Abstract
Human papillomavirus (HPV)-associated cancers (oropharyngeal, cervical, vulvar, vaginal, anorectal, and penile cancers) have previously been reported to have favorable survival outcomes making patients’ quality of life (QoL) an important consideration for clinicians. This scoping review examined the literature on the post-treatment psychosocial QoL outcomes in patients HPV-associated cancers in the United States. The final set of 57 articles were comprised of patients that predominantly identified as Non-Hispanic White, females, or those with cervical or gynecologic cancers. Physical and psychological QoL were the most studied domains. Qualitative studies demonstrated salient themes including low health literacy on HPV-associated cancers, decreased sexual well-being, and increased feelings of stress and fear. Future work is needed in understanding psychosocial QoL in non-gynecologic HPV-associated cancers among individuals from underrepresented racial/ethnic groups, male patients, and those of lower socioeconomic status. Additionally, cancer-related stigma is relatively understudied among patients with HPV-associated cancers.
Introduction
Human papillomavirus (HPV) is the sexually transmitted infection (STI) with the highest prevalence and incidence in the United States (US), accounting for 13 million new cases per year. Similarly, high rates are seen worldwide, with a global pooled prevalence of 31% for any genital HPV and 21% for high-risk HPV(Bruni et al., 2023). HPV infection, primarily with the high-risk types 16 and 18, has been associated with oropharyngeal, cervical, vulvar, vaginal, anorectal, and penile cancers (Hirth, 2019). In the US, cervical and oropharyngeal cancers (OPCs) remain the most common HPV-associated malignancies in women and men, respectively (Liao et al., 2022). The main risk factors for developing cervical cancer among women include having multiple sexual partners, having oral sex, and being immunosuppressed (Moscicki and Palefsky, 2011; Stanley et al., 2012). In contrast, OPCs, particularly HPV-associated OPCs (HPV-OPCs), are distinct entities that have been associated with the number of oral sex partners (Drake et al., 2021). However, the relationship between oral HPV infection and oropharyngeal squamous cell carcinoma (OPSCC) is complex, with nuances related to the timing, intensity of oral sex, and the type of sexual partner, further impacting the risk (Drake et al., 2021). The natural history of OPSCC differs from that of cervical cancer, with certain pre-lesions seen in cervical cancer that are absent in OPC. This makes the trajectory of OPSCC development less clear (Agalliu et al., 2016). While certain studies have indicated a higher prevalence of oral HPV infections among men who have sex with men, it is important to note that a direct association between sexual orientation and increased risk of HPV-OPC has not been conclusively established (Drake et al., 2021; Heck et al., 2010).
The epidemiological history of HPV-associated cancers and vaccination is important in contextualizing how the burden of these malignancies has shifted in affecting different demographic groups in the US. OPSCC was first recognized in 2009. In 2006, the Food and Drug Administration (FDA) recommended vaccination against high-risk HPV infection to decrease cervical cancer rates. The FDA’s Advisory Committee on Immunization Practices (ACIP) initially approved Merck Gardasil®, as a three-dose schedule for females aged 9-26 in 2006 for protection against four aggressive HPV strains (Slade et al., 2009). Gardasil® was later approved for males aged 13-21, as well as up to age 26 in high-risk male individuals; vaccination for all males up to age 26 was later approved in 2015 (Centers for Disease Control and Prevention, 2021a; Daley et al., 2017). In 2015, the FDA approved Merck’s multivalent version of the Gardasil® vaccine, which covered five additional oncogenic HPV strains (Markowitz et al., 2018; Slade et al., 2009). By 2018, vaccination was approved for both women and men ages 27-45 (Markowitz et al., 2018; Slade et al., 2009).
