Adoption Intention, PEI =Peer Influence, PEOU =Perceived Ease of Use, PU =Perceived Usefulness, RC = Regulatory compliance, TDL =Technology/Digital Literacy, TTS =Training and Technical Support.
Heterotrait-monotrait ratio (HTMT).
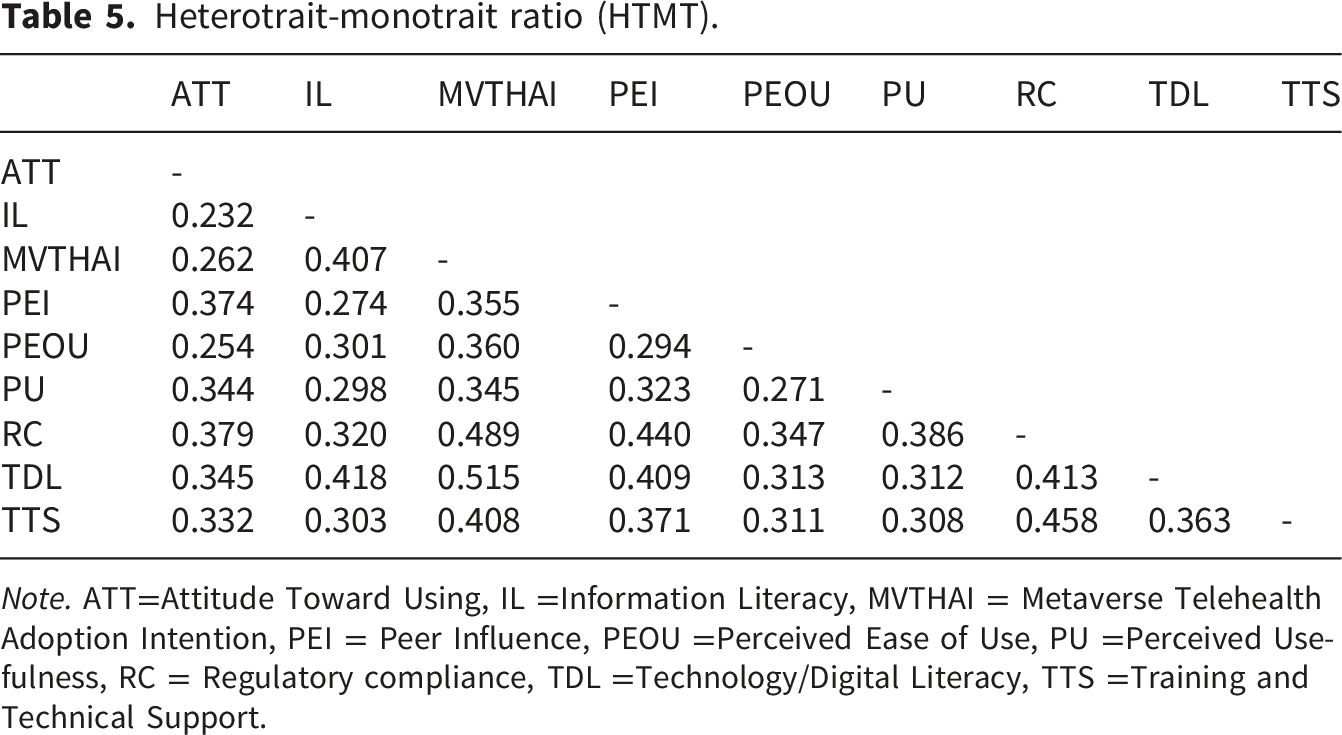
Note. ATT=Attitude Toward Using, IL =Information Literacy, MVTHAI = Metaverse Telehealth Adoption Intention, PEI = Peer Influence, PEOU =Perceived Ease of Use, PU =Perceived Usefulness, RC = Regulatory compliance, TDL =Technology/Digital Literacy, TTS =Training and Technical Support.
Structural model analysis
Structural model test.

Note. ATT=Attitude Toward Using, IL =Information Literacy, MVTHAI =Adoption Intention, PEI = Peer Influence, PEOU =Perceived Ease of Use, PU =Perceived Usefulness, RC = Regulatory compliance, TDL =Technology/Digital Literacy, TTS =Training and Technical Support.
