Abstract
Case series summary
Three adult cats were successfully treated for severe anaemia caused by a bleeding hard palate ulcer with a temporary palatal guard. Each cat required a blood transfusion and underwent surgical implantation of a customised temporary guard to protect the hard palate mucosa from ongoing irritation. The palatal guards were made from radiographic film in two cases and an acetate sheet in the third. Cats received varied concurrent treatments in conjunction with surgery, including amoxicillin/clavulanate or doxycycline, cyclosporine and prednisolone. Complete resolution of the hard palate ulceration and anaemia was observed in all three cases.
Relevance and novel information
Excessive licking can lead to mucosal erosion of the hard palate, delayed healing and severe haemorrhage. When a palatine ulcer is refractory to medical management or the anaemia is severe, surgical intervention may be required. Techniques previously described include electrocautery, horizontal mattress sutures and ligation of the palatine artery combined with a bipedicle mucoperiosteal flap. These techniques typically require advanced surgical skills or access to specific equipment, may involve repeat surgeries to correctly isolate the palatine artery, and may leave a secondary wound that could prolong anorexia or risk becoming a new site of haemorrhage. Placement of a temporary customised palatal guard is a novel surgical technique for the treatment of bleeding palatine ulcers that does not require isolation of the palatine artery, involves minimal tissue handling, provides immediate control of oral pain, encourages immediate return to appetence and prevents ongoing trauma to the area during healing.
Introduction
Feline palatine ulceration, or ‘Menrath ulcer’, is a condition that can cause severe life-threatening anaemia. 1 In the cat, the palatine arteries course rostrally from the major palatine foramina at the level of the fourth premolars to the palatine fissures and become superficial in the rostral hard palate.2,3 Repeated trauma by abrasive papillae on the feline tongue during excessive grooming can erode the palatine mucosa, leading to exposure of the palatine artery and haemorrhage. Palatine ulcers can be difficult to identify because of the intermittent nature of the haemorrhage; 4 however, in severe cases, they can require immediate surgical haemostasis and blood transfusion. 5
This paper presents a novel technique and associated outcome of a surgically implanted temporary palatal guard to treat three cats with palatine ulceration.
Case series description
Case 1
A 3-year-old castrated male Exotic Shorthair cat presented for acute haematemesis and anaemia. The cat had a history of flea infestation, chronic pruritus and recurrent lip ulcers previously treated successfully with prednisolone (1 mg/kg PO q24h, Pred-X; APEX). A complete blood count (CBC) showed a regenerative anaemia with a haematocrit of 0.07 l/l (reference interval [RI] 0.3–0.45). The cat received a fresh feline whole blood transfusion (type unknown owing to an incomplete record) and oral examination revealed a right palatine ulcer.
Under general anaesthesia, a steam-sterilised, single layer of radiographic film (polyethylene terephthalate [PET], Fujifilm Medical X-Ray Film; Fujifilm) was placed over the hard palate and cut to size intraoperatively by tracing around the lingual aspect of the upper dental arcade. The film was sized to be located under the medial cusps of the upper carnassial teeth (fourth premolars). The location of the fixing screw was marked on the guard, which was then removed, and screw holes were drilled using a 1.1 mm drill bit. The guard was replaced in the oral cavity and the screw holes extended into the palate mucosa and underlying maxillary bone. The guard was then attached to the hard palate bone using four 1.5 mm (6 mm length) cortical bone screws and metal washers (Figure 1). Sterile saline was flushed under the guard to ensure minimal direct contact with the mucosa. Postoperatively, the cat was treated with methadone (0.1 mg/kg IM q4h, Methadone; Ilium) and cyclosporine (6 mg/kg PO q24h, Atopica; Elanco). A transient pyrexia occurred 2 days postoperatively (temperature 39.7°C), which resolved with amoxicillin/clavulanic acid (15 mg/kg PO q12h for 10 days, Amoxyclav; Zoetis).