Public health campaigns to prevent cervical cancer through vaccination and enhanced screening have significantly reduced its age-adjusted incidence and disease burden (Van Dyne et al., 2018). In contrast, HPV-OPCs have seen a marked rise, especially in males. The incidence of OPC in men has recently exceeded that of cervical cancer in women, though the exact timing of this shift differs among studies (Centers for Disease Control and Prevention, 2021a; Centers for Disease Control and Prevention, 2021b; Lechner et al., 2022; Van Dyne et al., 2018). While cervical cancer and OPCs are the primary HPV-associated malignancies in women and men, respectively (Liao et al., 2022), HPV-OPCs in males now represents the most widespread HPV-linked cancer (Centers for Disease Control and Prevention, 2021a). HPV-OPCs currently affect younger individuals with fewer behavioral risk factors, such as heavy tobacco or alcohol consumption. HPV-associated anorectal cancers predominantly impact female patients (Liao et al., 2022; Lin et al., 2019; Saleem, 2011), and individuals with compromised immune systems, especially those with human immunodeficiency virus (HIV) (Walsh et al., 2015; Ye et al., 2020). Moreover, young individuals of color identifying as sexual and gender minorities face a higher incidence and prevalence of HIV (Koenig et al., 2016), which is a known risk factor for reduced HPV viral clearance and subsequent anorectal cancer development (Walsh et al., 2015; Ye et al., 2020).
Previous research indicated that HPV-associated cancers yield better health outcomes than non-virally mediated malignancies in similar anatomical sites (Guerendiain et al., 2022; Kugelman et al., 2022; Wang et al., 2015). Given their favorable prognosis and younger patient demographics, post-treatment survivorship and quality of life (QoL) become crucial. QoL, encompasses daily physical, emotional, and social functions reflects the interplay between a disease’s physiological factors and patients’ psychological experiences (Penson et al., 2006; Wilson and Cleary, 1995). These cancers, tied to behavioral risk factors like sexual activity, offer unique insights into patient QoL. Few studies have explored psychosocial distress in HPV-associated cancer patients. Compared to the general populace, OPC patients face higher depression and anxiety risks (Qualliotine et al., 2017), and exhibit reduced QoL (Hammermüller et al., 2021). Notably, previous research suggests HPV-positive oropharyngeal cancer patients experience more depressive symptoms than their HPV-negative counterparts (Bauman et al., 2016; Dodd et al., 2019). Studies also highlight the shame, embarrassment and guilt experienced among patients with HPV-associated anogenital and gynecological cancers (Leppard, 2016; Longabaugh, 2017; McCaffery et al., 2006).
This scoping review aimed to examine the existent literature and evaluate the current body of research on the QoL outcomes studied in patients with HPV-associated cancers, particularly focusing on the psychosocial needs of this unique cancer patient population. Through this scoping review, we aimed to identify areas for further research regarding psychosocial QoL outcomes among this patient population during and after oncological treatment.
Methods
Scoping review methodology offers researchers a key approach in examining both the breadth and depth of the scientific topic of interest (Arksey and O’Malley, 2005). They provide a comprehensive overview through identifying gaps within the literature and topical areas of scholarly engagement without being exhaustive or too cursory (Arksey and O’Malley, 2005; Peters et al., 2015). The frameworks of Arksey and O’Malley (2005) and Levac et al. (2010) were used to guide this scoping review.
Identifying research questions
This scoping review aimed to assess psychosocial QoL outcomes that have been studied, the methodologies employed, and their contexts. Due to the established link between HPV and the majority of anorectal, gynecologic, oropharyngeal, and penile cancers and the introduction of its vaccine, our emphasis was on studies from the post-vaccine era (post-2006).
The guiding research questions explored in this review included: (1) which psychosocial QoL outcomes have been studied and what measures, assessments, or tools have been used to examine these outcomes?; (2) what proportion of these studies included participants of both sexes as well as populations of color?; (3) what analytic approaches have been employed (qualitative, quantitative, mixed-methods)?; and (4) from a geographic perspective, where have these studies been conducted in the US? This broad search approach strategy was used in conceptualizing the present scoping review, since to our knowledge, no prior published work has specifically examined these topics among survivors of HPV-associated cancers.
