Abstract
Aims
The use of virtual care enabled by digital technologies has increased, prompted by public health restrictions in response to COVID-19. Non-hospitalized persons in the acute phase of COVID-19 illness may have unique health needs while self-isolating in the community. This scoping review aimed to explore the nature of care, the use of digital technologies, and patient outcomes arising from virtual care among community-based self-isolating COVID-19 patients.
Methods
Literature searches for peer-reviewed articles were conducted in four bibliographic databases: CINAHL, Medline, Embase and Cochrane Database of Systematic Reviews between January and February 2022, followed by hand-searching reference lists of included articles. Two levels of screening using defined eligibility criteria among two independent reviewers were completed.
Results
Of the 773 articles retrieved, 19 were included. Results indicate that virtual care can be safe while enabling timely detection of clinical deterioration to improve the illness trajectory. COVID-19 virtual care was delivered by single health professionals or by multidisciplinary teams using a range of low-technology methods such as telephone to higher technology methods like wearable technology that transmitted physiological data to the care teams for real-time or asynchronous monitoring.
Conclusion
The review described the varied nature of virtual care including its design, implementation, and evaluation. Further research is needed for continued exploration on how to leverage digital health assets for the delivery of appropriate and safe virtual COVID-19 community care, which can support patient recovery, control transmission, and prevent intensifying the burden on the health care system, especially during surges.
Introduction
The coronavirus disease (COVID-19) pandemic resulted in the implementation of a wide range of public health measures to control the circulation of the highly infectious virus.1,2 Individuals who tested positive for COVID-19 were ordered to self-isolate to prevent transmission of the virus; clearance from self-isolation was based on rapidly changing clinical management guidance. 3 At the height of the pandemic, case management and contact tracing were routinely conducted as part of infectious disease control practices. 4 However, much of the emphasis was placed on ensuring that the patient understood and complied with the quarantine order, rather than on well-being and recovery. Most recently, some jurisdictions around the world have begun easing public health restrictions such as modifying mask mandates and lifting legal self-isolation requirements.5–7 Despite the revocation of legislated orders to self-isolate, newly confirmed self-isolating COVID-19 patients may have unique health needs that warrant support provision beyond being given instructions to stay home. With virtualized health care advancing expeditiously across health systems, particularly related to preventing viral transmission and acquisition, there is potential for this modality to be integrated into COVID-19 care pathways.
The incorporation of digital technologies into health care, using information and communications technology, falls under the umbrella of digital health, 8 with which virtual care fits in. Recent literature describes a need for remote care to maintain health service provision when in-person visits are limited, 9 as well as, for continuity of care for populations such as diabetes, cancer, mental health, and obstetrics.10–13 A systematic review exploring telehealth's role during the COVID-19 pandemic finds that telehealth plays a key role in reducing viral spread while conserving health system capacity, even while the patient or provider has acquired COVID-19. 14 In response to the emerging need, jurisdictions across Canada have adapted physician billing, 15 similar to other countries such as the United States of America and Australia that have shifted policies to promote telehealth use.16,17
In contrast to hospitalized patients for acute COVID-19 treatment, asymptomatic persons or those who experience mild symptoms may have less care offered; however, the care for these individuals should not be neglected as appropriate medical interventions, and psychosocial and other supports are needed during the course of isolation. 18 For patients in the early phase of COVID-19 illness, telecare has the potential to effectively monitor for clinical deterioration and to provide at-home treatment. 19 COVID-19 and the rapid expansion of virtual care are both relatively novel; there may be gaps in knowledge about the use of virtual care for COVID-19 patients. A greater understanding of the range of virtual health services offered to self-isolating COVID-19 patients may improve their access to health care, contribute to monitoring for clinical deterioration, help to ensure compliance with self-isolation, and examine the overall quality of care during the active illness and isolation period.
Purpose and objectives
The purpose of this scoping review is to explore the nature and outcomes of health care services provided through virtual modality for community-based self-isolating COVID-19 patients and to identify gaps in the literature on the use of virtual care for this population. Objectives of this review include:
To examine the types of virtual health care services and supports that are provided to COVID-19 patients who are self-isolating in the community. To describe the technology that is utilized in delivering virtual care to COVID-19 patients who are self-isolating in the community. To describe who delivers virtual care, and for how long, to COVID-19 patients who are self-isolating in the community. To explore the COVID-19 patient outcomes arising from virtual care during the self-isolation period in the community.
