Abstract
Objective:
Intra-detrusor botulinum toxin (IDBT) injection is a proven treatment for detrusor overactivity (DO) but carries a low risk of transient urinary retention. Despite this, hospitals invest in educating patients on clean intermittent self-catheterization (CISC). This study examines whether pre-IDBT CISC education is necessary.
Methods:
In this retrospective cohort study, 67 patients underwent IDBT over 9 months. All received CISC education from a Clinical Nurse Specialist (CNS) and a follow-up phone consultation 2 weeks later. The primary outcome was new or increased CISC needs post-IDBT, with secondary outcomes assessing the cost of CISC education, and factors associated with CISC requirement.
Results:
The study included 67 patients, 9 (13.4%) developed a new or increased need for CISC following IDBT. Subgroup analysis of five patients with sustained CISC needs showed males and those with idiopathic detrusor overactivity (IDO) were at significantly higher risk. In addition, CISC naivety and lower IDBT doses strongly correlated with urinary retention in this subgroup. Educating patients on CISC required €3240.82 and 52 hours of CNS time.
Conclusion:
Prioritising CISC education for these high-risk groups, particularly males with IDO, could effectively address up to 90% of patients developing sustained CISC needs, optimising resource allocation and reducing unnecessary costs.
Levels of evidence:
This study is comprised of Level 2b evidence as per the Oxford Centre for Evidence-based Medicine Levels of Evidence (March 2009).
Introduction
It is estimated that up to 16.5% of people are living with the symptoms of an overactive bladder (OAB). 1 These include urinary urgency, usually accompanied by frequency, nocturia, and possibly urge urinary incontinence.1,2 OAB-type symptoms can exert a significant psychological impact on affected patients, with approximately 50% of patients reporting some degree of adverse mental health outcomes. 2 In addition, OAB is an ever-growing expense on healthcare systems due to its prevalence, chronicity and an aging population.3,4
When oral pharmacological therapies are ineffective in managing DO, patients will undergo urodynamic testing. If detrusor overactivity (DO) is detected they will be offered intra-detrusor botulinum toxin (IDBT) injections. IDBT is proven to exceed its oral medicinal contemporary.3,4 Previous evidence has elucidated that IDBT injection is cost-effective and is not associated with lasting health-related ramifications. Consequently, it has become the non-pharmacological first-line intervention for DO. 5
A potential side effect of IDBT injection is urinary retention, although this is invariably transient and has a low chance of occurring. 6 Nevertheless, in the contemporary surgical community, a significant emphasis is placed on patient education about the potential for post-injection urinary retention, which may require clean intermittent self-catheterisation (CISC).7,8 Previous research has suggested that formal CISC education before IDBT may be unnecessary. 9 While explaining the potential risk of CISC requirement is important, no CISC teaching or implementing a selective CISC education policy could yield substantial healthcare savings, improve efficiency, and enhance the patient experience without compromising clinical outcomes.
This study aims to determine the rates of CISC following IDBT at our facility and evaluate whether routine pre-procedural CISC education is necessary for all patients. This approach could establish evidence-based local and national guidelines, potentially reducing healthcare costs while ensuring that resources are directed towards patients with genuine clinical need.
Materials and methods
Ethical approval
Ethical approval was received in June 2023 from the relevant committee prior to inititating research (Appendix 1).