Identifying relevant studies
Four databases were searched in this scoping review which included: PubMed, Scopus, Web of Science, and CINAHL (Cumulative Index to Nursing and Allied Health Literature). The Boolean search term combinations were created using the following template: “HPV” and “[outcome of interest]” and “[cancer type]”. Examples of search term combinations include: “‘HPV’ and ‘quality of life’ and ‘anal cancer’”; “‘HPV’ and ‘stigma’ and ‘cervical cancer’”; “‘HPV’ and ‘depression’ and ‘oropharyngeal cancer’”; “‘HPV’ and ‘anxiety’ and ‘penile cancer’”; and “‘HPV’ and ‘sexual function’ and ‘vulvar cancer’”. A full list of search terms and their combinations are listed in Supplemental 1.
Study selection
We limited our review to peer-reviewed studies that met the following criteria: (1) based in the US; (2) written in English; (3) analyzed primary or secondary data; (4) were published January 01, 2007 to November 30, 2023; and (5) included adults (>18 years of age) diagnosed with an HPV-associated cancer. Studies were excluded if they were: (1) abstracts presented at scientific meetings, (2) dissertations/theses; (3) basic science studies involving non-human subjects research conducted in laboratory settings; (4) editorials or opinion pieces; or (5) other literature reviews of data syntheses.
The final list of combined Boolean search terms generated an initial set of articles imported into an EndNote library (n = 38,685) for screening. After the removal of the duplicates (n = 19,263), the study team (SV, QC, JS, and AR) initially screened the abstracts from the remaining articles (n = 19,422) and coded each article using the inclusion and exclusion criteria (Figure 1). In this phase, each article was screened independently by two team members. A third team member reconciled coding differences. This methodological approach minimized individual biases from each team member in the screening process. The remaining articles (n = 1344) were subjected to full-text reviews using the same approach as the screening phase, whereby a final set was generated for the analyses (n = 57). Figure 1 outlines the study selection methodology in the form of a PRISMA flow diagram. PRISMA flow diagram of article selection process.
Data extraction
General information extracted from each article included the author, publication year, study type, geographic location of study, demographics (if available) of the study population, study outcomes, and main study findings. Each article was read by one member of the research team and reviewed by another member during team meetings where discussions focused on thoroughly assessing the trends and broader themes of the literature.
Results
Demographics by sex, race, and geographic region
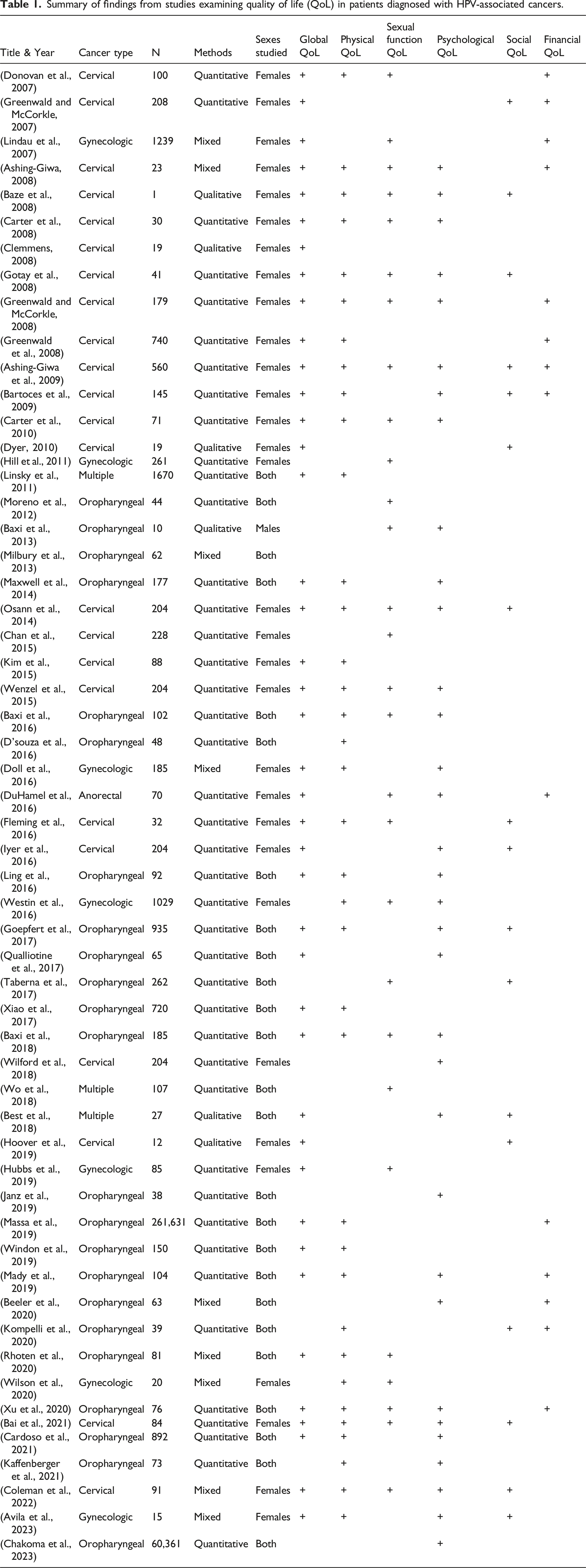
Summary of findings from studies examining quality of life (QoL) in patients diagnosed with HPV-associated cancers.

