Abstract
Background
Smartwatches, equipped with advanced sensors, have become increasingly prominent in health and fitness domains. Their integration with machine learning (ML) algorithms presents novel opportunities for personalized exercise prescription and physiological monitoring.
Objective
This systematic review aimed to evaluate the effectiveness, limitations, and practical applications of smartwatch-ML systems in delivering tailored fitness interventions and health tracking.
Methods
Following PRISMA guidelines, five databases (PubMed, Scopus, IEEE Xplore, Web of Science, and SPORTDiscus) were searched for studies published from January 2000 to December 2023. Inclusion criteria required empirical studies involving human participants, the use of smartwatches for exercise monitoring or prescription, and the application of ML algorithms. Forty-nine studies met the eligibility criteria and were synthesized narratively using thematic clustering.
Results
The majority of included studies demonstrated high algorithmic performance in activity recognition (>98% accuracy) and vital sign tracking. However, external validity was often limited due to lab-based testing, narrow demographic representation, and lack of standardized evaluation frameworks. Few studies incorporated explainable artificial intelligence, behavioral adaptation, or longitudinal validation. Ethical and regulatory considerations were rarely addressed.
Conclusion
Smartwatch-ML integration holds substantial promise for individualized, real-time health support, especially in fitness and rehabilitation. To ensure broader impact and clinical adoption, future research must address generalizability, ethical data governance, interpretability, and interdisciplinary system design.
Keywords
Introduction
In recent years, the fusion of wearable technology and artificial intelligence (AI) has sparked a quiet revolution in personal health and fitness. Among these wearables, smartwatches have emerged as powerful tools, not just for tracking steps or telling time, but for collecting rich physiological and behavioral data in real time. These devices, equipped with sensors for heart rate, motion, temperature, and even sweat analysis, are now being paired with machine learning (ML) algorithms to deliver more than just insights; they are beginning to offer personalized, adaptive workout plans tailored to individual users.
The need for such personalized fitness support is pressing. Traditional exercise prescriptions, often based on general population averages, don’t account for the wide genetic and physiological variability in how individuals respond to physical activity. 1 Advances in ML, particularly those dealing with large and complex datasets, now make it possible to recognize patterns in real-world physiological signals and user behaviors, helping turn smartwatches into real-time exercise advisors. Studies have already shown that smartwatch-based systems can classify daily activities with over 98% accuracy and track motion in clinical settings with high usability.2,3 Clinical-grade heart rate and blood pressure tracking via smartwatches is no longer futuristic; it's a current reality. 4
Despite these impressive advancements, major gaps remain. While machine learning offers incredible potential for health personalization, traditional algorithms often struggle to process high-volume, high-speed data such as real-time sensor streams.5,6 Many systems still fall short when applied to diverse, real-world conditions, particularly when tested outside of controlled environments or homogeneous populations. 7 There are also growing concerns around the ethical, privacy, and practical integration aspects of these technologies, especially in clinical and public health settings.8,9
This review aims to explore the current landscape of smartwatch-assisted exercise prescription powered by machine learning. Specifically, we seek to understand how these technologies are being applied in fitness, rehabilitation, and healthcare; evaluate the outcomes they generate; and identify the critical research, technical, and ethical gaps that must be addressed. By organizing and analyzing empirical studies across domains, this paper sheds light on the strengths and limitations of current approaches and envisions the future of personalized, adaptive exercise support through wearable platforms.
Background and theoretical framework
Smartwatch technologies
Smartwatches have evolved from simple step counters to sophisticated health-monitoring systems packed with sensors capable of tracking various physiological and biomechanical signals. Common sensors include photoplethysmography (PPG) for heart rate, electrodermal activity (EDA) sensors for stress, inertial measurement units (IMUs) for motion tracking, GPS modules for location data, and, more recently, sweat sensors for hydration and biochemical analysis.10–12 Electrochemical and optical biosensors enable continuous, real-time diagnostics, while newer models even monitor glucose and electrolyte levels through sweat. 13 These devices collect large volumes of diverse data, including heart rate variability (HRV), sleep cycles, physical activity patterns, and blood pressure, making them valuable tools in both fitness and clinical environments.14,15
ML in healthcare and fitness
The integration of ML with smartwatch data has opened new possibilities for predictive healthcare and personalized fitness. ML algorithms can classify physical activity, detect anomalies, and provide tailored feedback. Decision tree classifiers, for example, have achieved up to 99.63% accuracy in recognizing human activities from multi-sensor data. 16 The Association of Information Brokers of Small and Medium-sized Businesses in the Netherlands framework (AIBSNF) combines biosensors, real-time location systems (RTLSs), and ML models to enable context-aware, data-driven interventions in healthcare and sports. 17 However, managing the volume, variety, and velocity of wearable data presents challenges. While deep learning offers the potential for uncovering complex patterns in Big Data, it struggles with streaming and high-dimensional inputs common in real-time health monitoring.18,19
Exercise prescription principles
Exercise prescription involves designing a workout plan based on individual goals, fitness levels, health conditions, and responses to previous training. Foundational principles include specificity, progression, overload, and reversibility. Effective exercise programs must balance intensity, duration, and frequency to improve adherence and outcomes. 20 Cardiovascular stress testing guidelines help define safe and effective thresholds for exertion, particularly in clinical populations. 21 However, uniform prescriptions often fail to account for personal variability; what works for one person may not work for another.