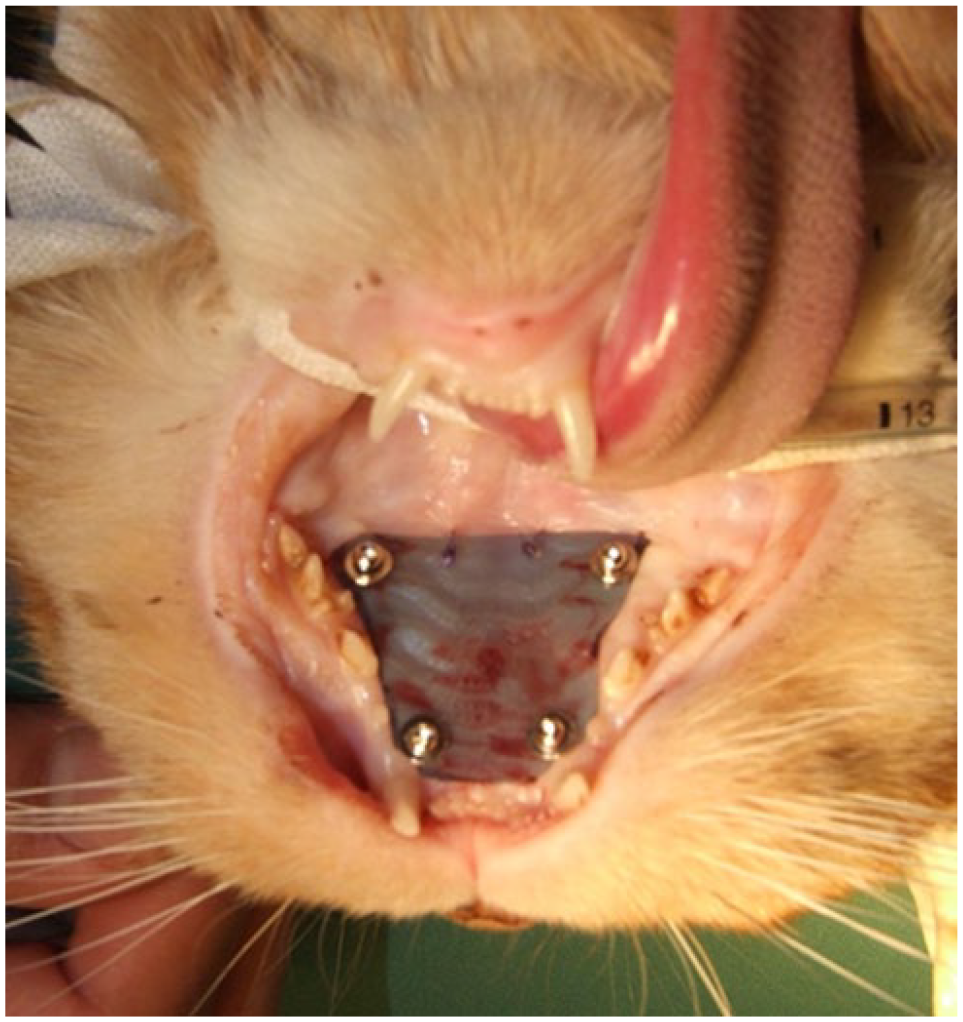
Case 1: palate guard in situ made of polyethylene terephthalate film secured to the hard palate using four cortical bone screws and washers, and two simple interrupted sutures on the caudal margin.
Six days postoperatively, the ulcer was persistent with minor food contamination under the palatal guard. By postoperative day 19, the ulcer had resolved and the guard was removed under general anaesthesia. Granulation tissue was present 24 h after screw extraction. No further palatine ulceration was noted at the last follow-up 1 month postoperatively.
Case 2
A 16-year-old spayed female domestic shorthair cat presented for severe anaemia, oral bleeding and melena. The cat had a 6-week history of lethargy, sparse hair coat and suspected flea allergy dermatitis. CBC showed a regenerative anaemia. Haematocrit reduced from 0.25 l/l to 0.13 l/l (RI 0.3–0.45) over 3 days. Serum biochemistry, platelet indices and coagulation tests, including prothrombin time (PT) and activated partial thromboplastin time (APTT), were reported to be within normal limits (no access to laboratory results). The cat received two feline whole blood transfusions, and a left palatine ulcer was identified (Figure 2a).

Case 2: (a) a left-sided palatine ulcer and (b) the respective palate guard in situ made of polyethylene terephthalate film secured to the hard palate using four cortical bone screws and washers, and three simple interrupted sutures on the caudal margin.
The ulcer was biopsied under general anaesthesia with a 2 mm skin biopsy punch (Sterile Dermal Biopsy Punch; KAI Medical) and closed with a 4-0 polydioxanone simple (PDS) interrupted suture (PDS II; Ethicon). A steam-sterilised, single layer of PET radiographic film (Fujifilm Medical X-Ray Film; Fujifilm) was cut to size intraoperatively and placed using the methodology described in case 1 (Figure 2b). Excessive pressure through the screw washer and guard was avoided and sterile saline was flushed under the guard to ensure minimal mucosal pressure. In this case, the caudal margin of the implant was secured to the soft palate using three 4-0 PDS sutures (PDS II; Ethicon) to prevent food contamination. Histopathology indicated focal necrotising stomatitis.
