Abstract
Objective
Increasing the physical activity of frail, older patients before surgery through prehabilitation (prehab) can hasten return to autonomy and reduce complications postoperatively. However, prehab participation is low in the clinical setting. In this study, we re-design an existing prehab smartphone application (BeFitMe™) using a novel standalone Apple Watch platform to increase accessibility and usability for vulnerable patients.
Methods
Design Science Research Methodology was used to (1) develop an approach to clinical research using standalone Apple Watches, (2) re-design BeFitMe™ for the Apple Watch platform, and (3) incorporate user feedback into app design. In phase 3, beta and user testers gave feedback via a follow-up phone call. Exercise data was extracted from the watch after testing. Descriptive statistics were used to summarize accessibility and usability.
Results
BeFitMe™ was redesigned for the Apple Watch with full functionality without requiring patients to have an iPhone or internet connectivity and the ability to passively collect exercise data without patient interaction. Three study staff participated in beta testing over 3 weeks. Six randomly chosen thoracic surgery patients participated in user testing over 12 weeks. Feedback from beta and user testers was addressed with updated software (versions 1.0–1.10), improved interface and notification schemes, and the development of educational materials used during enrollment. The majority of users (5/6, 83%) participated by responding to at least one notification and data was able to be collected for 54/82 (68%) of the days users had the watches. The amount of data collected in BeFitMe™ Watch app increased from 2/11 (16%) days with the first patient tester to 13/13 (100%) days with the final patient tester.
Conclusions
The BeFitMe™ Watch app is accessible and usable. The BeFitMe™ Watch app may help older patients, particularly those from vulnerable backgrounds with fewer resources, participate in prehab prior to surgery.
Introduction
Frailty is a high-risk factor for older adults undergoing surgery. Frail older adult patients may do better during and after surgery if their frailty is optimized before surgery. 1 The American College of Surgeons and other international societies recommend prehabilitation (prehab) focusing on exercise, nutrition, and social support 2 to mitigate frailty. Prehab has been shown to improve patients’ return to autonomy after surgery, as well as reduce length of stay, postoperative complications, and medical costs.1,3,4
Participation rates in prehab can be as low as 5% to 12% owing to time constraints, transportation barriers, and potential memory difficulties,1,5 and participation rates are likely even lower outside of the clinical trial setting. Technology, such as mHealth apps and wearable devices, can be leveraged to overcome these barriers by providing clear instructions and prompts for physical activity.6,7 While various health interventions utilizing technology have successfully demonstrated feasibility and acceptability,6–11 including among the older adult population,7,9,10 there remain challenges with technology-assisted prehab programs unique to older adults, such as patient confusion with mobile devices, disinterest or lack of confidence in using technology, or lack of designs addressing older patients’ needs. 12
We developed a smartphone application, BeFitMe™, using the behavior change wheel, 13 which has been shown to improve patient access to exercise and support clinicians in providing exercise program management. 9 The app was designed to provide, encourage, and track self-guided at-home exercise for frail older adult patients. The app included behavior-change text messages and exercise videos to increase patient access to resources, and recorded step count and self-reported exercise time (minutes) to support clinicians providing exercise management. However, our preliminary data showed that only 14% (10/70) of patients downloaded the app, with lack of interest, tech savviness, and compatible devices as reasons for not participating. This suggested the need to re-design BeFitMe™ to be more appealing and accessible to older patients in our underserved population (South Side of Chicago).
In this study, we re-designed the BeFitMe™ prehab smartphone application using a novel standalone Apple Watch platform. Apple Watches offer several advantages over a downloadable smartphone app. Apple Watches objectively monitor physical activity levels and provide real-time feedback relating to step-count and accrual of physical activity. 14 Additionally, wearable activity trackers and the behavior change techniques have been shown to increase physical activity in adults. 15 Consumers have positively reported on wearable devices’ ability to help manage personal health, assist with goal setting (such as reaching 5000 steps in a day), and maintain healthy routines.14,16 We hypothesize that the re-designed Apple Watch BeFitMe™ program will increase usability of BeFitMe and the standalone Apple Watch platform will increase accessibility to prehab.