Study design and population
This retrospective cohort study evaluated patients undergoing IDBT injections at our facility between September 2022 and May 2023. All new patients received in-person formal CISC education 2–3 weeks prior to undergoing their first IDBT. Patients returning for routine IDBT were evaluated retrospectively to determine if CISC education was provided at our facility or elsewhere by a Urology CNS. Demographic and clinical data were selected based on a priori literature review and included age (continuous variable), comorbidities (neurological vs non-neurological), urodynamic findings (idiopathic detrusor overactivity [IDO] vs neurogenic detrusor overactivity [NDO]), IDBT dosage (low dose ⩽ 150IU; high dose > 150IU), frequency of IDBT (<6 monthly vs >6 monthly), and visit type (first vs return visit). All CISC education sessions at our facility lasted 1 hour unless otherwise documented. This study is comprised of Level 2b evidence as per the Oxford Centre for Evidence-based Medicine Levels of Evidence (March 2009). 10
Inclusion and exclusion criteria
Patients were included if they had urodynamic evidence of DO and failed prior anticholinergic treatment. Patients were referred for IDBT following a joint decision between a specialist urologist and the patient. Patients were excluded if they had a suprapubic catheter (SPC) in situ, long-term catheter (LTC) in situ, were non-contactable after IDBT, or self-discharged from the service.
Primary outcome
The primary outcome was new or increased CISC use following IDBT. This was determined by CNS notes recorded during the 2-week post-IDBT phone consultation. Patients requiring CISC due to voiding issues or increased catheter use were included. Those who refused CISC despite clinical recommendations were excluded. CISC requirement was further categorised as transient or sustained based on follow-up records.
Secondary outcomes
The secondary outcomes were the cost of CISC education as estimated using data from the facility’s financial department for staff cost (Appendix 3) and equipment (Appendix 4), and the factors associated with new or increased CISC requirements.
Treatment and follow-up
Prior to receiving IDBT, patients were referred to a CNS for formal CISC training. This session lasted approximately 1 hour and involved the use of two single-use catheters for demonstration and patient practice. Patients underwent IDBT in a specialised clinic 2–3 weeks post-training. Two weeks after the procedure, the CNS conducted a phone consultation to assess bladder function and the need for CISC. If voiding difficulties or urinary retention were identified, patients were instructed to initiate CISC, with phone follow-up every 2 weeks until symptoms resolved or ongoing CISC was deemed necessary. All clinical interactions were documented in the patient’s medical record.
Statistical analysis
Data analysis was conducted using Jamovi software version 2.3. Pearson’s chi-square test was applied for non-parametric bivariate comparisons. Age, the only continuous variable, followed a normal distribution, allowing the use of Student’s t-test for mean comparisons between independent samples.
Results
The study initially included 79 patients. However, 12 were excluded for SPC (n = 6), LTC (n = 1), being non-contactable after IDBT (n = 3), or self-discharging from the service (n = 2). This left a final sample of 67 patients. Table 1 summarises the baseline characteristics, including sex, age, visit type, IDBT dose and frequency, urodynamic findings, and CISC history. Lower doses of IDBT, and CISC naïvity were significantly associated with new or increased CISC need, p=0.006 and p=0.003 respectively. DO subtype, idiopathic DO, trended towards significance (p=0.08). A breakdown of patient comorbidities are detailed in Table 2, with further detail available in Appendix 2.
Baseline characteristics of the patients undergoing IDBT (n = 67).
