Abstract
Case series summary
Medical records of two cats with chronic calcaneal wounds, managed using a single pedicle advancement flap combined with transarticular external skeletal fixation (TESF), were reviewed. Clinical presentation, surgical technique, and short- and long-term follow-up were documented. Both cats presented with chronic, non-healing wounds over the calcaneal tuberosities. After surgical debridement, a single pedicle advancement flap was harvested from the lateral distal tibia and sutured over the wound. A type I TESF using epoxy resin as the connecting bars was applied medially to stabilize the joint. In both cases, complete wound healing was achieved.
Relevance and novel information
These two cases demonstrate the successful use of a single pedicle advancement flap combined with a type I TESF for managing chronic calcaneal wounds in cats. The technique reduces flap tension and may enhance healing outcomes in anatomically difficult regions. This approach may be beneficial for treating chronic wounds over bony prominences in cats.
Keywords
Introduction
Chronic wounds on bony prominences present significant challenges. This is because of the limited soft tissue coverage and the mobility of the joint affecting the skin tension.1,2 In the calcaneal region, various wound closure techniques can be considered. These include local skin flaps (advancement, rotation or transposition flaps), axial pattern flaps and healing by second intention. 3 However, there is no perfect, one-size-fits-all technique. Second intention healing may require prolonged wound management and result in failure to achieve complete closure, particularly in distal limb wounds.4,5 Primary closure or flap techniques that place sutures directly over bony prominences may result in excessive tension, increasing the risk of dehiscence. 6
A single pedicle advancement flap is a straightforward technique used to close wounds where skin is available on one side of the defect. This flap is a subdermal plexus flap, meaning the skin and underlying subcutaneous tissue are elevated while preserving the vascularity of the subdermal plexus. Although simple in execution, this technique can lead to significant tension, requiring careful planning. 7
Transarticular external skeletal fixation (TESF) is a technique that allows control over joint movement and is designed to stabilize joints, notably on the tarsocrural joint.8,9 Several types of TESF exist but types I and II are often preferred for their easy application. Although TESF’s primary applications have traditionally focused on bone repair and temporary immobilization, particularly in cases of ligament and tendon injuries, its use in wound management has been reported in cats and dogs.10,11 It is less documented to support primary or delayed primary closure, but it has been adapted to support wound healing after a flap reconstruction.12,13
In this case series, the use of a single pedicle advancement flap, supported by TESF, is described for the treatment of calcaneal wounds in two cats.
Case series description
Case 1
A 5-year-old male domestic shorthair cat weighing 4.19 kg was presented with a plantigrade stance and a chronic wound on the right calcaneal region. The cat exhibited a 4/5 lameness. The wound had been present for over 1 year. This injury was caused by a prior calcaneal fracture that resulted in malunion. A mild retraction of the digital flexor tendons was also observed. The wound exposed an area where the calcaneus was covered by healthy-appearing granulation tissue. Although there was a rim of pale pink tissue along the wound edges, this was identified as granulation tissue, with no definitive signs of epithelialization. Radiographs revealed no evidence of osteomyelitis (Figure 1).