Hypotheses testing
Hypotheses testing.

Note. ATT=Attitude Toward Using, IL =Information Literacy, MVTHAI = Metaverse Telehealth Adoption Intention, PEI =Peer Influence, PEOU =Perceived Ease of Use, PU =Perceived Usefulness, RC =Regulatory compliance, TDL =Technology/Digital Literacy, TTS =Training and Technical Support.
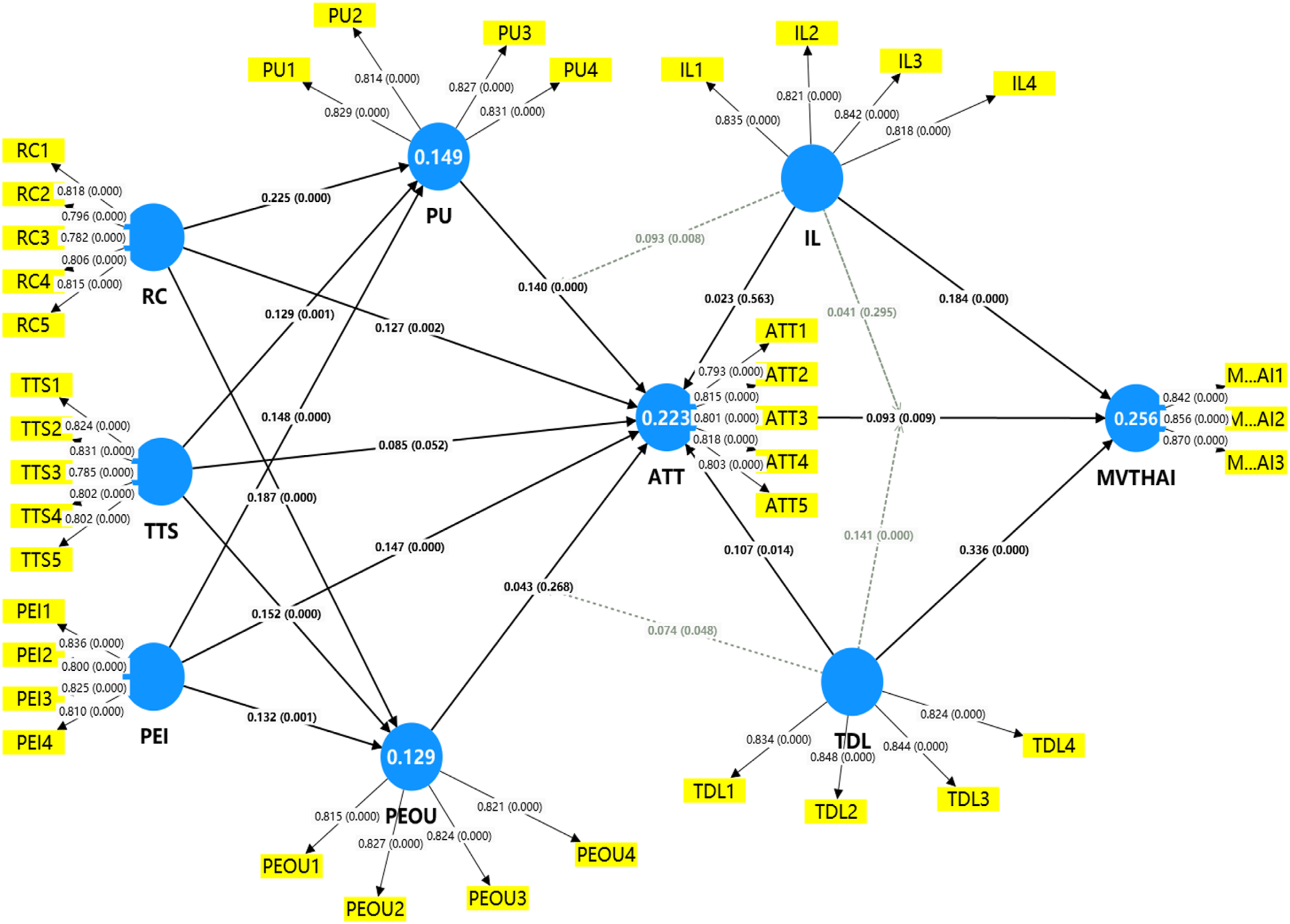
Validated structural MVTH model diagram.