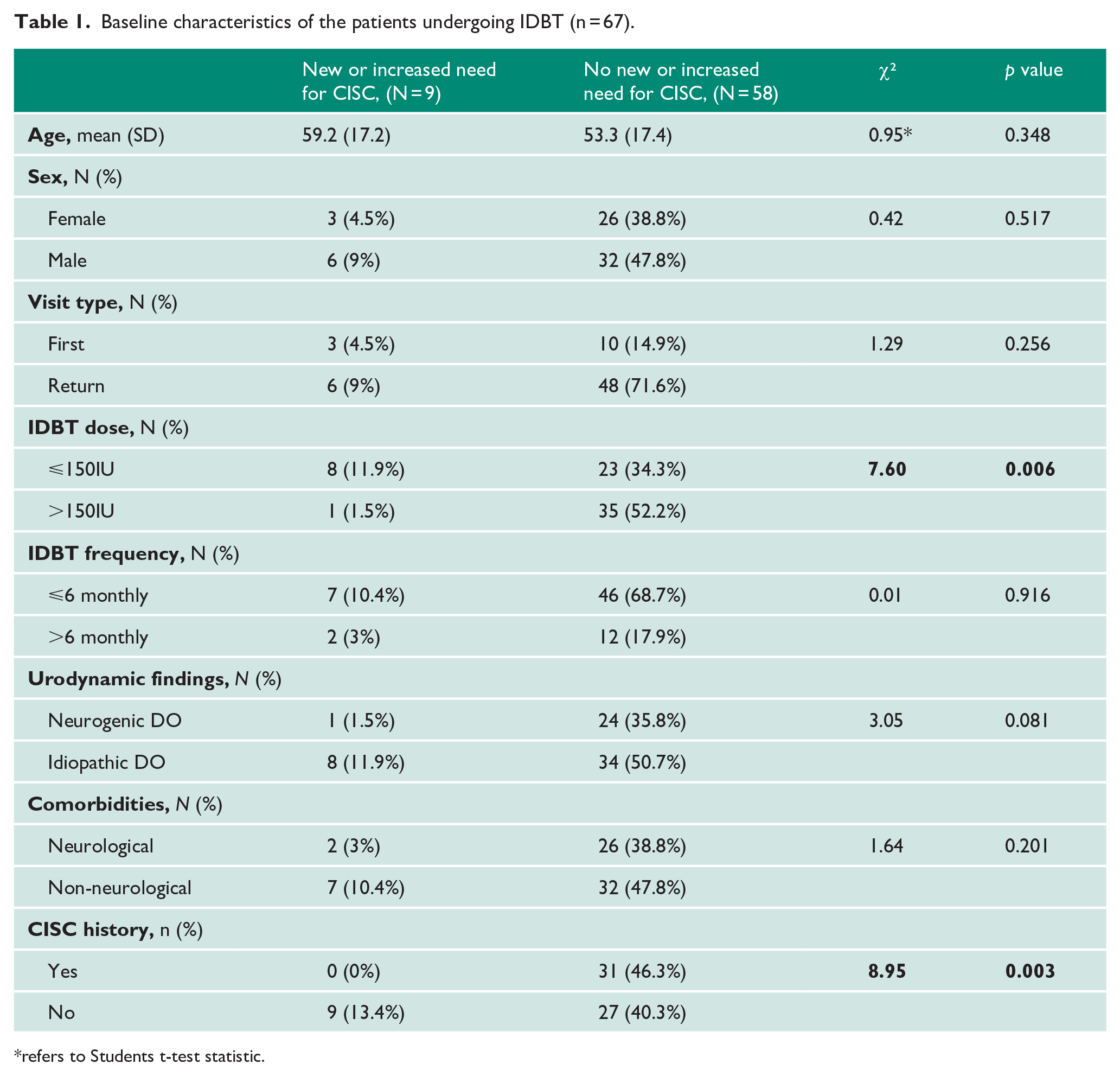
refers to Students t-test statistic.
Co-morbidities among patients undergoing IDBT.