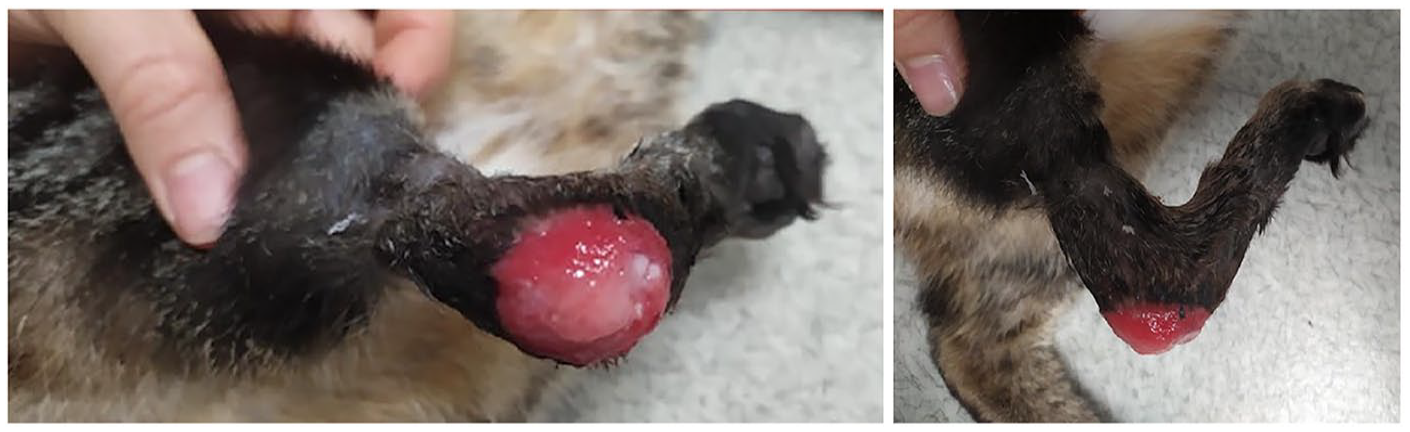
Initial presentation of cat 1’s right tarsal injury, showing chronic wound at the calcaneus
Surgical management aimed to temporarily stabilize the right tarsus in hyperextension to allow for wound healing before considering a pantarsal arthrodesis. The cat was induced with diazepam (0.2 mg/kg IV) and alfaxalone (2 mg/kg IV), maintained with endotracheal isoflurane in oxygen. Pain management was provided with an initial dose of morphine (0.2 mg/kg IV), followed by a continuous rate infusion throughout the procedure (0.1 mg/kg/h), alongside an antibiotic dose of amoxicillin and clavulanic acid (20 mg/kg IV). The right hindlimb was clipped and aseptically prepared.
After freshening the edges of the wound using a no. 15 scalpel blade, a single pedicle advancement flap was created. Two parallel incisions measuring 2.5 cm in length were made, beginning at the proximal and distal margin of the wound. The incisions extended in an oblique direction proximally onto the lateral aspect of the distal tibia. The flap was undermined, ensuring the dissection reached the underlying fascia, while preserving the subdermal plexus. The base of the flap measured 1.5 cm. The flap was closed using simple interrupted sutures with 4-0 poliglecaprone for the subcutaneous tissue and 4-0 nylon for the skin (Figure 2). A type I TESF was applied on the medial side of the limb, with two 1.2 mm positive profile threaded pins inserted into the distal tibia: one in the central tarsal bone and another in the proximal metatarsal bones II and III (Figure 3). The pins were connected using a plastic tube, which was then covered with epoxy resin. A 1 cm gap was intentionally maintained between the resin and the skin to avoid direct contact. Postoperative radiographs confirmed the correct positioning of the pins.
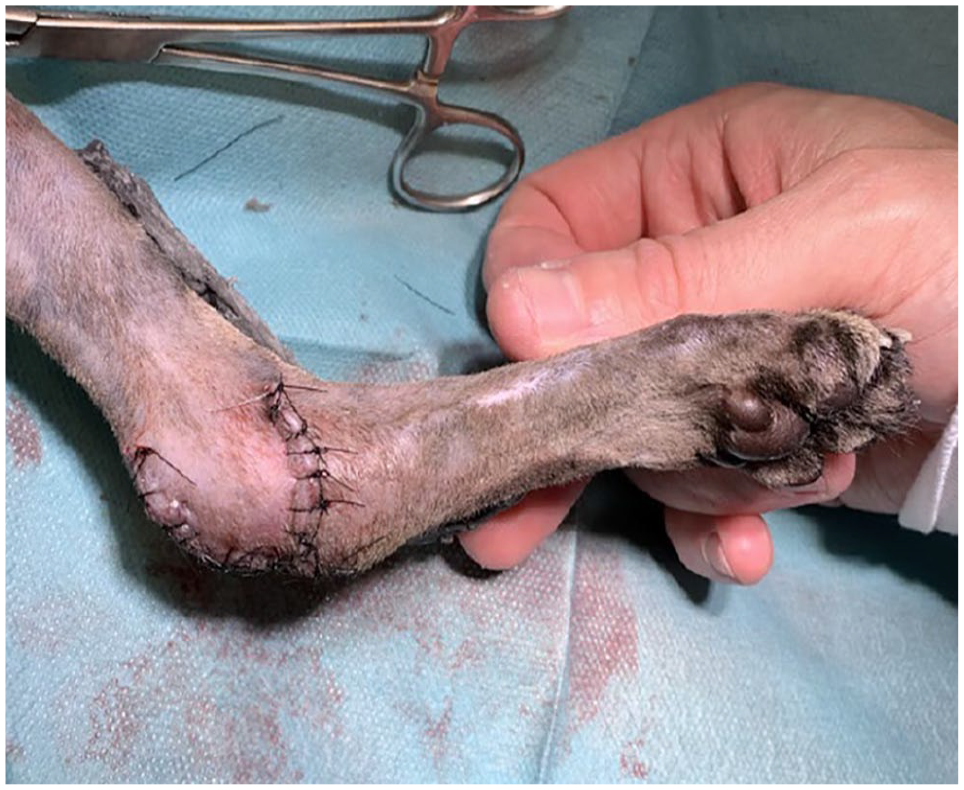
Picture of the pedicle advancement flap in cat 1

Picture of the type I transarticular external skeletal fixation on the medial aspect of tarsus in cat 1
