Abstract
This case report discusses two clinical encounters of a 62-year-old Hispanic woman initially hospitalized with suspected Stevens–Johnson syndrome, later correctly diagnosed with bullous fixed drug eruption during an outpatient visit for a similar eruption. The first encounter involved an extensive evaluation and an 11-day hospital stay, while the second was managed successfully as an outpatient with oral prednisone. This report highlights the importance of differentiating bullous fixed drug eruption from Stevens–Johnson syndrome/toxic epidermal necrolysis and emphasizes the need for a collaborative approach between Primary Care Providers and Dermatology to ensure optimal patient care.
Introduction
Fixed drug eruption (FDE) is a cutaneous adverse drug reaction that reappears at the same anatomical site whenever the individual is exposed to the offending drug. 1 Common triggers include antibiotics (particularly sulfonamides, trimethoprim, fluoroquinolones, and tetracyclines), nonsteroidal anti-inflammatory drugs, and barbiturates. Typically, within minutes to hours of exposure, well-defined, round patches that are erythematous or violaceous in color appear on the skin. 1 The condition is believed to be mediated by CD8+ memory T cells located in the basal layer of the epidermis in dormant FDE lesions. 1 Bullous fixed drug eruption (BFDE) is a severe variant of FDE, accounting for 30% of cases. 2 It can present as single or multiple lesions, or in a generalized form. Generalized bullous fixed drug eruption is rare and features numerous deep red, edematous plaques, and bullae that rupture easily, leading to widespread erosions. 2 This generalized form can resemble Stevens–Johnson syndrome/toxic epidermal necrolysis (SJS/TEN) due to their similar presentations of desquamating drug-induced bullous eruptions and full-thickness epidermal necrosis on histopathology. 3 SJS/TEN are life-threatening disorders marked by extensive epidermal and mucosal shedding, fever, malaise, and upper respiratory symptoms such as cough, rhinitis, sore eyes, and myalgias. 4 Over 80% of SJS/TEN cases are medication induced. 4 Consequently, these conditions are among the most acute drug-related reactions encountered in inpatient settings. 5 Although primary and acute care physicians are familiar with SJS and TEN, many may not recognize that bullous FDE can closely mimic conditions within the SJS/TEN spectrum, potentially leading to misdiagnosis and unnecessary treatments.
We present a case where a patient was initially diagnosed with Stevens–Johnson syndrome in the emergency department but was later correctly identified by Dermatology as having BFDE. The purpose of this report is to raise awareness among healthcare providers who encounter acute cutaneous diseases and to improve diagnostic accuracy and management by highlighting the clinical signs that differentiate classic BFDE from SJS/TEN.
Case report
A 62-year-old Hispanic woman with a medical history of rheumatoid arthritis, psoriasis, hypertension, gout, and obesity presented to the Emergency Department with widespread desquamating lesions and bullous eruptions. Upon examination, her skin revealed multiple diffuse hyperpigmented necrotic plaques that were violaceous in color, with some lesions appearing targetoid and others with inlying bullae (Figures 1(b) and 2(b)). These lesions, which had appeared 6 days prior, were located on her lower back, gluteal cleft, and both upper and lower extremities. The patient reported moderate to severe pain localized to the lesions. Her vital signs were stable, and the physical examination showed mild mucositis. Laboratory tests indicated elevated blood urea nitrogen and creatinine levels. During her hospital stay, two broad-shave biopsies were performed. Hematoxylin and eosin (H&E) staining revealed full-thickness epidermal necrosis, while Gram and PAS stains were negative, ruling out microbial infection. Direct immunofluorescence (DIF) studies showed no significant deposits of immunoglobulins (IgA, IgG, IgM), complement 3, or fibrinogen. The pathologist suggested a diagnosis of Stevens–Johnson syndrome and recommended clinical correlation. It was determined that the SJS was likely due to recent doxycycline use while on a cruise. Treatment included daily wound care, a 6-day course of IV Cefepime and Vancomycin, and a 9-day course of Solumedrol to manage discomfort. A dermatology consultation was not obtained during her admission. The patient was discharged in stable condition on day nine.

(a) Well-demarcated violaceous targetoid patch on the left thigh and violaceous-brown patch on the left leg, superimposed on a psoriatic plaque. The rash recurred in the same location during the second encounter in the Dermatology clinic. (b) One well-demarcated violaceous patch with bullae in various healing stages on the left shin, and one erythematous erosion with violaceous annular discoloration.