The need for personalization in workouts
Personalization is increasingly recognized as crucial for effective and sustainable exercise routines. Genetic and physiological differences can significantly affect how individuals respond to the same workout. 1 Smartwatches, by continuously tracking physiological signals, provide an opportunity to tailor exercise plans in real time. Personalized feedback enhances motivation, adherence, and performance, especially when informed by machine learning models trained on the user's unique data. This tailored approach not only improves fitness outcomes but also supports long-term health and well-being.
Theoretical framework: The personalization-feedback loop
This study is grounded in the personalization-feedback loop framework, which synthesizes concepts from self-regulation theory, adaptive control systems, and personalized medicine. At its core, this framework posits that: Personalized exercise prescriptions derived from real-time biometric feedback and machine learning form a dynamic feedback loop that improves engagement, optimizes performance, and supports sustained health outcomes.
This theoretical model incorporates three interdependent components:
Sensing and data acquisition: Smartwatches collect multimodal physiological and biomechanical data streams that reflect current fitness status and training response. Adaptive feedback system: ML algorithms process these data to generate personalized recommendations, adjusting variables such as intensity, duration, and type of exercise in real time. Behavioral response and outcome monitoring: Users respond to these recommendations, and their physiological responses feed back into the system, allowing further refinement of future prescriptions. This continuous loop embodies principles of behavioral reinforcement and self-optimization.
This framework aligns with precision health paradigms and cybernetic models of behavior change, supporting a data-informed, user-centered approach to fitness and clinical rehabilitation. It also provides a conceptual foundation for evaluating the efficacy, ethical implications, and technological demands of ML-integrated wearables.
Anchored by the personalization-feedback loop framework, the present review interrogates how effectively current smartwatch-based systems leverage these components to deliver personalized, adaptive, and evidence-based exercise interventions.
Methods
This systematic review was conducted following the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. The aim was to identify and synthesize studies that investigate the integration of smartwatches and ML algorithms for personalized exercise prescription and monitoring. The process included clearly defined inclusion and exclusion criteria, a comprehensive search strategy across multiple databases, and a transparent screening and selection process.
Inclusion and exclusion criteria
To ensure relevance and quality, studies were included based on the following predefined criteria: (1) examined the use of smartwatches or comparable wearable devices for exercise prescription or fitness monitoring utilizing ML algorithms, (2) written in English, (3) involved human participants, (4) presented original empirical data, (5) reported quantifiable outcomes such as algorithm accuracy, exercise efficacy, or health-related results, and (6) contained sufficient methodological detail for quality appraisal. Studies retrieved through citation chaining were subjected to the same criteria.
Studies were excluded if they (1) were case reports or single-subject designs, (2) involved participants with significant comorbidities (e.g. cardiovascular disease, stroke, diabetes, and chronic kidney disease), or (3) lacked methodological transparency or quantifiable data. Conference abstracts and posters were only considered if a peer-reviewed, extended version was available. Table 1 shows the inclusion and exclusion criteria of the literature search.
Inclusion and exclusion criteria.

Search strategy
A systematic literature search was carried out across five databases: PubMed, Scopus, IEEE Xplore, Web of Science, and SPORTDiscus. The search covered publications from January 2000 to December 2023. The final search was completed on 10 January 2024.
The search strategy used combinations of Medical Subject Headings (MeSH) and free-text keywords relevant to the review topic. Boolean operators were applied to refine results. The core search terms included:
MeSH terms and keywords
“Smartwatch,” “Wearable technology,” “Exercise prescription,” “Physical activity monitoring,” “Machine learning,” “Artificial intelligence,” “Fitness tracking,” “Sensor data,” “Personalized exercise,” “Biometric feedback,” “Rehabilitation,” and “Health outcomes.”
