Abstract
Objective:
To examine the readability of urology webpages to assess their suitability for the general population and their inclusivity for varied levels of health literacy.
Methods:
We accessed all urology department websites from NHS trusts in England. A standard framework was used to assess these for ease of navigation, availability and quality of urology-specific information. Text was analysed using Flesch–Kincaid Grade Level and Ease Score to measure readability.
Results:
From the 132 NHS trust websites investigated, 117 (88.6%) had a urology-specific webpage, a considerable increase from 98 trusts (68%) in 2010. However, a smaller proportion of websites explained their services and procedures, and only 23.9% explained common urological conditions. Websites still appeared outdated, 23.9% had spelling errors, and 75.2% made none or poor use of images. The mean reading grade level was 13.40, equivalent to a UK reading age above 18 years, and the mean reading ease score was 30.35, in the range of ‘difficult’ text.
Conclusion:
Our data suggest that urology-specific webpages are not providing useful content for patients and are too complex for the general population to understand. Improvement would allow patients to be able to utilise such resources to aid decision making and to navigate complex NHS pathways.
Level of evidence:
Not applicable
Introduction
NHS webpages provide patients with information on their treatment and care, and, when built to a high standard, can encourage patients to become informed decision-makers.1–3 As well as providing good quality relevant content, NHS websites should be accessible to all patients, including patients with lower health literacy rates4,5 complex care needs 6 and elderly patients.7–9 Greater health literacy is associated with a higher inclination to seek health information online, and is also positively correlated with better health outcomes10,11 as they are able to navigate online resources, better understand their treatment and ultimately become more able decision makers. A significant population of individuals with low health literacy may thus experience barriers, making it vital that NHS websites have a suitable readability for the general population. The NHS Digital toolkit advises that medical pages within the NHS should aim for a reading age of 9–11 years old as it suggests that 93% of the UK population has an average reading age of 10 years.12,13
In 2011, a study reviewed NHS Trust urology websites in England and found that 68.6% of the trusts providing urology services in 2010 offered a urology-specific webpage with varying levels of overall quality. 14 Our aim was to measure the readability of urology webpages by using the Flesch–Kincaid Grade Level (FKGL) and Flesch–Kincaid Ease Scores (FKES), in order to explore the accessibility of urology-related content for the general population. By using an adapted framework assessing ease of navigation and availability of urological content we also aim to evaluate the overall change in quality of urology websites.
Methods
From the NHS service directory, 132 trusts were identified as providing urology services out of a total 228 trusts in England. 15 The urology-specific websites from these trusts were examined using an adapted framework from March to August 2019. 14 The presence of a urology-specific webpage was first established, and ease of navigation was assessed. The availability and quality of relevant information on the urology-specific websites was examined by recording whether they provided explanations for common conditions and information on urological procedures. Availability of patient information leaflets (PILs), links to the British Association of Urological Surgeons (BAUS) website and to other useful external sources within the urology webpage were also noted. In addition, links to charities, use of images/videos, location and clinic details, and support groups were recorded, as well as referral guidance for healthcare professionals. Significant components to the accuracy of the webpage including any errors (e.g. broken links) and ‘date of last update’ were further recorded.
The readability of the available urology websites was assessed by extracting the main body of text from the urology webpage (excluding URLs, image footnotes, websites headers and toolbars) and analysing the text using the readability statistics function in Microsoft® Word (Version 16.27). This provides measures of the FKGL and FKES, as well other related statistics (e.g. number of sentences). The FK readability formula is a well-regarded and commonly used method for assessing readability in the USA, and has previously been used by studies investigating NHS PILs. 16 FK readability scores give an objective measure of how easy a passage of text can be understood by taking into account the average number of words per sentence and average syllables per word.
Results
Compared to data from 2010, 14 there has been an increase in the number of trusts providing a urology-specific webpage from 98/145 total trusts in 2010 to 117/132 in 2019 (Figure 1). Around half (49.6%) of the trusts in 2019 provided over two pages of urology-specific webpages, as opposed to a single page of information. Almost all websites (96.6%) were accessible by the services tab of the trust’s homepage, and slightly less (92.3%) were accessible by the search function.