Types of HPV-associated cancer studies by year.
Approximately half of the studies (54%; n = 31) exclusively recruited female patients. Twenty-three (40%) of the studies were conducted among patients of both sexes. Only one study (2%) exclusively recruited male patients. Within the subset of studies that examined patients with OPCs (n = 23), 65% of participants were male (n = 213,245), and 36% were female (n = 105,394). The only study conducted among patients with anorectal cancer exclusively recruited female patients. One qualitative study on emotions and fears associated with a diagnosis of OPC consisted only of male participants, whereas another study on anorectal cancer assessed only female individuals’ sexual QoL.
Of all studies that reported a breakdown of participants by ethnic or racial group, an aggregate of 64% of participants identified as Non-Hispanic White (n = 214,989). The aggregate sample was represented by 17% (n = 57,167) of participants that identified as Asian American/Pacific Islanders, 9% (n = 30,897) Black/African American, and 7% (n = 24,073) Hispanic/Latino. Among the studies conducted in patients with gynecologic cancers, 63% identified as Non-Hispanic White (n = 171,751), 20% as Asian American/Pacific Islander (n = 55,384), 9% as Black/African American (n = 25,975), and 5% as Hispanic/Latino/a (n = 13,745). For studies among those with OPC that provided a breakdown of race or ethnicity, aggregate proportions were represented by 65% Non-Hispanic White (n = 214,041), 17% Asian American/Pacific Islander (n = 57,162), 9% Black/African American (n = 30,834), and 7% Hispanic/Latino/a (n = 23,735). Figure 3 outlines the breakdown of participants in the included studies by race/ethnicity. While those that identify as Non-Hispanic White represent most of the sample, fluctuations in proportions were seen among other racial and ethnic groups across studies (Figure 3). HPV-associated cancer studies by race/ethnicity.
Analytical methods and outcome measures
Among the 57 final articles, 73% (n = 42) relied on quantitative methodologies such as survey research and employed regression modeling to assess patient QoL. Mixed quantitative and qualitative methods were employed by 16% (n = 9) and 11% (n = 6) of studies, respectively. Surveys or questionnaires used by both subsets were validated tools used in prior studies assessing different aspects of QoL, including global QoL, physical QoL, psychological QoL (depression, anxiety), sexual intimacy and function, social QoL, and financial QoL.