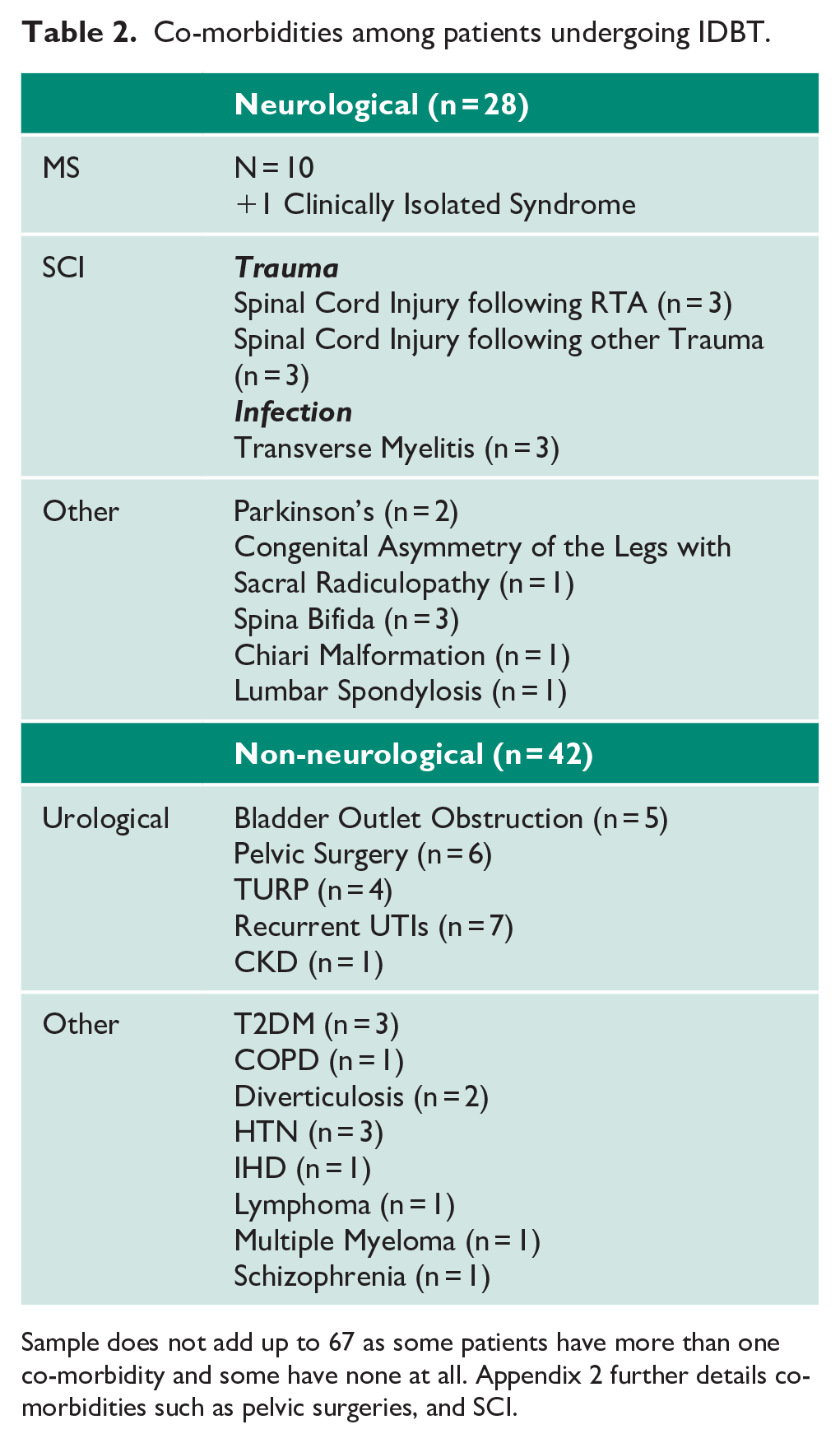
Sample does not add up to 67 as some patients have more than one co-morbidity and some have none at all. Appendix 2 further details co-morbidities such as pelvic surgeries, and SCI.
Post-IDBT urinary retention
Among 67 patients undergoing IDBT, 9 (13.4%) developed a new or increased need for CISC post-procedure. No significant differences were observed based on sex (p = 0.517) or age (p = 0.348). Urodynamic findings revealed that eight patients had IDO and one had NDO, showing a trend towards significance (p = 0.081). Patients naïve to CISC prior to IDBT were significantly more likely to require it afterward (p = 0.003). No shared comorbidities were identified among those requiring CISC, although two patients had a history of abdominopelvic surgeries. Post-procedure symptoms included incomplete bladder emptying (n = 5), dysuria (n = 2), and nocturia (n = 2). Of the nine patients needing CISC, four used it temporarily and were successfully weaned off, while five had a sustained requirement. Lower IDBT doses were significantly associated with increased CISC use (p = 0.006). No significant associations were found with injection frequency (p = 0.916) or whether the injections were initial or maintenance treatments (p = 0.256).