Methods
This scoping review followed the methods outlined by the Joanna Briggs Institute including a comprehensive search of four databases, staged eligibility screening using two independent reviewers, data extraction, and analysis. 20 Details on the scoping review methods can be found in our scoping review protocol. 21
Search strategy
Summary of yield and results by eligibility screening.

Studies were excluded if they (1) were not empirical studies, (2) reported on individual case studies or case presentations with

Flow diagram of databases, yield, and screening results.
Results
A total of 19 articles met the eligibility criteria and were included in the review.25–43 A summary of the included articles can be found in the Appendix. Of the 19 relevant records, most were conducted in Australia (
Furthermore, virtual health services and supports include the provision of health advice and patient education such as when to access emergency care, symptoms that signify clinical deterioration,25,34,37 and prevention of transmission and isolation requirements.32,37,39,42,43 Medication reconciliation or patient education about medication use were offered.28,32,37 Few of the included studies offered services and supports beyond the biomedical approach. Psychosocial supports were available either directly from the program or via a referral.28,29,33,42,43 Other services were also described, such as resource provision or linkages to community resources including grocery delivery or meal assistance,33,37,42 free personal protective equipment, 37 and peer connection with other COVID-19 patients. 43 Eleven studies also offered dedicated helplines, contact information, or similar safety system, whereby the patient can reach a provider directly, or message or page a provider when needed.26,28,29,32,34,36,39,40,42,43 Notably, research conducted in Australia and UK highlighted the use of “virtual wards” as an extended hospital service, using inpatient language such as admissions and bed days.28,30,35 However, these wards did not involve inpatient face-to-face admission; rather the ward provided virtual care remotely to patients in their homes or usual dwelling in the community.
The frequency of contacts with patients ranged from a low of only when initiated by the patient 36 to a high of up to three times daily 29 when there were synchronous interactions. When studies utilized automated vital sign monitoring, digital communication of health data by machine occurred up to fifteen-minute increments. 41 Table 2 outlines the variation in services and supports alongside the frequency of contacts.
Count of studies by types of services and supports, and frequency of contacts to patients.

Note: This table provides an overview of the number of studies offering each type of health service and support against the frequency of interactions. Some studies offered different levels of service for different groups of patients based on their virtual care protocol. The table is not intended for the counts to add up to the total number of studies included in the review.
The duration of the virtual care programming varied across studies with some specifying a minimum number of days such as 7 days 38 or maximum number of days such as 14 days.25,31,33 Other studies did not specify time frame parameters, where discharge relied for example, on symptom resolution, isolation clearance, or clinician judgment about recovery.26,28–30,32,34,35,37,39,41,43 Figure 2 summarizes the duration of virtual care.

Summary of duration of virtual care.
Summary of digital health technologies by study.