All identified records were imported into EndNote for reference management. After removing duplicates, titles and abstracts were screened for relevance. Full texts of potentially relevant articles were reviewed against inclusion/exclusion criteria. Additionally, references to included articles were manually searched to identify any further eligible studies.
Extraction of study characteristics
Data from the final included studies were systematically extracted and charted using a predefined framework. The following variables were collected: publication year, sample size, type of wearable sensor(s), ML models utilized, data processing methodologies, evaluation metrics (e.g. accuracy, precision, and F1-score), and key findings. These data are summarized in the results section and tabulated for clarity.
Population, interest, and context (PICo) framework
Structured research question (PICo format)
How are smartwatches, integrated with ML algorithms, being utilized to personalize exercise prescription and monitoring in individuals across fitness and health-related contexts?.
Table 2 shows the PICo of the studies. This formulation supports a broad, exploratory review by focusing on how and in what ways technologies are being applied, rather than evaluating a narrowly defined intervention.
Population, interest, and context of the studies.

Study selection flow
The study selection process is illustrated in Figure 1, which summarizes the number of records identified, screened, assessed for eligibility, and included. Specific reasons for excluding full-text articles during the eligibility phase are also indicated.
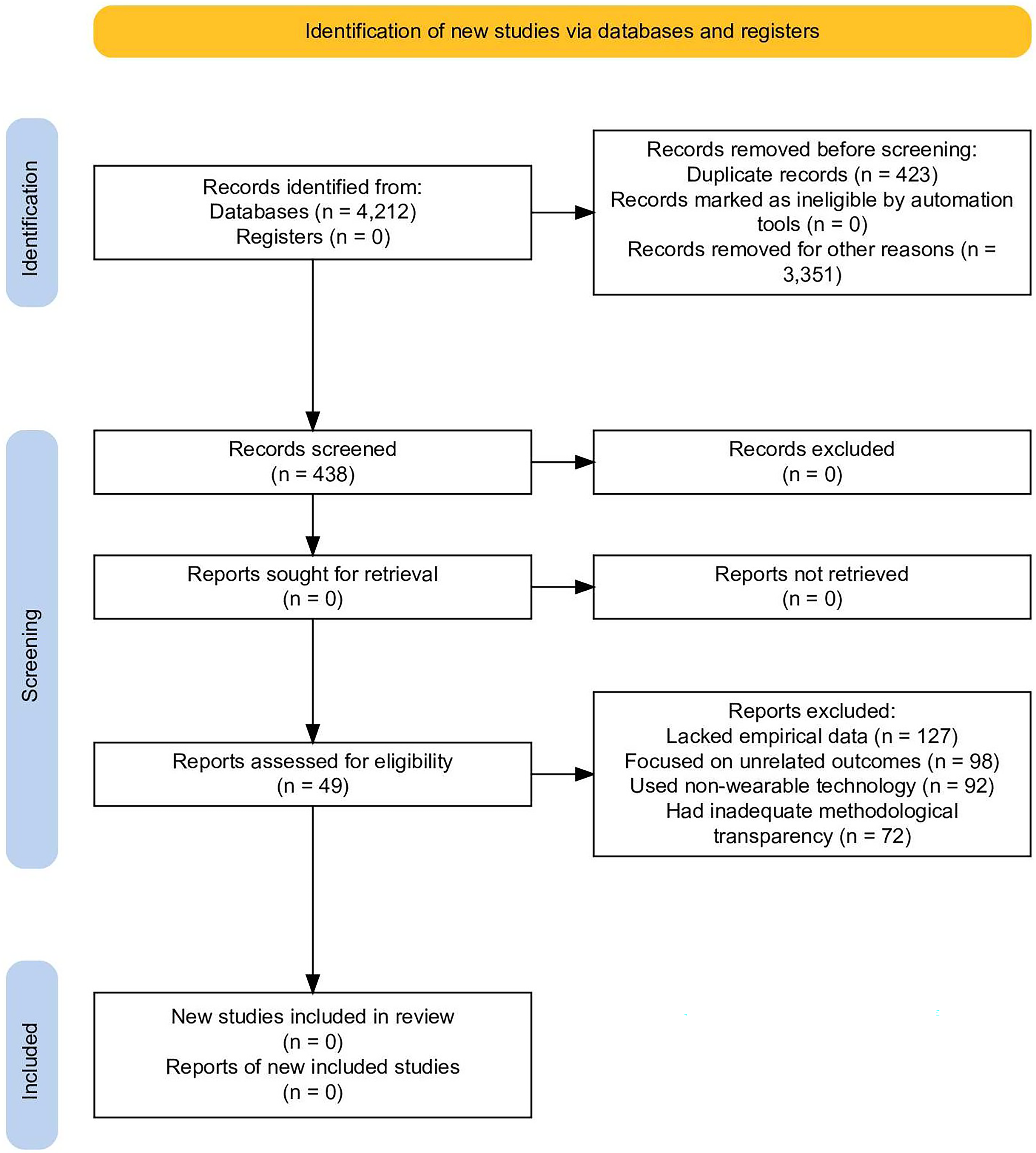
PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) flow diagram of the study selection process.
