Abstract
Objectives
To evaluate the perception of medical students of the new approach to problem-based learning which involves students writing their own problem-based learning cases based on their recent clinical attachment, and team assessment.
Design
Focus group interviews with students using purposive sampling. Transcripts of the audio recordings were analysed using thematic analysis.
Setting
Imperial College School of Medicine, London.
Participants
Medical students in the second year of the MBBS course, who attended the problem-based learning case writing session.
Main outcome measures
To elicit the students’ views about problem-based learning case writing and team assessment.
Results
The following broad themes emerged: effect of group dynamics on the process; importance of defining the tutor’s role; role of summative assessment; feedback as a learning tool and the skills developed during the process.
Conclusions
Overall the students found the new approach, writing problem-based learning cases based on patients seen during their clinical attachments, useful in helping them to gain a better understanding about the problem-based learning process, promoting creativity and reinforcing the importance of team work and peer assessment which are vital professional skills. Further tutor development and guidance for students about the new approach was found to be important in ensuring it is a good learning experience. We hope this evaluation will be of use to other institutions considering introducing students’ case writing to problem-based learning.
Keywords
Introduction
Problem-based learning is a form of learning based on the theory that a learner can acquire new knowledge or skills by applying pre-existing knowledge to generate their own learning objectives through case analysis and sharing this new knowledge with others.1,2
Problem-based learning was first introduced in 1969 at McMaster University in Canada by Howard Barrows to help encourage self-directed learning and development of professional skills to promote lifelong learning.3,4 This active way of learning has since been adopted into the medical curriculum by other medical schools worldwide, using various problem-based learning approaches ranging from the full problem-based learning curriculum advocated by Barrows to the hybrid curriculum which is used at Imperial College. 5
The use of problem-based learning in the clinical setting reinforces traditional bedside teaching because it integrates the patient encounter with related clinical skills, disease mechanisms and clinical management. 6
The problem-based learning approach at Imperial College involves a 10-step process as shown in Figure 1. This is a modified format modelled on the Maastricht ‘seven jump’ process and as described by Diana Wood.
2
As a small group teaching method integrated across first and second year medical curriculums at Imperial, problem-based learning encourages students to develop various professional skills during the process. These skills include team-working, case analysis, critical appraisal of literature and teaching skills such as questioning, presentation and feedback.
Summary of the Imperial style 10-step process.
The new approach we have introduced involves students writing their own problem-based learning cases based on their recent clinical attachment and assessing themselves and their peers. The rationale was to reinforce essential clinical and professional skills and to help students gain a better understanding about the problem-based learning process.
A literature search suggests that problem-based learning case writing by students is not an approach that is widely used in other medical schools within the United Kingdom, but it has been implemented in some medical schools in the United States. For example, Indianapolis medical school introduced a four-week elective for third and fourth year medical students with the aim of improving students’ skills and attitudes related to lifelong learning. 7 There is also some evidence that students gain a better appreciation of their curriculum development when they write their own problem-based learning cases. 8
The other important aspect of our new approach is to encourage students to participate in their own assessment. At our institution, the second year medical students are familiarised with verbal and written peer feedback in the first term. 9 Team assessment is a form of 360 degree evaluation, also known as peer assessment. It is often used in the medical profession to assess professionalism so could help students to reinforce the importance of professional attitudes and behaviours at an early stage of their learning. 10 Peer assessment is also reliable: it has been found to be consistent even when there are different peer raters hence facilitating a positive effect on students’ achievement and attitude towards learning.11,12
The new problem-based learning approach
During two terms of first year and the first term of second year, a group of 9–12 students, guided by a problem-based learning facilitator, explore cases written by the course lead, clinical and non-clinical teachers and past students. Each case is based on real patients and has specific knowledge-based objectives linked to the other teaching and learning in the curriculum.
A new process, whereby students write their own cases, was piloted with two groups of students per year for two years, no significant changes were made following the pilot, and the process was then implemented with the entire cohort. Each group splits into two teams and each team writes a case for the other team, based on their recent patient experiences. Each team then discusses the case written by the other team to identify, and then prepare presentations about, their learning objectives. All the team members have a specific role within the team to encourage active participation. Each team observes the other team for the discussion and presentation sessions (Picture 1). A process map of this new approach is seen in Figure 2.