Web-based platforms or applications allowed for two-way online consultation visits. Video conferencing was substituted by telephone calls when patients did not have digital access33,34 or conversely, telephone calls were supplemented by video conferencing when escalation of care was required for visual assessment. 37 Where provider-patient interactions took place over video platforms, several studies’ remote monitoring also comprised the use of equipment for the assessment of vital signs for some or all patients.27,29,32,33 Distribution of pulse oximeters and thermometers to patients isolating at home was also common.27,29,32,33,36 Telemedicine or telehealth provided solely through telephone calls (without any other equipment) was the mode of health care delivery in five studies.,25,26,28,30,38 Usage of digital applications designed for health care, such as the digital platforms with patient and clinician portals were used.33,35 For example, Swift et al. 35 operated a virtual ward through a digital platform where patients could enter information which were then transmitted and displayed on the clinical dashboard for clinician monitoring. Applications leveraging social media networking platforms were also described in two studies.40,43 Both studies, based in Asia, optimized the messenger feature for text communication, as well as the telephone function within the social media networking platform.40,43 One of them also relied on the Cloud for completion of telemedicine form that gathered assessment information on the patient. 43
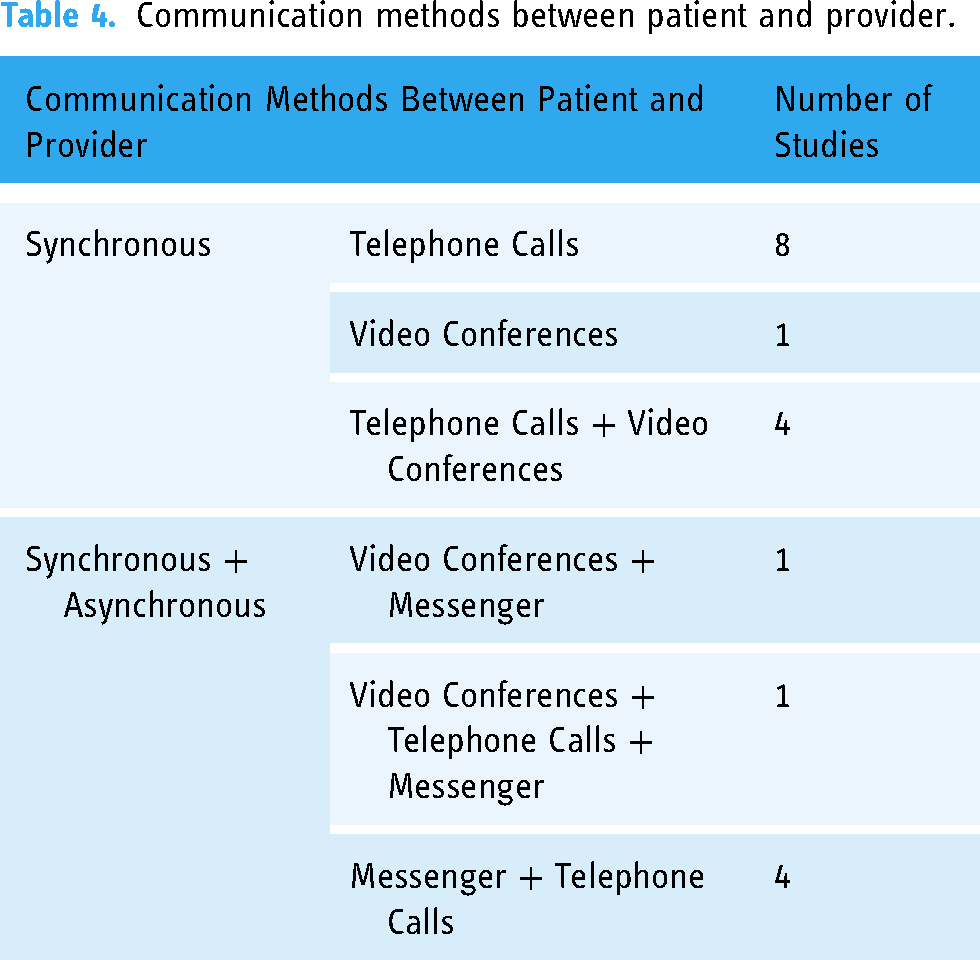
The deployment of wearables and equipment where vital sign data and bio-signals were transmitted electronically were reported by authors. For example, continuous monitoring was enabled by data collected every fifteen minutes from an in-ear device on patient oxygen saturation, respiratory and heart rates, and core temperature and sent via Bluetooth to a secure server. 41 Similarly, a wearable patch was applied to the axilla for continuous temperature monitoring, and a pulse oximeter for heart and oxygen saturation rates was used, with Bluetooth transmission. 29 In another study, patients were tasked with measuring their vital signs two times a day; although the emphasis was on self-monitoring rather than by the care providers, data for the vital signs were collected and transmitted via an application on the patients’ device and were reviewed by the team. 31 In sum, these studies allowed for transmission of the vital sign health data to be automated. Table 4 outlines the communication methods between patient and provider with the number of corresponding studies.
Communication methods between patient and provider.