Studies assessing the domain of global QoL employed the following instruments: Functional Assessment of Cancer Therapy (FACT-G or its cancer-specific variations, n = 11), European Organization for Research and Treatment of Cancer Quality of Life Questionnaire (EORTC-QLQ, n = 6), Short Form Survey developed by the Medical Outcomes Study (SF-12 or 36, n = 4), and University of Washington Quality of Life Questionnaire (UW-QoL, n = 4). Physical QoL was assessed with the following instruments: FACT-G (n = 11), SF-12 (n = 4), UW-QoL (n = 4), the EuroQol 5-dimension Questionnaire (EQ-5D, n = 3), and the Quality of Life Patient/Cancer Survivor Version Scale (QOL-CSV, n = 1). Psychological QoL was examined with the following instruments: FACT-G (n = 8), SF-12 or 36 (n = 4), UW-QoL (n = 4), Brief System Inventory 18 (BSI-18, n = 5), Center for Epidemiologic Studies Depression Scale (CES-D, n = 4), and the Patient Health Questionnaire-9 (PHQ-9, n = 2). Sexual QoL was surveyed with the Female Sexual Function Index (FSFI, n = 7), the Sexual Adjustment Questionnaire (SAQ, n = 6), and the Gynecologic Problem Checklist (GPC, n = 3). Social QoL was examined in studies that used the Medical Outcomes Social Support Survey (MOSS, n = 3), and items from the SF-12 or 36 (n = 3). Studies assessing financial QoL utilized elements from the EORTC-QLQ (n = 4), MOSS (n = 3), and the Comprehensive Score for Financial Toxicity (COST, n = 2). Among the studies included in this scoping review that employed quantitative methods, most used regression modeling to predict outcomes on QoL measures based on pre-existing conditions at the time of assessment. Quantitative studies typically sought to establish prevalence of various QoL outcomes among long-term cancer patients and survivors.
Qualitative studies (n = 6) represented 11% of the final set of included articles. These studies employed methodologies such as participant interviewing and thematic analyses. Through semi-structured or unstructured interviews, study authors elicited patient narratives to form the basis for needs assessments and hypothesis generation. Across qualitative studies or mixed methods studies that utilized more than one interviewee, thematic analysis identified common themes or phenomena across multiple participants’ responses regarding their QoL outcomes. Mixed methods studies generally relied more on survey data similar to quantitative studies and supplemented with anecdotal evidence from patient interviews to generate conclusions. Across all quantitative, qualitative, and mixed methods studies, 18 studies specifically incorporated author-designed surveys or interview questions.
Global QoL was assessed in a majority of studies (72%, n = 41). Among the subtypes of QoL, physical QoL was the most common outcome (63%, n = 36), of which pain and fatigue were the most surveyed physical symptoms. Sexual QoL outcomes was the next most commonly studied outcome, which primarily focused on sexual function (49%, n = 28). Psychological QoL was assessed in 58% of studies (n = 33) as either anxiety (49%, n = 28) or depression (46%, n = 26). Financial QoL (25%, n = 14), such as socioeconomic status (SES), insurance status, and financial toxicity, and social QoL (30%, n = 17) such as social support were the least common outcomes assessed. Three out of six studies assessing stigma were qualitative studies that drew from patient perspectives and interviews.
Qualitative and mixed methods studies highlighted several key findings on psychosocial outcomes from patient interviews. Firstly, there was a notable knowledge gap concerning HPV-associated cancers. Patients did not know that their cancers were caused by or strongly associated with prior HPV infection. Secondly, the significance of physician-patient communication was underscored. Two studies showed that improved communication could enhance prevention rates and patient comprehension of long-term management. Thirdly, studies emphasized the substantial impact on sexual function and intimacy among HPV cancer survivors. The lack of early discussions on these issues with physicians was identified as an area in clinical medicine needing improvement to significantly lower sexual health-related morbidity. Another study emphasized reinterpreting the survivorship experience to positively influence patient QoL. Fourthly, considerable stigma, stress, and fear were linked to HPV-associated cancers, often rooted in the guilt, shame, and embarrassment about acquiring the infection through sexual behavior. Lastly, financial burdens associated with HPV cancer treatments emerged as a concern, potentially affecting long-term QoL and treatment adherence.
Discussion
Research gaps among demographic groups
This scoping review highlights the current foci of HPV-associated cancer survivor subgroups included within the QoL literature and the QoL domains examined. Our findings show that the current body of literature has mainly focused on individuals diagnosed with HPV-associated cervical or gynecologic cancers (53%, n = 30), and predominantly recruited patients identifying as non-Hispanic White (64%) or exclusively female (54%, n = 31). Racial/ethnic minorities, males, and other types of HPV-associated cancers are largely underrepresented in research, and SES is not well-characterized.
