Abstract
Hansen's disease, also known as leprosy, is an infection caused by the bacteria Mycobacterium leprae. The authors present the case of a 52-year-old man, born in Tondela and living in Espinho, with no pathological antecedents. The clinical picture began in April 2017, when macular lesions appeared in the lower limbs and rapidly progressed to the trunk and upper limbs, associated with complaints of pruritus but without alterations in the analytical study. After several topical and systemic treatments with glucocorticoids, antifungals, antibacterials and unsuccessful antihistamines, he was referred to an external consultation of Dermatology. He performed a biopsy of one of the lesions that revealed the definitive diagnosis: “Lepromatous Leprosy”. After the biopsy result, he started triple treatment with rifampicin, clofazimine and dapsone with improvement of the condition.
Introduction
Leprosy is a chronic infectious disease caused by an acid-fast bacilli Mycobacterium leprae or Mycobacterium Lepromatosis. It is a rare disease in developed countries but one whose incidence has been increasing in countries like India, Brazil and Indonesia.
This type of bacteria is distinguished by its tropism by peripheral nerves, skin and respiratory tract’s mucosa. Symptomatology is complex, characterized by cutaneous, polymorphic and peripheral neuropathy. However, this disease is often silent in the first years after initial contact. The diagnosis is clinical and must be confirmed by biopsy.
Hansen's disease can be classified into 3 subtypes: Tuberculoid, Lepromatous or Indeterminate. The lepromatous form is more common in individuals with immunodeficiency (primary or acquired) and is associated with more severe manifestations of the disease, reaching the skin, kidneys, nose, testicles and cases of peripheral neuropathy more pronounced.

2- Further erythematous macular lesions.
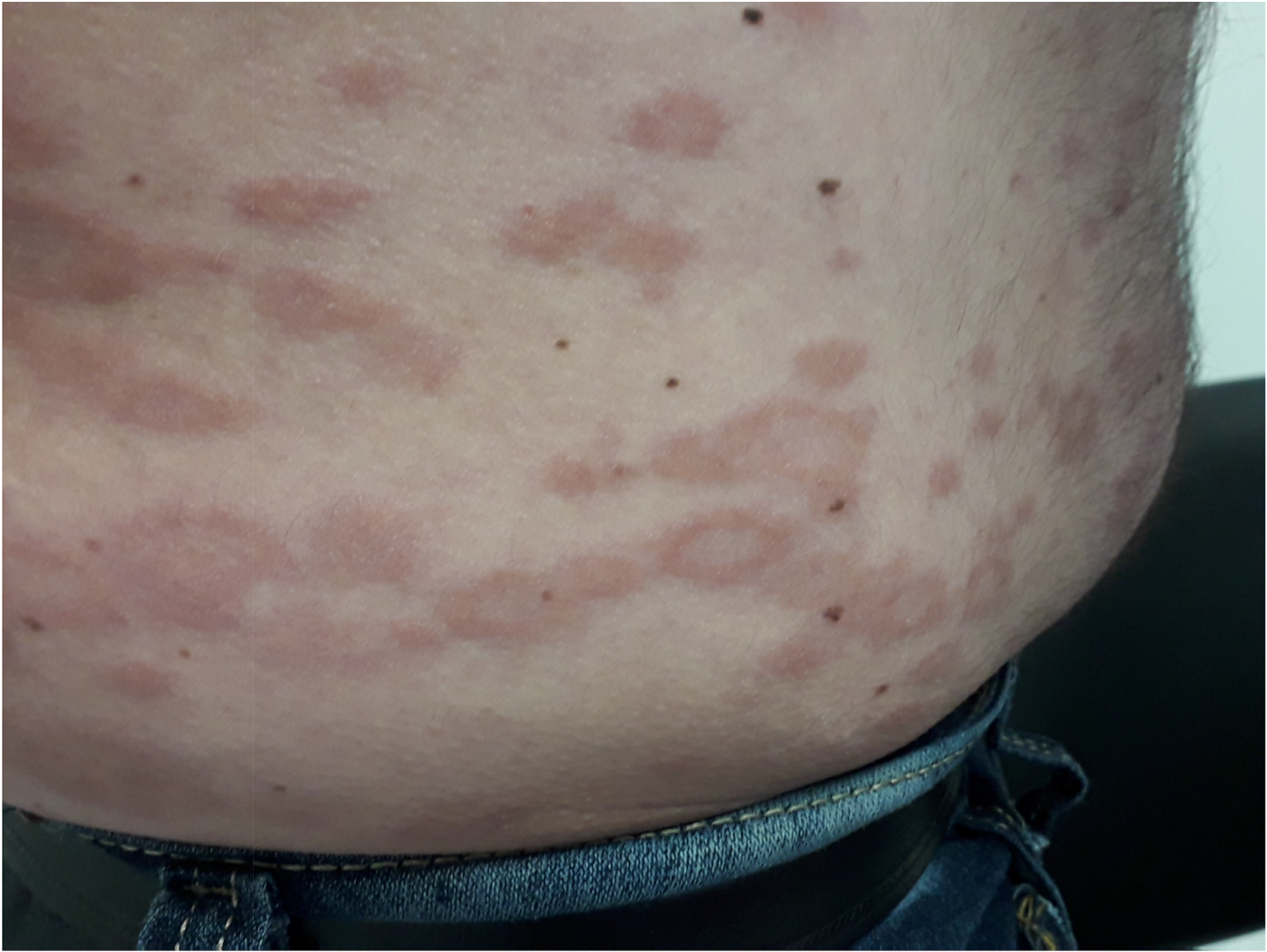
1- Erythematous macular lesions.