For virtual care teams that encompassed more than one professional discipline, there was no consistent composition of interdisciplinary teams. Nurses and physiotherapists provided care through video consultation in the UK, 35 obstetrical nurses and physicians provided telehealth in the US, 38 while other studies utilized teams with more interdisciplinary team members including physicians and nurses, complimented by psychologists, 43 mental health or social workers, pharmacists, practitioners,28,32,33 nurse practitioners,32,33 and pharmacy residents. 32 Where studies involved direct care by physicians, these physicians practiced in family medicine,32,33 infectious disease34,36 and obstetrics. 38 Many of the included studies had a clinical pathway that incorporated the consultation with or referral and escalation to physicians when signs flag clinical status decline.25,28,30,32,33,37–39,41,42 In the Canadian program with a comprehensive interprofessional team, the team held daily huddles and weekly rounds; physician specialists in this program also included internist, respirologist, and psychiatrists. 33 Likewise, an American study focusing on the obstetrical population also held daily team huddles. 38 Despite the virtual care being directly provided by nurse navigators in the French study, the authors emphasized the importance of interdisciplinary team meetings to assess the intervention on a regular basis. 42
Discussion
This scoping review aimed to explore the nature and patient outcomes of virtual health services provided during the active phase of the illness to persons with COVID-19 who were isolating in the community. The included studies converge on addressing a gap in the health care for newly diagnosed COVID-19 patients in the community. Table 5 summarizes key findings.
Discussion summary.

Leveraging social media as a platform for health promotion has been previously documented to engage in areas such as sexual health, 47 nutrition, physical activity, and smoking, 48 and most recently for COVID-19 vaccination campaigns. 49 Included in this scoping review, were two studies that made use of common social networking mobile applications; the research pointed to the convenience of using common and widely-used apps so that patients did not need to download a separate app,40,43 while also having the ability to facilitate peer support for patients to support other patients with providing tips in the group chat. 43 Social media use by health care organizations has become widespread for education, health information dissemination, mobilization for purposes such as influencing policy, and more. 50 The selection of applications may be dependent on contextual factors, including understanding specific communities and settings, while weighing the benefits of providing some form of care against the risks of an absence of care. The utilization of social media and networking platforms may have benefits; however, privacy and confidentiality implications cannot be overlooked. Alongside the convenience of digital solutions, distinctive cybersecurity challenges arise related to protecting personal health information, ensuring secure networks, finding a private location to conduct patient conferencing, and more. 51 From selection of platform to obtaining patient consent, implementation of virtual care using any platform or digital solution must involve performing privacy impact analysis, conducting privacy and security trainings, crafting and clearly outlining an information management framework and virtual care policy. 51
While deployment of more advanced digital technologies may be a facilitator for enhanced assessment and communication between patient and provider, the requisite of patients and their caregivers being able to use the technology, requires that digital solutions be user-friendly. 29 The reliability of these digital solutions and networks, as well as the comfort of wearable devices where they are used, can also affect the success of the virtual care intervention.35,41 Additionally, digital equity must be at the forefront of virtual care design for COVID-19 patients. Scaling up and spreading of virtual health care for COVID-19 patients cannot exclude population groups and communities who do not have access to the internet, devices, or other resources essential for receiving care remotely. Even while relying on a low technology model of using telephone modality in a virtual care program, researchers reported a substantially higher hospitalization rate among the sample compared to other studies included in this review. 37 In this particular study, the patient population was reported to commonly face barriers in accessing care and experience health disparities, suggesting that social determinants of health shaped their COVID-19 acquisition likelihood and severe illness trajectory. Especially prudent, is taking action to address digital and health equity among communities that have been disparately affected by COVID-19 infections. While virtual services aim to detect deterioration early on in the disease trajectory and to escalate care in a timely manner, navigating through the complex digital system requires thoughtful design. Clinicians, researchers, and policy-makers must ensure that under-served communities, which are significantly more affected by COVID-19, do not get left further behind as healthcare leverages digital tools to enable improved care.
Furthermore, this review demonstrates that care given by interdisciplinary teams can offer a more comprehensive continuum of services to community-based COVID-19 patients. Where care was provided by an interdisciplinary team, patient needs beyond the bio-medical nature may be met through provision of psychosocial supports and resource linkages.32,33,43 In parallel, tangible supports like grocery delivery and personal protective equipment 37 or supports addressing food insecurity 33 are also key to meeting patient needs more holistically when considering the realistic effects of the social determinants of health. This suggests that there is value in having a comprehensive basket of services, based on individual patients’ and families’ lived situations and scenarios, which could improve their recovery and well-being. The initial search for literature yielded some records on telerehabilitation53–55 and remote diagnostic imaging.56,57 These had a more core focus on diagnostics or longer-term COVID-19; although, they did not meet the review's inclusion criteria, they signal increasing advancement in the breadth of digital health services available for non-hospitalized COVID-19 patients.