Case writing exercise: student roles.
Also during the process, students are expected to assess themselves and other members of the team on their contribution towards the case writing process. The written formative assessment is carried out anonymously based on five criteria using a Likert scale. These five criteria include contribution to case selection and negotiation, background preparation, working collaboratively, implementation and communication.
Problem-based learning process: one team observing the other team discussing their clinical case.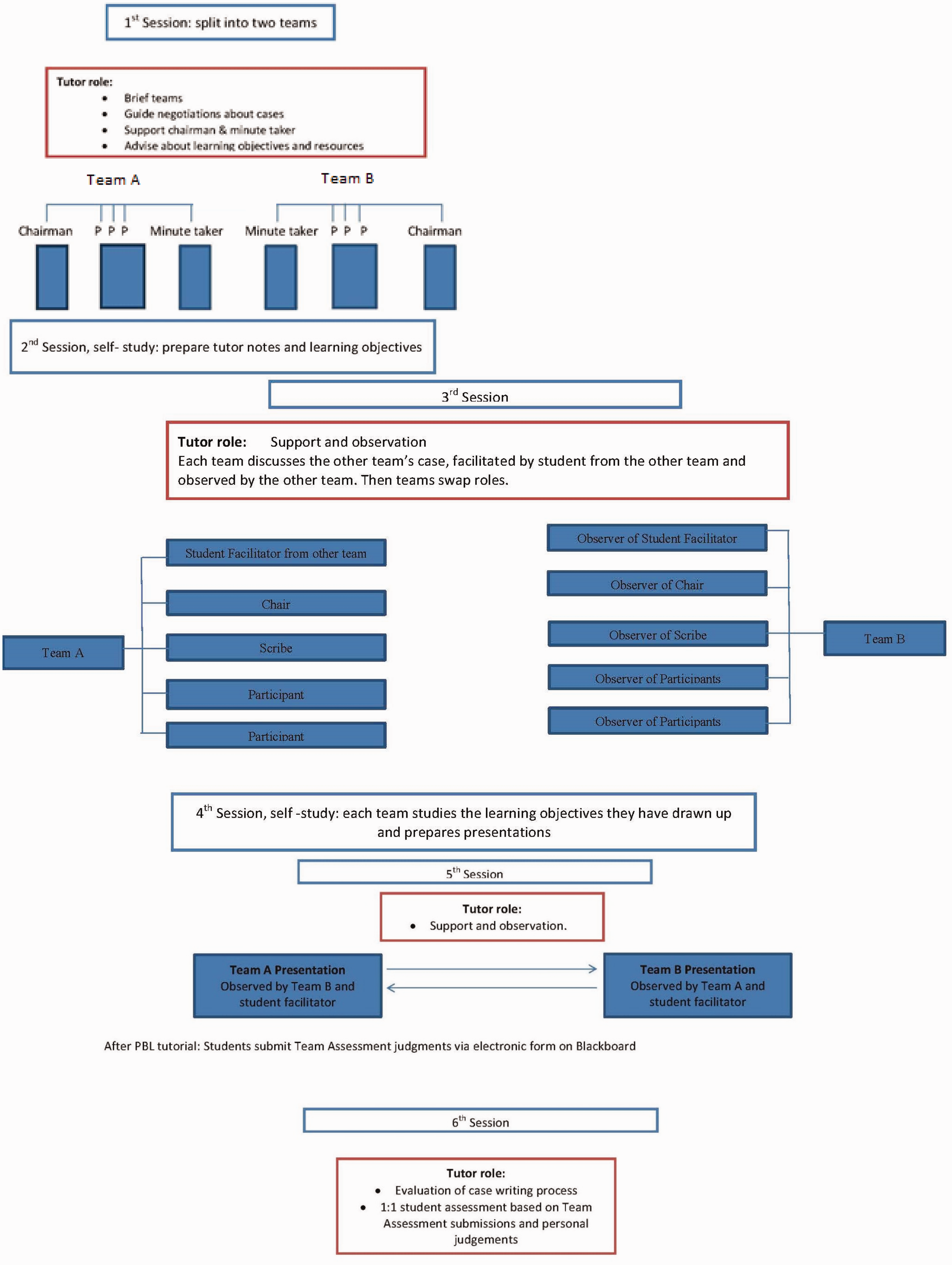
Aims
The aims of this study were:
To evaluate students’ perceptions of the new case writing and team assessment processes introduced into the second year of the problem-based learning course. To explore students’ ideas for innovative ways to improve the course.