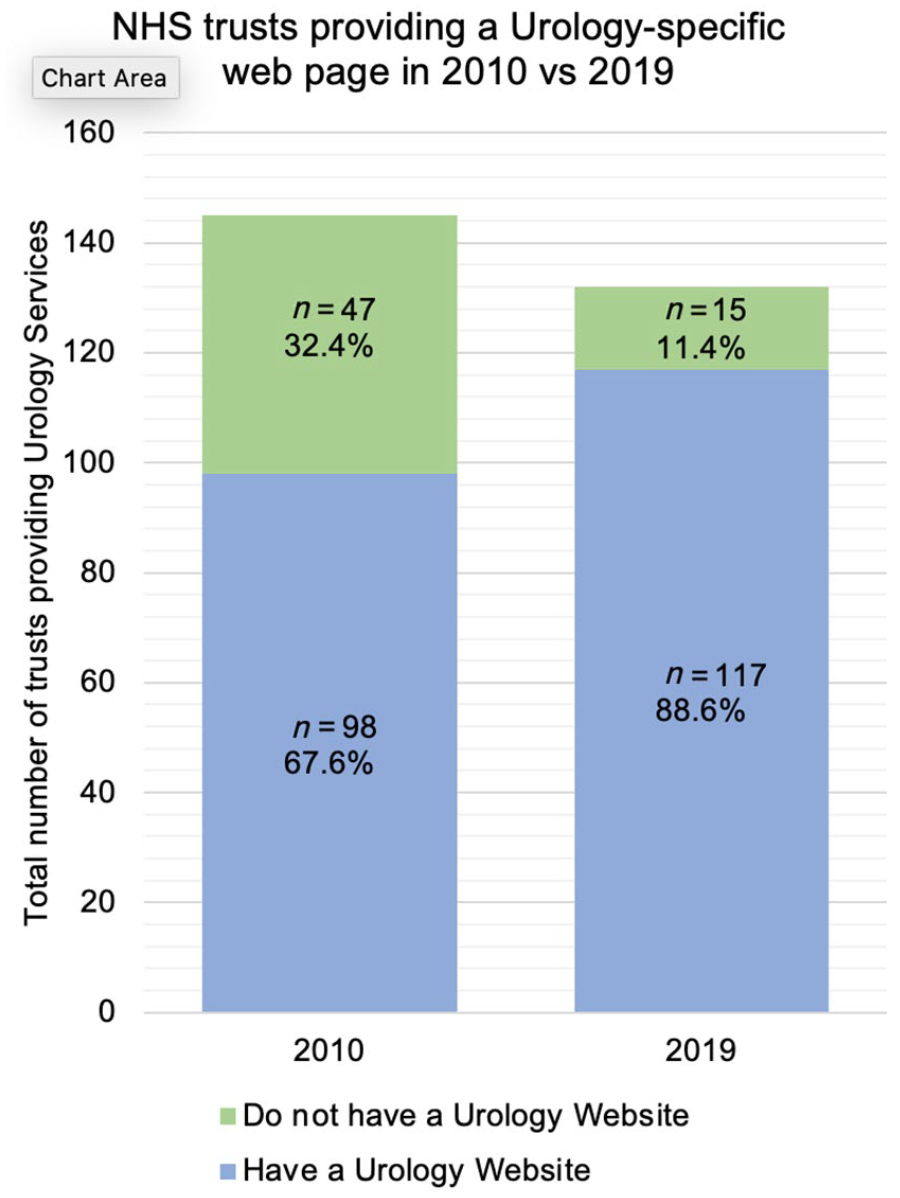
Proportion of NHS trusts providing a urology-specific webpage in 2010 v. 2019.