Treatment consists of polytherapy, including dapsone combined with other antimycobacterial drugs, thus reducing the rate of resistance. Drugs, while preventing the progression of the disease, do not reverse nerve damage and deformities. After the start of treatment, the patients become non-contagious.
Case description
The authors describe the case of a 52-year-old man, a plumber, married, with no relevant pathological history and no drug habits. He lived in a rural environment with his wife, in a house with all habitability conditions, with 3 domestic animals (one dog and two cats). The clinical picture began in April 2017, when the patient presented some erythematous macular lesions (Figures 1 and 2) in the lower limbs, with no other associated symptoms such as fever, pruritus, pain or other complaints. After a few days, due to progression of cutaneous lesions to the remaining body surface, without reaching the mucous membranes, and due to complaints of pruritus, it was medicated with topical glucocorticoids and antihistamines without any improvement.
Over a few months, the condition was aggravated, with the presence of a greater number of lesions and lack of improvement with the different treatments (antibiotics, antifungal, systemic glucocorticoids), and the patient was guided to observation in an external consultation of Dermatology. It should be noted that the patient never presented fever, weight loss, complaints of asthenia, adenopathy or other changes.
He performed a skin biopsy in May 2018 that revealed the diagnosis of lepromatous leprosy, the most severe form of the disease. After mandatory notification of the disease, the patient started treatment with dapsone, rifampicin and clofazimine with clear improvement of the lesions.
The patient was also observed in an outpatient clinic for infectious diseases, in which the hypothesis of some immunosuppressive disease such as Acquired Human Immunodeficiency or Immunoglobulin deficiency was excluded, and in the outpatient clinic of Neurology, due to the possibility of peripheral neuropathy, which was not confirmed.
Discussion
Hansen's disease is an infectious but relatively rare disease in developed countries. In Portugal, it is estimated that its incidence has decreased in recent years, however, the authors describe the case of a patient with this pathology without epidemiological context and no relevant background, whose diagnosis was confirmed by biopsy.
This pathology becomes more common in regions with poorer health conditions and may be transmissible in the untreated stage of the disease. This transmission is mainly done through nasal droplets or secretions. Thus, it is assumed that the contagion is carried out after contact with a sick person for an extended period of time. However, even after contact with the bacteria, the vast majority of immunocompetent people (about 95%) do not develop the disease, which makes the case described even rarer. Some studies reveal some genetic predisposition for the acquisition of the disease.
Conclusion
Hansen's Disease is a rare pathology and often still faced with some social stigma. The prejudice still prevalent in society can be justified by the fact that in the past “leprosy” was considered to be a highly contagious disease and associated with significant mortality and morbidity, given the lack of effective treatment. However, this case portrays the most severe form of the disease in a man with no relevant background and good socioeconomic conditions.
Currently, although prolonged therapy is effective, in the evaluation of this type of lesion the diagnosis of leprosy should be considered and excluded since it is not a disease of the past nor one that affects only the lower class.
Learning points
Leprosy is a rare disease worldwide;
The differential diagnosis is vast and difficult;
The diagnosis of this pathology, due to its rarity, can easily go unnoticed, so doctors should be alert.