Methods
Design
The evaluation was a qualitative study using focus group interviews as it is a well-established method of eliciting students’ perceptions.13,14
Sampling
We used purposive sampling to select students for the focus group interviews. 15 A total of 280 second year medical students who were involved in the course were sent emails inviting them to participate in the study and 11 students volunteered. There were six students in the first focus group (4 male and 2 female) and the second focus group consisted of five students (2 male and 3 female). After the investigator explained the purpose and nature of the evaluation, students were asked to sign a consent form to allow the use of the recordings and their quotes for educational purposes. It was made clear to them that they did not have to take part, could withdraw at any time without prejudice, and that they could choose not to have any of their anonymised quotes used in a final report.
Data collection
The focus group interviews were carried out in June 2014 by GE who was not involved in either teaching or assessment of problem-based learning. The first focus group interview lasted for 38 min and the second focus group lasted for 54 min. The audio recordings were transcribed by a professional transcription company.
Data analysis
Yewande Idowu analysed the transcripts manually using thematic analysis. 16 This involved analysing the transcript of the first focus group interview using open coding to create a thematic map. Then possible explanatory themes were identified from the codes, reflecting both the positive and negative aspects of students’ perceptions. The second transcript was then coded using the themes identified and these themes were reviewed using an iterative process until no new themes emerged. The themes were also validated with GE and EM independently and any arising conflicts, which were mainly semantics, were resolved.
Results
Five main themes were identified. Table 1 shows these themes with their positive and negative aspects; we will discuss these and illustrate with quotes from the medical students.
Group dynamics
The students found that as a result of an effective group dynamics, they were able to work well within their groups, sharing their clinical experiences. These invariably generated more ideas for the case selection and they were able to complete the case writing exercise swiftly.
‘ … it kind of, it brought a lot more cases to the group … ’
‘ … everyone in our group was very interested in their clinical attachment and all came forward with very interesting clinical scenarios’
Results.

‘ … some people who hadn’t been on the same firm … knew a lot about one particular subject which other people didn’t know, and it was quite difficult if you weren’t on that firm to give a good input to the session’
Role of tutors
Many of the students believed that the role of a tutor was very important in providing adequate guidance. Some of the students said that they received good guidance from their tutors during the sessions, but the majority found that their tutor’s guidance was inadequate with some tutors having the wrong concept about the session. They said that this was reflected in the quality of their case and their understanding of the various roles they were meant to carry out during the task. Hence they suggested that tutors should provide more guidance during the case writing session.
‘Our tutor flitted between the groups and made sure that we were on the right level and kind of did give us guidance’
‘ … ideally a bit more guidance would have helped, and maybe that would have meant our cases were richer … guidance about level of difficulty of the case, kind of how many aspects to the case we wanted … a medical legal aspect, a purely physiological aspect and then a social aspect, … so we weren’t entirely sure … ’
The students commented that having experienced and enthusiastic clinicians as tutors was an important factor because it meant that they had excellent guidance and support.
‘My tutor was really enthusiastic about the whole process and she was really actively involved in what we were doing … going between the two groups … she would have her own input … consider things in a clinical perspective and say things like “have you thought about it in this way?”’
Assessment to drive learning
All the students agreed that some form of assessment was important to drive their learning and improve student contribution. Some students suggested adopting a summative form of assessment, which was perceived to be a better form of incentive than a formative assessment, but others thought that it would have a negative impact on team work and it would be hard to ensure a fair summative assessment when there were difficult group dynamics and poor guidance from tutor.