Methods
Methods overview
The Design Science Research Methodology (DSMR) was used 17 (Figure 1). Apple Inc. (Cupertino, CA, USA) provided 100 Apple Watches for this study through its Investigator Support Program. The development of the study followed the six components of the DSMR (1) low participation with BeFitMe app (Identify Problem); (2) developing an approach to increase patient accessibility to prehab using standalone Apple Watches (Define Objectives); (3) re-designing BeFitMe™ for the Apple Watch platform (Design and Development); (4) beta and user testing the BeFitMe Watch application (Demonstration); (5) incorporating user feedback into the BeFitMe™ Watch app design (Evaluation and Adaptation); and (6) presenting findings for future research (Communication). During step 4, Beta testers (study staff) and user testers (patients) provided iterative feedback by responding to a set of standard interview questions facilitated through a follow-up phone call after one week. This study was approved by the University of Chicago Institutional Review Board (IRB21-1318 on 10/18/2021).

The six components of the design science research methodology and the question used as the research entry point to guide the re-design of BeFitMe™ Watch.
Procedure to preparing Apple Watches for reusable clinical use
We received 100 Series 5 Apple Watches from Apple through its Investigator Support Program with WatchOS9 in October 2022. We used one clinic iPhone 8 to set up the 100 watches, and since one Apple ID (‘parent’) can support 5 watches (‘child’), we created 20 Apple IDs with 20 different anonymous emails (Figure 2). We used Google Voice to create 2 phone numbers to support 20 Apple ID accounts (each Apple ID account requires a phone number, and one phone number can be used 15 times). We created ‘child’ anonymous iCloud accounts during the initial watch pairing process using the Apple Watch app on the iPhone. A different ‘child’ anonymous iCloud account was created for each watch (Figure 2).

Set up process and naming scheme for Apple Watches on one iPhone.
BeFitMe™ re-design procedure
During this phase of the study, the study team members worked with a contracted programmer to adapt BeFitMe™ for Apple Watch use over 5 months. Once the BeFitMe Watch app was initially approved for distribution on the App Store, incremental changes and versions were submitted for review to Apple. This requires uploading the new version to Apple and explaining what changes were made. Minor changes usually were approved within 24 h. Once a new version was approved by Apple, it could automatically be updated or manually updated at a time specified by the developer team.
Commercial Apple Watches already collect step count and active minutes; however, the data is not available over a prolonged perioperative period and accessing data requires connection to a parent iPhone. The BeFitMe™ Watch app allows us to collect and store unlimited data and to gather that data without the need for the watch to be paired with an iPhone. This is more cost effective for research and more accessible for patients who may not have an iPhone.
Beta and user testing
This phase of development elicited initial feedback from beta (study staff) and user (patient) participants to identify and address any problems with the BeFitMe™ Watch app re-design. BeFitMe™ Watch app content underwent 8 version upgrade (version 1.0 to version 1.10) based on beta and user feedback. The Ethics Committee of the University of Chicago waived the need for ethics approval and the need to obtain consent for the collection, analysis and publication of the retrospectively obtained and anonymized data for this non-interventional study.
Beta testing was conducted over three weeks with three study staff (S.K., E.D., M.L.M.). The study staff were given a watch and a charger to take home. They were asked to wear the watch daily, log physical activity when prompted by the BeFitMe™ Watch app and communicate any challenges or issues that arose.
Patient users were recruited from the University of Chicago Medicine thoracic surgery clinic from December 2022 to February 2023. Any patient 50 years or older who was having surgery was approached. Every new patient seen in clinic aged 50 or older is screened for frailty using Fried's Frailty Phenotype. 18 Screening consists of survey questions asking about current levels of physical activity, current feelings of tiredness or exhaustion, and weight change over the previous year, a hand grip test, and a gait speed test. The clinical team recommends prehab to any patient prior to surgery who meets the pre-frail or frail criteria. 50% (13/26) of the patients seen in clinic during that time were candidates and 46% (n = 6/13) of those patients agreed to participate. The six consenting patients were given the Apple Watch and a charger to take home in the days leading up to their surgery. Patients are instructed to wear the watch daily and log physical activity when prompted by the BeFitMe™ Watch local notifications. The watch was returned at the patient's postoperative visit, and all the health data collected (days of logged exercise, minutes of exercise, daily step count, pace, and heart rate variability) was saved in the BeFitMe™ cloud server. All patient information was then deleted from the Apple Watch.