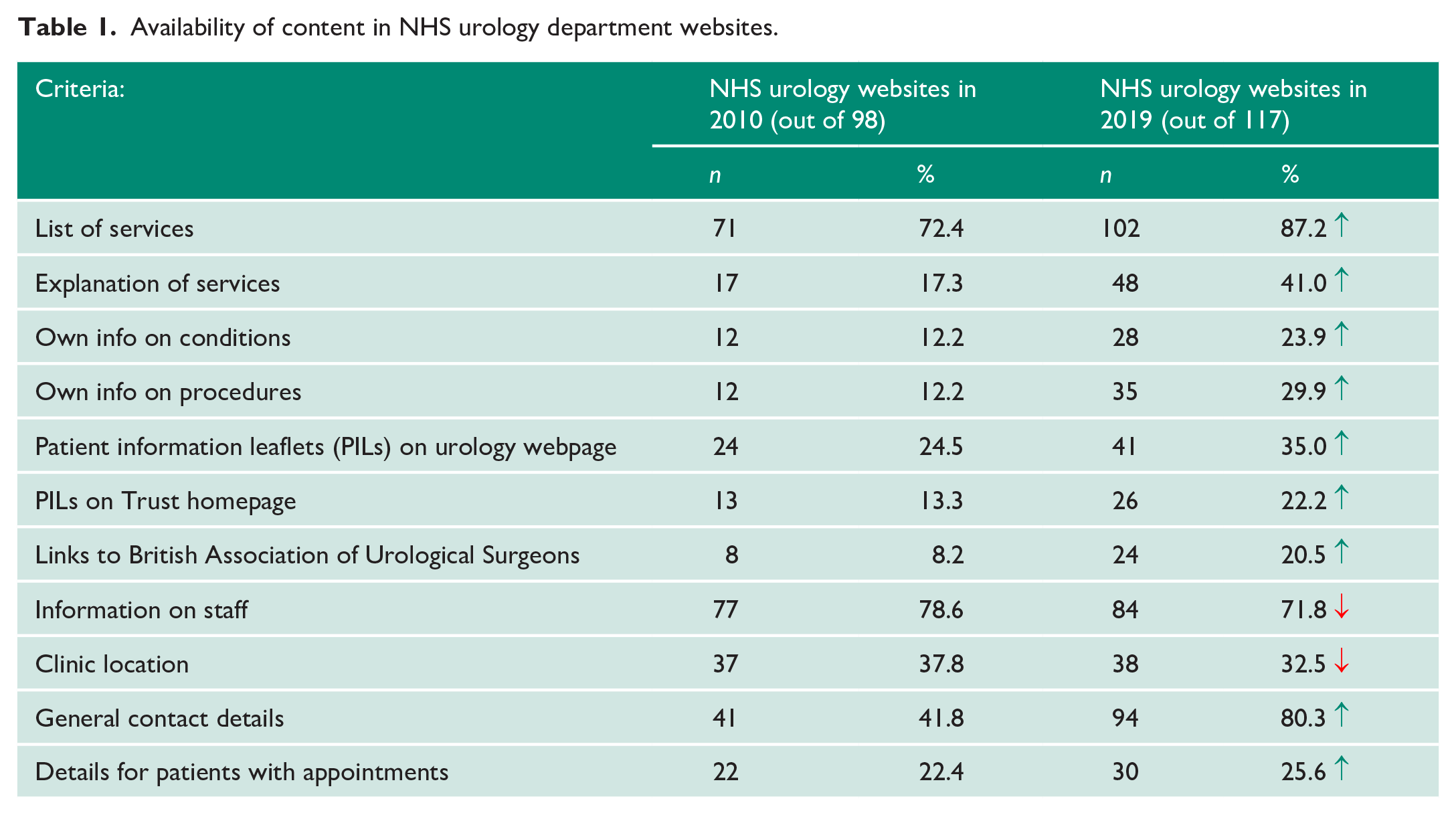
There was an overall improvement in the provision of urology-related content (Table 1), with a particular increase in the explanation of urology services provided, allowing patients to more clearly understand the services available to them. However, less than a third of websites gave specific information to explain and describe common conditions and procedures (e.g. ‘What is lithotripsy?’). PILs were also only available on 41/117 websites, and less than a quarter provided links to BAUS. Though not investigated in 2010, a third of websites in 2019 provided links to charities or support groups with Prostate Cancer UK being commonly provided. For contact details, 94/117 websites provided some form of contact information, most commonly as a general phone number. Only a quarter gave specific advice for patients with appointments, such as how to prepare for and what to expect at their visit. A quarter of websites also had some form of error (including 13 websites with broken links, nine directing to missing information and three with broken search functions).
Availability of content in NHS urology department websites.
Of the 117 websites accessed for readability and word count, over two-thirds had less than 500 words of information in total on their urology webpage, with 46/117 having less than 250 words and an average of only six sentences. Alternatively, 24/117 trust websites had more than 1000 words of text. Readability was assessed for 113 websites, as four had too few words necessary for analysis. The overall mean FKGL for these 113 websites was 13.40 (range = 7.9–18.9) equivalent to a UK education level of Year 13 and age of 17–18 years (Figure 2). The overall mean FKRES was 30.35 (range = 5.4–67.7), equivalent to a reading ease of ‘difficult text’ from FK standards (Figure 3). Finally, a total of 28/117 websites had spelling errors.
