Abstract
Objectives
We observed whether general practitioners are referring more appropriately for balanitis xerotica obliterans in regards to circumcision, especially at a time of clinical concern, and whether their discriminative abilities were affected by age. We also aimed to explore if balanitis xerotica obliterans was over-diagnosed by surgeons potentially leading to unnecessary circumcisions of healthy foreskins.
Design
Cross-sectional descriptive study.
Setting
Leicester Royal Infirmary.
Participants
All children less than 16 years of age were included and were subsequently split into two categories: those less than or equal to five years and those above five years. Circumcision was justified if surgeon found pathology under foreskin commissioning guidelines set by the Royal College of Surgeons of England. After clinical diagnosis of balanitis xerotica obliterans, the pathological database was searched for histological confirmation.
Main outcome measures
Has diagnostic accuracy improved amongst general practitioners for balanitis xerotica obliterans and is there a high clinical to histological confirmation.
Results
Of the total patients, 14.5% were diagnosed clinically with balanitis xerotica obliterans. Only 66.7% of cases were histologically confirmed with chronic inflammation found in the rest; 5.5% of all boys referred had balanitis xerotica obliterans on histology; and 8.2% of children <5 had clinical balanitis xerotica obliterans with 1.7% confirmed histologically. This was in contrast with 18.1% and 9.2% found in the older cohort.
Conclusion
There remains a high diagnostic inaccuracy amongst general practitioners when referring for balanitis xerotica obliterans. This is greatest in those under five years. Although balanitis xerotica obliterans was over-diagnosed, no healthy foreskin underwent unnecessary circumcision.
Introduction
Circumcision is one of the oldest and commonest performed surgical procedures throughout the world. Nearly 21,500 boys under the age of 18 years were circumcised on the NHS in England between April 2011 and March 2012. 1 Whilst an initial outpatient assessment costs £114 per individual, the procedure itself is estimated at £750 as an elective day case with a further £300 for an overnight stay. 2 It is therefore unsurprising the substantial financial savings of the NHS from appropriate general practitioner referrals and undertaking circumcisions that are absolutely indicated. One such pathology fitting this criterion includes pathological phimosis of which balanitis xerotica obliterans is a common cause. Such pathology of unknown aetiology causes failure in prepuce retraction secondary to distal scarring with a fibrotic circumferential band seen at the distal portion of the prepuce. 3 Left untreated, this can lead to meatal and urethral stenosis. Although previously thought to be rare in young children with an overall childhood incidence of 5%–6%,4,5 recent literature have shown it to be at least twice as common in this population, with one suggesting to be increasingly vigilant of balanitis xerotica obliterans in those under five years.6–10
Recently, a review by Celis et al. 11 suggested increased incidence may be secondary to more foreskins sent for histology and greater scrutiny of the foreskin by surgeons. The latter is owed to the fact that classical features of balanitis xerotica obliterans need not be present in children whilst early features are subtle and can be missed. Such ambiguity would certainly ease the appropriateness of general practitioner referrals questioning pathological phimosis. Extensive literature over the last three decades have shown high diagnostic inaccuracy amongst the front line providers of medical care in distinguishing between physiological (a developmentally non-retractile foreskin) and pathological phimosis, leading to many unnecessary referrals and financial implications.4,5,12–15 Such inaccuracies led to extensive educational measures including distinct guidelines and policies,1,16,17 aiming to enhance the understanding of the natural foreskin development and providing alternatively cheaper and safer treatment options including topical steroids.18,19 Now, coupled with the serious consideration of balanitis xerotica obliterans by surgeons in the paediatric population, one can expect a greater number of general practitioner referrals querying pathological phimosis to be appropriate particularly compared to previous studies. However, the low index of clinical suspicion of balanitis xerotica obliterans could potentially lead to its over-diagnosis and many unnecessary circumcisions. We aimed to investigate both of these. In addition, the diagnostic accuracy of balanitis xerotica obliterans in less than five year olds were compared with the rest of the paediatric population to observe if referral rates were affected by age based on recent concerns of balanitis xerotica obliterans no longer being a rarity in the younger cohort.10,13,14
Methods
All new patients less than 16 years of age referred to seven consultant paediatric surgeons at Leicester Royal Infirmary, United Kingdom, between June 2015 and June 2016 were retrospectively reviewed for an opinion regarding circumcision. They were identified from the Electronic Document and Records Management database which stored all general practitioner referral letters over the required time span. For each patient, their age, reason for circumcision referral and diagnoses made by the paediatric surgeon were recorded. Reasons for referral included: phimosis, non-retractile foreskin, recurrent balanitis/balanoposthitis on its own or in combination with one of the above and others. From previous literature, these are the commonest reasons for general practitioner referrals.4,5,11 General practitioner referrals were justified if the surgeon found pathologies for circumcision based on the foreskin conditions commissioning guidelines set by the Royal College of Surgeons of England. 1 They were also justified for conditions requiring alternative interventions including preputioplasty and frenuloplasty. The pathological database was searched for all patients with clinically diagnosed balanitis xerotica obliterans for histological confirmation. Finally, the management plan formulated was recorded to include: surgery, follow-up and discharge.