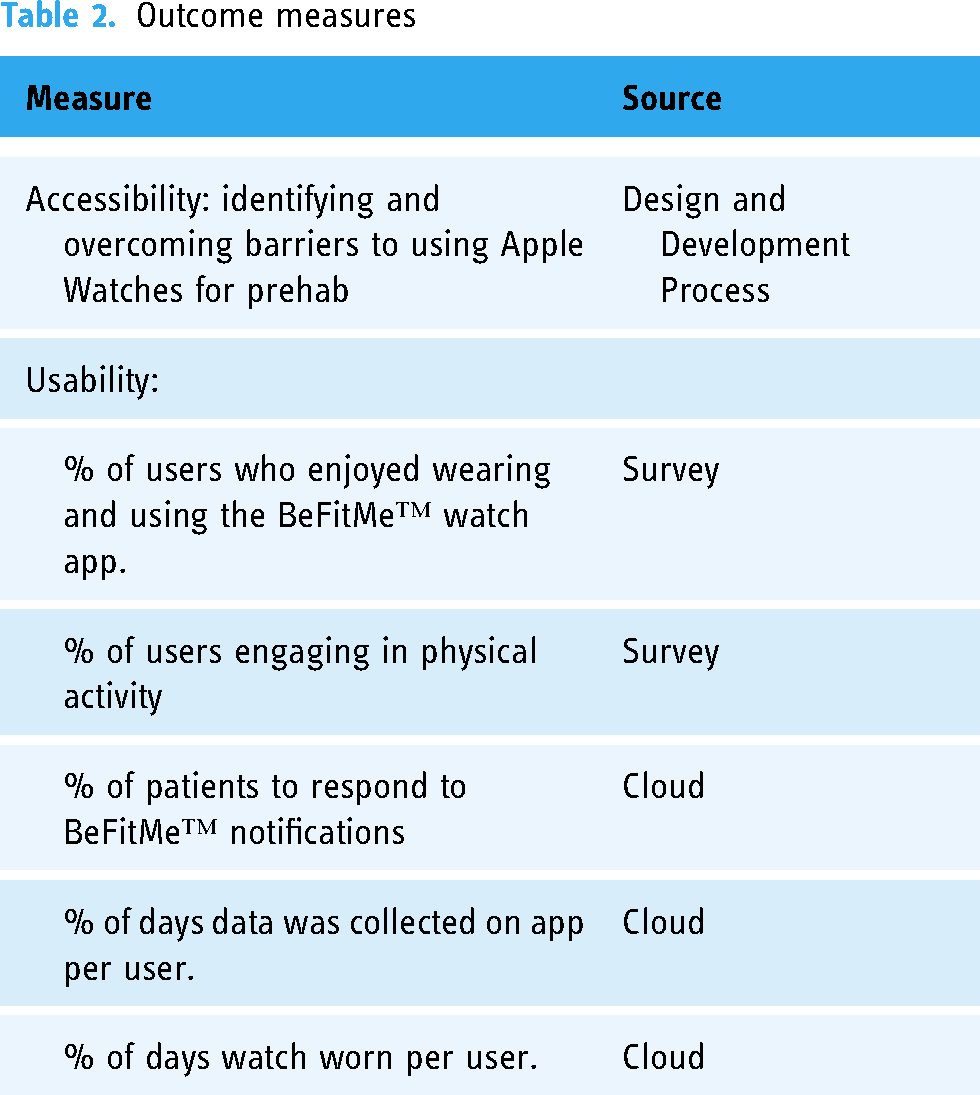
User feedback was collected at 1 week by telephone and then at the follow-up clinic visit. A set of standard questions was asked to every patient (Table 1). The research team extracted a user's exercise data by uploading the data to the BeFitMe™ cloud server upon return of the watch postoperatively. Descriptive statistics were used to summarize patients’ responses to questions on usability and exercise data was gathered from the watch. Outcomes are listed in Table 2.
List of questions asked at one week and at the follow-up visit.

Outcome measures
Results
BeFitMe™ was developed for the standalone Apple Watch platform. The overall process spanned five months. Our team members (E.B. and M.R.) performed software modifications, resulting in a labor-, time- and cost-effective process as detailed below.