Clear theoretical and operational definitions of the problem (such as lack of availability of care during the self-isolation period) are needed, especially with the continuously evolving nature of the pandemic The design of interventions relies on having clarity of the problem, a vision for the desired improvement, and outline of the active ingredients of the health intervention including components, mode, and dose. 58 In conceptualizing virtual care, researchers can wrestle with what constitutes the intervention. For instance, virtual care itself may be considered an intervention. An alternative approach may be to consider virtual care as the mode of delivery of an intervention, rather than the intervention. Studies included in this review offered virtual care for different lengths of time. Virtual care programming generally lasted for a duration of around 14 days, however there is no consistency in the dose of the intervention. Even when there is seemingly common duration such as services offered for 14 days, it is not always clear whether service was completed for a total of 14 days from enrolment or from the patient's symptom onset date, specimen collection date, case reported date, or another date. There may be opportunities for engagement in intervention research comparing the outcomes of groups with virtual care versus routine care, or outcomes of groups using different platforms and technologies. The recent appearance and authorization of oral antiviral medications signals another shift in treatment for patients, and may additionally prompt adjustments to and re-examination of virtual care program planning for COVID-19 patients.
Virtual programs covered by this scoping review frequently classified patients by risk category, which affected the frequency of contacts from the provider to the patient. However, these categorizations and classifications differed. Researchers can consider standardizing risk assessments. Similarly, common outcome measures for research could be applied for better comparisons in COVID-19 research. This is strongly advocated by the WHO Working Group of the Clinical Characterisation and Management of COVID-19 Infection (2020), urging the development of minimum data elements in research. 59 Patient experience, beyond patient satisfaction, emerged as a significant gap in the virtual COVID-19 care research.
Limitations
This scoping review was undertaken to explore the state of the literature on virtual care for the COVID-19 patient isolating in the community. A limitation of this review may be missing relevant records that were not identified from databases beyond those used in this search, and literature not published in English.
Conclusion
Despite a trend in easing of public health restrictive measures in some areas around the world, the threat of variants persists. 60 Early detection of clinical deterioration and disease progression can facilitate appropriate decision-making, which consequently ensures that there is no delay in assessment and treatment, while promoting the prioritization of patients who are in need of hospitalization. 61 The provision of virtual care for patients at home can meet patient needs while curbing spread of the virus to others. Amidst the shifting and ever evolving nature of the COVID-19 response, the safety and high-quality care for community-based isolating patients diagnosed with COVID-19 remain a gap in need of attention and narrowing. Findings from this scoping review mapped out the current evidence on virtual care provision for persons with COVID-19, who are self-isolating in the community, and point to a breadth of research, practice, and policy opportunities. Serving this particular population benefits the patients themselves, and the hospitals, while reducing the overall burden on an already stretched health care system. It is important to commit and invest in appropriate and safe virtual care pathways for infectious diseases to better prepare for future outbreaks and pandemic threats.
Footnotes
Acknowledgments
We would like to thank Don Kinder for consultation on the search strategy.
Contributorship
LCL and CC conceptualized the study, developed the protocol, conducted eligibility screening. Extraction of data and formal analysis were conducted by LCL and verified and refined by CC. Original draft was prepared by LCL, and substantive edits and revisions to manuscript content made by CC and LCL. All authors reviewed, edited, and approved the final version of the manuscript.