Subgroup analysis
Among the five patients with a sustained CISC requirement (7.5%), two required CISC once daily, while three needed it four times daily. Within the subgroup, lower IDBT doses and CISC naïvity were again found to be significant (p=0.012 and p=0.031, respectively). Males were significantly more likely to develop a new and sustained CISC requirement (p = 0.042). IDBT injection frequency was not a statistically significant predictor in this subgroup (p = 0.595). Table 3 outlines their baseline characteristics, including sex, age, visit type, IDBT dose and frequency, urodynamic findings, and CISC history.
Baseline characteristics of subgroup with sustained new requirement for CISC.
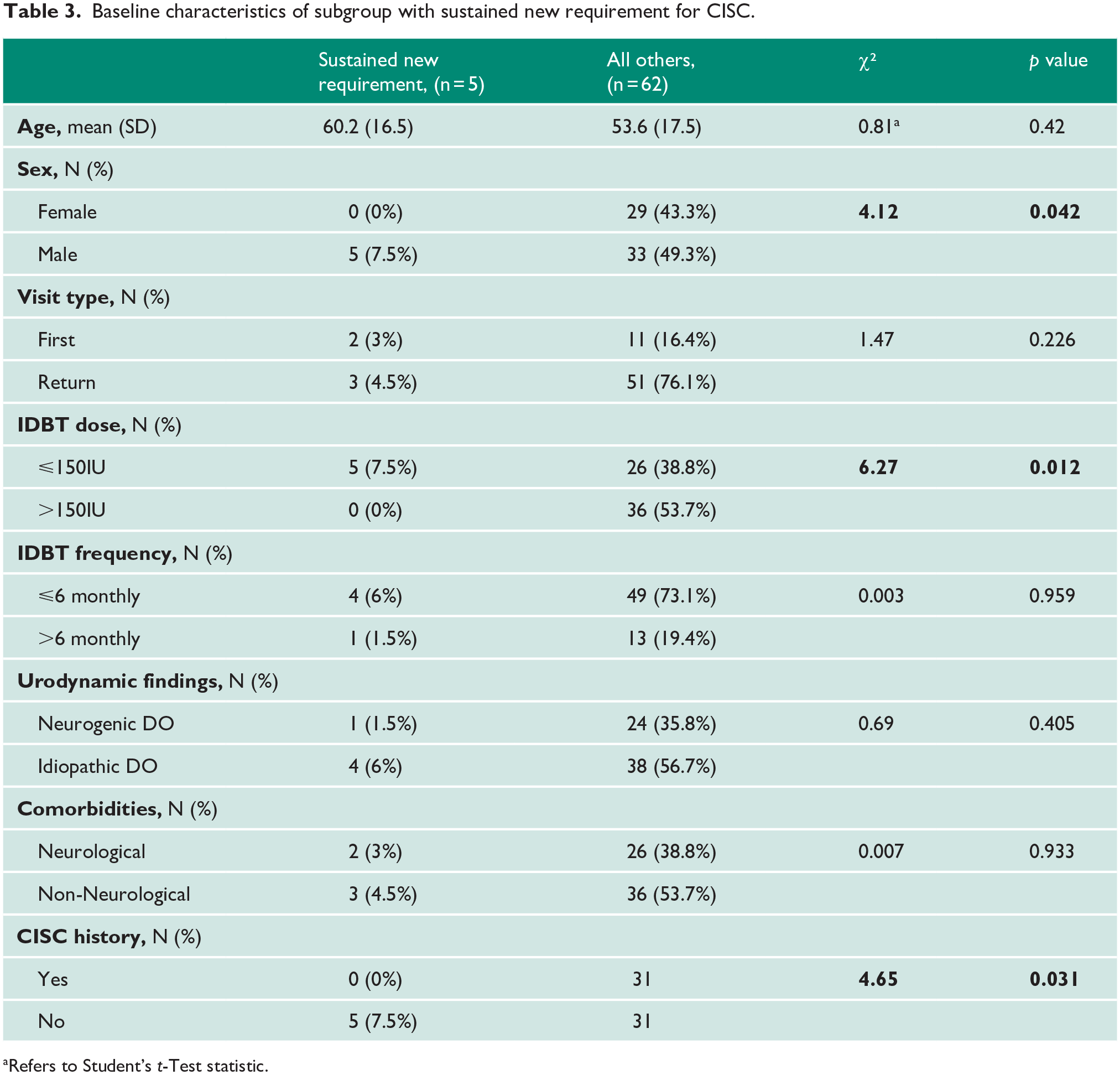
Refers to Student’s t-Test statistic.
