Abstract
We report atypical gastric outlet obstruction in a geriatric patient caused by acute mesenteroaxial gastric volvulus precipitated by a wandering spleen.
Background
Wandering spleen is defined as the migration of the spleen from its normal position in the left upper quadrant of the abdomen. As a rare entity, most cases occur in the paediatric population and are derived from congenital defects in the development of splenic ligaments. 1 Acquired causes include disruption of suspensory ligaments from trauma or hormonal relaxation of these ligaments in childbearing women. However, a wandering spleen is rarely seen or reported in geriatric patients.
The presentation ranges from an incidental finding during abdominal imaging to volvulus of an associated intra-abdominal organ, typically the stomach, followed by sudden onset of abdominal pain. 2 A gastric volvulus secondary to a wandering spleen is considered a surgical emergency due to compromised blood flow. We herein report an atypical presentation of gastric outlet obstruction in a geriatric patient caused by acute mesenteroaxial gastric volvulus precipitated by a wandering spleen.
Case report
An 84-year-old, otherwise healthy, woman presented to the emergency department with sudden onset left upper quadrant pain with associated nausea and abdominal bloating. She also reported a one-month history of progressive left lower quadrant pain. The patient denied any weight loss, anorexia or vomiting. She never had a colonoscopy or Esophagogastroduodenoscopy. Of note, the patient did not speak English and was only a relatively recent immigrant to the United States. Her physical exam was notable for abdominal distension, tenderness in both left upper and lower quadrants with a firm, palpable mass in the left lower quadrant. Laboratory results were significant for leukocytosis (11.6 × 109/L). A chest X-ray revealed significant gastric distention. A nasogastric tube was placed with difficulty. Imaging following passage of the nasogastric tube demonstrated findings consistent with a gastric volvulus (Figure 1).
Upright chest radiograph demonstrating gastric volvulus after nasogastric tube placement.
A computed tomography scan revealed marked gastric distention and gastric outlet obstruction secondary to a mesentero-axial gastric volvulus. A wandering spleen with a large splenic cyst appeared to be the lead point for the gastric volvulus (Figure 2). The patient received intravenous fluid resuscitation and the nasogastric tube remained in place. An upper endoscopy demonstrated a para-oesophageal hernia, gastric torsion and no evidence of ischemia. Surgical management, which would involve a gastropexy and splenectomy, was discussed at length with both the patient and her family. Given her significant improvement in symptoms as well as the patient’s and family’s concern of the peri-operative risks, they declined operative intervention. Over the next five days, her pain fully resolved, the NG tube was removed and the patient was transitioned to solid food and was ultimately discharged home. Upon follow-up she reports baseline dull abdominal pain in the left lower quadrant, denies weight loss and is otherwise well.
Computed tomography scan demonstrating markedly enlarged stomach with wandering spleen and associated splenic cyst.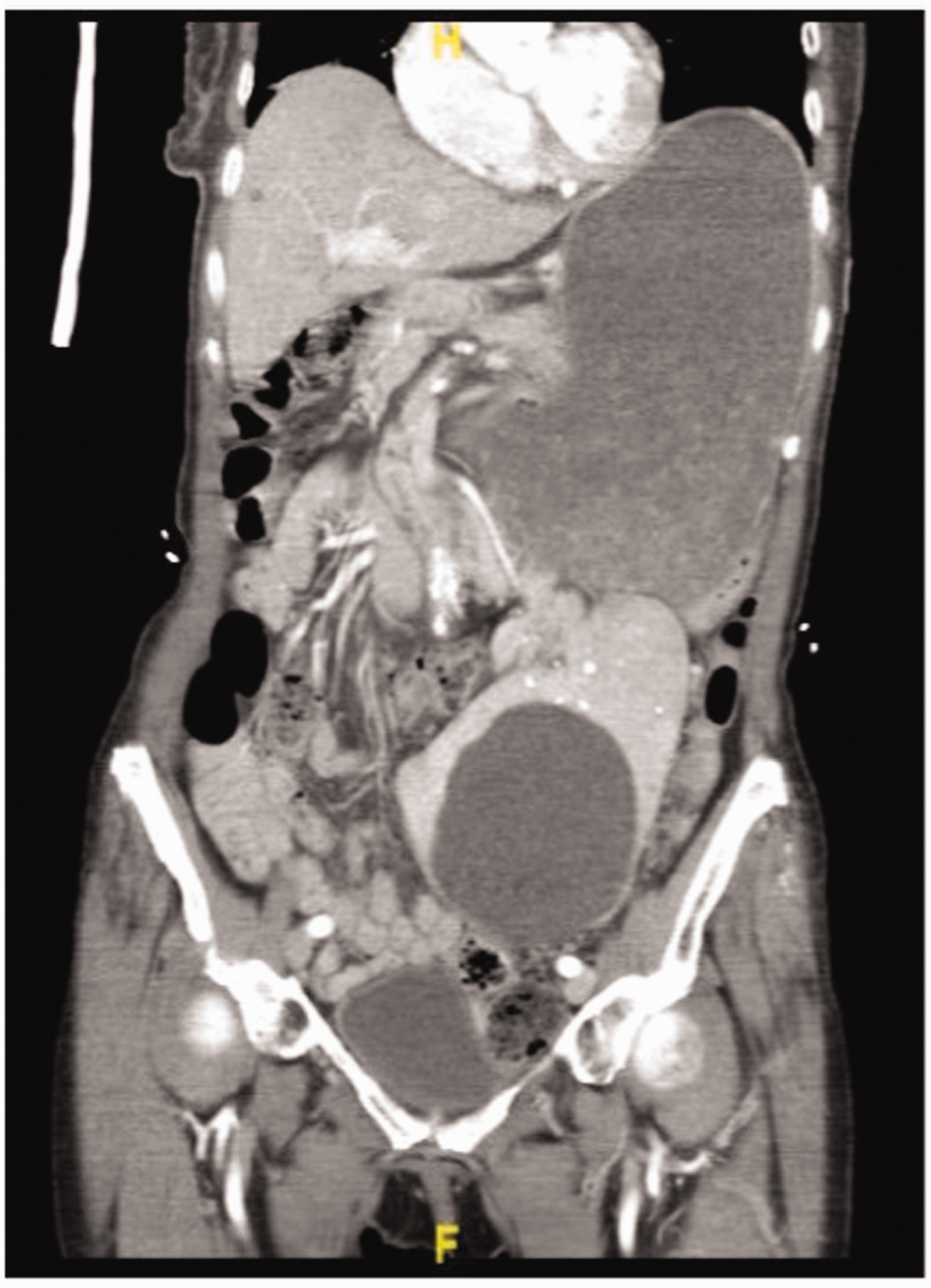
Discussion