Results
Total number of patients referred including GP’s diagnosis for referral and those that were justified.

Penile swelling, religion and ballooning do not fall under RCS guidelines.
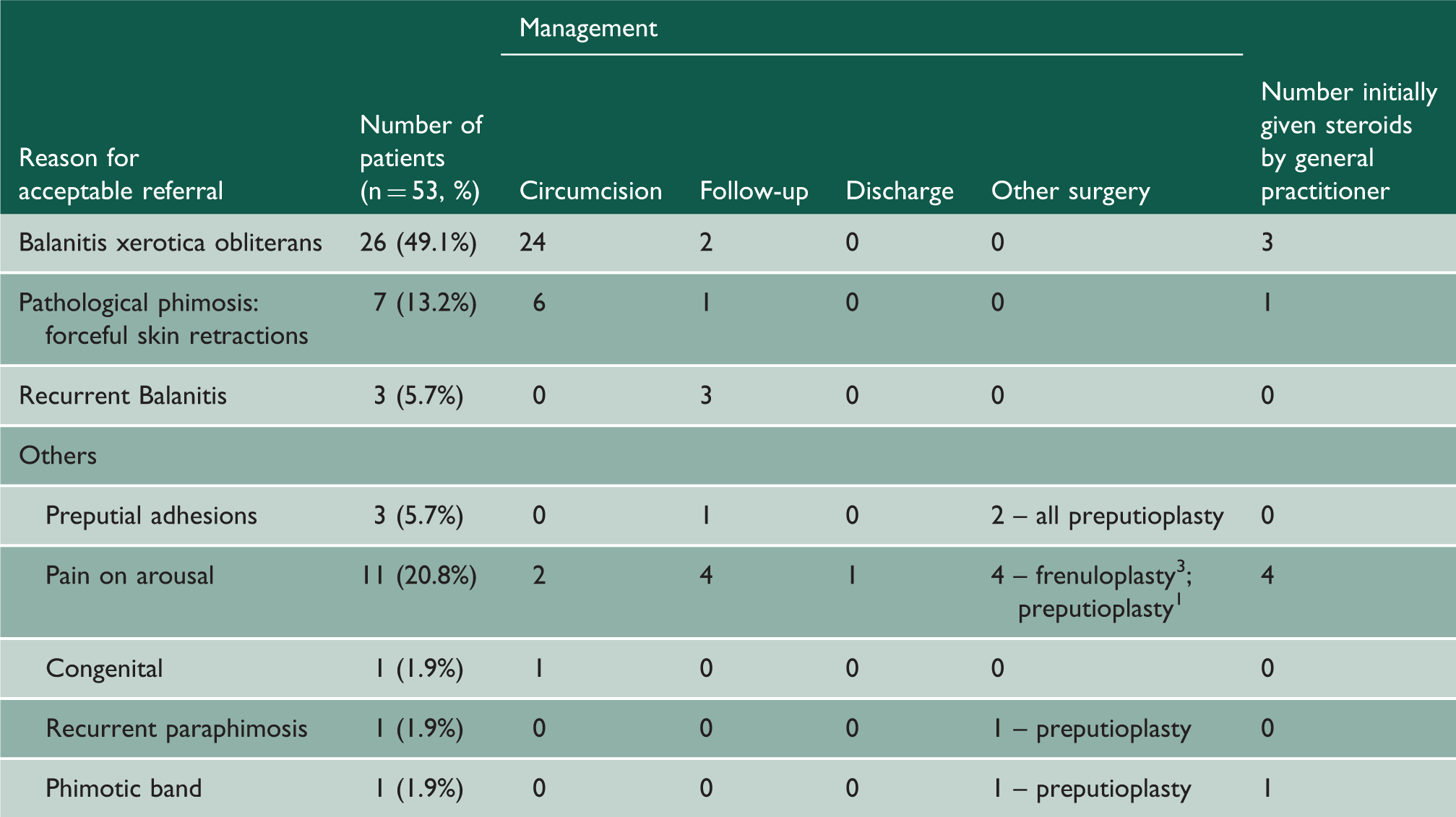
The management of patients justified for referral.