Underrepresented patient populations by race/ethnicity & sexual orientation
The underrepresentation of racial/ethnic minorities and underserved populations in cancer research has previously been identified as a pressing challenge for the field of oncology (Simon et al., 2014). Biomedical oncologic research has shown that when looking at over 230,000 biospecimens collected from cancer patients, 88% of the samples originated from patients who self-identified as non-Hispanic White. Our findings mirror this disparity and highlight the underrepresentation of ethnic/racial minorities in socio-behavioral research focusing on QoL of patients with HPV-associated cancers. Although the final set of articles reviewed had wide racial diversity with most of the studies including some patients of color, these groups still generally represented small proportions of participants across these studies. The underrepresentation of racial/ethnic groups within the QoL literature regarding HPV-associated cancers is further magnified when considering that the average annual percentage change (AAPC) in incidence was increasing significantly among particular patient subgroups and cancer types (Liao et al., 2022). For example, while anorectal HPV-associated cancers increased in both non-Hispanic White and Black patients from both sexes, non-Hispanic Black males represented the demographic subgroup with the largest increase in AAPC (Liao et al., 2022). The findings from our scoping review and the continuing demographic changes in the epidemiology of HPV-associated cancers in the US collectively call for future research exploring the QoL of patients with these cancers, particularly those of underrepresented racial/ethnic groups.
Another underrepresented demographic group worth noting was individuals with HPV-associated cancers that identify as sexual minorities. Only one qualitative study specifically analyzed the effect of sexual orientation on patients’ experiences with these cancers (Best et al., 2018). Research has shown that individuals who identify as lesbian, gay, or bisexual (LGB) have significantly higher odds of being diagnosed with cancer, regardless of type, when compared to their heterosexual counterparts of the same sex at birth (Gonzales and Zinone, 2018). Patients who identify as sexual minorities have been found to have increased risks of developing HPV-associated cancers (Quinn et al., 2015). Bisexual females face higher rates of cervical cancer than their heterosexual counterparts (Boehmer et al., 2011). Transgender men and women have been identified as a neglected population with respect to surveillance, prevention, and screening of HPV-associated cancers, making them one of the demographic subgroups at higher risk (Brown et al., 2017). Taken together, the notable underrepresentation of sexual minorities in HPV-associated cancer research warrants future work to include this uniquely vulnerable population to be included in QoL studies.
Patient populations of lower SES and risk of financial toxicity
Regarding financial QoL, only 25% (n = 14) of the studies included in this review reported or examined participant SES, detailing participants’ insurance and/or income status. Despite the advent of modern oncology therapies improving overall health outcomes, these advancements carry significant financial implications for patients, paralleling the physical and psychological challenges post-diagnosis. Approximately 22% to 64% of cancer patients express concern about paying their medical bills (Ell et al., 2008) and they are 2.5 times more likely to face bankruptcy than their healthy counterparts (Ramsey et al., 2013). Income has been previously identified as a predictor of overall QoL, influencing patients’ physical, emotional, and role functioning (Roick et al., 2019). Recent oncology literature has discussed financial toxicity, which is defined as the monetary burden and downstream consequences of receiving healthcare for complex medical conditions like cancer. These studies revealed an association between cancer patients reporting financial toxicity and decreased health-related QoL, reduced survival rates, and diminished treatment adherence (Lathan et al., 2016; Neugut et al., 2011; Ramsey et al., 2016; Zafar et al., 2015). Given that individuals with lower SES tend to have a limited awareness of HPV and its link to cancer (Chido-Amajuoyi et al., 2020), our findings suggest that financial QoL and financial toxicity in HPV-associated cancer patients is an under-researched yet critical area for future studies.