Step 1 (1 month): S.K. discovered a cost-effective method to pairing multiple watches with one iPhone, created necessary Apple ID accounts, and began preparing for clinical use. Step 2 (1 month; concurrent with Step 1): E.B. re-designed and recoded BeFitMe™ from the smartphone platform to the Apple Watch platform. Step 3 (1 month): Team members conducted beta-testing and modified software according to beta test results. Each software modification took only 1–2 days to process through Apple's app update review process. Step 4 (3 months): Team members conducted user-testing with patients and embarked on an iterative process involving incorporating user feedback, modifying software, and re-testing.
Developing an approach to clinical research using standalone Apple Watches
The watch pairing process began once all necessary Apple ID accounts were created (Figure 2). During the watch pairing process, restrictions were set on the watch to prevent patients from downloading any apps or making any purchases on the Apple Watch. After the watch is turned on, BeFitMe™ is downloaded onto the watch from the App Store. To download an app on the watch, a passcode must be active. Upon downloading the app, the parent phone must approve the app download. After BeFitMe™ is successfully downloaded onto the watch, we remove the passcode through Settings. The watch face home screen is set to the “Activity Digital” setting which allows highly visible watch complications displaying user steps and activity. The BeFitMe™ Watch app is added as a widget to the home screen in the top left corner and the heart rate app is added as a widget in the top right corner.
There were several challenges to pairing 100 Apple Watches to one iPhone. When pairing Apple Watches with an iPhone, those watches will stay connected to that phone, regardless if a new Apple ID account is used. Consequently, to pair a new set of five watches, the previously paired watches would need to be unpaired, resulting in erasing all data on those watches. To work around this, the iPhone must be factory reset each time before setting up five more watches with the next Apple ID account. Factory resetting the iPhone will unpair previously paired watches without erasing the watches and allow the pairing of five new watches.
To access a previously paired watch on the iPhone, both the phone and watch would need to be factory reset and re-paired after re-logging in with the appropriate ‘parent’ Apple ID account. Pairing the second time is easier, as the ‘parent’ Apple account will recognize the watch as a ‘child’ account, and after re-signing into the ‘child’ account when prompted, the previous ‘child’ account watch face and settings will reload onto the watch.
Another challenge to the pairing process is the need for adequate internet connectivity. The watch must be connected to Wi-Fi during a patient's initial enrollment. In our clinic environment, we experienced challenges with connecting the watches themselves to Wi-Fi due to poor signal and relied on the parent iPhone to connect to the internet – in which case the phone needed to be set to that watch's “parent” ID, leaving only five watches ready for enrollment at any one time. To work around this, once five participants were enrolled, we switched to the next iPhone Apple ID account and paired the next five watches. This limitation could be overcome by using more than one clinic iPhone or operating in a clinic with more stable Wi-Fi connectivity. By identifying and overcoming these barriers to using Apple Watches, we have developed an approach to prehab and clinical research utilizing Apple Watches without the need for a parent iPhone, making prehab more accessible.
BeFitMe™ app re-design
The original BeFitMe™ smartphone app consisted of links to a library of National Institute for Aging (NIA) Go4Life exercise videos, including demonstrations of a warm-up, a 20-min workout, upper body strength training exercises, lower body strength training exercises, and flexibility and balance exercises. Users could access their responses to frailty screening, log physical activity, and view their daily activity data. The smartphone app would send daily, automated behavior-change local notifications to improve patient access to exercise (“Have you performed at least 20 min of exercise today?” and if no, “May we suggest you watch the 20-min exercise videos provided?”). However, this app had low patient uptake partially due to need for smartphone, need to carry smartphone, and need for internet connectivity. Preliminary data from qualitative interviews indicated that a watch platform might be more appealing for patients. We therefore redesigned BeFitMe to function on an Apple Watch platform. BeFitMe™ was redesigned into an Apple Watch app (BeFitMe™ Watch app) to improve patient usability and participation while maintaining core features.
New data collected with the BeFitMe™ Watch app includes heart rate variability and patient app use (e.g., the frequency of interactions with notifications and the time at which activity is logged). Patients can view daily step count, pace, distance, and minutes of exercise in BeFitMe™ Watch app by clicking the “Show My Activity” button (Figure 3).

Befitme™ Watch app patient dashboard. A.) Daily steps; B.) Distance walked; C.) Average active pace; D.) Daily minutes of logged.