Ethical approval
The authors consulted with the institution's Research Ethics Board about the need for ethical review. Ethical review and approval were waived for this scoping review as it did not involve the use of either humans or animals as participants.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Guarantor
LCL
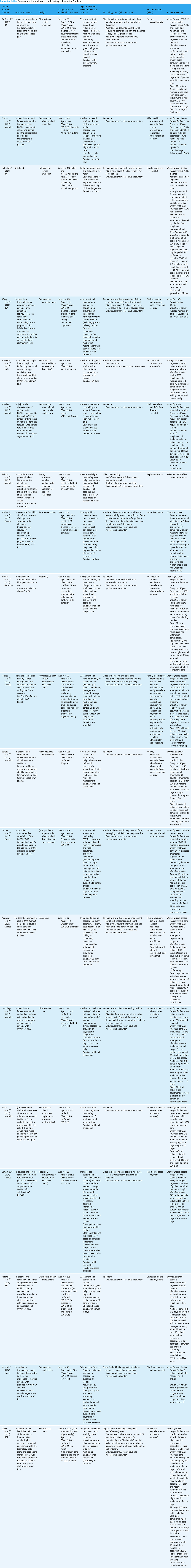
Appendix: Summary of Included Articles.
Summary of Characteristics and Findings of Included Studies
| Author, Year and Country | Purpose Statement | Design | Sample Size and Patient Characteristics | Type and Dose of Health Service and Supports | Technology Used (what and how?) | Health Providers (who?) | Patient Outcomes |
|---|---|---|---|---|---|---|---|
| Swift et al.
35
(2021) |
“to share a description of the service and early outcomes, as healthcare systems around the world face ongoing challenges.” (p.8) | Observational service evaluation | Virtual ward that includes remote support and follow-up post hospital discharge; helpline with daily symptom monitoring |
Digital application with patient and clinical portals, messenger, video, and clinical dashboard |
Nurses, physiotherapists | ||
| Clarke et al.
25
(2021) |
“to describe the rapid implementation of a telephone based COVID-19 community monitoring service and the demographic |
Retrospective mixed methods evaluation | Provision of health advice and support, clinical social and welfare assessments, education on isolation, symptoms signifying deterioration, post-discharge call |
Telephone |
Allied health providers, and |
||
| Bell et al.
36
(2021) |
Not stated | Retrospective service evaluation | Follow-up assessment and provision of test result |
Telephone, electronic health record system |
Infectious disease specialist | ||
| Wong et al.
37
|
“to describe a telehealth-based program to monitor patients in the outpatient |
Retrospective feasibility cohort | Assessment and monitoring of symptoms, education on prevention of transmission, resource-provision during isolation (including grocery delivery support from local community resources, free personal protective equipment and medication reconciliation) with daily weekday calls |
Telephone and video consultations (when escalation required/clinically indicated) |
Medical students and physician (when escalation required) | ||
| Malwade et al.
40
|
“to provide an example from a hospital in India using the social networking app, WhatsApp, as a teleconsultation (TC) alternative during the COVID-19 pandemic” (p.2) | Retrospective |
Provision of diagnostic reports and clinical advice such as blood tests for co-morbidities or assessment at hospital |
Mobile app, telephone |
Not specified (“Health care providers”) | ||
| Micallef et al.
26
|
To “[a]scertain characteristics of patients with COVID-19 managed by telehealth…Ascertain amount of time taken by staff to perform this care, and whether this care might reduce burden on other services of healthcare organisation” (p.2) | Retrospective observational cohort study, single centre | Review of symptoms, counselling and support; ‘safety net’ advice, prescription or medical notes |
Telephone |
Clinic physicians and, infectious diseases specialist | ||
| Raffan et al.
27
|
“to contribute to the growing body of literature on the virtual care experience by providing insight into the patient experience of a prescribed COVID-19 model of virtual |
Survey |
Remote vital signs monitoring twice daily, temperature monitoring, 24/7 access to RN |
Video conferencing |
Registered Nurse | ||
| Michaud et al.
31
|
“to assess the feasibility |
Prospective cohort | Vital sign (blood pressure, heart rate, respiratory rate, oxygen saturation, temperature) self-assessment twice a day, assessment of symptoms via questionnaire for self-monitoring, telephone call at day 3 and day 10 for discussion of concerns |
Mobile application for phone or tablet (to record vital signs) with transmission of data to database and algorithm (for patient's decision-making based on vital signs and symptom severity), telephone |
Nurse Practitioner | ||
| Wurzer et al.
41
|
“to reliably and continuously monitor biosignals relevant to the |
Feasibility |
Biosignal observation and monitoring by team 24/7 of biosignals taken for 3 min every 15 min, daily telephone support and assessment of symptoms and cognition |
Telephone |
Not specified (“trained members”) |
||
| Pimlott et al.
