Abstract
The aim of this review was to conduct a meta-synthesis of the experiences and perceptions of self-management of type 1 diabetes of children and young people living with type 1 diabetes (CYPDs). Six databases were systematically searched for studies with qualitative findings relevant to CYPDs’ (aged 8–18 years) experiences of self-management. A thematic synthesis approach was used to combine articles and identify analytical themes. Forty articles met the inclusion criteria. Two analytical themes important to CYPDs’ experiences and perceptions of self-management were identified: (1) negotiating independence and (2) feeling in control. The synthesis contributes to knowledge on contextual factors underpinning self-management and what facilitates or impedes transition towards autonomous self-management for CYPDs.
Introduction
Type 1 diabetes (T1D) is a relatively common chronic illness that frequently has its onset in childhood and adolescence (Mayer-Davis et al., 2018). Management of T1D is onerous and includes frequent blood glucose monitoring, administering insulin and balancing insulin requirements with food and exercise. The unrelenting nature of these tasks is burdensome for children and young people living with type 1 diabetes (CYPDs; Hood et al., 2006). During adolescence, metabolic control tends to deteriorate (Cameron et al., 2018). This deterioration is partly physiological because of pubertal insulin resistance and partially related to reduced adherence to T1D management, engagement with risk taking behaviours (Cameron et al., 2018) and difficulties engaging with self-management (Campbell et al., 2014).
The ability of CYPDs to carry out T1D management is dependent on cognitive, motor and emotional maturity levels, and these levels may determine which T1D management tasks the CYPDs are ready to assume responsibility for and take ownership of (Hanna and Decker, 2010; Silverstein et al., 2005). Though adolescents may have the necessary motor skills to complete the tasks of T1D management, research indicates that parents maintaining involvement in their children’s care lead to better medical outcomes (Markowitz et al., 2015). Self-management of T1D involves sharing responsibilities with others such as parents and healthcare professionals (HCPs), and autonomous decision-making, with the goals of achieving control over health and well-being (Schilling et al., 2002). While parental involvement is important for T1D management, it can impact on parent–adolescent relationships with research indicating that CYPDs and their parents may experience T1D-related conflict and that parents and CYPDs may not always agree about the level of competence of the CYPDs to carry out T1D management tasks independently (Butner et al., 2009; Hood et al., 2007). Childhood and adolescence is a critical time for children and young people (CYPs) living with a chronic illness to gradually develop autonomy in chronic disease management, with complete autonomy in health-related tasks and decision-making often arriving in late adolescence (Beacham and Deatrick, 2013).
Previous reviews have synthesised CYPDs’ experiences of living with T1D (Ellis and Jayarajah, 2016; Spencer et al., 2010) and of managing T1D (Kelo et al., 2011; Marks et al., 2016; Rankin et al., 2017) in specific contexts such as health service provision at paediatric diabetes clinics (Curtis-Tyler et al., 2015) or T1D management in school settings (Kelo et al., 2011; Marks et al., 2016). Of these reviews, none synthesised evidence specifically relating to CYPDs’ experiences and perceptions of self-management of T1D. Experiences of younger children (under 12 years) have been recently synthesised (Rankin et al., 2017). Therefore, given the developmental differences that occur across age groups, a synthesis of older children and adolescent experiences of self-management of T1D in day-to-day contexts may contribute to knowledge and allow current qualitative evidence relating to this group to be collated.
As late childhood and adolescence is an important time when CYPDs assume increasing self-management responsibilities and where management difficulties and parental conflict can occur, aggregation and further interpretation of research around CYPDs’ experiences of self-management is warranted. This suggests a need for a synthesis of evidence from wider contexts, including studies that focus on experiences in settings beyond schools and also explicitly considering all attributes of self-management which include activities, processes and goals (Schilling et al., 2002). Understanding how CYPDs experience self-management of T1D may inform HCPs and others involved in the care of CYPDs on how best to assist families of CYPDs which in turn may lead to improvements in clinical and psychosocial outcomes. The aim of this review was, therefore, to conduct a meta-synthesis of qualitative studies exploring experiences and perceptions of self-management of CYPDs (age 8–18 years).
Method
This systematic review and qualitative meta-synthesis was conducted and reported in accordance with the Enhancing Transparency in Reporting the Synthesis of Qualitative Research (ENTREQ) statement (Tong et al., 2012).
Search strategy
A search for eligible articles, from database inception up to 26 July 2018, was undertaken across six electronic databases; PubMed, Medline via Ovid, EMBASE, CINAHL, PsycINFO and Web of Science (Web of Science Core Collection). A search strategy combining controlled vocabulary (e.g. MESH) and free-text words was created and adapted to each database (see example search strategy in Appendix A in the supplementary material). The search strategies reflected the meta-synthesis’ focus on CYPDs, T1D, self-management and qualitative methodologies. Searches were limited to articles published in English and studies carried out with human participants. The search in EMBASE was limited to records unique to EMBASE.
Article selection criteria
Articles were selected for inclusion if they (1) were empirical, peer reviewed articles published in English; (2) included CYPDs aged 8–18 years of age (or where data for this group could be clearly disaggregated from other data collected in the article, for example, if parents, individuals aged over 18 years or individuals living with other conditions were also included); (3) included qualitative data pertaining to the experience of self-management of T1D (mixed methods, intervention or quantitative studies with open-ended questions were included if qualitative data were reported separately). Any qualitative studies (1) that explicitly examined self-management of T1D from CYPDs’ (8–18 years) perspectives as the primary focus of the study, (2) that examined self-management of T1D from CYPDs’ perspectives as a sub-focus of a larger study or (3) where findings pertaining to self-management of T1D from CYPDs’ perspectives emerged as a theme or sub-theme, or formed part of a theme or sub-theme were included. Self-management was considered as a range of behaviours, carried out as part of illness management and the promotion of well-being, that have relevance to medical, psychological and social outcomes. Based on the definition used by Panagioti et al. (2014), included studies had to mention actions taken by an individual to lead a healthy lifestyle, care for their condition, meet psychosocial needs and prevent complications or further illness. Table 1 summarises the inclusion and exclusion criteria of the qualitative meta-synthesis.
Inclusion and exclusion criteria.
