Abstract
Dual biologic therapy is not often used in psoriasis and psoriatic arthritis due to cost and safety concerns, with limited literature supporting its use. We present a case of a 31-year-old man with severe plaque psoriasis and erosive psoriatic arthritis, refractory to multiple therapies. While guselkumab improved skin symptoms, joint inflammation persisted. Given the patient’s reluctance to discontinue guselkumab and his poor response to prior therapies, bimekizumab was added. This combination led to near-complete skin clearance and significant joint improvement within 3 months, with sustained benefits and no adverse effects at 17 months. This case illustrates how targeting multiple points in the interleukin-23/interleukin-17 pathway can improve outcomes in patients unresponsive to monotherapy. Dual biologic therapy may be a viable option for select patients with complex disease, though further research is needed to evaluate its long-term safety and efficacy.
Introduction
Literature on dual biologic therapy for severe cases of psoriasis and psoriatic arthritis remains limited. This approach is generally restricted for patients due to the elevated infection risk and high cost of biologics. Previous studies have reported combinations between ustekinumab plus etanercept,1–5 adalimumab,3,5,6 golimumab, or certolizumab 5 ; as well as guselkumab plus adalimumab 7 or etanercept. 1 Most patients had no serious adverse events and presented good responses to the regimens. To date, no publications have yet explored the combination of bimekizumab with other biologic treatments.
Case report
This report concerns a 31-year-old White male with severe and recalcitrant plaque psoriasis and erosive seronegative psoriatic arthritis affecting both peripheral and axial joints, demonstrated by X-ray. He also exhibits erosive changes in his shoulders and hands. His medical history is complex, including cigarette use, latent autoimmune diabetes, hypothyroidism, non-healing wounds, avascular necrosis (AVN) of both hips with synovitis, bilateral hip replacements in 2021 and 2023, in addition to multiple follow-up losses. He has been dealing with plaque psoriasis since his teenage years and was diagnosed with psoriatic arthritis in 2017, requiring the use of a cane by age 25, when he was also erythrodermic with over 90% body surface area affected. After failing a 2-year course of subcutaneous methotrexate, phototherapy, and topical treatments, he began a journey of multiple biologics with varying responses.
His biological treatment history started in 2018, with a 4-month course of adalimumab, which improved joint symptoms, but only 30% of the skin. Next, he tried ixekizumab that was stopped after 16 months, despite dose optimization, due to lack of effect on the skin and continued arthralgia. Brodalumab was then attempted but discontinued after 4 months due to minimal improvement in his psoriasis and to difficulty obtaining the medication during the COVID-19 pandemic. Rather than switching to another anti-interleukin-17 (IL-17) agent, the patient agreed to start guselkumab in 2020, leading to approximately 80% skin clearance in 6 months, the most favorable response so far. Unfortunately, he continued having marked joint symptoms. Nonsteroidal anti-inflammatories and prednisone had been contraindicated because of his right hip AVN and gastric ulcers. The patient was inconsistent in follow-up over the subsequent 2 years and was not seen in person during the COVID-19 pandemic. By late 2022, he was assessed in follow-up (Figure 1) and had a Psoriasis Area and Severity Index (PASI) of 20.9. Resistant to stopping guselkumab due to its effectiveness on his skin, the patient was hesitant to switch therapies since he had not responded to anti-TNFs or IL-17 inhibitors in the past. In addition, drugs requiring regular monitoring were not recommended due to his history of missed follow-ups. After discussing combination therapies, he agreed to the uncommon approach of adding an additional biologic to his regimen. Bimekizumab was secured, and the plan was to overlap both medications until skin clearance. Within 3 months, during the loading phase, his PASI decreased to 0.2 (Figure 2), and his joint symptoms significantly improved. Seventeen months into the combined therapy, he experienced no side effects. He still had mild skin symptoms (Figure 3) and a swollen knee, but sustained better results than with single treatment, which was the rationale for continuing his current management.