Postoperatively, the cat received methadone (0.1 mg/kg IM q4h, Methadone; Ilium), iron dextran (10 mg/kg IM, Feron; Elanco), amoxicillin/clavulanic acid (16 mg/kg PO q12h for 14 days, Amoxyclav; Zoetis), cyproheptadine (0.5 mg/kg PO q12h for 14 days, Periactin; Merck), cyclosporine (6 mg/kg PO q24h until loss of follow-up, Atopica; Elanco) and flea control. Seven days postoperatively, the guard was partially removed and the wound assessed to be healing appropriately. On day 18, the mucosa had completely healed and the guard was removed. A right lingual ulcer was identified at this time but resolved after 5 days. No recurrence was reported at the last follow-up 7 months postoperatively.
Case 3
A 3-year-old spayed female domestic shorthair cat presented for severe anaemia, oral bleeding, haematemesis, melaena and ptyalism. The cat had a history of chronic pruritus, and a 1-week history of stomatitis managed with sucralfate (500 mg PO q8h, Carafate; Aspen Pharmacare) and omeprazole (1 mg/kg PO q24h, Losec; AstraZeneca). Oral examination revealed a right palatine ulcer. The initial haematocrit was 0.25 l/l (RI 0.3–0.48). Biopsies carried out by the referring veterinarian showed an ulcerative stomatitis. The cat subsequently presented with a haematocrit of 0.08 l/l (RI 0.3–0.48), which improved without intervention to 0.19 l/l. Surgery was initially declined and the cat received iron polymaltose (10 mg/kg IM once, Ferrosig; Sigma) and prednisolone (1 mg/kg PO q24h for 7 days then tapered, Pred-X; APEX).
Five days later, the cat presented with a haematocrit of 0.14 l/l (RI 0.3–0.48), which increased to 0.15 l/l after a 20 ml transfusion of type B feline whole blood. A mild transfusion reaction was noted (facial oedema and pyrexia), leading to discontinuation of the remaining transfused volume. Under general anaesthesia, a steam-sterilised single-layer, 250 µm-thick transparent acetate sheet (polyvinyl chloride; Meter) was placed over the ulcer and cut to size intraoperatively. Screw holes were pre-placed following the methodology used in cases 1 and 2. The implant was attached to the hard palate bone using four 1.5 mm (6 mm length) cortical bone screws and metal washers, along with two rostral and four caudal simple interrupted 4-0 PDS sutures (PDS II; Ethicon) ensuring a gap with the underlying mucosa (Figure 3a).

Case 3: (a) oral cavity at time of surgery and (b) immediately after removal of a palate guard made of polyvinyl chloride acetate sheet and secured to the hard palate using four cortical bone screws and washers, along with four caudal margin and two rostral margin simple interrupted sutures. Screw holes (yellow arrows) and healing ulcer (blue arrowhead) are evident
The cat received methadone (0.1 mg/kg IM q4h for 24 h, Methadone; Ilium), buprenorphine (0.02 mg/kg PO q12h for 5 days, Bupredyne; Jurox) and doxycycline (5 mg/kg PO q12h for 10 days, Doxy 50; APEX). Prednisolone (Pred-X; APEX) was reduced (0.5 mg/kg PO q24h for 7 days) then tapered over 3 weeks. Weekly visual assessments were performed with a conscious oral examination feasible because of a transparent implant. At 28 days postoperatively, the implant was removed under general anaesthesia and the ulcer had epithelial tissue covering the mucosal defects (Figure 3b). At the latest follow-up, 2 months postoperatively, the palatine ulcer had healed with no visual evidence of recurrence and the haematocrit was 0.34 l/l (RI 0.3–0.48).
Discussion
Palatine erosion in cats typically occurs with excessive grooming as a result of pruritic skin disease 2 and has been reported in connection with insect bite allergies, food allergies, bacterial or viral infections, atopy, 6 gingivostomatitis, 7 squamous cell carcinoma 8 and eosinophilic granuloma complex. 6 The cases in this report had chronic skin hypersensitivities; however, neoplastic lesions can be visually indistinguishable from inflammatory lesions.8,9 Biopsy of all oral inflammatory lesions is recommended before treating a palatine ulcer.
Previously described surgical treatment options for actively bleeding palatine ulcers include electrocautery, 10 horizontal mattress sutures 2 and palatine artery ligation combined with a bipedicle mucoperiosteal flap. 11 Although these conventional methods are effective, they can be overly invasive or technically demanding. They may require multiple surgeries to successfully isolate the affected artery or location, can require advanced surgical skills, and leave a wound that may prolong anorexia and delay wound healing. 12 The authors acknowledge that some of these techniques may be simpler in practice; however, at the time of presentation, all owners expressed concern about the chronic nature of the problem, and because of financial constraints, were seeking an immediate solution. In the absence of active haemorrhage, the authors therefore elected to pursue this novel approach of implementing a palatine guard as the first surgical intervention. The palatal guard described provides a physical barrier that eliminates oral pain during eating, promotes immediate normal feeding and allows for an uninterrupted healing process. Correctly applied, the palate guard technique may also be advantageous for some practitioners as it does not require the knowledge or significant undermining of mucosa to perform a mucosal flap technique. However, in the case of strong pulsatile bleeding, this technique would need to be supplemented with direct ligation of the palatine artery.