Age distribution of those with balanitis xerotica obliterans, chronic inflammation, other forms of pathological phimosis and pain on arousal.
Six out of seven patients with pathological phimosis of known aetiology including forceful skin retractions underwent circumcision. Three patients had recurrent episodes of balanitis up to six to seven episodes in one year requiring multiple oral antibiotics. Patients with pain on arousal either had surgery, two of whom had circumcisions or follow-up with the option of intervention if conservative management failed. The final patient for circumcision had congenital penile torsion. The rest were managed appropriately for preputial adhesions, phimotic band and recurrent paraphimosis (Table 2).
A total of 141 patients were referred unnecessarily; 129 of these cases were due to general practitioner concerns of pathologically non-retractile foreskin but were found to be physiological by the surgeon. After excluding seven patients appropriate for referral but with surgeons’ concerns of other pathology, only 30 of 166 referrals (18.1%) were consistent with the surgeon’s diagnosis of pathological phimosis regardless of whether this was balanitis xerotica obliterans or other forms.
Based on age, Figure 2 shows the incidence of preputial pathology in patients where general practitioners were concerned with pathological phimosis. Sixty-one patients ≤ 5 years and one hundred five patients > 5 years were referred for this. Physiological phimosis was more likely seen in the younger age group, with 8.2% (n = 5) having clinical balanitis xerotica obliterans compared with 18.1% (n = 19) in the older group. Of the total 166 patients, 24 had balanitis xerotica obliterans (14.5%). As described, nine patients had unavailable histological reports, two of which were from the younger cohort. After histological confirmation, 1.7% and 9.2% of those referred had histologically proven balanitis xerotica obliterans in the younger (1 of 59) and older groups, respectively (9 of 98).
Incidence of preputial pathology in those referred for pathological phimosis. Distributed by age. *Seven patients referred appropriately but for specialist diagnosis not matching initial referral reason: 3 – preputial adhesions, 3 – pain on arousal and 1 – tight phimotic band.
Of the 141 referrals, 103 patients were immediately discharged with physiological phimosis being the reason in 93.2% of cases (n = 97). However, 35 patients were followed up, with 33 having physiological phimosis. The reasons for such were patients started on steroid cream (57.6%), reassurance (12.1%) and assessing ease of foreskin retraction over time (12.1%). The rest were followed up due to other incidental findings in clinic including undescended testicles (6.1%), urinary incontinence (9.1%) and bladder spasms (3%). Three patients, aged 5, 10 and 11 years, underwent circumcision despite having physiological phimosis. Parental concerns of the foreskin were reported in two of them.
A total of 36 circumcisions were performed from all referrals (18.6%), 30 of which had pathological phimosis (83.3%) with 24 of these having clinical balanitis xerotica obliterans (66.7%).