The cat was discharged 24 h postoperatively with amoxicillin and clavulanic acid (20 mg/kg PO q12h for 15 days), meloxicam (0.05 mg/kg PO q24h for 5 days) and tramadol (4 mg/kg q12h for 5 days). Strict rest was advised. Wound care instructions included cleaning and application of sulfapyridine ointment to the pins site once daily. The use of oral antibiotics was continued as a prophylactic measure to prevent infection. A light protective dressing was also placed over the fixator.
Three weeks postoperatively, the wound was fully healed, allowing for suture and fixator removal under sedation with medetomidine (20 μg/kg IM) and morphine (0.2 mg/kg). A decreased range of motion of the tarsus was observed. Minor discharge was observed at the pin insertion sites, leading to the continuation of topical treatment. At the 2-month follow-up, the wound remained completely healed, but a moderate plantigrade stance recurred. A definitive arthrodesis was recommended but was declined for financial reasons. The use of a supportive brace was advised.
Case 2
A 3-year-old female domestic shorthair cat weighing 4.5 kg was presented with a similar wound on the left calcaneus of unknown origin. It had been managed for 2 months with bandage changes, but a 1.5 cm diameter lesion persisted. Orthopedic examination was unremarkable (no lameness). Preoperative radiographs showed no abnormalities.
The same anesthetic protocol was performed. The wound was debrided (Figure 4). The superficial digital flexor tendon was found to be luxated laterally. It was repositioned and secured to the medial retinaculum with three simple interrupted sutures using 3-0 polydioxanone. A single pedicle advancement flap was harvested from the lateral distal tibia and sutured to cover the defect, using the technique described for case 1 (Figure 5). Similarly, the TESF was applied. Postoperative radiographs confirmed correct implant placement (Figure 6).

