Abstract
Exposed prosthetic grafts are a challenge to vascular specialists. Groin dissections in vascular surgery can lead to local tissue breakdown, especially in patients who have multiple comorbidities and poor nutritional status. In this report, we describe a patient with exposed prosthetic bypass conduits in the groin region which was successfully covered with bilateral myocutaneous flaps. A 75-year-old Sri Lankan male with diabetes, hypertension and Parkinson’s disease presented with bilateral non-healing wound and rest pain for 3 months. Since his premorbid status precluded the aortic cross-clamping and aorto-bifemoral graft, a decision was made to perform a right axillo-bifemoral bypass using a prosthetic graft. Re-operation was required for graft thrombectomy on the same day of surgery. His post-operative period was complicated with lymph leak and surgical site infection of bilateral groin wounds which ultimately led to exposed prosthetic graft which was fortunately patent. After optimizing his nutritional status and comorbidities, he underwent bilateral rectus femoris myocutaneous flaps to cover the soft-tissue defect over the exposed prosthetic grafts. His initial post-operative period was unremarkable except for a small area of skin breakdown. Myocutaneous flaps are preferred as they are more resilient to breakdown compared to facio-cutaneous flaps, especially in a patient with compromised blood supply. The type of loco-regional flap should be carefully selected in an individualized manner depending on the regional vascularity. The rectus femoris flap is a suitable option in terms of ease of surgical technique and durability. Comorbidities and local factors should be optimized prior to definitive reconstruction to maximize the chances for optimal wound healing.
Keywords
Introduction
Exposed prosthetic grafts are a challenge to vascular specialists. 1 Exposed grafts lead to infections and may threaten patency as well. Groin dissections in vascular surgery can lead to local tissue breakdown, especially in patients who have multiple comorbidities and are nutritionally depleted. 1 Other local factors such as lymphocele and surgical site infections may contribute to graft exposure. Elimination of infection, preservation of distal limb perfusion and achieving an early robust soft tissue cover are the main objectives of treatment. Based on nearby vessels, pedicle-based flaps can be raised with different tissue components to obtain soft-tissue cover. Myocutaneous flaps are a good choice in management to address the above concerns. In this report, we describe a patient with exposed prosthetic bypass conduit in bilateral groin regions which were covered with bilateral rectus femoris myocutaneous flaps.
Case presentation
A 75-year-old Sri Lankan male with diabetes, hypertension and Parkinson’s disease presented with a bilateral non-healing wound and rest pain for 3 months. His bilateral lower limb pulses were absent from femoral downwards with an ankle brachial pressure index of 0.5. His evaluation of vascular disease showed bilateral aortoiliac disease (Figure 1). His BMI was 18 kg/m2 with low albumin level (2.1 g/dL). Since his premorbid status precluded the aortic cross-clamping and aorto-bifemoral graft, a decision was made to perform a right axillo-bifemoral bypass with a prosthetic graft. Re-operation was required for graft thrombectomy on the same day of surgery. His post-operative period was complicated by lymph leak and surgical site infection of bilateral groin wounds, which ultimately led to exposed prosthetic grafts (Figure 2). The swab culture isolated methicillin-resistant Staphylococcus aureus and the infection was treated with intravenous vancomycin for 14 days. Fortunately, the graft was functional and he noticed significant improvement in rest pain. He was then referred to the plastic surgical unit to manage the exposed prosthetic graft. Surgical site infection was initially managed with antibiotics, and local dressings and his comorbidities including malnutrition were optimized. Lower limb computed tomography angiogram showed well-perfused bilateral rectus femoris pedicles which were suitable for flap harvest. He underwent bilateral rectus femoris myocutaneous flaps to cover the soft-tissue defect over the exposed prosthetic grafts (Figure 3). The overlying skin only had multiple minor perforators which were not suitable to raise a facio-cutaneous flap. Therefore, muscle flaps were chosen as they were more resilient to breakdown and can address lymphorrhea as well. Bilateral flaps were raised based on the vascular pedicle supplying the rectus femoris muscle. Myocutaneous flaps were tunnelled under the upper thigh skin to reach the exposed prosthetic grafts without tension (Figure 4). Drains were inserted bilaterally.