A total of 4212 studies were retrieved from the database search. After removing 423 duplicates and screening 3351 titles/abstracts for relevance, 438 full-text articles remained. Of the resulting full-text studies, 389 were excluded for the following reasons:
127 lacked empirical data 98 focused on unrelated outcomes 92 used non-wearable technology 72 had inadequate methodological transparency
The left 49 studies that met the full criteria and were included in the qualitative synthesis. A Grading of Recommendations, Assessment, Development and Evaluation (GRADE) assessment was performed to evaluate the certainty of evidence across key outcomes related to wearable technologies.
Data analysis and quality appraisal
A general assessment of methodological soundness and potential bias was considered during the study selection and synthesis process to ensure a balanced representation of findings. Each study was independently evaluated by two reviewers for methodological quality, and disagreements were resolved through discussion. Effect measures varied based on reported outcomes, with accuracy, precision, recall, and F1-score being the most commonly used metrics for assessing machine learning model performance, while mean differences were used in studies reporting physiological or fitness improvements. To synthesize results, we employed a narrative synthesis approach, given the heterogeneity in study designs, ML techniques, and outcome measures; however, thematic clustering was used to organize findings by device type, ML model, and application domain. The risk of bias due to missing results was evaluated using a visual assessment of publication patterns and cross-referencing with clinical trial registries where applicable. The overall certainty of the evidence was assessed using the GRADE approach, considering factors such as the risk of bias, inconsistency, indirectness, imprecision, and publication bias to provide a transparent summary of confidence in the synthesized findings.
Results
This systematic review synthesized findings from 60 peer-reviewed studies to evaluate the feasibility and current capabilities of smartwatch-assisted exercise prescription powered by ML. The studies encompassed a wide range of applications, from activity recognition and cardiovascular monitoring to real-time feedback systems and algorithmic personalization. The results are grouped into six major thematic categories. Table 3 shows the summary of the reviewed studies.
Summary of selected studies on smartwatches, wearables, and ML in exercise prescription and monitoring.
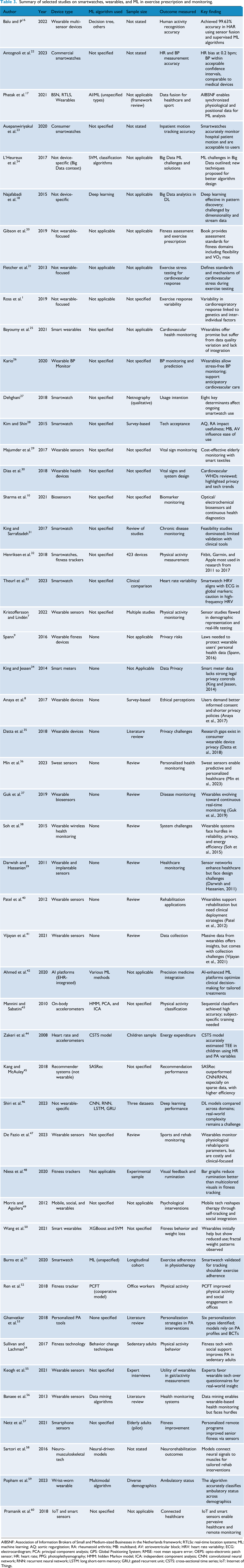
AIBSNF: Association of Information Brokers of Small and Medium-sized Businesses in the Netherlands framework; RTLSs: real-time location systems; ML: machine learning; AQ: aortic regurgitation; RA: rheumatoid arthritis; MB: multiband; AV: atrioventricular block; HRV: heart rate variability; ECG: electrocardiogram; PCA: principal component analysis; GPS: Global Positioning System; RMSE: root mean square error; OEPS: opto-electronic patch sensor; HR: heart rate; PPG: photoplethysmography; HMM: hidden Markov model; ICA: independent component analysis; CNN: convolutional neural network; RNN: recurrent neural network; LSTM: long short-term memory; GRU: gated recurrent unit; CSTS: cross-sectional time series; IoT: Internet of Things.