Debridement and partial granulation tissue removal to create a fresh wound bed in cat 2

Cat 2: postoperative view of advancement flap over the tarsal region with a type 1 external fixator in place for joint stabilization
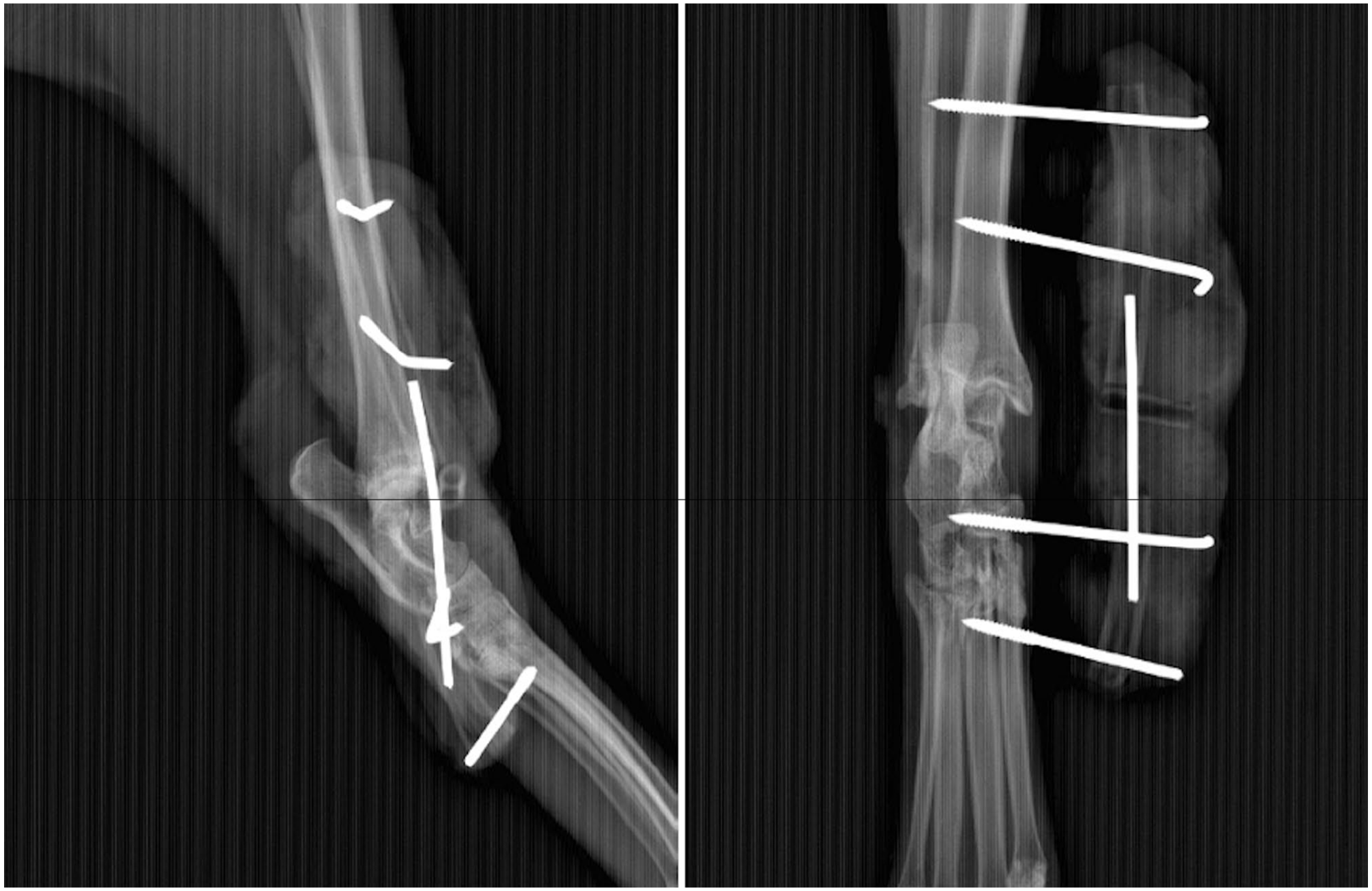
Cat 2: immediate postoperative radiographs (lateral and craniocaudal views) show placement of type 1 external fixation
Cat 2 recovered well from surgery and was transitioned to buprenorphine (0.02 mg/kg IV q8h) postoperatively. Amoxicillin and clavulanic acid (20 mg/kg IV q8h) was continued for 24 h. A dark red skin discoloration at the flap’s extremity was observed. It resolved completely within 48 h. The cat was discharged 72 h after surgery. The postoperative care instructions for cat 2 were similar to those for cat 1.
The sutures and fixator were removed 3 weeks postoperatively, with the wound exhibiting complete healing (Figure 7). Seven months later, the cat was seen for an unrelated cause and no recurrence of the wound was observed.