Discussion
Pathological phimosis, particularly balanitis xerotica obliterans, is an absolute indication for circumcision and is a common reason of general practitioner referrals. Three decades ago Rickwood and Walker 13 reported an over-diagnosis and under-recognition of pathological and physiological phimosis, respectively, leading many studies to subsequently examine general practitioners’ discriminatory abilities of the two and their efficiency in referrals. A diagnostic accuracy of 16.9%–25% was seen, with Yardley et al. suggesting this to be as high as 35%, although no reasons for general practitioner referral were given.4,6,15 Lately, the incidence of balanitis xerotica obliterans in the paediatric population is increasing, 12 coinciding with the extensive measures put in place to aid the diagnoses made in primary practice. Therefore, one would expect improved diagnostic accuracy of pathological phimosis by general practitioners, particularly with the expected lower threshold for considering balanitis xerotica obliterans in foreskins by surgeons.8,9
Although our results showed many general practitioners were also concerned with pathologically non-retractile foreskin, with it making up a larger proportion of justified referrals (62.3%) and circumcisions (83.3%), this did not however reflect an improvement in diagnostic accuracy. This is underlined by only 18.1% of all pathological phimosis referrals found to have true pathology. Unlike previous studies, however, the prevalence of balanitis xerotica obliterans clinically was higher (14.5%),4,15 suggesting more general practitioners referring appropriately for the balanitis xerotica obliterans form of phimosis which underwent circumcision in the majority of cases. Unfortunately, upon closer inspection, many of these diagnoses may have aimed to necessitate referral rather than relying on one’s true judgement, highlighted by only 12.5% of general practitioners able to recognise scarring on examination. However, scarring need not be clinically present in the early forms of balanitis xerotica obliterans which could otherwise significantly under-diagnose the condition. 21 Although this may refute the idea of general practitioners diagnosing balanitis xerotica obliterans just to necessitate referrals, it is highly unlikely the remaining 87.5% of those diagnosed clinically as balanitis xerotica obliterans were in their early forms with the potential of being missed. This is supported by Kiss et al. 8 who found only 19.2% of balanitis xerotica obliterans was of this state. Furthermore, the specialist themselves saw clear scarring in all these foreskins. There is the possibility many of the balanitis xerotica obliterans were recognised in primary practice but failure to mention in referral letters was secondary to concerns of it only having a definitive diagnosis on histology. Even then an initiative approach, centred on commissioning guidelines, would be primarily treating with potent topical steroids where 40% improvements in clinical balanitis xerotica obliterans are reported, particularly in its early phases.12,22 As only four general practitioners started this, it remains likely that prior to referral they did not suspect balanitis xerotica obliterans but rather the need for wanting expert opinion. Before their effects on balanitis xerotica obliterans, topical steroids have long been known for their supreme efficacy on retracting a physiologically phimotic foreskin due to their anti-proliferative epidermal properties and reduced collagen and fibrinogen deposition in the epidermis.2,23 Two recent systematic reviews have shown satisfactory results with one suggesting success in 95% of such foreskins.24,25 Not only do these findings propose easy and inexpensive alternatives but prevention also of costly premature referrals. Although many patients with physiologically phimotic foreskin were discharged, we found over half of them that were followed up were secondary to surgeons starting steroid treatment. These were not initiated at primary practice and subsequent follow-up was essential to assess foreskin progression. Unfortunately, direct comparisons to earlier studies cannot be made but one can conclude several costly implications arising from delayed steroid treatment. First, it showed conservative management has remained under-recognised despite its importance as stated in literature and commissioning guidelines.1,16 Second, as it can take up to six months to be seen in clinic, the severity of phimotic foreskin can worsen during that period. 26 Such efficacy of topical treatment potentially becomes affected, increasing the number of circumcisions that were potentially avoidable.
