Abstract
Exposure to certain drugs can trigger new-onset psoriasis or flaring of existing psoriatic disease. The clinical presentation of drug-induced psoriasis can vary, and although there are features suggestive of drug-induced psoriasis, there are currently no standardized criteria to differentiate it from conventional psoriasis. Patients may present with localized psoriasiform plaques, or variants such as palmoplantar, nail disease, or widespread erythroderma. Histopathology of drug-induced psoriasis can also be indistinguishable from conventional psoriasis but features suggestive of drug-induced include lack of suprapapillary epidermal thinning, a limited number of Munro microabscesses, and the presence of eosinophils and/or a lichenoid reaction pattern. We report a case of suspected drug-induced psoriasis due to dapagliflozin (Farxiga) in a 76-year-old man. Evidence indicating this to be a probable drug-induced reaction includes the sudden onset of symptoms; atypical pathology with the presence of eosinophils; and clearance of the lesions upon discontinuation of the suspected causative drug.
Introduction
Drug-induced psoriasis refers to new onset or exacerbation of psoriatic skin lesions due to exposure to certain drugs.1,2 The onset of psoriasis may vary from weeks to months to years after the introduction of the offending drug. 4 Patients may exhibit localized psoriatic plaques affecting the scalp, knees, elbows, buttocks, and genitalia.4,5 In addition, they can present with widespread plaques or erythroderma.4,5 Common causative drugs that may precipitate drug-induced psoriasis include beta-blockers, lithium, anti-tumor necrosis factor (TNF) alpha inhibitors, non-steroidal anti-inflammatories, anti-malarial drugs, and antibiotics, notably amoxicillin and tetracyclines.1,6,14 Pertinent comorbidities that may predispose an individual to drug-induced psoriasis include diabetes, hypertension, hyperlipidemia, and smoking.1,4 Histopathologic features suggestive of drug-induced psoriasis include the presence of both psoriasiform and spongiotic dermatitis, as well as eosinophils. 3 Conventional psoriasis typically lacks both spongiosis and eosinophils. 8 If there is suspicion of drug-induced psoriasis, the typical management approach generally consists of discontinuing the causative drug. However, if skin lesions do not spontaneously improve in a timely manner, patients may be treated with topical corticosteroids, phototherapy, immune modulators, or biologics. 4
Herein we report a case of probable drug-induced psoriasis due to dapagliflozin (Farxiga: AstraZeneca), a sodium–glucose co-transporter 2 (SGLT-2) inhibitor.
Case report
A 76-year-old Caucasian man presented to the dermatology outpatient clinic in early March 2023 with a 2-month history of widespread, sharply demarcated, erythematous, scaly plaques (Figure 1). The eruption initially affected his groin area and progressively worsened over a period of weeks to involve most of his trunk, proximal extremities, and scalp. No involvement of palms/soles, oral cavity, or eyes. He reported fluctuating moderate-severe pruritus.
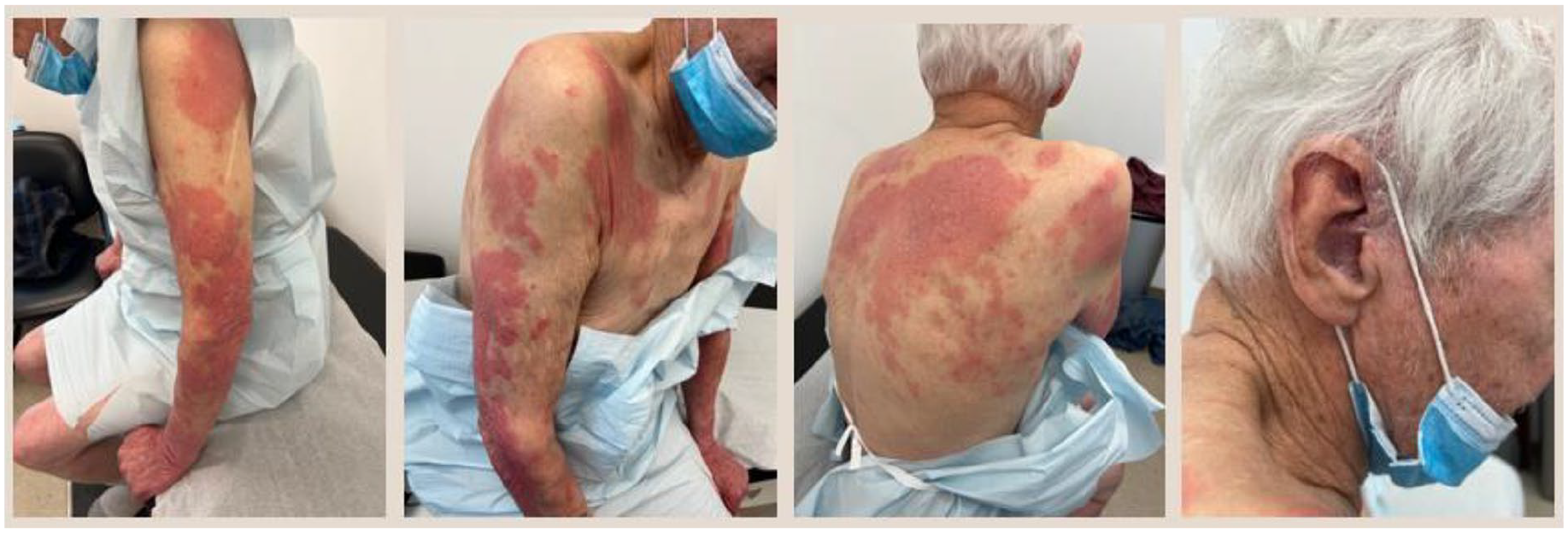
A 76-year-old male with probable drug-induced psoriasis to dapagliflozin, exhibiting well-defined psoriasiform plaques on the trunk, upper extremities, and scalp.