No significant difference was observed between patients receiving their first IDBT treatment and those undergoing maintenance injections (p = 0.226). However, CISC history was a significant factor: patients without prior CISC use had a higher risk of developing sustained requirements compared to those with prior experience (p = 0.031). Within this subgroup, lower IDBT doses were strongly associated with a sustained CISC requirement (p = 0.006), while higher injection frequency showed no correlation (p = 0.959).
Costs of CISC
During the study period, 16 patients received CISC education outside our facility, while 51 were educated on-site prior to IDBT. Most educational sessions were 1 hour, except for one patient requiring 2 hours due to specific needs, considered an outlier. For the 51 patients educated at our facility, the total nursing time amounted to 52 hours, with a staffing cost of €1732.12. Including both resources and nursing expenses, the total cost of providing CISC education to these patients over 9 months was €3240.82, averaging €63.55 per patient.
Discussion
Our results showed a urinary retention rate of 13.4% post-IDBT, where urinary retention is defined as a new or increased need for CISC following IDBT. This reflects the rate among a heterogeneous group of adults where age and sex are normally distributed. Our study reiterates rates in larger populations with similar baseline characteristics.11,12 Subgroup analysis of patients with a sustained new or increased requirement for CISC following IDBT resulted in a figure of 7.4%. This figure appears to correspond with studies comprising less rigorous criteria for CISC initiation following IDBT, along with more stringent inclusion criteria for their study population, excluding patients using CISC pre-operatively.13,14 Similar to our findings, studies which include patients using pre-operative CISC tend to reflect higher overall rates. However, de novo rates of urinary retention remain in keeping with current literature. 15 Notably, urinary retention following IDBT is inconsistently defined, with a lack of globally accepted guidelines for diagnosis, leading to highly variable rates and preventing an accurate assessment of true retention rates among a given study group.16,17
In our cohort, urinary retention was significantly associated with lower doses of IDBT, specifically doses less than 150IU. This is contradictory to many other studies suggesting higher doses are linked to higher rates of urinary retention, with doses >150IU often being associated with a raised post-operative PVR (>200ml). 18 Tullman et al. 19 echoed this in a study showing a significantly decreased requirement for CISC at 100IU when compared to 200IU of BoNT/A. This association remained significant in our subgroup analysis of patients with sustained new requirements for CISC. Notably, there are very few studies in the literature focused on IDBT dosage as a predictor of urinary retention. However, in our study, naivety to IDBT was significantly associated with CISC requirement; therefore, we hypothesise that the true association is not with lower doses of IDBT but bladder muscle naivety to IDBT itself, resulting in increased CISC need. This appears consistent with contemporary literature from Abrar et al., 20 which reflects a trend towards significance with lower doses of IDBT.
The subgroup analysis showed a statistically significant increase in sustained new or increased requirement for CISC in male patients (p = 0.042). These findings support Jiang et al. 20 and Abrar et al. 21 who both concluded male sex is an independent risk factor for adverse events following IDBT. Similar findings were seen in a larger scale study across 5 years by Kuo et al. 22 Nevertheless, there remains a paucity of studies focused on adverse events and outcomes of IDBT in males when they constitute a significant proportion of patients with OAB. 23 Previous literature, though it may be sparse, combined with the results of this study, emphasises the need for specific CISC education in the male gender cohort prior to IDBT.