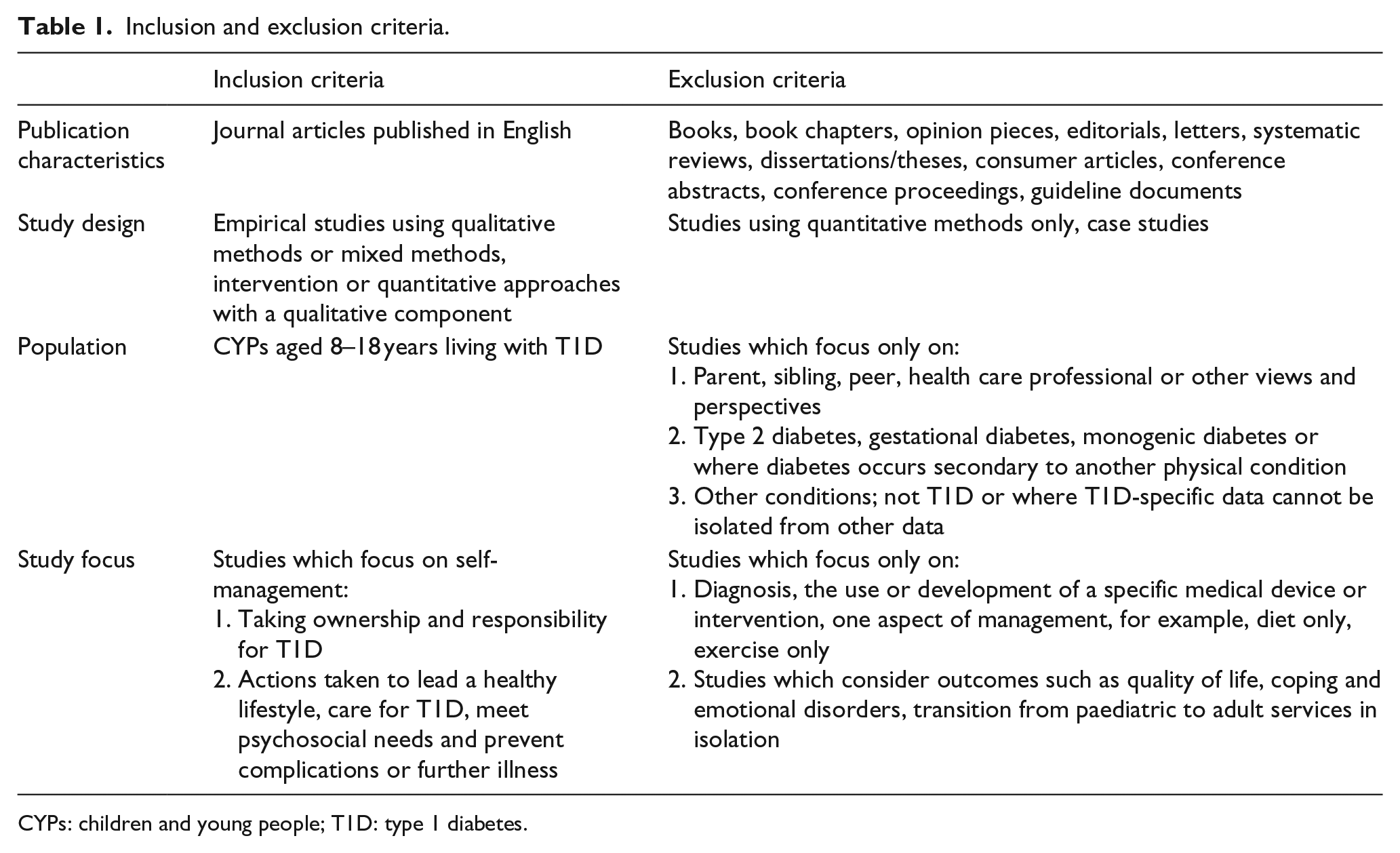
CYPs: children and young people; T1D: type 1 diabetes.
Screening process
After removing duplicate articles across the databases, a two-stage screening process was undertaken to identify eligible articles that met the inclusion criteria:
Two reviewers (E.T., C.R.) independently screened retrieved titles and abstracts;
E.T. and C.R. independently read full-texts of retrieved articles. E.T. screened reference lists for potentially eligible articles. Discrepancies were resolved through discussion with two further reviewers V.L. and P.G.
Data extraction
The following information was extracted for each article: author, year, country of origin, aim/objective, recruitment setting, sample, data collection method, analytical approach and findings. Data were extracted by E.T. and cross-checked by C.R.
Methodological quality of included studies
Included articles were independently assessed for methodological quality by E.T. and C.R. using the Critical Appraisal Skills Programme (CASP) (2018) which assesses methodological quality across 10 items. Reviewers indicated whether each checklist item was addressed within the article using yes, no or can’t tell. Discrepancies were resolved through discussion and where a decision could not be reached, V.L. and/or P.G. resolved the discrepancy. Quality appraisal aided critical consideration of the methodologies and findings of included articles.
Qualitative meta-synthesis method
In this qualitative meta-synthesis, thematic synthesis (Thomas and Harden, 2008), comprising of three stages, was used to combine primary studies. An inductive thematic synthesis was carried out without an a priori framework for analysis, as described by Thomas and Harden (2008): (1) Line-by-line coding of the available text found in the results and findings sections of included articles. At least one code was applied to each section of relevant data. Codes were examined, and where necessary an additional level of coding was applied before the final list of codes was generated. (2) Descriptive themes were developed through grouping resulting codes according to similarities, differences and patterns across the codes. Descriptive themes were labelled based on the data which they were describing and remained close to the findings of the primary studies. (3) Analytical themes were developed by ‘going beyond’ the initial study findings to produce the synthesis product which may indicate new concerns, issues or recommendations in light of the topic under investigation (Barnett-Page and Thomas, 2009). Analytic themes were inferred based on the descriptive themes and the initial review question posed. The results/findings sections of included studies were extracted verbatim and entered into NVivo 11 software for analysis (QSR International Pty Ltd, 2015).
Results
After a systematic search yielding 5341 articles, 40 articles reporting on 34 studies were included (see Figure 1 and Table 2).
