Abstract
Introduction and aim
The popularity of complementary and alternative medicine (CAM) in treating functional gastrointestinal disorders (FGIDs) has steadily increased in Western countries. We aimed at analyzing available data on CAM effectiveness in functional dyspepsia (FD) patients.
Methods
A bibliographical search was performed in PubMed using the following keywords: “complementary/alternative medicine,” “hypnosis,” “acupuncture” and/or “functional dyspepsia.”
Results
In community settings, almost 50% of patients with FGIDs used CAM therapies. Herbal remedies consist of multi-component preparations, whose mechanisms of action have not been systematically clarified. Few studies analyzed the effectiveness of acupuncture in Western countries, yielding conflicting results and possibly reflecting a population bias of this treatment. Hypnosis has been extensively used in irritable bowel syndrome, but few data support its role in treating FD.
Conclusions
Although some supporting well-designed studies have been recently performed, additional randomized, controlled trials are needed before stating any recommendation on CAM effectiveness in treating FD.
Introduction
Patients’ requests for a “holistic” treatment to functional gastrointestinal disorders (FGID) have been steadily increasing in recent years.
1
Nonetheless, this approach is often dismissed by physicians, based on the perception of a lack of scientific back-up to complementary and alternative treatment (CAM).
2
The available literature on CAM has been historically limited by a poor research approach in terms of sample size, randomization, outcome parameters and statistical evaluation.1,2 However, a number of randomized, controlled trials (RCTs) have recently provided sound evidence of CAM effectiveness in FGIDs.
3
CAM is broadly defined as “Medical practices neither taught widely in medical schools nor generally available in public hospitals”
4
(Figure 1). Recent United States (US) reports suggest that CAM therapies to treat GI disorders have been increasingly employed all over the world.
4
In a Canadian community setting, almost 50% of gastroenterology outpatients were found to implement treatments with supportive CAM therapies.
5
More recently, a multicenter study of 199 FGID patients found that 64% were using diet/herbal remedies and 49% CAM as supportive treatment options.
6
Women and whites tend to use CAM more than men and African Americans do, respectively.
6
Higher levels of education, higher annual incomes and comorbid medical conditions also correlate with CAM usage.4,6 This information might be useful to gastroenterologists to determine which patients are likely to use these therapies. Regardless of the therapies employed, CAM modality is intended by patients to restore balance and to facilitate the body’s own healing responses, thereby ameliorating troublesome symptoms.
6
Definition of complementary and alternative medicine (CAM) therapy according to the Cochrane Collaboration.