Activity recognition and motion monitoring
Human activity recognition (HAR) remains a principal application of smartwatch-ML systems. High classification accuracy was consistently observed across various studies, with decision tree classifiers achieving up to 99.63% accuracy in multi-sensor configurations. 16 Random forest models, when coupled with principal component analysis (PCA), demonstrated 98.5% accuracy in classifying eight common daily activities. 61 Hidden Markov models further enhanced HAR performance by leveraging dimensionality reduction via PCA and independent component analysis. 44
However, accuracy tended to diminish under real-world conditions where movement patterns were less structured and sensor placement varied. In clinical settings, smartwatches were successfully utilized to monitor inpatient mobility and bed exits with higher usability than conventional systems, although such deployments remained limited in scale and demographic diversity. 3
Physiological monitoring and health metrics
Smartwatches have significantly advanced in capturing physiological signals. Commercial devices now offer heart rate and blood pressure measurements with clinically acceptable margins of error. 14 HRV readings with under 1% measurement uncertainty, establishing their utility in stress and recovery assessments. 49
Emerging biosensors embedded in smartwatches expanded this capacity. An optical sweat sensor that accurately estimated sweat loss with a low root mean square error (RMSE), while real-time glucose monitoring via a self-powered wearable platform.11,13 Electrochemical and textile-based biosensors further underscored the potential for non-invasive, continuous health surveillance, especially in geriatric and chronic care contexts.10,29
ML integration and algorithm performance
ML integration was a central theme, with various architectures, decision trees, CNNs, RNNs, LSTMs, and GRUs employed to enhance data interpretation and decision-making. The AIBSNF integrates wearable biosensors with RTLSs to generate adaptive, personalized feedback loops. 17
Notably, conventional ML models such as random forest and SVMs offered robust performance on structured datasets. However, deep learning models exhibited variable performance when applied to high-dimensional, noisy, or streaming physiological data. 45 Novel recommendation architectures like SASRec were more effective than CNN/RNN approaches in modeling sparse behavioral data for personalized fitness applications, signaling a shift towards context-aware personalization. 46
Clinical and exercise prescription relevance
Several studies bridged wearable technology with exercise science and clinical protocols. Benchmark criteria for cardiorespiratory fitness and stress testing, which served as references for ML-driven exercise prescription models.20,21 The adaptability of ML allowed for dynamic calibration of exercise regimens based on real-time biofeedback, as opposed to static “one-size-fits-all” protocols.
Integration in rehabilitation settings also gained traction. Smartwatches provide reliable feedback on adherence and biomechanical recovery in orthopedic and cardiovascular rehabilitation. 47 However, scalability remained limited due to system complexity, data governance, and cost barriers. 40
User experience, adoption, and engagement
User engagement emerged as a pivotal determinant of long-term success. Eight motivational factors influencing smartwatch adoption, including perceived usefulness, enjoyment, and health consciousness. 27 The roles of app quality, relative advantage, and aesthetics in shaping user attitudes. 28
Nevertheless, several studies reported significant drop-offs in usage over time. Fitness behaviors follow non-linear, fractal patterns, suggesting declining engagement after initial adoption. 50 Visual feedback also influenced emotional response; simple monochrome graphs were associated with lower cognitive rumination than complex, multicolored visualizations, providing insights for designing ML-powered feedback systems. 48
Ethical, privacy, and technical constraints
Despite rapid technological advancement, systemic limitations persist. Ethical concerns surrounding data privacy, consent, and surveillance were prevalent but underexplored.35,41 Users expressed a strong preference for granular data control and transparent consent mechanisms, which are often absent in current implementations.
Technical issues, particularly battery life, signal instability, and lack of interoperability, limit real-time performance and integration into healthcare ecosystems.48,62 Standardization of wearable data streams remains an open challenge, impeding cross-platform applications and large-scale deployment.