The study also finds that attitude toward using MVTHS (β=0.093, t=2.598, p<0.01), IL (β=0.184, t=4.944, p<0.001), and TDL (β=0.336, t=8.467, p<0.001) have a significant positive impact on the Adoption intention of MVTHS. This means that the positive attitude toward MVTHS and digital literacy can play an important role in the adoption of MVTHS in China, validating
Moreover, our analysis revealed that RC (β = 0.187, t = 4.435, p<0.001), TTS (β = 0.152, t = 3.694, p<0.001), and PEI (β = 0.132, t = 3.32, p<0.01) have a significant positive impact on PEOU of MVTHS in China. The findings consequently provide support for
Additionally, the interaction term between IL and ATT (β = 0.041, t = 1.046, p > 0.05) on the adoption intention of MVTHS was not significant, indicating that IL did not play a significant moderating role in the relationship between ATT and the adoption intention of MVTHS. This finding fails to provide support for
Discussions
This paper explores the factors influencing the adoption of MVTHS from the lens of an extended Technology Acceptance Model (TAM). Based on the results analysis, we have demonstrated that RC positively influences ATT, suggesting that both individuals and healthcare providers are more inclined to feel secure and assured in their engagement with these services when the right legal regulatory frameworks are in place and complied with. Telehealth services within the metaverse, guided by regulatory frameworks and compliance standards,94,95 have the potential to enhance utilization rates, advance patient outcomes, and contribute to a more resilient healthcare system that seamlessly incorporates digital health technologies. Moreover, the positive influence of regulatory compliance on attitudes toward metaverse-telehealth services reflects China’s robust legal framework governing health data. China has established comprehensive regulations, including the Cybersecurity Law, Data Security Law, and Personal Information Protection Law, which collectively govern internet healthcare provision. 96 The National Health Commission further mandates that medical institutions implement strict data security protocols, including access controls and traceability mechanisms for electronic medical records. 97 For metaverse healthcare applications specifically, scholars emphasize that proactive development of legal frameworks is imperative for sustainable development. 98 This regulatory environment demonstrates to users that their sensitive health data receives legal protection, thereby fostering positive attitudes toward adopting these innovative services within China’s uniquely structured digital health landscape. It has also been noted that legal concerns prevent the application of the metaverse in the health sector, 99 limiting its transformative role in the healthcare ecosystem. This transformation can be realized in the form of efficient healthcare delivery, improved patient outcomes, and reduced healthcare costs. 98 Maximizing the value of the medical metaverse requires proactively shaping technical and legal standards and continuously monitoring their performance to ensure sustainable development. 98 This finding cannot be compared to any current or past studies due to novel testing.