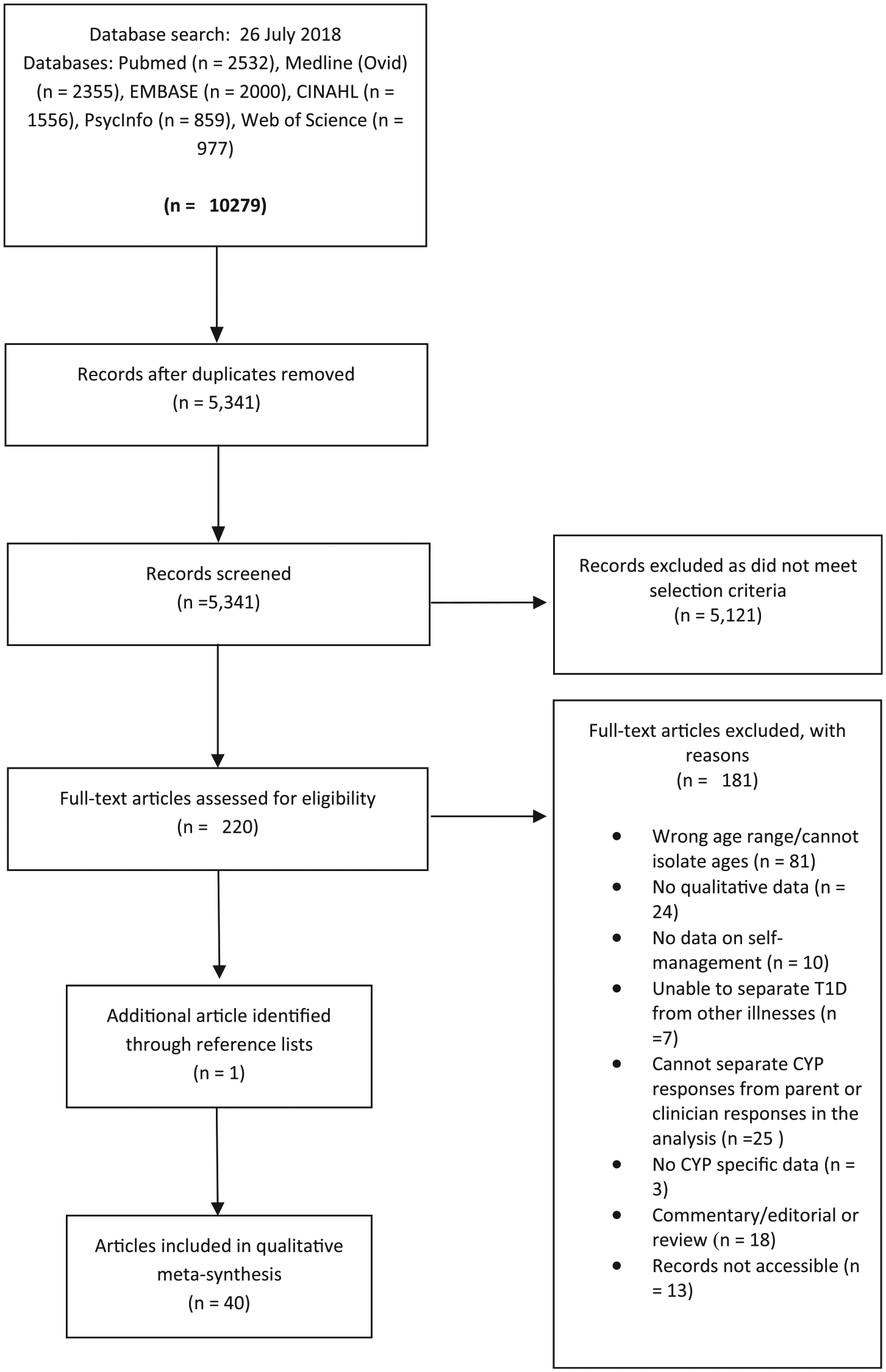
Flow diagram representing flow of article identification and selection process.
Overview of included articles.
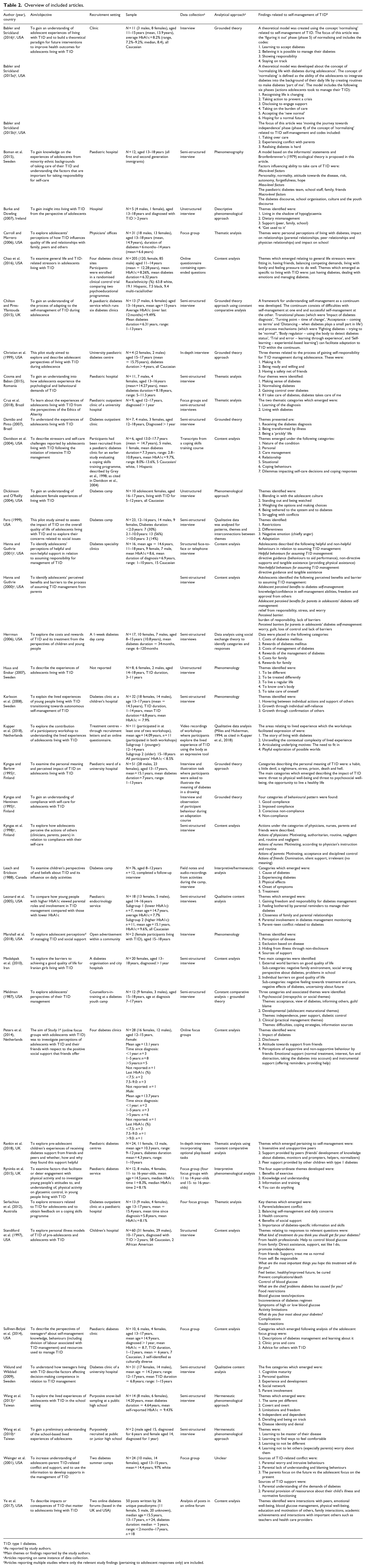
T1D: type 1 diabetes.
As reported by study authors.
Main themes or findings reported by the study authors.
Articles reporting on same instance of data collection.
Articles reporting multiple studies where only the relevant study findings (pertaining to adolescent responses only) are included.
Characteristics of included studies
In total, there were 862 participants in the 34 studies (across 40 articles). Of the 34 studies which reported data on separate participants, 30 provided a breakdown of the gender of participants (50% male and 50% female). Included articles were published between 1987 and 2018. Articles originated from the United States (n = 19), Sweden (n = 4), Finland (n = 3), the United Kingdom (n = 3), Taiwan (n = 2), Netherlands (n = 2), Ireland (n = 1), Romania (n = 1), Brazil (n = 2), Canada (n = 1), Iran (n = 1) and Australia (n = 1). The majority of participants were recruited from doctor’s offices, clinics or hospitals (n = 22). Other recruitment settings were through diabetes camps (n = 6), not specified (n = 2), a national diabetes organisation and hospital (n = 1), open advertisement in community (n = 1), online forum (n = 1) or school (n = 1).