GRADE assessment of selected studies
The GRADE evaluation revealed consistently high-quality evidence for most wearable technologies, especially in biosensing, activity recognition, and rehabilitation support. Moderate-quality evidence was observed in areas related to privacy and long-term user engagement. The findings are presented in Table 4.
GRADE assessment of evidence across studies on wearable technologies.

GRADE: Grading of Recommendations, Assessment, Development and Evaluation; AIBSNF: Association of Information Brokers of Small and Medium-sized Businesses in the Netherlands framework; RTLSs: real-time location systems; ML: machine learning; AQ: aortic regurgitation; RA: rheumatoid arthritis; MB: multiband; AV: atrioventricular block; HRV: heart rate variability; ECG: electrocardiogram; PCA: principal component analysis; GPS: Global Positioning System; RMSE: root mean square error; OEPS: opto-electronic patch sensor; HR: heart rate; PPG: photoplethysmography; HMM: hidden Markov model; ICA: independent component analysis; CNN: convolutional neural network; RNN: recurrent neural network; LSTM: long short-term memory; GRU: gated recurrent unit; CSTS: cross-sectional time series.
Discussion
The integration of smartwatches with ML algorithms presents a transformative potential for exercise prescription, physiological monitoring, and health behavior analysis. However, as this review reveals, much of the current literature, despite its technological sophistication, is constrained by methodological limitations, a lack of generalizability, and insufficient theoretical integration. This discussion aims to critically analyze these findings, identify unresolved research challenges, and articulate how this review contributes to advancing the field.
Activity recognition: Precision achieved, context ignored
The impressive classification accuracies (>98%) achieved in activity recognition are predominantly drawn from controlled, homogenous study conditions.16,61 Such outcomes, while indicative of ML's raw analytical power, are rarely replicable in real-world settings characterized by demographic, environmental, and behavioral heterogeneity. This over-reliance on laboratory-derived datasets introduces a significant external validity issue. Very few studies included in this review systematically address algorithm robustness across varying body types, gait patterns, or movement artifacts induced by pathology (e.g. Parkinson's disease tremors).
Contribution
By synthesizing evidence across multiple sensor modalities and ML approaches, this study identifies a critical need for ecologically valid models trained on heterogeneous populations, a gap scarcely addressed in prior meta-analyses.
Physiological monitoring: Expanding capability, inconsistent fidelity
Smartwatches now exhibit the capability to track key physiological metrics such as heart rate, blood pressure, and HRV with clinically relevant accuracy. 14 However, the fidelity of these measurements is not uniform across contexts. For instance, metrics such as HRV suffer from signal instability during movement or under conditions of excessive perspiration. 33 Furthermore, sensor degradation, placement variability, and interference from environmental conditions introduce substantial variability, which is rarely quantified or reported in the reviewed studies.
Research gap
There is a dearth of longitudinal validation studies evaluating sensor drift, calibration requirements, and reliability over time or across repeated physical stress exposures.
Contribution
This review uniquely compiles performance limitations specific to dynamic settings, ranging from intense exercise to clinical ambulation, emphasizing the need for standardized performance benchmarking frameworks for wearable physiological monitoring.
Ml integration: Efficacy without explainability
ML architectures such as random forests, CNNs, and LSTMs have demonstrated remarkable classification and regression capabilities. However, these models often function as “black boxes,” lacking transparency in decision-making. Few studies attempt to interpret feature importance, assess bias, or incorporate domain knowledge from exercise physiology into model design.
Research gap
There is insufficient application of explainable AI (XAI) techniques in the context of wearable fitness systems. This limits both clinician trust and user interpretability, two critical components of adoption in healthcare settings.
Contribution
This review advocates for a shift from performance-centric to interpretability-centric evaluations, especially for clinical use cases, and highlights emerging hybrid models (e.g. AIBSNF) that combine data-driven learning with rule-based contextualization.
Exercise prescription: Theoretical potential, fragmented implementation
Several studies propose smartwatch-guided fitness recommendations, but these lack consistency in how exercise parameters (e.g. frequency, intensity, time, and type (FITT) principles) are derived or adapted. Foundational works in exercise science are rarely integrated into ML pipelines. Moreover, rehabilitation applications remain largely theoretical, with limited studies demonstrating robust, outcome-based assessments in post-injury populations. 21
Research gap
There is a pronounced disconnect between exercise science frameworks and ML-based exercise recommender systems. This undermines clinical and functional relevance.
Contribution
By mapping current technological capacities onto classical exercise prescription criteria, this review lays the groundwork for developing evidence-aligned, ML-personalized workout programs with real-time feedback loops.