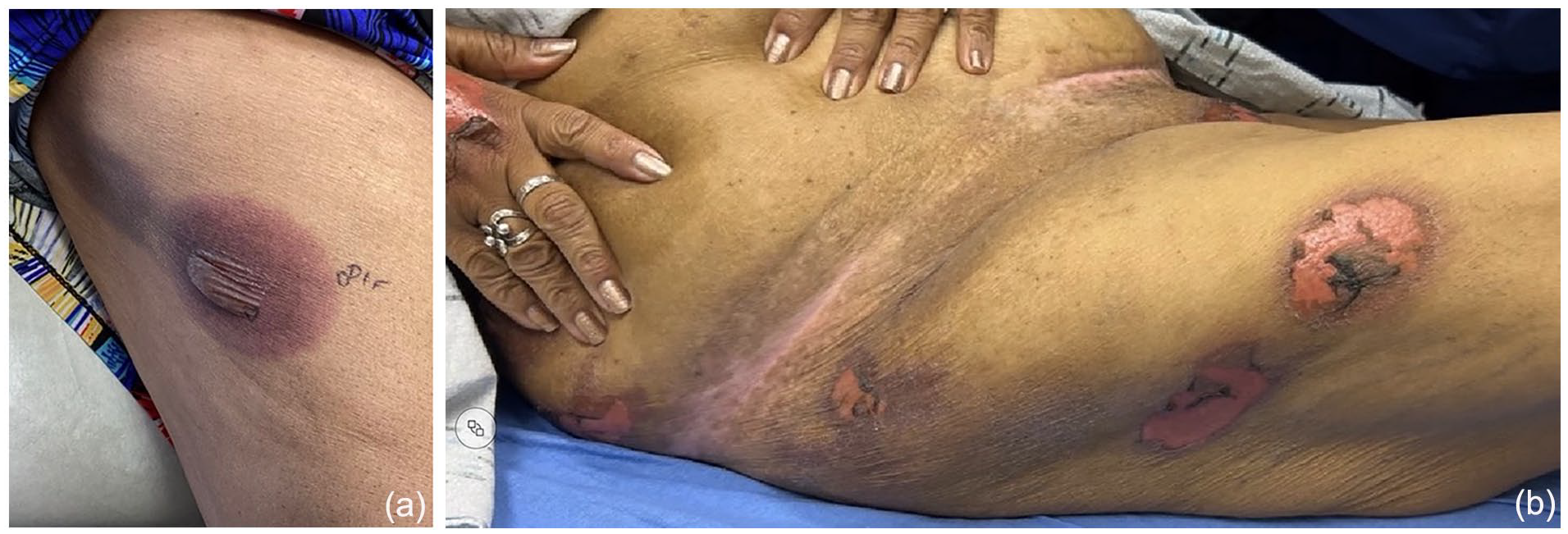
(a) Well-demarcated violaceous patch with bullae on the right lateral thigh, recurring in the same location during the second Dermatology clinic visit. (b) Two well-demarcated erythematous erosions on the right lateral thigh were observed in the ED.
Two years later, the same patient returned to our office with a similar eruption: multiple diffuse hyperpigmented smooth plaques, violaceous in color, some targetoid and others with inlying bullae (Figures 1(a) and 2(a)). These lesions were located on her bilateral lower extremities, dorsal hands, and trunk. The patient also pointed out a hyperpigmented patch on her right inner arm, which she identified as a previous rash that had led to hospitalization several years ago. At this presentation, she denied any systemic symptoms and reported that the rash had been present for about 1 week. Notably, she mentioned being exposed to a new medication prescribed by a provider at a free-standing emergency room 1 week prior.
We suspected a BFDE and performed two punch biopsies to confirm the diagnosis—one for H&E staining and another for DIF. While awaiting results, a chart review compared her current presentation to photos from her hospitalization 2 years earlier, revealing identical lesion locations, which supported the BFDE diagnosis. The pathology report returned as “Full thickness epidermal necrosis. Note: This is consistent with toxic epidermal necrolysis/Stevens–Johnson syndrome in the appropriate clinical context.” DIF studies returned as negative. Both pathology and patient history confirmed BFDE. The patient was educated about her diagnosis, given wound care instructions, advised to avoid tetracyclines, and treated with topical corticosteroids and oral prednisone. She showed good progress without recurrence.
Discussion
As demonstrated in this case, distinguishing between bullous FDE and SJS/TEN can be challenging. The following key clues may assist in making this distinction:
Constitutional symptoms are typically mild in BFDE, but severe in SJS/TEN.
BFDE rarely affects true mucosa (e.g., eyes, nose), while SJS/TEN does. BFDE may impact oral and anogenital mucosa, but these are not considered true mucosa. 5
Lesions associated with BFDE typically display a distinct red-brown discoloration in Fitzpatrick I-III patients and brown-gray discoloration in Fitzpatrick IV-VI patients, which is absent in cases of SJS or TEN. 5
Accurate differentiation of BFDE from SJS/TEN relies on a detailed medication history and lesion recurrence in the same locations. BFDE usually appears within 30 min to 24 h after drug exposure, while SJS/TEN manifests after 1–3 weeks. 5
BFDE has a better prognosis than SJS/TEN, with mild cases rarely needing hospitalization and severe cases requiring only short stays. 5 Recovery is typically within 7–10 days with no long-term complications other than hyperpigmentation. In contrast, SJS/TEN often results in prolonged hospitalizations and long-term complications such as ocular and genital scarring. 5 Accurate diagnosis improves management and reduces healthcare costs. Treatment involves stopping the offending medication and may include topical or systemic steroids. 1 In cases with extensive BSA involvement acuity of care may need to be upgraded to a Burn ICU; however, these cases are rare. 6
Histopathological analysis may not always clearly distinguish BFDE from SJS/TEN, as severe BFDE can show full-thickness epidermal necrosis similar to SJS/TEN. 5 Thus, it’s important for all medical providers, not only dermatologists, to have the skills to accurately diagnose BFDE.
BFDE frequently mimics SJS/TEN but typically follows a less severe clinical course. This case highlights key diagnostic indicators to help primary care physicians better recognize BFDE, which can reduce healthcare costs and unnecessary interventions. While these diagnostic hints aim to simplify BFDE identification, it’s important to maintain a low threshold for diagnosing SJS/TEN and to consult a Dermatologist when in doubt, as they are specialized in managing these conditions.
Footnotes
Acknowledgements
None.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Patient consent
Consent for the publication of all patient photographs and medical information was provided by the authors at the time of article submission to the journal stating that all patients gave consent for their photographs and medical information to be published in print and online and with the understanding that this information may be publicly available.