His medical history was significant for a remote history of mild psoriasis affecting his hands and feet (in remission for many years), hypertension, nonischemic cardiomyopathy, heart failure, severe chronic obstructive pulmonary disease (former smoker), and hearing impairment.
His medications were dapagliflozin (Farxiga) started in mid-November 2022 (approximately 7 weeks prior to the onset of the rash), eplerenone (started late December 2022), sacubitril/valsartan (Entresto), bisoprolol, toloxin, apixaban, and furosemide.
A punch biopsy was performed and showed hyperkeratosis, acanthosis, hypogranulosis with superficial lymphohistiocytic inflammation, and occasional eosinophils6,7 (Figure 2).

H&E 10× punch biopsy showing hyperkeratosis, acanthosis, and hypogranulosis with superficial lymphohistiocytic inflammation and occasional eosinophils.
A diagnosis of likely drug-induced psoriasis was made, and after a review of his medications, the patient was advised to discontinue dapagliflozin. He was prescribed desoximetasone cream and applied twice daily to affected areas as needed. He was seen in a follow-up 6 weeks later (April 2023) and had mild improvement in skin lesions. During the next follow-up appointment in June 2023, there did not appear to be any further improvement. While waiting on the results of baseline laboratory tests to consider initiating a biologic therapy, the patient had complete spontaneous clearance of plaques in August 2023 (Figure 3). There were no other changes to his medications. At the time of manuscript submission (February 2024), he has not had any recurrence.

A 76-year-old male with probable drug-induced psoriasis had complete clearance of skin lesions approximately 5 months after discontinuing dapagliflozin.
Discussion
SGLT-2 inhibitors, such as dapagliflozin, empagliflozin, and canagliflozin, improve glycemic control by reducing renal tubular reabsorption of glucose and increasing urinary excretion. These medications are commonly prescribed for patients with cardiovascular diseases or type II diabetes as they reduce cardiovascular risk and play a preventive role in diabetes complications such as chronic kidney disease. 12 SGLT-2 inhibitors have been shown to exert anti-inflammatory effects by decreasing the activation of the NOD-like receptor protein 3 (NLRP3) inflammasome, which is involved in the pathogenesis of psoriasis.9,11 Various studies have described serious cutaneous adverse events related to SGLT-2 inhibitors. Reported adverse events include generalized eruptions, urticaria, erythema, and atopic dermatitis. Cutaneous manifestations occur as early as 2 weeks following exposure to the offending drug. 13 Erüpsiyonu 10 published a similar case of a diabetic patient who developed psoriasiform plaques on their forearms after taking dapagliflozin for 1 year. This patient also had a history of plaque psoriasis. A drug eruption was suspected and subsequently supported by histopathology. He had complete resolution of skin lesions after stopping the SGLT-2 inhibitor. 10
Our case highlights an example of probable drug-induced psoriasis due to dapagliflozin (Farxiga). Three key factors made this a likely case of drug-induced psoriasis: the sudden onset of symptoms experienced by the patient; atypical pathology with multiple inflammatory patterns and the presence of eosinophils; and complete clearance and sustained remission of cutaneous findings upon discontinuation of the drug. With increased prescribing of SGLT-2 inhibitors, it is important that physicians recognize potential cutaneous adverse events.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Verbal and written informed consent for publication was obtained from the patient.