The data reported in each article were collected via interviews (n = 25), focus groups (n = 5), open-ended questionnaire (n = 1), a combination of interview and an illustration task (n = 1), interviews and focus groups (n = 1), field notes and audio-recording of diabetes camp activities (n = 1), interview and observation (n = 1), interview and play-based task (n = 1), transcripts from coping skills training meetings (n = 1), recording of a workshop (n = 1), online forum posts (n = 1) and online focus groups (n = 1). The approaches to analysis reported by the included articles were content analysis (n = 13), phenomenology (n = 9), grounded theory analysis (n = 9), thematic analysis (n = 5) and other type of analysis or unclear (n = 4). Characteristics and findings of included studies are summarised in Table 2.
Quality appraisal
The results of the quality appraisal are detailed in Appendix B in the supplementary material. Where articles received no or can’t tell ratings, it was unclear whether the area for appraisal was addressed. This may have been a feature of the reporting within the particular article rather than the methodological quality of the research. For example, it was often not possible to assess the appropriateness of the recruitment strategy or whether the researcher–participant relationship had been adequately considered due to insufficient information reported, and these articles often received no or can’t tell ratings.
Thematic synthesis findings
The synthesis of the findings of the 40 included articles resulted in the identification of two analytic themes associated with CYPDs’ experiences of self-management of T1D: ‘Negotiating independence’ and ‘Feeling in control’. The eight descriptive themes that contributed to these analytic themes are outlined in Table 3. The analytic and descriptive themes with example quotations to illustrate how themes were developed are presented in Table 4. The numbers of extracts coded for each descriptive and analytic theme, and the contribution of each individual article to the development of the descriptive and analytic themes are presented (see Appendix C in the supplementary material).
Overview of analytic themes and descriptive themes.
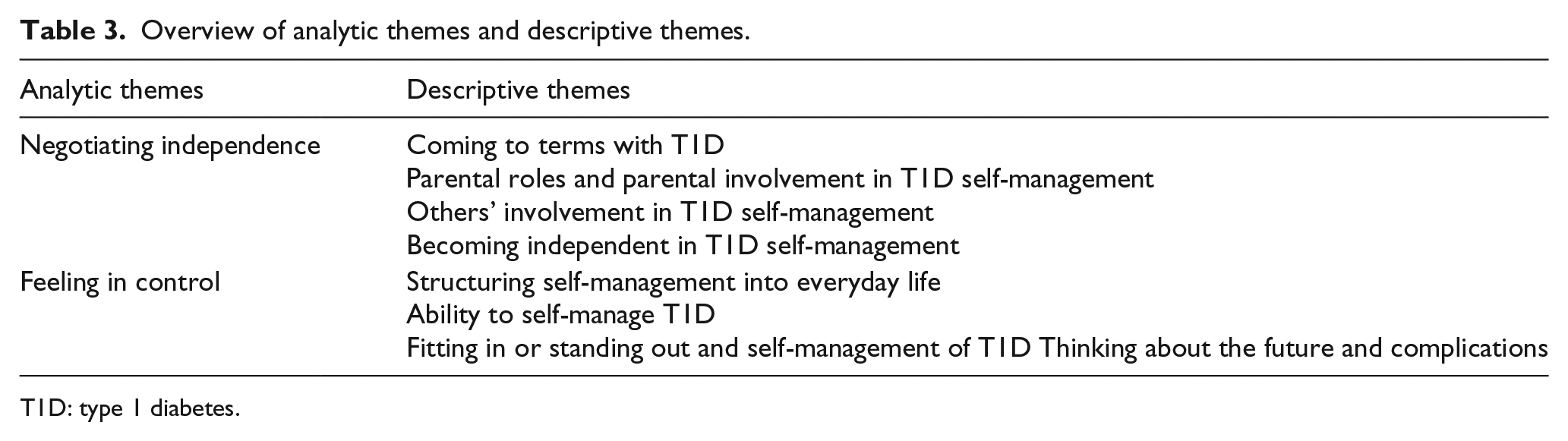

T1D: type 1 diabetes.
Qualitative meta-synthesis: analytic themes, descriptive themes, example codes and illustrative quotations.

T1D: type 1 diabetes.
Negotiating independence
This analytic theme reflects balancing the demands of living with and managing T1D and how this occurs as CYPDs interact with others while moving towards independence in T1D self-management. The analytic theme presents the dynamic nature of the movement towards independence and outlines how internal (in the descriptive theme ‘Becoming independent in T1D self-management’) and external (‘Parental roles and parental involvement in T1D self-management’ and ‘Others’ involvement in T1D self-management’) factors may feature within this move towards autonomous self-management. CYPDs gradually accept T1D as a part of their lives, often moving from an initial point of non-acceptance, and how this occurs may influence engagement with self-management for CYPDs as they navigate the process of becoming independent in their self-management (‘Coming to terms with T1D’). The demands of self-management may be negotiated with others such as parents or HCPs. The demands of self-management may also be negotiated internally by the CYPDs as they become independent in all aspects of their lives while also becoming independent in T1D self-management.
Coming to terms with T1D
This descriptive theme depicts adapting to the requirements of living with T1D, which is a process that occurs over time. The prospect of lifelong self-management of T1D is introduced at diagnosis and may be marked by feelings of uncertainty, fear, sadness or confusion (Babler and Strickland, 2015a; Cosma and Baban, 2015; Leach and Erickson, 1988). The diagnosis experience may have relevance for current feelings and health beliefs held towards T1D as feelings about diagnosis, time since diagnosis or level of maturity may influence the CYPDs’ acceptance of T1D self-management (Chilton and Pires-Yfantouda, 2015; Cosma and Baban, 2015; Damião and Pinto, 2007).