The positive impact of PEI on ATT indicates that individuals are more inclined to embrace and utilize MVTHS when they witness their peers positively interacting and advocating for them. The positive experiences shared by friends, family, or colleagues 100 regarding MVTH can play a significant role in alleviating skepticism and fostering greater acceptance of these services among others. This contributes to building trust in MVTH platforms, thereby encouraging users to feel more at ease when seeking care in a virtual setting. Healthcare organizations can create online communities where individuals can share their experiences with MVTH. These platforms can provide peer support, thereby increasing comfort levels and encouraging more individuals to utilize telehealth services. Our findings contradict a study that demonstrated that social influence failed to influence intention to use innovative healthcare technologies. 101
Furthermore, the positive effect of PU on ATT towards the use of MVTHS means that individuals are more likely to have a positive outlook on these services if they perceive that engaging with metaverse technology leads to better health outcomes or provides considerable benefits in comparison to traditional telehealth or in-person appointments. This positive perception can foster greater acceptance and utilization of telehealth solutions within the metaverse, as individuals acknowledge their ability to provide timely, effective, and personalized healthcare. This discovery aligns with research findings that PU drives the users’ attitudes toward telehealth technology. 47 It also supports a study that performance expectancy is positively related to attitude towards AI-based healthcare technology. 101
The positive influence of TDL on ATT demonstrates that with a higher level of digital literacy, patients can confidently navigate virtual environments, effectively engage with healthcare providers, and smoothly access online resources that enhance their understanding of health issues. Those who are adept with technology tend to regard MVTHS as valid and beneficial, which helps to alleviate skepticism and opposition. Users equipped with significant digital skills are more prone to engage proactively in their health management, contributing to greater adherence to treatment strategies and health guidelines, including health care behaviors. 102 Our finding is in line with a study that e-health literacy has a positive influence on attitude towards internet health information. 103 It also supports a study in a non-metaverse context that digital literacy is positively associated with attitude using information technology. 104
Furthermore, the positive influence of ATT on the adoption intention of MVTHS means that individuals who hold a favorable view and positive emotions regarding these services are more likely to express an intention to utilize them. This further implies that if users perceive MVTHS as advantageous, efficient, and user-friendly, they are more likely to embrace and interact with MVTH technologies. If users become aware of the benefits, like enhanced access to healthcare, personalized interactions, and improved relationships with healthcare providers, they are more likely to adopt a positive attitude. Positive attitudes toward digital health solutions promote the exploration, use, and trust of eHealth tools, facilitating their integration into routine healthcare. 105 Our findings validate previous studies that attitude drives the adoption intention of telehealth technology.106,107
The positive influence of IL on the adoption intention of MVTH means that individuals who possess higher levels of IL are more likely to embrace and utilize these innovative healthcare solutions. Because IL enhances individuals’ capacity to efficiently locate, assess, and utilize information, 108 which is essential for successfully navigating the intricacies of telehealth services within a metaverse context. Individuals who sharpen their information literacy skills are more capable of understanding the features, advantages, and potential hazards related to MVTHS. This level of understanding can help alleviate worries and foster greater confidence in engaging with MVTHS. This discovery aligns with previous research that IL, in the form of e-health literacy, drives technology adoption. 107
The positive influence of TDL on the adoption of MVTHS suggests that individuals with higher levels of technological understanding and skills are more likely to embrace and use telehealth services in the metaverse environment. Technologically literate personnel are more aware of the benefits and potential hazards linked to MVTHS, allowing them to make more prudent decisions about their healthcare options. Low digital literacy is a significant barrier to e-health services adoption. 109 Higher technology literacy can reduce anxiety and stress while using new technologies and boost confidence in one’s own ability to use those technologies. 110 Research confirms that increasing digital skills through training programs encourages adoption of telemedicine. 111 Our findings align with a study that technology literacy (i.e., digital competence) drives the adoption of telehealth. 112
Additionally, the positive influence of RC on both PU and PEOU of MVTHS indicates that when there are clear regulatory frameworks and compliance standards in place, users are more likely to view these services as beneficial. To comply with regulations, providers should be required to embrace best practices and technologies that prioritize user-friendliness and improved overall user experience (i.e., alleviating ambiguity and uncertainty). Moreover, these findings established a trustworthy operational foundation within China’s strict legal system. Feng, Niwa 113 found that regional regulations in East Asia significantly shape users’ expectations of mHealth, with Chinese users exhibiting heightened sensitivity to compliance signals that enhance perceived utility. Jiang and Zheng 114 demonstrated that internet hospital apps achieving higher compliance scores provide clearer data processing protocols, reducing cognitive burden and thereby improving PEOU. Furthermore, Akiogbe, Feng 115 identified legal supervision as an indirect but significant factor shaping healthcare professionals’ technology perceptions, suggesting compliance frameworks facilitate acceptance by legitimizing system functionalities. Thus, regulatory compliance will push users to use these services and, consequently, will enhance both PU and PEOU. These results, though, could not be compared with any past or current studies on MVTHS. However, these findings are supported by a non-metaverse study that government regulation drives PU and PEOU of a technology. 116