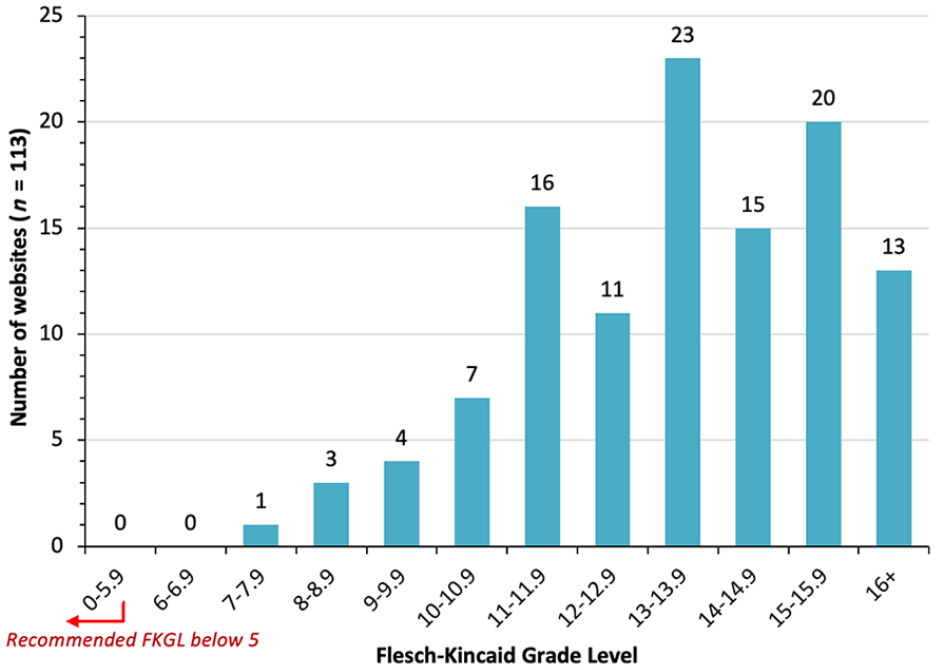
Flesch–Kincaid Grade Level scores (readability) of the text from the 113 NHS urology-specific webpages investigated in 2019.
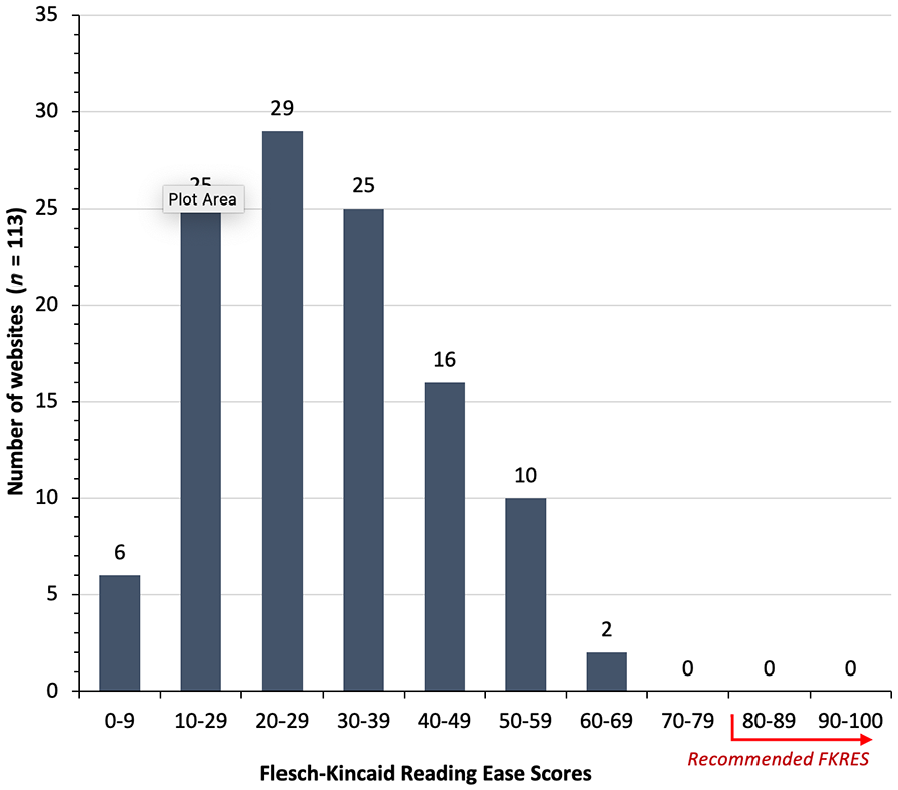
Flesch–Kincaid Reading Ease score (readability) of the text from the 113 NHS urology-specific webpages investigated in 2019.