Following initial resistance and questioning in relation to a T1D diagnosis, CYPDs spoke about beginning to accept the lifelong nature of T1D (Chilton and Pires-Yfantouda, 2015). CYPDs contend with living with T1D, adjusting to diets and insulin pumps and indicate how specific management activities were initially considered challenging (Babler and Strickland, 2016; Cosma and Baban, 2015; Damião and Pinto, 2007; Dickinson and O’Reilly, 2004; Herrman, 2006). This acceptance was evident in descriptions of getting used to T1D as adjustment to a ‘new reality’ (Cosma and Baban, 2015: 237). Acceptance of T1D involves coming to the realisation that T1D is part of life and is manageable (Babler and Strickland, 2015a, 2015b, 2016; Herrman, 2006; Meldman, 1987). CYPDs may consider management of T1D to be more arduous than the demands posed by other illnesses (Babler and Strickland, 2015a; Carroll and Marrero, 2006; Meldman, 1987; Wang et al., 2013). In contrast, others may frame a diagnosis of T1D positively (Babler and Strickland, 2016; Chilton and Pires-Yfantouda, 2015; Marshall et al., 2018; Meldman, 1987; Wang et al., 2013).
Parental roles and parental involvement in T1D self-management
Parents’ involvement in the management of their child’s care can range from general assistance with specific tasks such as calculating doses to reminding the CYPDs to do ‘everything’ (Leonard et al., 2005: 410). Parental involvement may be less tangible, relating to just knowing that parents are ‘there’ and as a result of this, the CYPDs feel that they do not always have to ‘think all the time what I have to do next’ (Cosma and Baban, 2015: 239). This can then alleviate the burden posed by self-management. Parents may temporarily take over management, which may be viewed positively by the CYPDs (Viklund and Wikblad, 2009).
Parents can motivate the CYPDs to assume an active role in self-management through incentivising responsibility for independent self-management (Hanna and Guthrie, 2001). As parents hand over responsibility for T1D management, they balance this with the readiness of the CYPDs to assume an active role (Babler and Strickland, 2015a, 2015b, 2016; Carroll and Marrero, 2006; Chao et al., 2016; Cruz et al., 2018; Hanna and Guthrie, 2000, 2001; Huus and Enskar, 2007; Karlsson et al., 2008; Kyngas et al., 1998; Leonard et al., 2005; Meldman, 1987; Sullivan-Bolyai et al., 2014; Viklund and Wikblad, 2009; Wang et al., 2013).
When not restricted to times when the CYPDs need parental assistance with a specific aspect of their management, conflict and frustration can ensue (Leonard et al., 2005); this is evident in situations where parental involvement was perceived as nagging (Babler and Strickland, 2015a, 2015b, 2016; Boman et al., 2015; Carroll and Marrero, 2006; Cosma and Baban, 2015; Davidson et al., 2004; Dickinson and O’Reilly, 2004; Herrman, 2006; Huus and Enskar, 2007; Kyngas et al., 1998). However, parental involvement is valued by CYPDs (Dickinson and O’Reilly, 2004), especially when additional assistance is needed such as during a hypoglycaemic incident (Cruz et al., 2018; Maslakpak et al., 2010). Therefore, CYPDs’ responses to parental input may vary depending on the situation.
Others’ involvement in T1D self-management
Self-management of T1D for CYPDs also occurs in the context of others’ (in addition to parents) involvement and in the presence of others. Friends (Babler and Strickland, 2016; Boman et al., 2015; Burke and Dowling, 2007; Carroll and Marrero, 2006; Christian et al., 1999; Cosma and Baban, 2015; Damião and Pinto, 2007; Dickinson and O’Reilly, 2004; Herrman, 2006; Huus and Enskar, 2007; Karlsson et al., 2008; Kupper et al., 2018; Kyngas et al., 1998; Kyngas and Hentinen, 1995; Maslakpak et al., 2010; Rankin et al., 2018; Serlachius et al., 2012; Standiford et al., 1997), extended family (Boman et al., 2015; Burke and Dowling, 2007; Christian et al., 1999; Cosma and Baban, 2015; Hanna and Guthrie, 2001; Herrman, 2006; Leonard et al., 2005; Maslakpak et al., 2010; Standiford et al., 1997), teachers (Burke and Dowling, 2007; Carroll and Marrero, 2006; Christian et al., 1999; Cosma and Baban, 2015; Dickinson and O’Reilly, 2004; Herrman, 2006; Maslakpak et al., 2010; Ryninks et al., 2015; Sullivan-Bolyai et al., 2014; Wang et al., 2013) and HCPs (Boman et al., 2015; Carroll and Marrero, 2006; Christian et al., 1999; Dickinson and O’Reilly, 2004; Karlsson et al., 2008; Kyngas and Barlow, 1995; Kyngas et al., 1998; Kyngas and Hentinen, 1995; Meldman, 1987; Standiford et al., 1997; Sullivan-Bolyai et al., 2014; Viklund and Wikblad, 2009; Ye et al., 2017) are also present as CYPDs learn about and carry out self-management. Attending hospital appointments and interacting with HCPs becomes the norm (Boman et al., 2015). CYPDs begin working with HCPs in relation to their T1D management through setting targets, identifying areas for improvement (Sullivan-Bolyai et al., 2014) and beginning to rely on their own judgements and capabilities in their interactions with HCPs (Kyngas and Hentinen, 1995). CYPDs may move towards collaboration with HCPs rather than passively receiving advice (Boman et al., 2015; Karlsson et al., 2008; Kyngas et al., 1998).
Within the family setting, when family members strive towards common goals such as maintaining healthful habits, this contributes to a context that motivates CYPDs’ independence in T1D management (Herrman, 2006). T1D presents negative impacts when it causes the family stress or inconvenience (Chao et al., 2016; Herrman, 2006; Maslakpak et al., 2010).
Friends of CYPDs may provide support, reminders or possess knowledge on how to assist the CYPDs such as during a hypoglycaemic incident (Wang et al., 2013). Supportive behaviours of others can contribute to formation of beliefs that self-management is within the CYPDs’ capabilities to handle successfully, such as through awareness that friends are available to offer support (Babler and Strickland, 2016; Boman et al., 2015; Carroll and Marrero, 2006; Dickinson and O’Reilly, 2004; Karlsson et al., 2008). Conversely, CYPDs may decide to not involve their peers in their T1D management and may avoid T1D management when in the presence of their friends (Kyngas et al., 1998). CYPDs may struggle to explain T1D to peers who may not have any prior T1D knowledge (Peters et al., 2014). When peers lack knowledge or question the CYPDs, this can contribute to frustration felt towards T1D (Carroll and Marrero, 2006; Leach and Erickson, 1988; Rankin et al., 2018). Therefore, appropriate support and involvement of others may contribute to CYPDs’ engagement of self-management through the creation of supportive settings in which self-management can occur.