Sex at birth
The majority of studies (54%, n = 31) in the final set recruited and included exclusively female patients. Only one study exclusively included male patients with OPC (Baxi et al., 2013). Among the studies that included both males and females, males comprised 65% (n = 213,761) of the study population. When looking at the epidemiologic trends of HPV-associated cancers between 2001 and 2017 across all anatomic sites (including malignancies affecting the reproductive organs of both sexes), female patients represented approximately 60% of all virally related cases of which 71% were gynecologic cancers (cervical, vaginal, or vulvar) (Liao et al., 2022). It is important to note that while screening methods for HPV-associated gynecologic cancers, particularly cervical cancer, exist and are relatively efficient due to the identifiable precancerous lesions, there is currently no established screening method for OPC. This is largely because OPC lacks recognizable precancerous lesions, making developing efficient screening strategies challenging (Kepka et al., 2016). A recent study by Liao et al. (Liao et al., 2022) reported a significant increase in the AAPC in all HPV-associated cancers among male patients, particularly oropharyngeal and anorectal cancers. As previously discussed, the landscape of HPV-associated cancers is changing such that male patients represent an increasing proportion of those affected by these virally related malignancies (Centers for Disease Control and Prevention, 2021a; Centers for Disease Control and Prevention, 2021b; Liao et al., 2022; Van Dyne et al., 2018). The observed epidemiological shift in OPC may be influenced by several factors: the rise in HPV infection rates, including potentially long-standing oral infections; the success of cervical cancer screening and vaccination initiatives affecting cervical cancer trends; and traditional risk factors like alcohol and smoking. While cervical cancers have shown changes possibly linked to interventions, HPV-associated OPC has a longer development timeline, making the immediate impact of preventative measures less evident. Additionally, it is worth noting that screening for precancerous oropharyngeal lesions is currently not feasible (Chaturvedi et al., 2018; Finneran et al., 2021; Osazuwa-Peters et al., 2017). Collectively, the findings from this scoping review additionally highlight the relatively understudied area of QoL research, particularly among males with HPV-associated cancers.
Heterogeneity of QoL measures
This scoping review evaluated the aspects of QoL and the measures used to study patients with HPV-associated cancers. The primary domains of QoL investigated were: global, physical, sexual function, psychological, social, and financial. Notably, most studies assessed the physical (63%, n = 36) or sexual function (49%, n = 28) domains of QoL. Of the 28 studies focusing on sexual function, 20 (71%) exclusively included female patients with HPV-associated cancers, predominantly those with gynecologic cancers. Among the seven studies that examined sexual function in both male and female patients, six were among those with OPCs. Notably, no studies in our final set of articles addressed the psychosocial QoL of males with penile cancers. This aligns with the relative rarity of penile cancers among all of the HPV-associated cancers (Liao et al., 2022). Our findings underscore the research gap in understanding sexual function in males with HPV-associated cancers across all anatomical sites and in patients of both genders with virally mediated anorectal cancers.
Furthermore, psychological QoL was predominantly gauged using surrogate markers for anxiety, depression, and stress rather than established measures. These markers are inherently symptomatic, so their precision in identifying genuine clinically significant psychological distress or mood disorders may be limited. Our findings align with recent work by Silver et al. (Silver et al., 2023), which underscored a paucity of research specifically focusing on the psychosocial aspects of quality of life in OPC patients. They highlighted the importance of addressing these patients’ emotional, social, and mental well-being, reporting that many past studies were geographically limited and varied in their methodological approaches. This further emphasizes the need for consistent and comprehensive psychosocial QoL measures in the context of HPV-associated cancers.
Among the studies included in this scoping review, the measures employed in assessing psychological QoL ranged from elements borrowed from general QoL questionnaires such as the FACT-G, SF-12/36, and UW-QoL, or specific psychological QoL surveys such as the BSI-18, CES-D, and PHQ-9. The heterogeneity and varying degrees of depth between instruments made it difficult to assess specific psychological QoL across multiple studies. Aspects of psychological QoL that warrant further exploration are the rates of psychological distress and clinically significant mood-related psychiatric disorders among patients diagnosed with HPV-associated cancers using validated psychiatric diagnostic tools, such as the PHQ-9 and GAD-7.