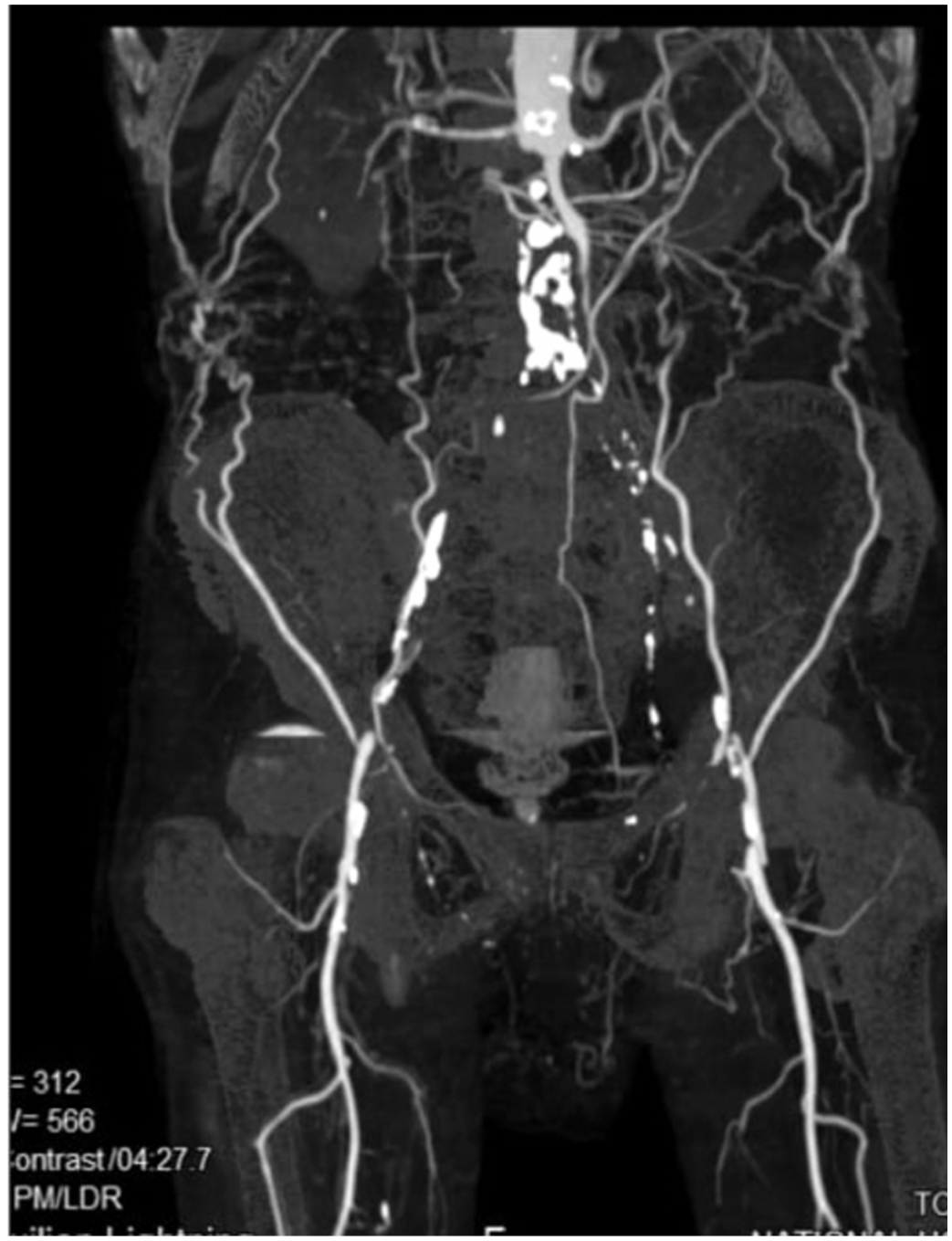
CT angiogram showing extensive aorto-iliac disease.

Image showing the exposed prosthetic grafts.

Image showing marking of the flaps (a) and dissection of the myocutaenous flap (b and c).

Image showing the final appearance after graft positioning and closure.