The positive influence of training and technical support on PU and PEOU of MVTHS suggests that effective training and technical support empower users to perceive telehealth services as useful and easy to use, leading to a higher degree of engagement with MVTHS. The provision of training and technical support reduces the frustrations that arise from technical challenges. 117 Therefore, providing necessary training and support is essential for keeping users informed about new features and best practices in the use of MVTHS. This approach helps sustain high levels of PU and PEOU over time, which is vital for the long-term viability of telehealth services within the metaverse. A lack of adequate technical support has been identified as a significant barrier to the adoption of video-based telehealth services. 118 Our findings are similar to a study, though from a non-MVTH field, that training and technical skills have a direct influence on both PU and PEOU.39,119
Moreover, the non-significant influence of TTS on the ATT toward the use of MVTHS indicates that while there may be a slight tendency for increased training and support to improve users’ attitudes, this effect is not strong enough to be statistically significant. It further implies that users may not view TTS as a crucial component influencing their attitudes, suggesting that other factors, such as service quality, accessibility, or individual experiences, may have a more substantial impact. This finding contrasts with a study from a non-MVTH area that indicated technical support directly drives the attitudes toward the use of technology. 39 It also contradicts a study that prior training in computer use, along with the frequency of computer usage, significantly shapes attitudes toward ICT. 104
Furthermore, PEI showed a significant positive impact on both PU and PEU of MVTHS, suggesting that PEI plays a crucial role in shaping individuals’ perceptions and acceptance of MVTHS. Additionally, it implies that if peers advocate positively for these services based on positive experience and outcomes, individuals are more likely to regard them as beneficial. 105 This highlights the importance of peer-driven initiatives and community engagement 120 in the diffusion of health technologies such as MVTHS. This further indicates that constructive peer influence may lead individuals to consider telehealth services as more accessible, due to common experiences or recommendations from their peers. In line with our findings, social influence, similar to peer influence, positively drives PU and PEOU of telemedicine. 121
However, the lack of significant influence of PEOU on attitudes toward MVTHS indicates that ease of use alone does not lead to a positive attitude. In the Chinese context, the non-significant PEOU→Attitude path can be robustly explained by the nature of the user sample and technology type. Tang, Yang 122 study of Chinese online medical websites found PEOU influenced behavioral intention only indirectly through attitude and usefulness, suggesting that for health-related technologies in China, ease of use may function as a basic expectation rather than an attitude-shaping factor. 122 This aligns with meta-analytic evidence showing that user type (students vs. professionals) and technology characteristics moderate TAM relationships. 123 For Chinese users with prior digital health experience, PEOU becomes a hygiene factor—necessary but insufficient to generate positive attitudes when metaverse telehealth promises transformative rather than merely convenient healthcare solutions. Furthermore, the non-significant impact of PEOU on attitude aligns with cross-cultural meta-analyses demonstrating that TAM relationships function differently across contexts. Li, Zhu 124 found that while PEOU has stronger effects on PU and attitude in Eastern cultures compared to Western cultures, this relationship attenuates when technology complexity exceeds users’ existing competency schemas. Guo, Zhu 125 further revealed that effect sizes among TAM constructs are greater for supervisory employees or in Eastern cultures, yet PEOU’s direct influence diminishes when pragmatic utility—specifically, regulatory compliance and peer influence in collectivist contexts—supersedes usability concerns. Similarly, the insignificant impact of information literacy on attitudes suggests that simply being informed on how to use the technology does not improve users’ views, indicating that there are more complex challenges involved beyond just understanding the technology or its information. These findings contradict studies that have shown PEOU has a positive impact on attitudes towards telemedicine 106 and other studies that eHealth literacy (information literacy) has a positive and significant impact on attitudes towards telehealth-medicine. 95 Also, given that neither perceived ease of use nor information literacy had a significant impact on attitudes, it may be advantageous for policymakers to support a more comprehensive strategy for telehealth that incorporates metaverse solutions alongside conventional healthcare services. This approach could entail the promotion of hybrid models that merge virtual and in-person interactions, effectively addressing potential user apprehensions regarding technology while simultaneously improving access to care.