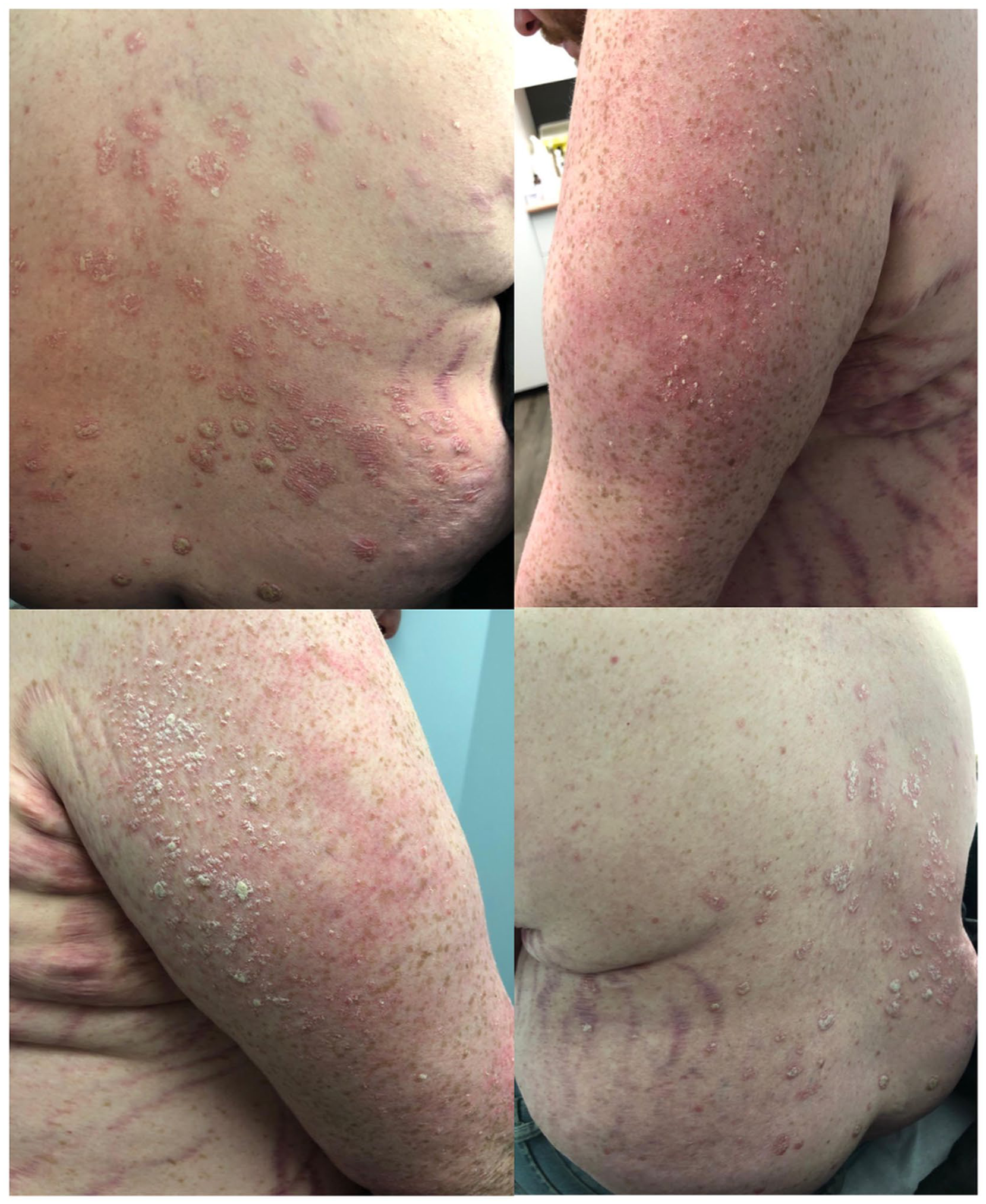
Baseline photos (December 12, 2022) of the patient’s psoriatic plaques on bilateral arms and back after recent treatment with guselkumab only. Multiple striae can be seen in this photograph from substantial topical corticosteroid use.