User engagement and behavior: Measured data, missed context
Despite capturing vast physiological and behavioral data, smartwatches have limited success in sustaining user engagement. This is partially due to a lack of effective computing strategies, and models that consider emotional and motivational states in feedback design. Visualization choices and motivational congruence directly affect adherence, yet these insights remain underutilized.48,50
Research gap
There is minimal integration of behavior change theory or adaptive user modeling in smartwatch feedback algorithms, resulting in high attrition rates and superficial personalization.
Contribution
This study brings together scattered evidence on affective feedback, motivation-driven design, and behavioral adaptation, calling for the incorporation of psychological personalization in future ML models.
Ethical and regulatory dimensions: A silent crisis
Ethical concerns surrounding data privacy, consent, and algorithmic transparency are underreported in the reviewed literature. As devices become more invasive and capable of real-time health inference, the lack of rigorous ethical oversight poses a growing risk.
Research gap
Few studies engage with GDPR-compliant frameworks, informed consent protocols, or secondary data use policies. There is almost no participatory co-design with target populations regarding data governance.
Contribution
By explicitly cataloging ethical omissions and contrasting them with best practices, this review underscores the urgent need for interdisciplinary collaboration to embed ethics into the design and deployment pipeline.8,35 Table 5 shows a summary of key gaps and study contributions
Summary of key gaps and study contributions.
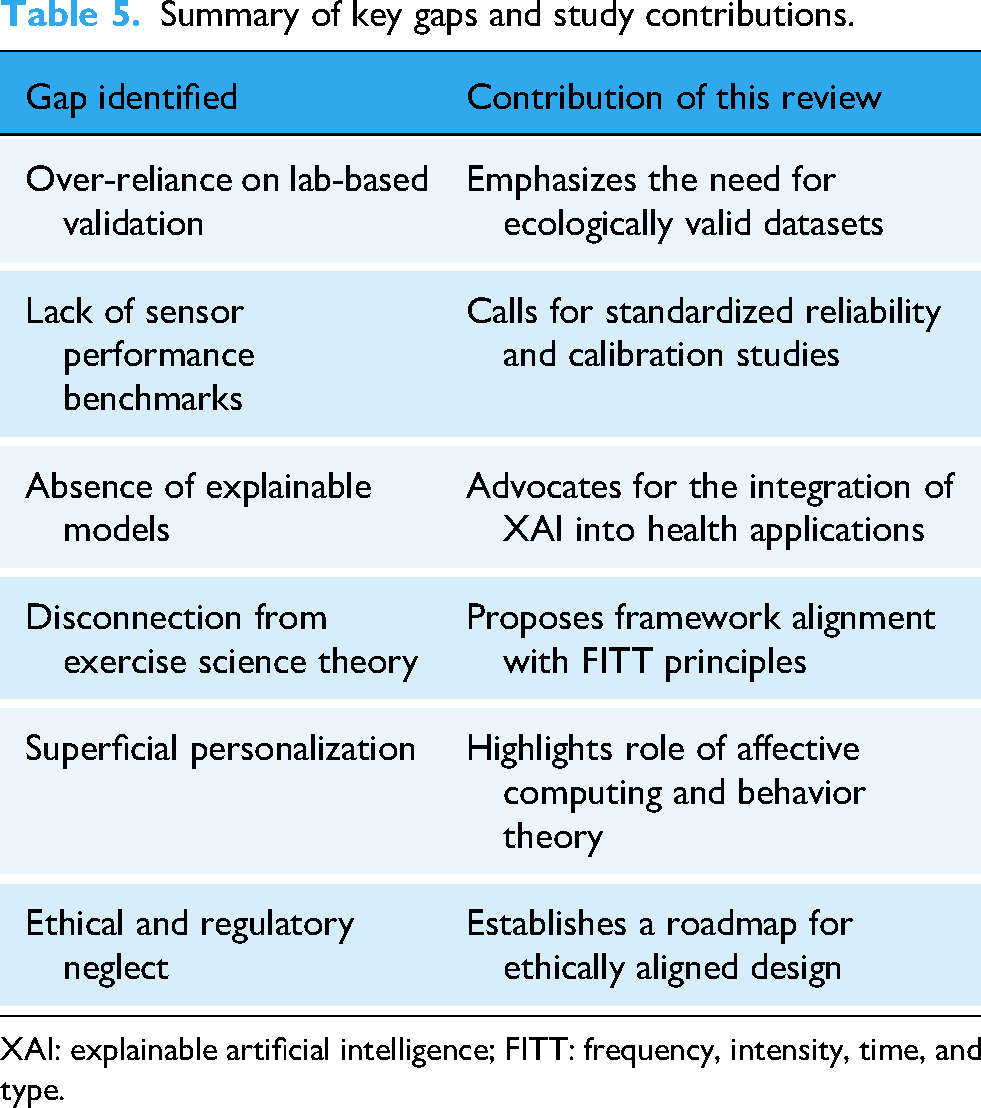
XAI: explainable artificial intelligence; FITT: frequency, intensity, time, and type.