Our study reflected a tendency towards the significance of the OAB subtype when reviewing patients who had a new or increased need for CISC following IDBT (0.081), with only one patient of the group having NDO and all others IDO. This echoes a large-scale clinical trial, the RELAX study, where women with IDO underwent IDBT; retention rates as high as 25% were observed in the cohort. 24 Unfortunately, there are no comparable adult studies for NDO, likely due to iatrogenic urinary diversions such as LTC, SPC, or urostomies being created for this cohort making urinary retention difficult to measure. A large-scale investigation of patients with NDO reported that over half of the patients had urinary diversions. 25
In terms of cost-benefit analysis, our facility spends €63.55 per patient on CISC education, with an overall cost of €3,240.82. However, only 9 of the 51 patients educated required CISC, reflecting a cost of €571.95. Directly comparing this cost to the system-wide cost of emergency department (ED) CISC use due to urinary retention following IDBT would be useful however this cost is difficult to define and most cost-effective analyses do not specifically report it. However, an American systematic review of 5-year cost analysis following IDBT reported an average cost of $867.36 (~€755.24) per patient presenting with acute urinary retention. 26 While this does not include an isolated breakdown ED CISC cost, removing the price of CISC education computed in our study there remains a significant cost burden even when allowing for intercontinental healthcare system differences. While there are no European equivalent studies available, and our institution offers emergent access to specialised urology clinic thus avoiding ED presentation, we can infer the cost of emergency intervention far outweighs the price of educating the high-risk population, further strengthening the findings of this study. If we focus our educating hours and equipment on males with IDO, 66% of the patients with the new or increased requirements would be educated, and almost 90% of the patients with the sustained new requirement would be educated with a cost saving of €2668.87. Moreover, all patients with a new or increased requirement for CISC (n = 9) following IDBT self-reported symptoms at the 2-week phone consultation with the CNS. This echoes findings from Aldrich et al., 9 who concluded that routine follow-up may not be necessary as patients will acknowledge troublesome voiding and will seek medical intervention if required.
A limitation of our study was that data regarding urinary retention were self-reported by patients without measuring a numerical PVR, subjective symptomatology may lead to less accurate results. Another limitation was that the nursing hourly pay rate was not inclusive of employer’s social insurance deductions or annual leave, which may lead to minimal numerical discrepancies.
Conclusion
This study reveals that males are at a higher risk than females for sustained CISC requirements, and patients with IDO demonstrate a trend towards higher risk. To optimise cost-effectiveness, we recommend leveraging these associations to target physical education on catheterisation. Specifically, prioritising facility funding for educating males with IDO who are naïve to IDBT could effectively address approximately 90% of patients with sustained new or increased CISC needs in our cohort.
Footnotes
Appendices
Co-morbidities further details.