Exploring the role of stigma & social support
Of the articles included in this scoping review, only five addressed stigma’s impact on patients’ QoL. In the broader cancer patient population, stigma prevalence varies from 18 to 80% (Cho et al., 2013; Ernst et al., 2017; Phelan et al., 2013; Yilmaz et al., 2020). Over 30% of cancer survivors harbor negative views towards their cancers, and about 10% feel discriminated against due to their diagnosis (Cho et al., 2013). The challenge in studying this area lies in its complexity and the diverse methods of measuring cancer-related stigma across studies (Fujisawa and Hagiwara, 2015; Huang et al., 2021). Certain cancer patient subgroups, such as male patients, individuals with lower SES, and those with concurrent mood-related disorders (i.e., depression or anxiety), tend to experience heightened stigma (Huang et al., 2021). This review highlights the existing gap in the literature addressing stigma in HPV-associated cancer patients.
Both tobacco-associated and HPV-associated cancers are tied to individual behavioral risk factors. The stigma surrounding lung cancer, often associated with smoking, has been well documented (Brown Johnson et al., 2014; Chambers et al., 2015; Ostroff et al., 2019). Confirmed HPV infection leads to higher stigma levels, largely attributed to HPV being an STI and the subsequent perception of promiscuity (Daley et al., 2015; Shepherd and Gerend, 2014). Furthermore, increased public awareness due to HPV vaccine promotions has intensified stigmatization among HPV-associated cancer patients (Bachman et al., 2018; Wearn and Shepherd, 2020). Past research indicates these patients are often perceived as unwise, dishonest, and unclean compared to patients with other cancers (Shepherd and Gerend, 2014). Much like lung cancer patients, those with HPV-associated cancers are often perceived as responsible for their condition due to assumed risky behaviors (Lebel and Devins, 2008; Lebel et al., 2013). Given these factors, future research on HPV-associated cancer patients should prioritize understanding stigma, especially considering their predisposition to psychosocial distress.
Lastly, 30% (n = 17) of the studies addressed social support as a QoL aspect post-diagnosis. Given the associated stigma with HPV, there is a pressing need for further research into how these patients perceive and seek social support following diagnosis.
Study limitations
There are several limitations present in this study. As the goal of this scoping review was to provide a general overview of the literature on HPV-associated cancers and identify topic areas for future research questions, the final set of articles analyzed was produced with liberal exclusion criteria and was not as exhaustive as those found in systematic reviews. Individual rater biases were attempted to be minimized with the screening and iterative methodology. The present review excluded studies conducted at institutions or populations outside of the US. These studies were excluded to minimize the heterogeneity in the patient populations when conducting our analyses.
Conclusions
To the best of our knowledge, this is the first scoping review examining which psychosocial aspects of QoL have been studied in patients with HPV-associated cancers. The current body of research in this area is primarily focused on non-Hispanic White female patients diagnosed with cervical or other gynecologic cancers. Our analyses identified significant gaps in this literature, particularly regarding the lack of inclusion of patients from underrepresented racial/ethnic groups, males, and individuals of lower socioeconomic status. The studies included in this review demonstrate a broad range of QoL measures with differing domains of focus. This heterogeneity presents a challenge when drawing meaningful comparisons across multiple studies. It underscores the need for more standardized methodologies and measures to facilitate an integrated and comprehensive understanding of QoL among patients with HPV-associated cancers. Finally, despite HPV being the most common STI in the US and the associated stigmatization from the virus, the examination of cancer-related stigma is notably sparse in the context of HPV-associated cancers. Future research should also include a more nuanced exploration of the psychological, social, and financial aspects of QoL. Comprehensive and inclusive studies will enable the development of more targeted and effective interventions to improve the QoL of all patients with HPV-associated cancers.
Supplemental material
Supplemental Material - Psychosocial aspects of quality of life outcomes in post-treatment human papillomavirus-associated cancer survivors in the United States: A scoping review
Supplemental Material for Psychosocial aspects of quality of life outcomes in post-treatment human papillomavirus-associated cancer survivors in the United States: A scoping review by Seiichi Villalona, Aravind Rajagopalan, Qianwei Chen, Julie Sumski and Sharon Manne in Health Psychology Open
ORCID iD
Seiichi Villalona https://orcid.org/0000-0003-2442-576X
Statements and Declarations
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