The notification schema was also updated on the BeFitMe™ Watch app, from one notification a day to three notifications each day, at 5pm, 5:30pm, and 8pm. The notification asks the patient “Did you do at least 20 min of activity today?” (Figure 4). Upon answering “Yes”, the patient will be prompted to answer, “How many minutes did you exercise today?” with a ± button or stepper that they can use to input the number of minutes. If the patient instead answers “No”, rather than the ability to watch a video demonstration of exercise, a randomly generated exercise recommendation from a list developed based on the NIA Go4Life campaign 19 (Table 3) will appear, as well as a link to the library of NIA Go4Life exercise videos. The patient can either access the video link if connected to the internet or dismiss the notification (Figure 4).

The watch home face screen, notification scheme, and self-report.
List of suggestions BeFitMe™ Watch app offers.

Patients can clear the notification from their home screen by answering the notification, swiping up on the notification (or ignoring), or pressing dismiss. If a patient answers “Yes” to the first notification at 5pm, they will not receive any more notifications. If the patient ignores, dismisses, or answers “No” to the 5pm notification, they will receive the next notification at 5:30pm. If a patient ignores, dismisses, or answers “No” to all three notifications, they can log exercise activity manually in the app from 8pm to 11:59pm (Figure 4). If the patient ignores, dismisses, or answers “No” to all three notifications, step count, pace, and heart rate variability is still gathered passively in the background; however, no data for daily exercise activity will be recorded. The notification scheme restarts at midnight each night.
The greatest challenge in adapting BeFitMe™ to the watch was due to the smaller screen real estate. This was accomplished by casting the watch functionality to that of data collection instead of data presentation that was easily viewable on the phone. All data collection, except for the number of minutes exercised were collected in the background without user interaction. Users’ responses to local notifications triggered the collection of exercise minutes and also the other study data. If a user never responded to an exercise notification, all the other data would be collected as a background task at a set time of day.
To make the app more accessible and to overcome patient barriers with internet connectivity, BeFitMe™ Watch app was programmed where Wi-Fi is not needed for the features of the app to function. The only time when wi-fi is needed is during enrollment and to export user exercise data to a cloud-hosted database upon return of the watch. No protected health information is transmitted or stored on the watch or cloud database.
Beta user testing
We conducted beta testing of BeFitMe™ Watch app with three study staff members (67% (2/3) white, 67% (2/3) female, and age range of 25–68) over three weeks. Clinical experience of the study staff members ranged from research analyst to thoracic surgeon. Beta testing identified several problems with the initial BeFitMe™ Watch app software. For example, early versions would erase participant data between some uses, requiring a participant to be re-enrolled. This was due to an easily fixable coding error. Additionally, the early versions did not allow the team to change a patient's stop date-which controls the notification schemes (i.e., if a patient's stop date passed, the participant will no longer receive notifications).
The BeFitMe™ Watch app notification scheme was also modified. For example, the beta testers said it would be beneficial for a user to have the ability to manually log activity within the app. As a result, in version 1.3, the team added the ability for a participant to manually log activity after the 8pm notification until 11:59pm (Figure 4). The beta tests also allowed us to evaluate how participant responses to notifications would be collected. We learned that if a user does not respond to a notification, then user data would not be collected. This was addressed in version 1.5, which allows BeFitMe™ Watch app to silently upload and save heart and step data with no user actions required. Additionally, beta testers recommended adding exercise suggestions after a patient responded “No” to a notification, which promoted the app developers to create a list of suggestions (Table 3) which would be randomly generated every time a patient responds no to a notification. The problems identified by beta testers were addressed in iterative versions (1.0–1.5) (Table 4).
Updates in each new version of BeFitMe™ Watch app

Patient user testing
We conducted user testing with six thoracic surgery patients (12/02/2022–02/22/2023). Participants were mostly women (67%, 4/6), Black (67%, 4/6), with an average age of 68 (range 58–82). During qualitative interviews, we obtained user feedback on how to make the watch prehab program user-friendly regardless of technology expertise. Feedback about the Apple Watch and the BeFitMe™ Watch app usability and participation in physical activity was collected at 1 week by telephone and again during the patient's postoperative visit using a set of standard questions (Table 1).