Wandering spleen is caused by laxity of supporting ligaments in the splenic pedicle. The risk of splenic migration is higher when these ligamentous laxities are associated with splenomegaly. 1 In this case, the large splenic cyst likely contributed to the spleen’s migration into the lower abdomen. Although cases of wandering spleen have been reported in patients with Marfan’s syndrome, Prune Belly syndrome and congenital diaphragmatic hernia, a wandering spleen is not typically associated with syndromes or connective tissue disorders. The clinical presentation varies from asymptomatic to an acute abdomen, with the most common presentation being a lower abdominal mass with non-specific abdominal discomfort either in the paediatric or post-partum populations. Our patient’s history of persistent dull abdominal pain generalized to the lower left abdomen corresponded to the spleen’s migration.
Gastric volvulus is a life-threatening disease characterized by abnormal rotation of the stomach along either the long axis (organoaxial, 60% of cases) or short axis (mesenteroaxial, 40% of cases). A gastric volvulus most commonly presents as acute gastric outlet obstruction presenting as Borchardt’s triad of upper abdominal pain, emesis and inability to pass a nasogastric tube. Initial management consists of resuscitation and nasogastric tube decompression, followed by endoscopy to assess for ischemia and attempted de-torsion. If decompression is achieved, then non-operative management may be undertaken in the hemodynamically stable patient. Strangulation and necrosis occur in 5–28% of cases and must be considered a surgical emergency. Gastropexy is carried out with a gastrostomy tube to prevent recurrent volvulus. Of note, case reports also describe pancreatic and colonic volvulus associated with wandering spleen. 1
For wandering spleen, imaging demonstrates a spleen not located in the left upper quadrant. Imaging with Doppler can demonstrate absent blood flow and a ‘whirl’ sign indicating splenic vascular pedicle torsion. Treatment for either asymptomatic or symptomatic wandering spleen involves splenectomy or splenoplexy. The paediatric literature predominantly supports splenoplexy due to the risk of overwhelming post-splenectomy sepsis. However, in older patients, the risk of failure of splenopexy out-weighs the risk of overwhelming post-splenectomy sepsis and splenectomy is recommended.
Despite numerous family meetings, the patient and her family declined operative intervention citing the patient’s age, risk of peri-operative complications and a preference for non-Western care. Approximately 22 million Americans have limited English proficiency. Despite the use of trained interpreters or ‘language lines’, 2 mistrust and difficulties in direct communications still exist. Communication and cultural barriers potentially played a role in the informed consent of this patient. Predictors of barriers to communication among individuals for whom English is not the first language include female gender, being single, lower financial status and stronger identification with one’s own health beliefs. 3
Wandering spleen is very rarely reported in elderly patients. Older patients may present with vague and atypical symptoms mandating a broad differential. Discussions regarding operations for rare diseases can be difficult among elderly patients for whom English is not a first language. Wandering spleen may cause torsion of adjacent organs, such as the stomach, and potentially lead to gastric volvulus presenting as a surgical emergency. We urge careful consideration of patient culture and family dynamics prior to informed consent for unusual surgical emergencies.
Footnotes
Declarations
Acknowledgements
None.