Becoming independent in self-management
This theme relates to taking ownership of T1D and becoming self-reliant in self-management tasks and decision-making pertaining to care. Making decisions is a feature of gaining independence in T1D management (Christian et al., 1999; Hanna and Guthrie, 2000; Karlsson et al., 2008; Kyngas et al., 1998; Viklund and Wikblad, 2009). CYPDs strive towards independence in self-management as they come to realise that independence is necessary in order to achieve autonomy (Babler and Strickland, 2015a, 2015b, 2016; Carroll and Marrero, 2006; Cosma and Baban, 2015; Dickinson and O’Reilly, 2004; Hanna and Guthrie, 2000; Serlachius et al., 2012; Standiford et al., 1997; Sullivan-Bolyai et al., 2014; Wang et al., 2013). As CYPDs move from childhood into adolescence, a more collaborative approach where the young person is more actively involved in interactions with HCPs is adopted (Karlsson et al., 2008).
As CYPDs become independent in self-management of T1D, they begin to realise that being prepared, through carrying supplies and having plans in place for hypoglycaemic incidents, is their responsibility. For example, CYPDs will ensure that they are aware of their surroundings, such as when away from the home setting, and ensure that it will be possible to carry out required management tasks when needed (Babler and Strickland, 2015a; Damião and Pinto, 2007; Dickinson and O’Reilly, 2004; Herrman, 2006; Karlsson et al., 2008; Kyngas and Hentinen, 1995; Standiford et al., 1997; Sullivan-Bolyai et al., 2014; Viklund and Wikblad, 2009). Engaging with self-management in a positive manner and carrying out tasks as required is described as a source of ‘comfort’ for CYPDs (Viklund and Wikblad, 2009: 3265).
Feeling in control
This analytic theme relates to the CYPDs’ ability and confidence to engage with self-management of T1D. On a daily basis, CYPDs carry out self-management activities which are incorporated into their life in an individualised way, while also contending with situations where it is necessary to resist the temptation to mismanage T1D (‘Structuring self-management into everyday life’). Carrying out T1D self-management, while believing that medical targets are attainable, may be dependent on holding the belief that self-management is compatible with the CYPDs’ lifestyle in terms of their school life, home life and hobbies.
There are also situations where control is considered beyond the CYPs’ capabilities such as when blood sugar readings fall outside recommended ranges (‘Ability to self-manage T1D’). Living with T1D and engagement with its self-management can lead to CYPDs feeling that self-management causes them to stand out among others, which in turn impacts on CYPDs’ attitudes towards engagement with self-management and their approach to their self-management (‘Fitting in or standing out and self-management of T1D’). Living with T1D may also prompt the CYPDs to consider their future and the potential consequences of not managing T1D in the present (‘Thinking about the future and complications’). This can lead to promotion of engagement with self-management or where control over these potential negative consequences or complications is not perceived as possible, it may contribute to disengagement with self-management.
Structuring self-management into everyday life
This theme relates to how CYPDs incorporate self-management into daily life, including managing high and low blood sugars, making adjustments to insulin dosages and carrying medical supplies (Babler and Strickland, 2015a, 2016; Burke and Dowling, 2007; Carroll and Marrero, 2006; Chao et al., 2016; Chilton and Pires-Yfantouda, 2015; Cosma and Baban, 2015; Faro, 1999; Herrman, 2006; Kyngas and Barlow, 1995; Leach and Erickson, 1988; Maslakpak et al., 2010; Meldman, 1987; Peters et al., 2014; Ryninks et al., 2015; Serlachius et al., 2012; Sullivan-Bolyai et al., 2014; Wang et al., 2010, 2013; Weinger et al., 2001). Difficulties associated with food management and eating in social situations were referred to in a number of articles (Babler and Strickland, 2015a; Burke and Dowling, 2007; Chilton and Pires-Yfantouda, 2015; Cosma and Baban, 2015; Faro, 1999; Leach and Erickson, 1988; Meldman, 1987; Rankin et al., 2018; Viklund and Wikblad, 2009; Wang et al., 2013; Weinger et al., 2001). CYPDs who use an insulin pump describe how its use can increase dietary flexibility; however other CYPDs consider insulin pump management to be incompatible with their lifestyles (Boman et al., 2015; Cosma and Baban, 2015) and for others insulin pumps are not readily available (Cruz et al., 2018).
More generally, adopting a routine in relation to carrying out daily management tasks can lead to the formation of the view that T1D is not overly burdensome (Babler and Strickland, 2015a). Positive and negative aspects of the routine nature of self-management are described in a number of articles (Babler and Strickland, 2015a; Cosma and Baban, 2015; Kyngas and Barlow, 1995; Meldman, 1987; Wang et al., 2010). For some, the benefits of routines are outweighed by the unrelenting nature of T1D management (Babler and Strickland, 2016; Chao et al., 2016; Cosma and Baban, 2015; Davidson et al., 2004; Peters et al., 2014). When the regimen is perceived as restrictive, negative attitudes towards T1D may ensue (Burke and Dowling, 2007; Christian et al., 1999; Cosma and Baban, 2015; Damião and Pinto, 2007; Faro, 1999; Herrman, 2006; Kyngas and Hentinen, 1995; Wang et al., 2013; Weinger et al., 2001). In addition, CYPDs may feel that they do not possess a desirable level of control over the impact of T1D management on their life (Babler and Strickland, 2015b; Davidson et al., 2004).
Successful self-management includes maintaining blood glucose readings within target ranges and becoming familiar with physical symptoms (Herrman, 2006). The physical effects of high or low blood glucose level can limit participation in activities, and this is especially the case when CYPDs have not prepared for their occurrence (Babler and Strickland, 2015a, 2015b, 2016; Burke and Dowling, 2007; Carroll and Marrero, 2006; Chilton and Pires-Yfantouda, 2015; Cosma and Baban, 2015; Faro, 1999; Herrman, 2006; Kyngas and Barlow, 1995; Leach and Erickson, 1988; Maslakpak et al., 2010; Peters et al., 2014; Ryninks et al., 2015; Serlachius et al., 2012; Sullivan-Bolyai et al., 2014; Wang et al., 2010; Weinger et al., 2001).