When asked about wearing the Apple Watch every day, most patients (5/6, 83%) enjoyed wearing and using the Apple Watch. One patient said, “I really like it and I’m even thinking about getting one myself.” Another patient said, “I haven’t worn a watch in years, so I was worried about wearing this, but it has gone well, and I have been wearing it every day.” When asked about any barriers to wearing the Apple Watch every day, the main barrier patients reported was remembering to wear the watch. Only one patient did not like the watch due to it being unfamiliar.
When asked about using the BeFitMe™ Watch app, the majority of patients (5/6, 83%) said they had engaged with the BeFitMe™ Watch app and half the patients (3/6, 50%) found the BeFitMe™ Watch app notifications to be beneficial reminders to engage in physical activity. When asked about barriers to logging activity in the BeFitMe™ Watch app, three of six patients (50%) reported success in responding the notifications and logging activity daily. The remaining patients (3/6, 50%) experienced difficulties responding to the BeFitMe™ Watch app notifications due to BeFitMe™ app errors and patient unfamiliarity with the Apple Watch notification system. For example, each new version of BeFitMe™ Watch app required a research member to physically update the app on the watch, resulting in patients with older versions experiencing errors with notifications. Ultimately, the majority of patients (5/6, 83%) participated by responding to at least one notification.
When asked about performing daily physical activity and doing prehab, five out of six patients (83%) responded positively to participating in prehab through BeFitMe™ Watch app. One patient said the prehab program was beneficial because she liked how the watch would show step count and felt BeFitMe™ Watch app daily notifications helped remind her to do physical activity, and said, “I can see the benefits of keeping up with things like how I’ve been doing and like how much I walk”. Another patient said, “I can really see the benefit of a doing a program like this”. When asked about the kind of activity they had been doing, most patients reported actively engaging in some physical activity (5/6, 83%), and walking was the most common form of exercise. Only one patient did not complete prehab through BeFitMe™ Watch app due to a general disinterest in doing physical activity and the BeFitMe™ Watch app notifications being “too complicated” to respond to.
Patient user feedback revealed additional limitations to BeFitMe™ Watch app. For example, three patients (50%) felt notifications could be difficult to respond to. One patient did not know how to respond to the BeFitMe™ Watch app notifications and another patient said the notifications disappeared and were difficult to access after. During the check-in phone call with each patient, research staff walked the patients who were having trouble with the notifications through the process of logging activity. Four out of six patients (67%) said that check-in phone call was beneficial and helped them respond to notifications. In response, we developed instructional videos visible on the watch to demonstrate to patients during enrollment how to answer BeFitMe™ notifications, even after they disappear from the home screen. Additionally, the first two patient testers thought that the font was too small and difficult to read. This was consistent with beta testing, and in response, we made the default Apple Watch font larger and bolder, the default sound the loudest, and set the vibration to prominent. The patient feedback received from each phone call allowed for evaluation and adaptations to be made before the next user tester through iterative versions (1.6–1.10) (Table 4).
Extracting patient exercise data
Daily exercise data collected on the watch app is not accessible until the watch was returned, and the patient data cleared from the watch, which automatically saves all data to the BeFitMe™ cloud database. Data is accessed by downloading exercise, heart rate, and pedometer data from the BeFitMe™ website. Data was successfully collected for all beta testers. Data was able to be collected for 54/82 (68%) of the days patients had the watches, including days where a patient did not respond to a notification and health data was recorded silently in the background. When patients did not wear the watch, no data was able to be collected. Patients had the watch for an average of 30 days (SD 13). The amount of data collected in BeFitMe™ Watch app increased over time from 2/11 (16%) days with the first patient tester to 13/13 (100%) days with the final patient tester as versions were updated and patient education was integrated.
Evaluation and adaptation
Beta and user testing showed that the BeFitMe™ Watch app and prehab program are accessible and usable. The feedback received from the beta and user tests allowed the research team to evaluate each version and make appropriate adaptations (Table 4). The three beta testers gave feedback on the initial versions of BeFitMe™ Watch app and the notification scheme and the six user testers gave feedback on the acceptability of wearing an Apple Watch daily and the usability of the BeFitMe™ Watch app. Both beta and user tests gave feedback on the sound and haptics of the Apple Watch and made the watch accessible and useable to the patient population.