Discussion
NHS Trusts have made improvements in their provision of urology-specific webpages since 2010; however, 15 trusts with a urology department still have no official website as of August 2019.
Undoubtedly some of the most important aspects of a useful urology website is the availability of relevant content. Most websites provided information on services, and a small proportion (slightly higher than in 2010) explained common conditions and procedures, information that could be considered vital for patients who are seeking to learn more about their health condition and future treatments. It could be argued that this information is usually explained during a face-to-face consultation; however, not all patients may feel comfortable in asking questions, there may be time constraints or patients may simply prefer to read information for themselves to become better prepared. Similarly, whilst PILs are provided, these may not explain everything a patient wants to know, or alternatively, may be too complex for patients to understand. 17 Only a quarter of websites provided guidance for patients with appointments, such as how to prepare and what to expect from their visit. Considering the invasive nature of some treatments and investigations, this demonstrates a shortfall in trusts preparing their patients for their expectations of the service.
There has been an increase in the number of websites providing links to BAUS, and a third also linked to relevant charities that could help support patients. Many websites also provided contact details and many provided information regarding staff in the department (particularly regarding consultants). However, worryingly only 16 websites gave a ‘date of last update’, with one website not having been updated since 2012, potentially providing old and inaccurate information. With NHS websites considered a reliable source of information, they should be monitored and regularly updated.
In relation to readability data, NHS recommends aiming for an average reading age of 9–11, thus NHS websites should have a FKGL of 5 (age 11 equivalent) or below and a FKRES of above 80 (considered ‘easy text’). The overall mean FKGL investigated was very high at 13.40, corresponding to the UK education grade system above grade 13 (sixth form). The mean FKRES was equally high at 30.35, indicating a ‘difficult’ text, usually the level used when aiming content at college graduates. The readability level of the websites is therefore beyond the advised level of 9–11 years for the general population. Importantly, no websites in our investigation were in the recommended FKGL and FRES levels. These results fall in line with recent investigations into the readability of health information online in the UK18–20 and depict a worrying conclusion about the readability of available health information online. Considering that patients will be accessing these sites to understand more about their condition or symptoms, a high readability is a significant constraint and may only allow certain patients with adequate literacy to make use of this resource. Fortunately, not all websites were poor in this regard with some displaying useful diagrams and medical glossaries.
Limitations to this study may include the use of the FK readability tests, which take into account the number of words and syllables, but fail to interpret the complexity of the lexis itself. In future analysis of online health information, it may be beneficial to combine multiple readability methods to more accurately assess comprehension of health-related text. 21 Certain medical terms were used frequently in the investigated urology websites, such as ‘HoLEP’ or ‘haematuria’, which might not be analysed by FK as a high readability age text, but are clearly terms that would warrant further explanation for most urology patients to be able understand them. Websites may therefore have used complex language which has not translated into a high FKGL or FRES. Furthermore, whilst a low readability may indicate that a website is at a suitable reading age, this does not mean that it is a functional or useful website for patients. Such websites may still lack in other useful components such as relevance of content or ease of navigation. Similarly, a text with a high readability may be considered a good website by a urology patient if the website is effectively explaining certain medical concepts. Thus readability is not an exclusive indicator of a good quality urology website. We emphasise that multiple components including readability, ease of navigation, availability of content and clarity are all inherent factors required for a urology website to fully support health-information seeking behaviour by patients, and facilitate the development of well-informed patients.
Conclusion
Patients today want to learn more about their health, and most are using the internet in order to do so. NHS urology websites could act as a single reliable resource for patients and could be of immense value, but many websites are still lacking in quality and may not be considered comprehensive. Current NHS urology websites are also doing poorly in terms of readability, and should thus be adapted for the general population, using recommended guidance from NHS Digital. 13 Individual NHS Trusts need to take responsibility for the information they provide online. It is their duty to provide high-quality information for patients to be able to act as informed decision makers in the collaborative healthcare environment that the NHS is striving so much to create.
Footnotes
Acknowledgements
We would like to thank Miss Mary Garthwaite for her assistance and encouragement on this project.
Conflicting interests
The authors declare that there is no conflict of interest.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
The study has been registered as an audit as per local guidelines.
Informed consent
Not applicable.
Guarantor
MB.
Contributorship
MB and KT designed and directed the project. CP collected data and wrote the first draft. All authors reviewed and approved the final draft for submission. CP prepared and submitted the manuscript for publication.