According to the Rome IV criteria, functional dyspepsia (FD) refers to a heterogeneous group of symptoms arising from the epigastric region in the absence of organic disease that are likely to explain the symptoms. 7 FD pathophysiology is still uncertain but seems to be related to multiple mechanisms 8 and despite current guidelines, the treatment of FD remains unsatisfactory.7,8 Studies suggest that patients often look for person-centered care and personal physician-patient interactions. This search for a “holistic” approach might explain patients’ choice to implement prescription treatment with CAM in FD. 1 This review will focus on the efficacy, safety and clinical data of CAM in FD to improve the physician approach to this appealing therapeutic option. Consideration is mostly limited to randomized or quasi-randomized trials to avoid emphasizing the magical allure still clouding some CAM approaches.
Herbal supplements
Randomized trial of herbal supplement therapies in functional dyspepsia (FD) patients.
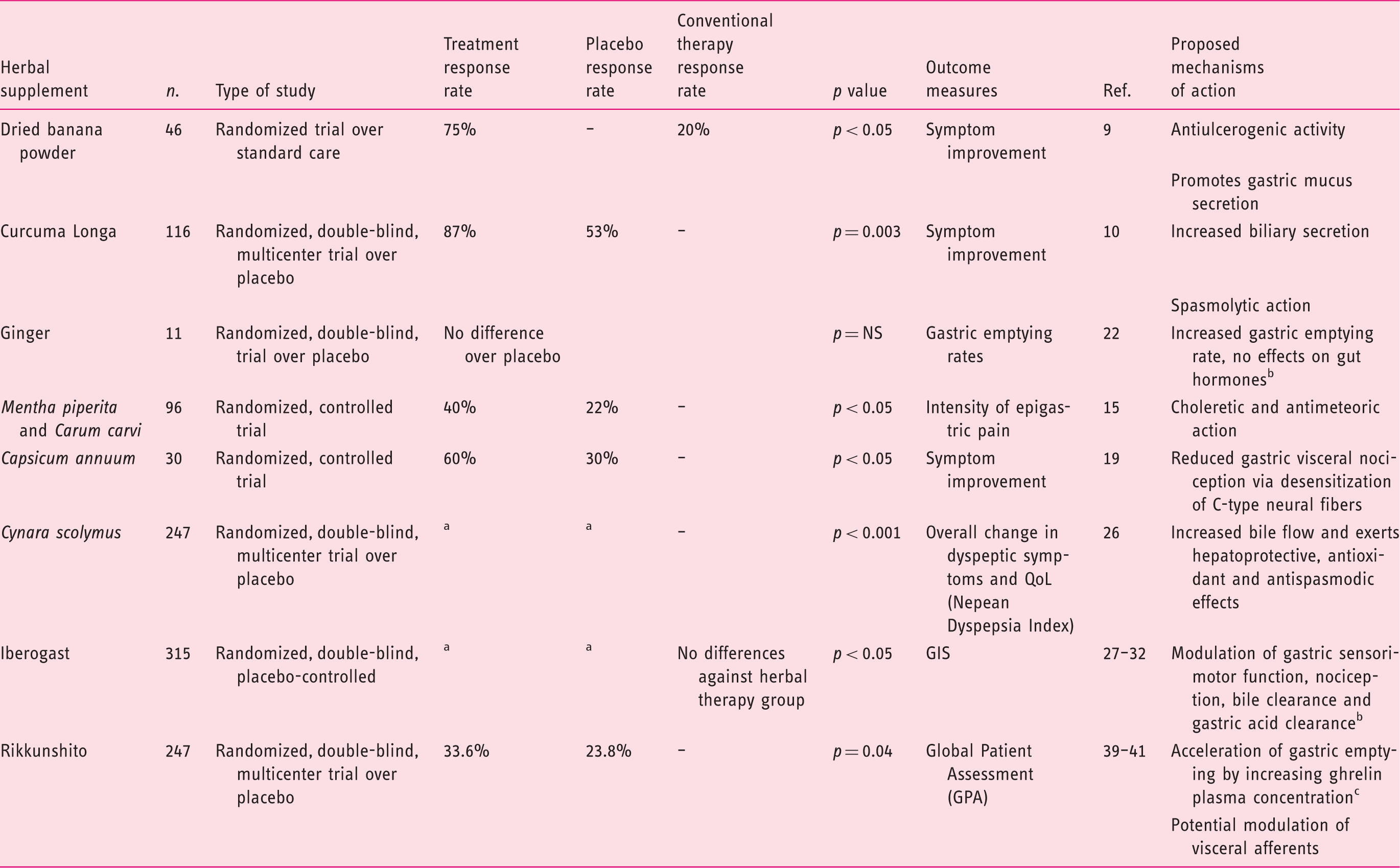
Results expressed as change in symptoms from baseline rather than response rate, by intention-to-treat analysis. bNo relationship between symptom improvement and acceleration of gastric emptying could be demonstrated in vivo. cIn animals, not confirmed in humans.
QoL: quality of life; GIS: gastrointestinal symptom score.
Traditional Chinese and Japanese medicine have been used for centuries to treat a number of symptoms, but only recently, the Kampo therapy has been systematically evaluated.
35
The ailment most studied is the rikkunshito treatment, which has been studied in Japanese scientific literature since 1500.
36
Rikkunshito is a complex herbal remedy composed of eight constituents. However, recent deeper chromatographic analysis showed that the rikkunshito formula was even more complex, revealing several additional ingredients.
35
In animal models, rikkunshito seems to accelerate gastric emptying by increasing ghrelin plasma concentration, but human studies are inconclusive.36–39 However, a barostat study researching gastric response to environmental stress showed that rikkunshito improved gastric volume thresholds for generation of first sensation and epigastric discomfort, suggesting a potential modulation of visceral afferents.
38
A recent multicenter RCT has been run in Asia on 247 FD patients (Rome III) to compare the efficacy of rikkunshito or placebo for eight weeks.36–40 Symptomatic improvement was recorded, as well as plasma ghrelin levels before and after treatment. Approximately one-third of patients in the rikkunshito group met the primary aim, without reaching statistical significance versus placebo (
Acupuncture
Acupuncture has been used to treat FD in Eastern countries for several millennia, although the underlying mechanism remains unclear. The practice of acupuncture consists of inserting fine, solid needles (32 to 36 gauge) into selected body locations (acupoints). More than 300 points located in systematic fashion on meridians or channels of energy flow are mapped onto the body surface. Key principles in traditional Chinese medicine are that both wellness and illness result from an imbalance of A schematic representation of the four classic acupuncture points for gastric disorders: ST34 (Liangqiu), ST36 (Zusanli), ST40 (Fenglong) and ST42 (Chongyang).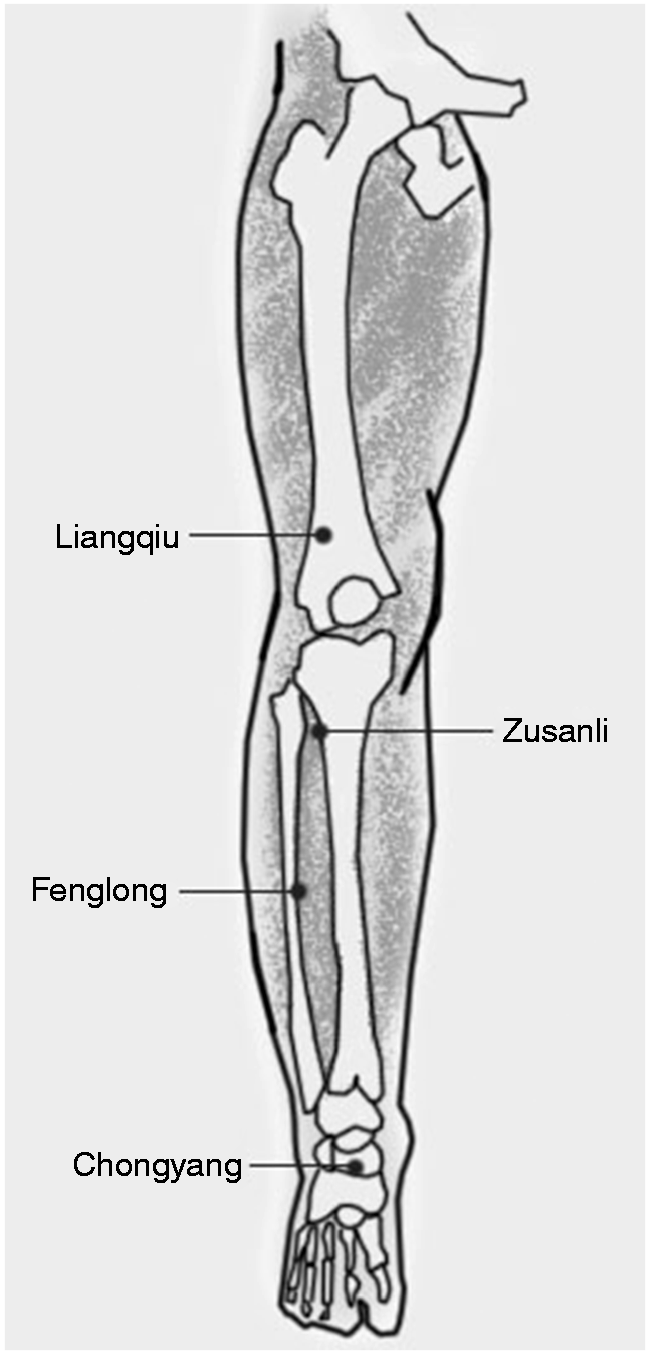
Hypnosis