Follow-up photos (May 8, 2023) after 3 months on bimekizumab and guselkumab combination therapy.
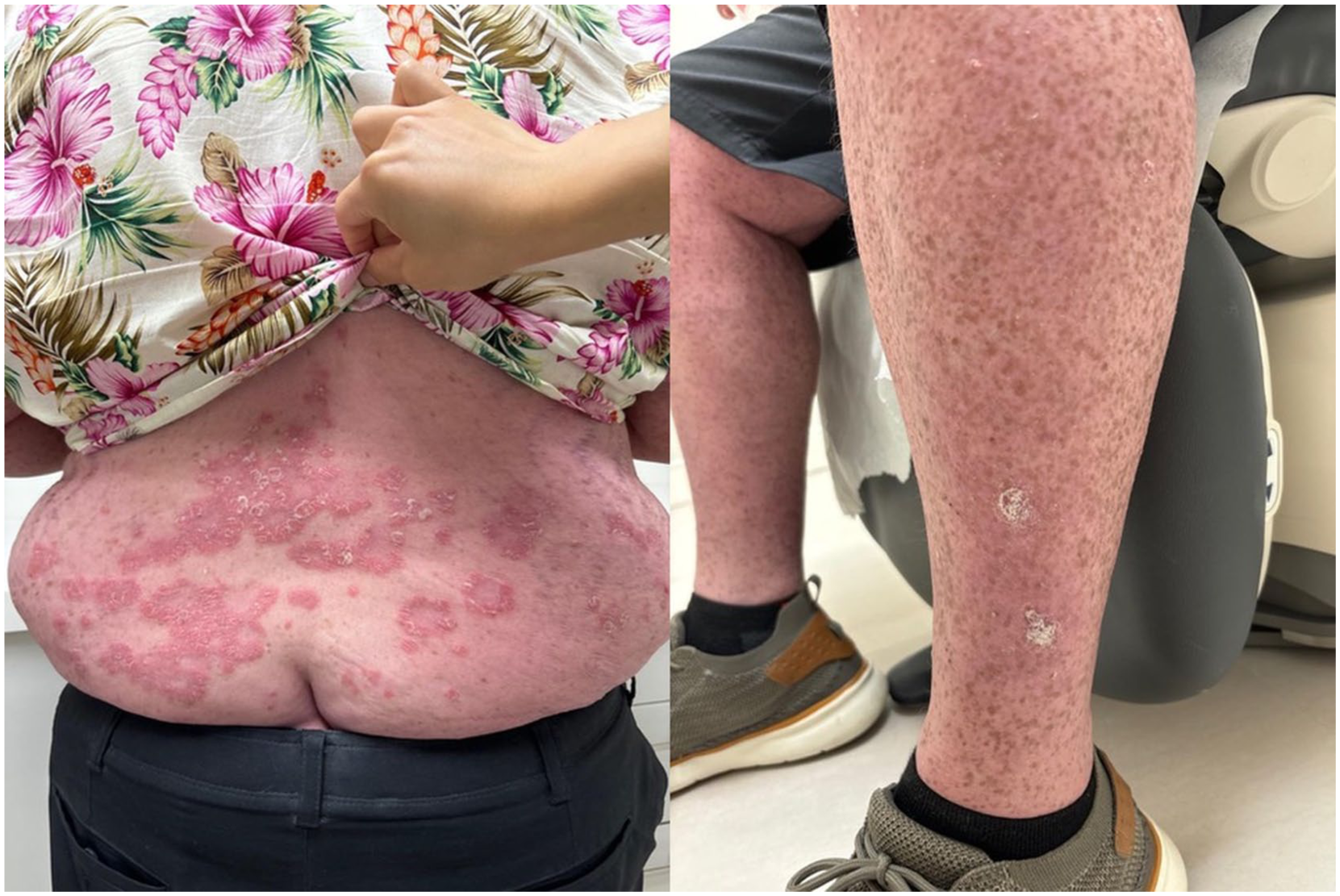
Follow-up photos (July 2024) after 17 months on bimekizumab and guselkumab combination therapy. Psoriatic plaques on the lower back and lower leg.