The recent fear of under-diagnosing balanitis xerotica obliterans may lead to its over-diagnosis reflected in our study where only 5.5% of all boys were confirmed to have balanitis xerotica obliterans. This is in contrast with the 14.5% referred for phimosis that had clinical diagnosis of balanitis xerotica obliterans and the 13.4% from all referrals. The clinical to histological correlation was 66.7%. As this is lower than certain studies, it may lead to unnecessary circumcisions in healthy foreskins which have their own potential risks and concerns.13,27 Nevertheless, we showed all patients circumcised for concerns regarding phimosis had pathology on histological examination whether that was balanitis xerotica obliterans or chronic inflammation. This was better than those observed in previous studies where healthy foreskin was excised.7,8 However, selection bias could be present as only a small number of reports were available with nine absent, potentially leading to those with only severe scarring at time of surgery being sent to histology. This is unlikely, however, owing to seven different paediatric surgeons involved in the diagnosis of balanitis xerotica obliterans, each with their own threshold for sending specimen for routine histology. Furthermore, four pathologists examined the variety of specimens reducing outcome reporting bias. Both biases are likely more profound in other literature where only one or two surgeons and histo-pathologists were involved in interpreting findings.7–9 The overall prevalence of balanitis xerotica obliterans in our study is similar to Griffiths' and Huntley's results (5%–6%) but in disagreement with Yardley’s (12.1%).4,5,7 We believe our findings are of significant importance. This is because whilst recent literature indeed shows incidence of balanitis xerotica obliterans may have truly increased in the pathologically phimotic foreskin, it does not clarify the true prevalence of balanitis xerotica obliterans in the total paediatric population including those without foreskin pathology. Such clarification is of clinical value for general practitioners as it can aid in facilitating decisions for referral. However, as the high incidence of histological balanitis xerotica obliterans has been reported solely from the phimotic foreskin, the danger is primary physicians mistaking this with foreskins of all nature. Ultimately, this can play a role in many unnecessary referrals for circumcision, potentially explaining further why there was only an 18.1% diagnostic accuracy for such pathology despite recent advancements in educational measures.
Balanitis xerotica obliterans has long been a diagnosis of rarity in those under five years.13,14 Failure to retract the foreskin in this age group is usually an anatomical one, where there is co-adherence of the inner epithelium between the foreskin and glans at birth. After intermittent erections, gentle retractions and keratinisation of the inner epithelium does the foreskin become retractable. 28 However in 10% of cases, developmental adhesions may still persist at six years of age with failure of full retraction closely monitored and the options of lesser invasive interventions subsequently offered. 18 This includes adhesiolysis and preputioplasty, the latter of which were performed for two of three patients in this study with such adhesions. Although developmental adhesions are at the hierarchy of differentials, recent evidence has shown a rising incidence of balanitis xerotica obliterans in the younger child, especially those less than five years.7,9 Again however these were only in foreskins with phimosis and as mentioned previously may lead to many unnecessary referrals. This was reflected here where the chance of balanitis xerotica obliterans was less likely to be present in those five years or under (8.2%) compared to those over five (18.1%). With histological confirmation, balanitis xerotica obliterans was over five times less likely for those referred for pathological phimosis (1.7% vs. 9.2%). Until ours, there was no study to date looking at the overall prevalence of balanitis xerotica obliterans in this younger cohort. However, our study is limited as we cannot estimate the true prevalence for two reasons. First, the estimated prevalence is partly dependent on the diagnostic accuracy of general practitioners. Poor diagnostic accuracy from all referrals leads to lower prevalence of balanitis xerotica obliterans and vice versa with higher discriminative abilities. Second, these findings are based only on our centre. However, the distinct guidelines, policies, newsletters, existing literature and educational measures in place are providing an equal source of information and aid throughout all centres nationally. Therefore, one would expect similar prevalence of balanitis xerotica obliterans in those under five in other regions of England.
Conclusion
Despite a combination of guidelines, educational measures and low clinical index of suspicion by surgeons for balanitis xerotica obliterans, there still remains a high diagnostic inaccuracy amongst general practitioners when referring for such pathology. This is greatest in those under five years of age. Due to recent concerns of an increasing rise of balanitis xerotica obliterans in childhood, many unnecessary circumcisions may occur from over-diagnosis.
Footnotes
Declarations
Acknowledgements
The authors would like to thank Leicester Royal Infirmary for their support in facilitating the work.
Provenance
Not commissioned; peer-reviewed by Eugen-Matthias Strehle.