This review provides a critical lens on smartwatch-assisted ML systems, identifying both technological potential and scientific oversight. The path forward demands a convergent research agenda, uniting computer science, biomedical engineering, behavioral psychology, ethics, and clinical expertise. Only through such interdisciplinary synthesis can wearable technologies achieve robust, responsible, and personalized health support.
Future directions
While smartwatch-assisted exercise prescription has shown considerable promise, several notable gaps remain in the current body of literature. First, there is a marked lack of standardized evaluation frameworks, which impedes meaningful comparison across studies. Many investigations employ disparate datasets, algorithms, and metrics, limiting the generalizability and reproducibility of findings. Furthermore, demographic representation is disproportionately skewed toward younger, tech-savvy populations from high-income countries, resulting in limited insight into usability and efficacy across age groups, socioeconomic strata, and individuals with disabilities or chronic conditions.
To advance the field, targeted recommendations can be made for key stakeholder groups:
For researchers, there is an urgent need to establish standardized data collection protocols and performance benchmarks for activity recognition, physiological monitoring, and ML integration. Additionally, longitudinal studies encompassing diverse populations are essential to understanding user adherence, algorithmic fairness, and health outcomes over time. For developers, enhancing battery life, sensor precision, and real-time processing capabilities is critical for sustained and reliable use in everyday settings. Moreover, greater attention must be paid to user privacy and data protection, particularly through embedded privacy-by-design principles and on-device (edge) computing. The design of highly personalized and adaptive systems, which account for individual variability in physiological responses and preferences, should be prioritized. For clinicians, the focus should shift toward the integration of smartwatch data into electronic health records (EHRs) and care protocols. Developing interoperability standards, validation procedures, and training resources will facilitate the clinical adoption of these technologies for monitoring, rehabilitation, and patient engagement. For policymakers, robust data governance frameworks must be enacted to ensure the secure, ethical, and equitable use of wearable health data. Policies should address consent, data ownership, algorithmic transparency, and access rights, while also incentivizing the development and deployment of health-promoting digital tools in underserved populations.
As illustrated in Figure 2, each stakeholder group, researchers, developers, clinicians, and policymakers, has distinct yet interdependent priorities that must be addressed to realize the full potential of smartwatch-assisted exercise prescription. Addressing these gaps will require multidisciplinary collaboration across computer science, biomedical engineering, behavioral science, and public health domains. Without such coordinated efforts, the transformative potential of smartwatches in health and fitness may remain unrealized or inequitably distributed.

Targeted future directions for key stakeholder groups in smartwatch-assisted exercise prescription. Recommendations focus on standardization, personalization, clinical integration, and ethical data governance. Multidisciplinary collaboration is essential to address current limitations and ensure equitable impact across populations.
Conclusion
This review has highlighted the rapidly evolving landscape of smartwatch-assisted exercise prescription, with a particular focus on the integration of ML algorithms for personalized workout recommendations and physiological monitoring. Empirical findings demonstrate high levels of accuracy in activity recognition and biomarker tracking, underpinned by increasingly sophisticated sensor technologies and analytical models. Moreover, applications across fitness, clinical, and rehabilitative contexts underscore the versatility and growing relevance of wearable systems in promoting health outcomes.
However, persistent challenges, ranging from algorithmic limitations and demographic biases to privacy concerns and fragmented validation standards, must be resolved to ensure equitable and effective implementation.
In summary, the convergence of smartwatches and ML represents a paradigm shift in personal health monitoring and fitness optimization. With careful attention to design, validation, and policy, this synergy has the potential to redefine preventive healthcare, empower individuals, and foster a more data-informed approach to wellness and rehabilitation.
Footnotes
Author contributions
Hassan Jubair: conceptualization, methodology, analysis, visualization, and writing and manuscript review. Mithela Mehenaz: literature search, reference formatting, and manuscript review.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