In terms of moderating role results, the positive moderating effect of IL on the relationship between PU and adoption intention indicates that individuals with advanced IL skills possess a greater capacity to comprehend and value the advantages offered by telehealth services in the metaverse environment. This enhanced understanding can strengthen the favorable correlation between the perceived utility of these services and their willingness to embrace them. Additionally, the non-significant moderating influence of information literacy on the relationship between attitude and adoption intention means that information literacy does not have a statistically meaningful effect on how an individual’s attitude toward MVTHS influences their intention to adopt those services. The research findings imply that an individual’s level of information literacy does not influence their attitude toward MVTHS, which remains a reliable predictor of their intention to adopt such services. Consequently, this suggests that merely increasing information literacy may not enhance adoption rates if individuals’ attitudes toward the services are not positively oriented.
Furthermore, the positive moderating influence of TDL on the relationship between PEOU and ATT means that individuals with greater TDL experience may have a more pronounced positive effect of PEOU on their ATT regarding the use of MVTHS. People with higher levels of technological proficiency are more inclined to perceive MVTHS as user-friendly, resulting in a more favorable disposition toward the adoption of these services.
Finally, the positive moderating effect of TDL on the relationship between ATT and adoption intention of MVTHS suggests that individuals with advanced TDL tend to exhibit more positive attitudes towards these services (metaverse telehealth services), thereby enhancing their likelihood of adopting them. Developers of MVTH solutions ought to take into account the diverse levels of technological proficiency among prospective users. The findings on the moderating outcomes cannot be compared with any prior or contemporary literature, particularly regarding telehealth services in the metaverse, as these interactions were never tested before. However, our findings are similar to those of a non-metacosmic study of e-pharmacies, which showed that technological literacy plays a significant moderating role between users’ willingness to use e-pharmacies platforms and their actual use of those platforms. 126
Theoretical implications
This study extends the technology acceptance model (TAM) by integrating regulatory compliance, training, and technical support, and peer influence as antecedents of PU, PEOU, and ATT towards the use of MVTHS. The study introduces IL and TDL as direct influencers on ATT and adoption intention, as well as moderators between ATT and the adoption intention of MVTHS. These integrations highlight the importance of contextual and social factors in technology acceptance. The study found that individual understanding of PU, PEOU, and ATT toward technology is not formed in isolation but is influenced by external factors, which could lead to the development of a more comprehensive framework for understanding technology adoption, such as MVTHS. Our findings have established that RC, TTS, PEI, IL, and TDL jointly accounted for 14.9%, 12.9%, and 22.3%, respectively, towards PU, PEOU, and attitudes. Additionally, attitude, along with information and technology literacies, explained about 25.6% of the variance in the adoption intention of MVTHS. These findings provide a theoretical foundation for studies to further validate TAM in the context of metaverse integration into healthcare delivery systems.
Limitations
While this study offers valuable insights into the factors influencing the adoption of MVTHS, several limitations should be acknowledged when interpreting the findings.
Sample generalizability
First, the data for this study were collected in a specific geographical and cultural context (Chinese). The advancement and application of metaverse technology in healthcare may vary significantly across countries due to differences in technological infrastructure, regulatory environments, cultural attitudes toward digital health, and the robustness of the healthcare system. As a result, careful interpretation is necessary when extending these findings to broader or more diverse populations.
Scope of investigated variables
Second, this research did not investigate all potential elements that drive the adoption of metaverse telehealth services. While the study focused on key constructs derived from established technology acceptance theories (e.g., perceived usefulness, perceived ease of use, peer influence), it is impractical for a single study to address every potential determinant.
Research design and causality
Third, this study employed a cross-sectional design, collecting data at a single point in time. While this approach is appropriate for examining relationships between variables, it limits the ability to establish causal direction or assess long-term behavioral patterns. For instance, it is possible that actual use of MVTHS could, over time, influence perceptions of usefulness and ease of use, creating reciprocal relationships that cannot be captured in a cross-sectional design. Furthermore, adoption intentions measured at one point may not reliably predict actual long-term adoption behavior.