Inherent with incorporating self-management into daily life is feeling that meeting these daily demands of T1D and other aspects of life is possible. CYPDs may prioritise certain T1D tasks over the demands of social lives and school (Kyngas et al., 1998; Viklund and Wikblad, 2009). This can imply making a conscious decision to stop being ‘lazy’ and actively complete the tasks of T1D management (Babler and Strickland, 2016: 128). When CYPDs avoid or forget to engage with T1D self-management, they may lie about self-management to others (Babler and Strickland, 2015a; Davidson et al., 2004; Kyngas and Barlow, 1995; Kyngas and Hentinen, 1995; Leonard et al., 2005; Weinger et al., 2001) in order to avoid conflict (Babler and Strickland, 2015a; Kyngas and Barlow, 1995).
Living with T1D can lead to feelings of isolation, anxiety and guilt for CYPDs (Kyngas and Barlow, 1995; Maslakpak et al., 2010). In addition, feelings of worry, frustration, burden and stress may be attributed to the requirements imposed by T1D by the CYPDs (Babler and Strickland, 2015a, 2015b; Chao et al., 2016; Kyngas and Hentinen, 1995). Not meeting targets such as desired blood glucose readings can result in worry about upsetting others such as HCPs (Carroll and Marrero, 2006; Dickinson and O’Reilly, 2004).
Ability to self-manage T1D
Individuals’ belief in their ability to self-manage T1D extends beyond the carrying out of management activities to include a more general awareness in terms of one’s competency levels: ‘. . . just feeling that you can take care of it yourself . . .’ (Hanna and Guthrie, 2000: 169). Gaining confidence in self-management abilities can contribute to feeling that control over T1D is possible and that CYPDs are capable of integrating its management into daily life (Babler and Strickland, 2016; Christian et al., 1999; Hanna and Guthrie, 2000). This sense of confidence may be preceded by particular barriers, such as injection fear (Karlsson et al., 2008). CYPDs may also demonstrate that they can exert control over T1D by resisting opportunities for mismanagement (Viklund and Wikblad, 2009). CYPDs may encourage themselves to continue with self-management even during times where the desired results are not easily attained, such as when T1D management is perceived as a burden (Babler and Strickland, 2015a) or when glycosylated haemoglobin (HbA1c) targets are considered unattainable (Boman et al., 2015). When blood glucose levels are within normal ranges for the CYPDs, this can contribute to enhanced perceived control over T1D self-management (Karlsson et al., 2008).
CYPDs gradually gain a sense of control over T1D through learning what works for them personally (Cosma and Baban, 2015; Kyngas and Barlow, 1995; Wang et al., 2013). For some CYPDs, awareness of physical symptoms influences engagement with management of T1D through allowing the CYPDs to judge whether management may be temporarily delayed (Kupper et al., 2018).
Fitting in or standing out and self-management of T1D
Living with T1D may highlight differences between the CYPDs and their peers (Babler and Strickland, 2015a; Faro, 1999; Herrman, 2006; Huus and Enskar, 2007; Kyngas and Barlow, 1995; Kyngas and Hentinen, 1995; Peters et al., 2014; Rankin et al., 2018; Wang et al., 2010, 2013). From the CYPDs’ perspective, being unable to eat in the same manner as friends can emphasise differences that exist (Huus and Enskar, 2007; Wang et al., 2013). CYPDs choose between either fitting in and being like peers or making adjustments to their daily routines for their T1D. In some cases, T1D management is neglected (Babler and Strickland, 2015a; Herrman, 2006; Kyngas et al., 1998; Wang et al., 2013). Others may feel that it is possible to fit in among healthy peers and also live with T1D (Dickinson and O’Reilly, 2004). The CYPDs may secretly manage T1D or may make the decision to not manage by ‘ignoring’ T1D (Boman et al., 2015: 8).
The CYPDs may be treated differently through friends asking questions, parents preventing their participation in activities or teachers highlighting differences (Carroll and Marrero, 2006; Chao et al., 2016; Maslakpak et al., 2010; Weinger et al., 2001). Others in the CYPDs’ life may not always understand T1D and some feel that sport coaches ‘singled them out’. (Dickinson and O’Reilly, 2004: 103). Though the CYPDs may wish to engage fully with teenage life, they may be prevented by parents who they consider overprotective or overinvolved in their care (Carroll and Marrero, 2006). Similarly, differences are perceived through knowing their parents are more worried about them in comparison to friends’ parents (Karlsson et al., 2008). Therefore, the individual CYPDs’ approach to self-management may vary depending on their views on perceived differentness resulting from T1D management.
Thinking about the future and complications
In addition to carrying out self-management in the present, CYPDs also may find themselves considering how living with T1D may impact them in the future. CYPDs are aware that their parents will not be available to provide assistance as they get older (Cosma and Baban, 2015). Therefore, it is important that CYPDs feel that independent management of T1D in the future is possible (Babler and Strickland, 2016). The risks posed by not managing and developing complications in the future are sources of uncertainty or may exacerbate worries in relation to living with T1D (Babler and Strickland, 2015a, 2016; Chao et al., 2016; Christian et al., 1999; Dickinson and O’Reilly, 2004; Faro, 1999; Kyngas and Barlow, 1995; Kyngas and Hentinen, 1995; Meldman, 1987; Ye et al., 2017). Awareness of the consequences of not engaging with self-management can prompt CYPDs to strive to achieve control over T1D (Babler and Strickland, 2016; Chilton and Pires-Yfantouda, 2015; Kyngas and Hentinen, 1995; Standiford et al., 1997). Others may feel that preventing complications is beyond their control and this then causes disengagement with self-management of T1D (Viklund and Wikblad, 2009). Some CYPDs choose to avoid envisaging the risk of complications of T1D (Damião and Pinto, 2007; Weinger et al., 2001). This avoidance may be indicative of feeling that T1D self-management and meeting self-management goals is beyond the CYPDs’ capabilities.
Discussion
This qualitative meta-synthesis systematically examined the available evidence on the experiences and perceptions of self-management of T1D from the perspectives of CYPDs aged 8–18 years. The meta-synthesis provides insight into the complexity of the experience of self-management of T1D, including the considerable time and emotional demands it can place on CYPDs. Moreover, insight is provided into the experience of gaining independence and increasing responsibility for self-management of T1D for CYPDs. The meta-synthesis also highlights the many common experiences and issues that CYPDs encounter across a range of countries and contexts.