‘a difficult group dynamic … I think that could bring us down in assessment in an unfair way’
‘ … and I think assessing each person individually could create some form of competition … working less cosily as a team and a bit more like every man for himself … ’
Feedback as a learning tool
The students found that giving and receiving constructive feedback from their peers was useful in gaining more insight about their attitude and performance. In addition, they valued having a well organised and structured individual feedback session with their tutors. Some of the students did not receive critical feedback from their peers and had suggested a need for more guidance on how to give feedback.
‘I found the paragraphs … people had written, incredibly useful … the most useful part’
‘I actually liked being able to hear feedback from others in my group of how they thought I did, because you contribute but you are not actually sure how you come across or how well you did, so it was good to hear other people’s feedback, in an anonymous way’
‘I remember … we had a session … on how to give like appropriate feedback. I think that perhaps maybe this year … it could be reinforced … perhaps tutors could look at the feedback and say actually what you could do better about giving feedback … ’
Learning new skills
The students found the entire process worthwhile because they were able to use their creative thinking skills, reinforce the generic professional skills they had learned previously, and consolidate their knowledge.
‘I quite like the fact that we had free creative rein on what we made as our case … actually use your imagination and get thinking … it was a kind of refreshing change, particularly from the normal PBL sort of format … ’
‘ … I found it a very useful team working exercise because creating something together is different from discussing something together, like in the other PBL sessions.’
‘ … it’s nice to consolidate and revise things … but primarily in terms of its strengths, it’s your presentation skills and your team working skills … it brings together … This is why I like it as a component of our learning … we’re allowed to experience.’
Discussion
This is the first evaluation looking at students’ perception of the new problem-based learning approach for second year medical students at Imperial College.
The results suggest that student value having the opportunity to write their own problem-based learning cases based on the patients they had seen during their clinical attachments and to assess themselves and their team members.
Students said that they gained a better understanding of the problem-based learning process. A particular advantage of this new approach over the more traditional problem-based learning format is the opportunity they have to be innovative, using their creative skills to write a case, integrating their clinical experience with problem-based learning. They also found the experience rewarding because it strengthened their team working and presentation skills as well as being able to give and receive critical peer feedback in a safe setting and consolidated their knowledge.
The effectiveness of tutors is essential to the success of problem-based learning; 17 one of the major challenges identified by the students was having inadequate support from their tutors. As a result, the students suggested various options to ensure they had more robust support; these included more effective briefing about the process for tutors and extended guidance about case writing and feedback for students. Also a form of incentive, such as prizes for well written cases, was suggested by the students to help improve the attitudes of students towards problem-based learning and to drive the learning process.
Limitations
From our analysis we were able to identify important themes and sub-themes emerging from the students’ views about the new approach but our evaluation has limitations. The misrepresentation of data could occur as only 11 students in two focus groups might not capture the views of all the students about the new problem-based learning approach and further focus group interviews could be conducted as thematic saturation may not have been attained. Although the interviews were conducted by an independent teacher as a recognised faculty member there might still be some bias relating to power imbalances and confidentiality, which might inhibit their contribution during the discussion. However, it was reassuring to note that the students did not appear to be inhibited at all, and seemed comfortable offering both negative and positive comments about the course.
Implications
This evaluation has been helpful in implementing further significant changes to our new problem-based learning approach at Imperial. Following the evaluation more tutor development workshops have been organised and the course guides for students and tutors have been updated to include further guidance about case writing and feedback. Also the students are encouraged to prepare more during their clinical placement for the case writing session that follows, e.g. by recording case stories and results.
This is the first publication evaluating students’ perception about writing problem-based learning cases based on early years clinical attachment and team assessment. A follow-up study is needed to evaluate the impact of the new changes implemented to improve the quality of tutors on the course.
In conclusion, this new approach to problem-based learning was well received by our students in terms of sharing clinical experience and writing a case based on their clinical attachments. We hope that they will continue to use the process when working with patients and teams in the later years of the course and after graduation. This may be of interest to other medical institutions in the United Kingdom as it facilitates a better understanding of problem-based learning and reinforces the generic professional skills.
Footnotes
Declarations
Acknowledgements
The authors thank Imperial medical students who volunteered for the focus groups, and the Digital Literacies Team, Professor Azeem Majeed and the Medical Education Research unit at Imperial College for their advice and support.
Provenance
Not commissioned; peer-reviewed by Edward Peile.