Explained variance
Fourth, the relatively low amount of explained variance (R2) observed in this study for certain dependent variables warrants consideration. This suggests that while the model includes significant predictors of MVTHS adoption, there might be additional factors that can influence users’ adoption intentions. The low R2 values may be attributed to the complexity of human decision-making in emerging technology contexts, where uncertainty and lack of prior experience may introduce variability that is difficult to explain with traditional technology acceptance models.
Measurement considerations
Finally, this study relied on self-reported measures for all constructs, which may be subject to common method bias and social desirability effects. Although statistical precautions were taken to minimize these concerns, the reliance on perceptual data means that the findings may not fully align with objective behavioral patterns.
Despite these limitations, this study provides a meaningful foundation for understanding the adoption of MVTHS and offers practical guidance for stakeholders seeking to implement these technologies.
Conclusions and practical implications
This study offers several actionable implications for policymakers, healthcare managers, educators, and future researchers. By understanding the factors that drive the adoption of MVTHS, stakeholders can make informed decisions to facilitate the successful integration of this technology into healthcare systems.
Implications for policy making
Policymakers play a foundational role in creating an environment where MVTHS can thrive safely and equitably. First, it is essential to establish robust regulatory frameworks that ensure user safety, data privacy, and protection against fraud, as these are prerequisites for building trust in new digital health services. Second, to prevent a digital divide in healthcare access, policymakers should advance and fund digital education initiatives at the community level. These programs should specifically target less tech-savvy and vulnerable populations to ensure that all citizens can acquire the necessary skills to benefit from MVTHS.
Implications for healthcare management
For healthcare administrators and managers, the findings underscore the need to address both the technical and social dimensions of MVTHS adoption. First, marketing strategies should focus on enhancing perceived value and trust. This can be achieved by disseminating success stories and peer testimonials that demonstrate the tangible benefits and positive patient outcomes associated with MVTHS. Second, managers must prioritize the development of comprehensive training programs. These programs should be tailored to the needs of different user groups, particularly patients with lower digital literacy, to build their proficiency and confidence in using the platforms effectively.
Implications for education
Educators and healthcare trainers should integrate modules on digital health literacy into their curricula for both healthcare professionals and patients. For medical and nursing students, training should include hands-on experience with MVTH platforms to prepare them for the future of healthcare delivery. For patient education, healthcare providers should develop accessible learning materials and workshops that demystify the technology, emphasizing its ease of use and the improved access to care it provides.
Implications for future research
While this study provides valuable insights, several avenues for future investigation remain. Researchers are encouraged to conduct longitudinal studies to examine how user perceptions and adoption intentions evolve as they gain more experience with MVTHS. Additionally, comparative studies across different cultural and socioeconomic contexts would help determine whether the drivers of adoption identified here are universal or context-dependent. Also, future research could explore the potential negative outcomes of MVTH adoption, such as technology fatigue or the depersonalization of patient-provider interactions, to provide a more holistic understanding of its impact. It is further recommended that future research disaggregate specific metaverse features (e.g., VR immersion, avatar interaction, haptic feedback) to examine their differential effects on user acceptance. We finally suggest that subsequent studies test whether attitude partially or fully mediates relationships between RC, TTS, PEI, and adoption intention.
Supplemental material
Supplemental material -Metaverse-driven telehealth services adoption in China: The role of regulatory compliance, training and technical support, peer influence and literacy determinants in an extended technology acceptance model
Supplemental material -Metaverse-driven telehealth services adoption in China: The role of regulatory compliance, training and technical support, peer influence and literacy determinants in an extended technology acceptance model by Isaac Kofi Mensah, Deborah Simon Mwakapesa and Muhammad Khalil Khan in DIGITAL HEALTH.
Footnotes
Ethical considerations
This study follows the institutional guidelines and the 2024 Declaration of Helsinki Ethical standards. Ethical approval (No. NTU-IRB24-SML05) was granted by the Institutional Review Board (IRB) of NingboTech University, China.
Consent to participate
Written informed consent was obtained from all the participants.
Author contributions
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by the High-Level Talent Introduction Program and Hubei Private Enterprise Innovation and Development Research Center (HPEIDRC) of Wuhan College.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The raw data will be available to the corresponding author on reasonable request.
Supplemental material
Supplemental material for this article is available online.