Self-management has previously been described as a process of negotiation of illness management and other areas of life in adults living with chronic illness (Audulv et al., 2009). In our meta-synthesis, CYPDs’ descriptions of experiences of negotiating independence have parallels with references to how individuals experience inner conflicts as they encounter barriers to engagement with self-management (Audulv et al., 2009). In the present meta-synthesis, CYPDs negotiate independence in self-management rather than illness management more generally. This underlines the scope for continued development of models of self-management that are specific to the paediatric setting. Future research may also consider exploring adolescent perceptions of becoming independent in self-management rather than focussing on general experiences of living with T1D. This may add depth to knowledge on issues relating to self-management for CYPDs.
In the current review, there are instances where CYPDs describe the positive impact of friends supporting their self-management. Previous research indicates that parents and peer groups do influence metabolic control and engagement with T1D management (Guo et al., 2011), therefore highlighting the importance of others (parents, peers, HCPs, etc.) in contributing to independent engagement with self-management. However, given that CYPDs may vary in their responses to support, further research addressing the influence of the types of support for different age groups on self-management specifically may be warranted. Increasing the awareness of others such as school staff and peers in line with guidelines on management of T1D in adolescence (Cameron et al., 2018) may contribute to ensuring that CYPDs can feel open towards their self-management and lead to settings where independent self-management is facilitated.
Our second analytic theme ‘Feeling in control’ supports Spencer et al.’s (2010) review highlighting factors facilitating or impeding engagement with self-management such as the impact of adolescent level of knowledge, self-efficacy, and peer influences. Previous research indicates that higher levels of self-efficacy and confidence in management abilities are associated with better metabolic control and more engagement with T1D management activities (Iannotti et al., 2006), while this analytic theme highlights the importance of perceived control of T1D and self-management. This sheds further light on the relevance of self-efficacy within conceptualisations of CYPDs’ self-management. Similar to Spencer et al.’s (2010) review, this meta-synthesis also provides some insight into barriers and facilitators to self-management and how these may impact on perceived levels of control over T1D self-management. More in-depth exploration may be warranted in order to delineate barriers and facilitators to engagement with self-management of T1D during childhood and adolescence, as has been conducted in the context of adult chronic illness (Schulman-Green et al., 2012). This may contribute to the development of a model of CYPDs’ self-management of T1D that pays specific attention to the processes of self-management, such as the acquisition of independence and perceived control over T1D, over time.
Our findings indicate that positive experiences and attitudes held by CYPDs towards T1D may contribute to more positive engagement with self-management of T1D that promotes the transitioning of responsibilities for self-management. Differences in how CYPDs respond to the involvement of others’ (parents, peers, school staff, HCPs, etc.) in their self-management indicate the importance that those involved in the CYPDs’ care adopt approaches that are individualised to the CYPDs. In addition, the review highlights the importance of the role of others in promoting independence in self-management and also how others’ reactions can enhance feelings of perceived control of T1D. Consideration that childhood and adolescence presents a unique set of demands lends to the importance of combining studies which take this developmental period and the unique demands of T1D management into account. This may then eventually contribute to the development of supports that are tailored to CYPDs.
The theme ‘Feeling in control’ also encompasses the role of perceived normality or difference between the CYPDs and others. In the context of childhood and adolescent chronic illness, adhering to treatment regimens does contribute to feelings of differentness among CYPs living with chronic illness (Lambert and Keogh, 2015). Previous research carried out in the adult context on self-management indicates adults’ feelings on normality and stigmatisation as a result of chronic illness can impede engagement with self-management (Audulv et al., 2009). However, in order to understand the impact of increasing responsibilities for self-management during childhood and adolescence, further research which investigates feelings of normality on self-management during this time of transitioning autonomy is required.
When T1D self-management is engaged with positively, the improvements in CYPDs’ physical and emotional well-being can enhance feelings of control over T1D. In addition, fostering more long-term goals may contribute to positive engagement with self-management. Fear or powerlessness towards abilities to minimise complications may also be experienced. This indicates that it may be important for others, such as parents and HCPs to be mindful that the CYPDs’ perceived control over T1D may contribute to differences in engagement with T1D treatment and is suggestive of a need for individualised approaches.
This qualitative meta-synthesis provides an important contribution to knowledge as it is, to the authors’ knowledge, the first qualitative meta-synthesis that aims to combine qualitative evidence on CYPDs’ (8–18 years) experiences of self-management of T1D. The scope of this meta-synthesis advances existing reviews by incorporating specific evidence on the self-management experiences of CYPDs aged 8–18 year and captures an influential developmental stage as self-management patterns transition to adolescent dominant (Schilling et al., 2006). However, this meta-synthesis also highlights the difficulties of isolating data across a relatively wide age range. Articles included varied with respect to the amount of contextual data presented, such as methodologies and participant characteristics, and therefore, it was not possible to report on all contextual factors for all studies. Including these characteristics within published reports minimises the risk of decontextualising findings of primary research during the conduct of the meta-synthesis (Thomas and Harden, 2008). A potential limitation of our search strategy is the lack of a uniform definition of self-management with much divergence in the reporting of definitions employed across studies (Barlow et al., 2002), meaning relevant studies may have been missed. In the current meta-synthesis, a broad search strategy was employed which encompassed several terms that are related to self-management.
In conclusion, our findings provide insight into CYPDs’ experiences and perceptions of self-management of T1D. Parents, HCPs and peers may facilitate transition towards independent self-management. Conversely, incidences of non-support from parents, peers, HCPs, and so on, can contribute to feelings of frustration towards T1D and also its self-management. The scope of the studies included in this review highlights a gap in research that explores processes of self-management and suggests that exiting conceptualisations of self-management may be extended to take processes of self-management into consideration. Continued research that aims to understand these interactions from multiple perspectives may contribute to knowledge on how positive engagement with self-management of T1D can be facilitated in settings such as within the home, the clinic and at school and may lead to improved outcomes in terms of self-management engagement.
Supplemental Material
Supplementary_material_HPO – Supplemental material for Children and young people’s experiences and perceptions of self-management of type 1 diabetes: A qualitative meta-synthesis
Supplemental material, Supplementary_material_HPO for Children and young people’s experiences and perceptions of self-management of type 1 diabetes: A qualitative meta-synthesis by Ella Tuohy, Caroline Rawdon, Pamela Gallagher, Michele Glacken, Nuala Murphy, Veronica Swallow and Veronica Lambert in Health Psychology Open
Footnotes
Acknowledgements
Thank you to our Youth Advisory Group for assisting us with this research.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This qualitative meta-synthesis forms part of a larger programme of research funded through a project grant (HRA-HSR-2015-1233) awarded by the Health Research Board to Prof. Veronica Lambert (Dublin City University).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