Discussion
Psoriatic inflammation is caused by innate and adaptive cutaneous immune responses. 8 IL-23, a pro-inflammatory cytokine, drives the expansion and differentiation of Th17 cells.8,9 The inflammatory effects of Th17 cells are then mediated by IL-17A, IL-17E, and IL-22, leading to epidermal keratinocyte proliferation. Guselkumab, a humanized immunoglobulin monoclonal antibody, targets the p19 subunit of IL-23, turning off its pro-inflammatory effects. Bimekizumab, a humanized immunoglobulin monoclonal antibody, targets both IL-17A and IL-17F neutralizing their biologic functions.9,10 The concomitant use of these biologics addresses multiple steps of the IL-23/IL-17 axis that drives psoriatic inflammation in both the skin and the joints.
This case highlights the varying responses of skin and joints to the same treatment. The patient previously experienced treatment failures with TNF-alpha, IL-17, and IL-23 inhibitors individually. However, once two molecules were combined, it led to noticeable improvements in his skin and joints. Despite the promising discoveries in psoriasis treatment, some patients unfortunately still struggle to achieve adequate disease control. In this case, the rationale for combining an anti-IL-17 with an anti-IL-23 arises from the patient’s apprehension about relapsing into poorly controlled skin disease, lack of improvement with TNF-alpha inhibitors, and difficult clinical and laboratory monitoring. In addition, the choice was influenced by the faster action of anti-IL-17 on joints. It is important to note that this patient, who relied on a cane at the age of 25 and underwent hip surgery due to severe arthritis, also battled severe skin psoriasis, resulting in erythroderma. Despite attempting multiple therapies over a 6-year period, achieving control over both skin and joints has made the current management effective. Consequently, there is hesitancy in modifying a successful and well-tolerated treatment strategy given previous multiple treatment failures.
Dual biologic therapy has its limitations. One is the high cost of these therapies, which can be a burden for the patient, health insurance companies, or the government. Another disadvantage is the potential for adverse effects. Reported side effects include one case of unstable angina requiring percutaneous coronary intervention 4 ; furuncles and autoimmune hemolytic anemia 3 ; herpes zoster flares; retrotonsillar abscess; erysipelas and bacterial pneumonia; skin infection of lower leg 5 ; as well as increased urinary tract infections/upper respiratory tract infections and hospitalization for H2N1 flu. 1 However, there are also reports of patients experiencing no side effects.2,3,5–7 Our patient was aware of the limitations, but the benefits outweighed the risks, and fortunately, no adverse events have been observed 17 months after starting dual therapy, such as candidiasis, tinea infections, inflammatory bowel disease, or systemic infections.
Considering the continuous discovery of new molecules, recognizing the safe benefits of dual biologic therapy is crucial for patients, especially the ones with severe disease. As with other chronic diseases like hypertension or diabetes, some psoriasis patients may require multiple medications to achieve symptom control. Our case report aims to inspire dermatologists and rheumatologists to explore dual biologic treatment for non-responsive patients and share their findings through publications. Further research with larger cohorts is necessary.
Footnotes
Acknowledgements
During the preparation of this work the authors used ChatGPT to reduce word count. After using this tool/service, the authors reviewed and edited the content as needed and take full responsibility for the content of the publication.
Consent for publication
Consent for the publication of all patient photographs and medical information was provided by the authors at the time of article submission to the journal, stating that the patient gave consent for their photographs and medical information to be published in print and online, and with the understanding that this information may be publicly available.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