Hypnosis can be defined as an altered state of consciousness, different both from sleep and normal wakefulness, characterized by highly focused attention and heightened compliance with suggestion. 49 Clinical hypnosis relies on deliberately inducing the state of hypnosis in a patient through verbal guidance, and making use of its properties for targeted therapeutic purposes. Hypnotherapy delivered as a structured, multi-session, focused intervention has been extensively used to treat irritable bowel syndrome according to the gut-focused protocols of the Manchester or the North Carolina group. 50 Recently, the Manchester group has also provided experimental evidence to support the use of hypnotherapy in FD. Calvert et al. 50 randomized 126 FD patients to hypnosis, supportive therapy plus placebo medication, or medical treatment (ranitidine 300 mg/day) for 16 weeks. Change in symptoms from baseline was assessed both short term (16 weeks) and long term (56 weeks). QoL was also measured as a secondary outcome. Hypnosis was induced using eye fixation followed by progressive muscular relaxation and deepened by standard procedures. Suggestions of improvement in gastric motor function, sensitivity and gut secretion activity were also given. At the short-term follow-up, hypnotherapy was significantly more effective than both the supportive and the medical treatment in ameliorating symptoms and QoL scores, even at long-term follow-up. In addition, general practitioner consultations for dyspeptic symptoms were dramatically decreased. The authors concluded that hypnotherapy is both an effective and cost-effective treatment for FD, but the mechanism(s) of action remained speculative. 50
Chiarioni et al.
51
studied gastric emptying by ultrasonography and epigastric sensations in 11 healthy individuals and in 15 FD patients under three conditions: (a) basal, (b) after cisapride 10 mg and (c) during 90 minutes of a gut-oriented hypnotic trance. Eight healthy individuals repeated an emptying study listening to relaxing music. Hypnosis was significantly more effective than cisapride and relaxing music in decreasing gastric emptying duration both in dyspeptics and healthy volunteers (
Conclusions
CAM therapies offer the potential to be considered in alternate and mainstream treatment of FD. An increasing body of literature provides sound evidence of effectiveness of herbal supplements in FD, although supporting well-designed studies aimed at identifying the active components, the potential receptors and the mechanism of action involved in symptom relief are needed. However, the overriding lesson seems to be that the clinical efficacy of these multi-component preparations relies on a multi-targeted approach to multifactorial disorders. Acupuncture is a traditionally accepted therapy in Asia, but its use in Western countries is far from being considered by the general population for the lack of scientific background. In the future, hypnosis might be an appealing treatment option, but studies supporting its therapeutic efficacy are eagerly awaited.
Footnotes
Declaration of conflicting interests
G.S., A.F. and M.P. have nothing to declare. G.C. is a consultant/member of the speaker’s board for: Alfa Wassermann, Allergan, Malesci and Takeda, and is a member of the Rome Foundation Anorectal Committee.
Ethics approval
Not aplicable, being this paper a review, non involving subjects or patients
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Informed consent
Not aplicable, being this paper a review, non involving subjects or patients