32
|
“describes the natural history, clinical management and |
Retrospective chart review, observational, descriptive study | Assessment and monitoring daily or every two days (depending on patient's condition), management included messages about self-isolation, hydration, and medication use |
Video conferencing and telephone |
Family medicine-led interdisciplinary team: Family medicine residents, staff family physicians, nurses (initial visit by family medicine resident and physician with follow-up by resident and physician or nurse) |
||
| Schultz et al.
28
|
“to describe and evaluate the implementation of a virtual ward as a COVID-19 |
Mixed methods observational | Virtual ward that includes risk assessment, |
Telephone |
Nurses, pharmacists, social workers, medical officers, administrative officers, and medical officers (when escalation required) | ||
| Ferrua et al.
42
|
“to provide a comprehensive description of the CAPRI-COVID intervention” and “to provide feedback on the usefulness of this platform for cancer patients” (p.4486) | (Not specified – |
Assessment and education of minimizing COVID-19 exposure with patients and relatives, home care and meal assistance, symptom monitoring (telenursing or by patient via app) |
Mobile application with telephone platform, messaging, and dedicated telephone line |
Nurses (“Nurse Navigators”) and assistant nurses | ||
| Agarwal et al.
33
|
“to describe the model of care in COVIDCare@ |
Descriptive | Initial and follow-up assessments every other day, or every 3 days dependent on risk level, brief counselling and linking to community resources, communication with patient's primary care provider as applicable |
Telephone and video conferencing, patient portal with messenger, dashboard |
Family physician, family medicine resident, Registered Nurse, mental health worker or social worker, nurse practitioner, pharmacist |
||
| Hutchings et al.
29
|
“to describe the implementation of and early experience with virtual health care for community management of patients with COVID-19” (p.1) | Observational cohort | Provision of “welcome package” delivered to home, vital sign monitoring (no BP), symptom monitoring for clinical assessment, provision of psychosocial support with scheduled contacts from team 3 times a day (at least one video conference daily |
Telephone and video conferencing, Mobile application |
Nurses and medical officers (when escalation required) | ||
| Ferry et al.
30
|
“(1) to describe the |
Retrospective clinical assessment, single-centre |
Virtual ward that includes symptom monitoring, assessment of well-being and social factors |
Telephone |
Nurses and medical officers (when escalation required) | ||
| Lam et al.
34
(2020) |
“to develop and test the feasibility of a virtual |
Feasibility |
Standardized assessments for initial and follow-up contacts), follow-up contacts explore symptom changes, education on the disease and symptoms which would signal need for medical attention |
Video conferencing (for patients who have access to video-based platform) and telephone |
Infectious disease physician | ||
| Reforma et al.
38
|
“to describe the feasibility and clinical and process outcomes associated with a multidisciplinary telemedicine surveillance model to triage and manage obstetrical patients with known exposures and symptoms of COVID-19” (p.1) | Descriptive (quality improvement) | Assessment and education on isolation, symptoms, hygiene, with follow-up calls daily or every other day, and encouragement to contact primary OB care provider for OB-related needs |
Telephone |
Obstetrical nurses and physicians | ||
| Xu et al.
43
|
“to evaluate a telemedicine model that was developed to address the challenges of treating patients with progressive COVID-19 who are home-quarantined and shortages in the medical workforce” (p.1) | Retrospective single-centre | Telemedicine form on Cloud for initial and subsequent assessment, guidance on isolation requirements, group chat with other participants and team; worsening symptoms or decline in mental state would be escalated for hospital care; mood support from psychologist |
Social Media Mobile app with telephone calling, e-counselling, messenger |
Physicians, nurses, and psychologist | ||
| Coffey et al.
39
|
“to determine the feasibility and safety of the COVID-19 [remote patient monitoring] as measured by patient engagement with the technology, rate of alerts and escalations managed by virtual care teams, acute care resource utilization rates, and patient clinical outcomes” (p.3) | Retrospective cohort | Symptom assessment two times a day, vital sign data collection, education on care plan, and when to go to emergency with 24/7 monitoring |
Digital app with messages, telephone |
Nurses and physicians (when escalation required) |