His initial post-operative period was unremarkable except for a small area of skin breakdown that was managed with dressings to achieve secondary healing. The output of drains used in bilateral groins gradually reduced and was removed after 10 days. After 3 months of follow-up, the patient was symptom-free with a patent prosthetic graft.
Discussion
Exposed prosthetic implants cause significant morbidity with resistant infections and graft dysfunction. Anatomically, the superficial nature of the groin vessels renders the surrounding soft tissue vulnerable to surgically related complications. In the reported patient, several factors have contributed to the soft-tissue breakdown. It is likely that comorbidities such as diabetes, hyperlipidaemia and malnutrition had contributed to poor wound healing. Local factors such as re-operation, surgical site infection, lymph leak and local vascular compromise may have also contributed to the soft-tissue breakdown. Exposed bilateral groin prosthetic grafts are extremely rare, and one case has been reported in the literature where the exposure occurred on different occasions. 1 We report a rare occurrence of simultaneous exposure of bilateral prosthetic grafts in the groin region.
Various techniques have been utilized to achieve soft-tissue cover over exposed grafts. The use of negative-pressure wound therapy can be considered as a temporary cover to preserve graft function until a definitive soft-tissue cover is achieved.2,3 Negative-pressure wound therapy was not used as it was costly in our setting and was not affordable to the patient. Considering the factors of soft-tissue cover, myocutaneous flaps are more resilient towards infections and ischaemia than facio-cutaneous flaps due to better blood supply. 4 Furthermore, muscle flaps are used for the treatment of lymph leak with a success rate of more than 95%. 5 More importantly, the potential compromisation of facio-cutaneous flap blood supply due to dissection of femoral vessels precluded its utilization.
Previous reports have described the use of vertical rectus abdominis muscle flap for unilateral groin and supra pubic graft cover. However, the option was less feasible due to the requirement of bilateral cover. 6 Furthermore, the donor site morbidity due to the anterior abdominal wall defect may be considerable. 7 Some studies have shown utilization of obturator bypass for revascularization of lower limb in exposed infected prosthetic grafts in the groin with compromised flow. 8 However, in the reported patient, such a strategy was not utilized since the bypass was patent and the infection was localized to the surgical site. Performing a bypass using materials resistant to infections, such as autologous, biosynthetic and prosthetic grafts impregnated with antimicrobial agents, is recommended. However, due to the economic crisis in our country and very limited resources, a cheaper alternative material was used due to non-availability of resilient prosthetic grafts.
Pre-operative angiogram showed a good blood flow in the profunda femoris vessels and therefore, the regional myocutaneous flaps seemed feasible. Computed tomography angiogram was useful in delineating the vascular anatomy as well as assessing the patency of the vascular pedicles in patients with peripheral vascular diseases. 9 Rectus femoris flap was considered over the gracillis flap because of the ease of dissection and patient positioning during surgery. 10 Moreover, primary closure of the donor site was feasible as a minimal cutaneous cover was needed to close the wound. 11 Functional loss of quadriceps strength is also reported to be similar to matched controls. 12 In our patient, the excess muscle parts were used to cover the graft beyond the cutaneous coverage to prevent graft exposure. Post-operatively, native skin breakdown was noted but the graft was not exposed due to the coverage by the muscle flap. Initial swelling of the area due to lymphatic leak was resolved within 2 weeks and likely due to new lymphatic channel formation.
Conclusion
The exposed vascular prosthetic graft is a significant morbidity for the patient while posing a significant challenge to the treating surgeon. Comorbidities and local factors should be optimized prior to definitive reconstruction to maximize the chances for optimal wound healing. Myocutaneous flaps are preferable as they are more resilient to breakdown compared to facio-cutaneous flaps, especially in a patient with compromised blood supply. The type of loco-regional flap should be carefully selected in an individualized manner depending on the regional vascularity. Rectus femoris flaps are a suitable option in terms of ease of surgical technique and durability.
Footnotes
Author contributions
OB, UJ, and DD contributed to the collection of information and writing of the manuscript. DD contributed to writing and final approval of the manuscript. All authors read and approved the final version of the manuscript.
Availability of data and material
All data generated or analyzed during this study are included in this published article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient for anonymised information and accompanying images to be published in this article. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