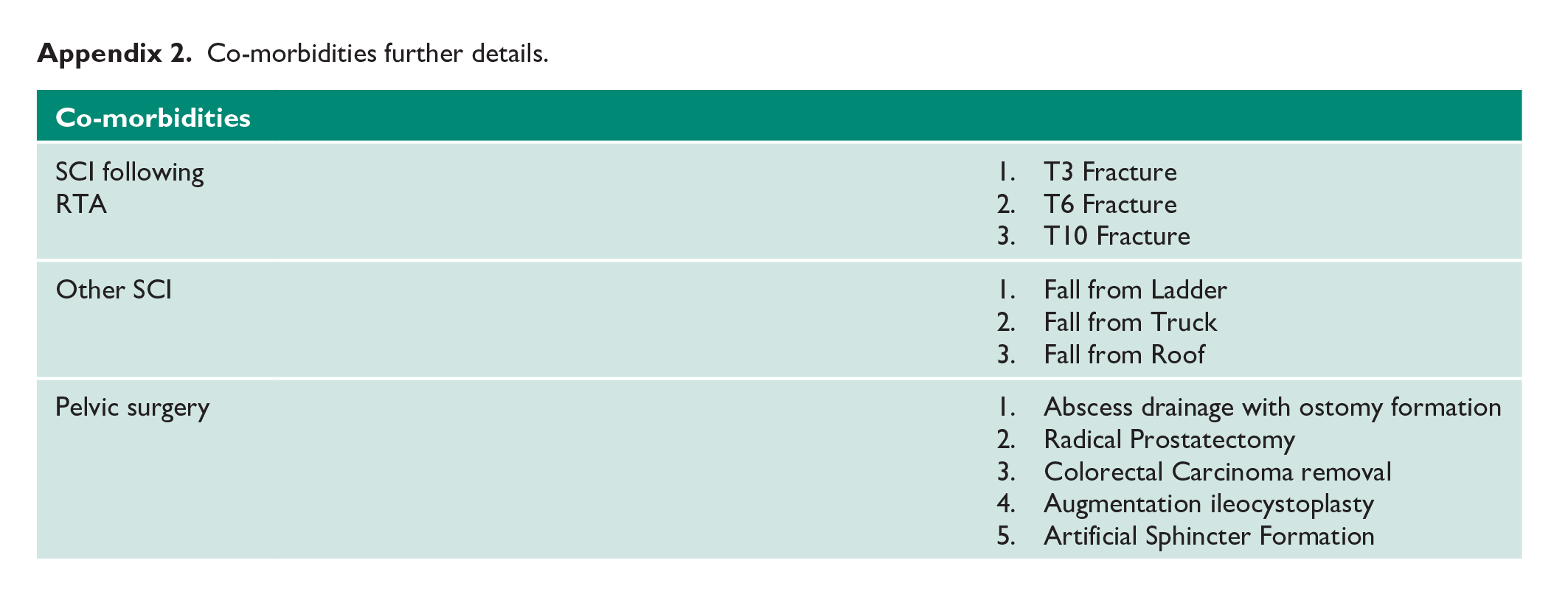
|
|
|
|---|---|
| SCI following RTA | 1. T3 Fracture 2. T6 Fracture 3. T10 Fracture |
| Other SCI | 1. Fall from Ladder 2. Fall from Truck 3. Fall from Roof |
| Pelvic surgery | 1. Abscess drainage with ostomy formation 2. Radical Prostatectomy 3. Colorectal Carcinoma removal 4. Augmentation ileocystoplasty 5. Artificial Sphincter Formation |
Acknowledgements
The authors express their sincere gratitude to Mr Derek Hennessey for his constant guidance, supervision and mentorship throughout this project. They thank Mr Ciaran Brady and Mr Paul Sweeney and the entire Urology Department in the Mercy University Hospital for making this project possible.
Conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical considerations
Ethical approval was received from Clinical Research Ethics Committee (CREC) of Cork Teaching Hospitals, Ireland, prior to initiation of data collection (Number: ECM 4 (f) 09/05/2023 & ECM 3 (ee) 20/06/2023).
Consent to participate
Patient consent was not required as per CREC guidelines, retrospective analysis reviewing existing medical records that were collected as part of standard clinical care.
Consent for publication
Not applicable.
Data availability statement
Data are freely available within our institution and can be shared upon request. We give permission to reproduce this material.
Guarantor
D.B.H.
Contributions
D.B.H. and C.B. conceptualised the project and developed the methodology; M.H., J.O.B., and O.T.C. acquired the data; O.T.C., and D.B.H. analysed and interpreted the data; O.T.C. drafted the manuscript; D.B.H. and C.B. revised it critically for intellectual content; O.T.C., C.B., and D.B.H. approved the final manuscript, submitted and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