Discussion
Principal findings
Our study indicates that a prehab watch app can be developed to encourage older adult prehab prior to thoracic surgery. This study outlines the adapted design and development process of the BeFitMe™ Watch app for the Apple Watch and provides a model for a novel technology-assisted intervention using standalone Apple Watches. By incorporating end-user feedback from our clinicians and vulnerable older adult patient population, we found that the re-designed BeFitMe™ Watch app was more user-friendly and increased patient engagement through daily reminders and notifications to log activity. Added functionality such as the ability to view daily step count and minutes of exercise performed enabled patients to see their own progress through the prehab program.
We anticipate that developing the BeFitMe™ Watch app to function on the Apple Watch without the need for internet connectivity or an iPhone will allow us to increase accessibility and equity for patients, particularly the vulnerable population we serve living in the South Side of Chicago where up to 40% of households lack adequate internet connectivity. 20 Minority groups and people with low socioeconomic status have claimed an interest in using smartwatches but continue to experience a digital divide compared with wealthier and majority groups.21,22 Black and ethnic minorities also experience frailty on a greater scale than their white counterparts. 23 Our program helps meet the needs of vulnerable populations to enhance reach and use of smartwatches to older patients in our underserved population.
Having team members performing the necessary software modifications and programming was unique for this project and helped minimize cost and time. The labor necessary for this project is feasible. There were challenges during the watch pairing process, such as finding that one iPhone only allowed five paired watches and developing a work around; however, these challenges existed due to this being a first-of-its-kind project utilizing standalone watches for clinical research. Our developmental process may be used as a guide for future projects to help limit these challenges. The accessibility and usability, of BeFitMe™ Watch app may help improve future participation in prehab.
Comparison with prior work
mHealth apps designed for prehab have the potential to overcome transportation barriers, are cost-effective, and can increase patient empowerment. 24 Consistent with prior studies that utilized wearable devices,6,7,10 we found positive engagement between the participants and the watch devices. While prior work shows there remain certain barriers with technology-assisted prehab programs, such as patient confusion with mobile devices, disinterest in technology, or that mobile applications were not responsive to older patients’ needs, 12 we found that most enrolled patients liked using the Apple Watch and that BeFitMe™ Watch app was helpful for their exercise needs. Perhaps this is because it may be easier to engage in physical activity by wearing a watch rather than holding a smartphone.
To our knowledge, this is the first-of-its-kind study utilizing a standalone Apple Watch app, where an iPhone is not provided and neither wi-fi nor cellular service is necessary for longitudinal clinical use and medical research. Previous studies utilizing Apple Watches have collected longitudinal data by asking patients to voluntarily share their Apple Watch health data, 25 by providing patients with an iPhone, 26 or by excluding patients who do not have an iPhone or Apple Watch. 27
Limitations
This study has limitations. The population sample was small, with only three beta testers and six user testers. However, the sample was representative of the population we serve, and the small sample size did not take away from the overall goal of the study, which was to determine the usability and acceptability of BeFitMe™ Watch app. Secondly, Beta testing was only conducted with study staff. However, the three staff members were from three different areas of expertise, which allowed for diverse and thorough testing. Lastly, of the six patients selected for user testing, only three ultimately underwent surgery. Future studies will examine BeFitMe™ Watch app in a larger surgical population and determine whether this technology impacts prehab participation.
Conclusion
This study details the development, design, and demonstration of an accessible and efficient standalone Apple Watch BeFitMe™ prehab intervention. Continued use and evaluation of the BeFitMe™ Watch app will help us determine whether this format will increase prehab participation for older patients undergoing surgery and potentially improve patient outcomes.
Footnotes
Acknowledgments
I would like to also thank all of my colleagues for their wonderful collaboration and review of the final manuscript for publication.
Declaration of conflicting interests
Apple Inc. was not involved in the study or analysis.
Ethical approval
The University of Chicago Institutional Review Board (IRB21–1318 on 10/18/2021) approved this study.
Funding
This work was supported by the Healthcare Delivery Science and Innovation Grant from the University of Chicago.
Guarantor
SK.
Contributorship
SK and MLM researched literature and conceived the study. EB was involved in the software development and design of the BeFitMe™ Watch app. SK wrote the first draft of the manuscript and MLM was involved in the ongoing revision process. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