Cat 2: postoperative follow-up images show the healed advancement flap on the tarsal region
Discussion
The calcaneal region is considered at increased risk of dehiscence due to the mobility of the tarsus. The size of the wounds in both cases caused excessive tension, ruling out direct appositional closure as an option. Axial pattern flaps, such as caudal superficial epigastric, lateral genicular or reverse saphenous conduit flaps, are effective options for distal hindlimb reconstruction; however, they are associated with higher morbidity. For caudal superficial epigastric flaps, distal necrosis was more likely when extending beyond vascular bound-aries, sometimes requiring healing by second intention. 14 Reverse saphenous conduit flaps showed minimal necrosis (under 15%) but were associated with venous congestion and mild sloughing. 15 Given the invasiveness and complications of these techniques, a local flap was preferred as first intention.
There are no guidelines regarding the length:width ratios of single pedicle advancement flaps.16,17 The commonly accepted maximal ratio is 2:1.16,18 This ratio is similar to findings in humans, where the length:width ratios of 1:1 or 2:1 are used to maintain flap viability.19,20 However, it is important to recognize that these ratios cannot be uniformly applied across all areas because of regional differences in skin vascularity. 21 Nathanson and Jackson 22 showed that flap survival is more dependent on blood flow, with flaps of the same length having similar blood flow, regardless of their width. Despite that, in our cases, the 2:1 length:width ratio of the flaps was respected, not as a rigid rule, but as a conservative approach adapted with the vascular limitations of the distal tibia and calcaneal region.
Single pedicle advancement flaps are relatively straightforward, but careful planning is essential. TESF was employed here as a supportive technique. Immobilization is critical for creating an adequate environment for wound healing by eliminating disruptive shearing forces. Research in humans has shown that TESF can improve flap survival, particularly in lower-extremity reconstructions. 23 Despite physiological and anatomical differences, similar conclusions on the benefits of immobilization can be drawn for cats. 24 However, the use of TESF showed a 19% complication rate, primarily owing to implant failure and superficial pin tract infection. 25
A bandage or cast could have been considered for stabilization. Their use comes with significant risks such as soft tissue injuries, pressure sores, erythema and necrosis, particularly with prolonged application or improper fitting.26,27 One study reported soft tissue complications in 63% of cases involving casts in distal limbs, highlighting the importance for careful case selection and cautious application. 27 In addition, cats show poor tolerance for external coaptation. 26 TESF was preferred as it provides immobilization without circumferential compression, which is beneficial in the presence of fragile or compromised skin. Minor complications were observed in our cases.
A type I TESF was positioned medially, owing to the availability of safer anatomical corridors. 28 Epoxy resin was used for its low weight, versatility and to reduce soft tissue irritation. This technique has been shown to support soft tissue healing and does not impede wound drainage or management, even in the presence of open injuries.29,30 The TESF was left in place for 3 weeks, slightly longer than the 2-week duration recommended for skin healing. This decision was made because of the chronic nature of the wounds and their location over the calcaneus, where delayed healing is more likely. The relatively short duration of fixation contributed to the low complication rate observed, as prolonged fixation is often associated with higher risks of pin-tract infections and implant failure. 25
Conclusions
A single pedicle advancement flap associated with TESF was successfully used to manage chronic wounds on the calcaneal region in two cats. The flap allowed effective wound coverage in a challenging anatomical location. The combination of TESF with this technique minimized tension of the skin over the calcaneus by immobilizing the joint, thereby maximizing chances of successful healing.
Footnotes
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognized high standards (‘best practice’) of veterinary clinical care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS Open Reports. Although not required, where ethical approval was still obtained, it is stated in the manuscript.
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animal(s) described in this work (experimental or non-experimental animals, including cadavers, tissues and samples) for all procedure(s) undertaken (prospective or retrospective studies). For any animals or people individually identifiable within this publication, informed consent (verbal or written) for their use in the publication was obtained from the people involved.