The described technique utilises inexpensive and easily obtainable materials and is relatively quick and easy to apply. Although the surgical application time was not recorded for each patient, general anaesthetic durations were in the range of 31–39 mins. In review, surgical application of the guards was relatively quick and the major time-limiting steps included customising the shape of the acrylic guard, carefully pre-drilling the hard palate and hand-driving the respective screws into the hard palate. The authors are of the opinion that this novel alternative approach for treating feline palatine ulcers can be readily applied in the clinical setting as the only specific tools required include a surgical drill, a 1.1 mm drill bit, and 1.5 mm cortical screws and washers.
One disadvantage of the described novel technique is the requirement for anaesthesia in patients that are potentially compromised by low haematocrits. Other potential risks include the use of cortical screws in the hard palate breaching the nasal cavity floor, causing neurovascular injury or dental injury to tooth roots. Anatomical knowledge is required to ensure correct screw placement in the lateral aspect of the palate while avoiding tooth roots and the major palatine artery exiting the major palatine foramen medial to the fourth maxillary premolar, approximately halfway between the dental arch and median plane. An important consideration during screw application is avoiding excessive pressure to reduce the risk of mucosal necrosis from an incorrectly fitted guard. The shortest available 1.5 mm cortical screws were 6 mm. When used with appropriately sized washers and the acrylic guard itself, no nasal cavity penetration was observed during screw placement. A limitation of this study is the lack of postoperative radiographs to confirm implant positioning; however, the authors recommend obtaining postoperative radiographs in future cases to ensure proper placement.
The materials used for the reported palatal guards were sourced opportunistically within the clinic, chosen for their softness, flexibility and resistance to tearing or folding. Radiographic film was used in the first two cases, while a clear acetate sheet was used in the third. The authors found that an appropriately sized implant would lock in place dorsal to the fourth premolar cusps. Use of the clear acetate guard allowed visualisation of the underlying mucosa without the need for removal. Suture placement at the caudal periphery of the implant helped minimise the risk of food becoming trapped under the guard. The palatal guard was shaped to avoid placing pressure on the underlying mucosa, either from excessive tightening or from bends in the guard material.
Complications associated with the guard were minimal and included one case of infection, which resolved with antimicrobial therapy, and one transient lingual ulcer that resolved spontaneously without intervention. Ensuring a low-profile implant with smoothed margins before application can help reduce the risk of iatrogenic ulceration. Although limited by a small sample size, the aim of this case series was to present an alternative technique to traditional interventions that may be impractical or contraindicated. Further research into less traumatic techniques that cause less iatrogenic tissue damage to the hard palate or tongue is warranted. One such approach may involve the use of ultraviolet light-cured dental acrylic to create a temporary palate guard anchored to the teeth rather than the hard palate.
The success of this treatment depended on the concurrent management of the underlying aetiology. All cases received antibiotic and anti-inflammatory or immunomodulatory therapies before palatal guard placement without resolution of the underlying pruritis. The treatments were continued after placement of the palatal guard, which led to resolution of both the ulcer and the underlying condition, with no recurrence observed.
Conclusions
Palatine ulceration should be considered a differential diagnosis in cats presenting with regenerative or microcytic anaemia and clinical signs such as oral bleeding or melaena. Surgical intervention may help expedite mucosal healing and prevent ongoing haemorrhage. Biopsy at the time of guard placement is recommended to rule out neoplasia or unusual infection. In the three reported cases, surgical implantation of a temporary palatal guard, alongside management of the underlying pruritic condition, resulted in complete resolution of both the chronic ulcers and associated anaemia.
Footnotes
Acknowledgements
We would like to express our appreciation to Dr Emily Pritchard, who generously provided her knowledge, expertise and feedback in writing this research article, and to Dr David Simpson for his support and feedback. Additionally, this endeavour would not have been possible without the support and facilities provided by the Animal Referral Hospital, Homebush, NSW, Australia, which is where these cases were managed.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The work described in this manuscript involved the use of non-experimental (owned or unowned) animals. Established internationally recognised high standards (‘best practice’) of veterinary clinical care for the individual patient were always followed and/or this work involved the use of cadavers. Ethical approval from a committee was therefore not specifically required for publication in JFMS Open Reports. Although not required, where ethical approval was still obtained, it is stated in the manuscript.
Informed consent
Informed consent (verbal or written) was obtained from the owner or legal custodian of all animal(s) described in this work (experimental or non-experimental animals, including cadavers, tissues and samples) for the procedure(s) undertaken (prospective or retrospective studies). No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.
