Abstract
Acquired long QT syndrome caused by hypopituitarism and transient ST-segment elevation has not been reported in cardiac arrest patients. We report a case of extremely dangerous acquired long QT syndrome and transient ST-segment elevation. A 44-year-old Chinese woman with renal failure experienced sudden cardiac arrest in the haemodialysis room. Subsequent electrocardiogram showed QT prolongation and transient ST-segment elevation. This patient’s medical history, subsequent laboratory results and pituitary magnetic resonance imaging suggested hypopituitarism. Transient ST-segment elevation on the electrocardiogram was considered to be caused by repeated direct current shocks. The patient was diagnosed with acquired long QT syndrome and was not taking any antiarrhythmic drugs. Her corrected QT interval normalized after hormone replacement therapy. This case highlights the importance of the awareness of hypopituitarism; early identification and intervention can prevent the occurrence of this life-threatening arrhythmia. ST-segment elevation is not always due to acute myocardial infarction, and a variety of other causes, especially electrical cardioversion, should be considered.
Introduction
Among the various manifestations of hypopituitarism, fatal ventricular arrhythmias are very rare. Hypopituitarism is associated with changes in the electrocardiogram (ECG), including giant T-wave inversion, QT prolongation and ST-segment changes.1,2 ST-segment elevation after cardioversion is an easily overlooked phenomenon that occurs rapidly and resolves within the first few minutes after shock. 3 We report a case of extremely dangerous acquired long QT syndrome (LQTS) and transient ST-segment elevation.
Case presentation
A 44-year-old Chinese woman with renal failure experienced sudden cardiac arrest in the haemodialysis room. ECG monitoring showed ventricular fibrillation. The sinus rhythm of the patient was restored after receiving a single-phase direct current (DC) shock of 360 joules. ECG monitoring immediately after defibrillation showed sinus tachycardia with a prolonged QT interval (QTc) and a large T-wave inversion in leads I, AVL and V1–V6 (Figure 1). The patient’s further course of illness was turbulent, and recurrent episodes of haemodynamically unstable ventricular tachycardia required cardioversion (Figure 2). Subsequent ECG showed transient ST-segment elevation in leads I, AVL and V1–V6 (Figure 3). Her family did not have any history of heart disease or sudden cardiac death. Twenty years prior, the patient was diagnosed with a pituitary tumour and received partial radiation therapy. She was followed up for 2 years after radiation therapy, but because she was unlikely to experience recrudescence, she stopped attending follow-up visits. The patient’s laboratory results (Table 1) indicated neglected panhypopituitarism. Pituitary magnetic resonance imaging (MRI) showed that the pituitary gland had almost disappeared and was filled with cerebrospinal fluid (Figure 4). The patient did not take antiarrhythmic drugs, and with hormone replacement therapy, her condition gradually stabilized, the ejection fraction (EF) increased from 45% to 55%, and the corrected QTc returned to normal (Figure 5). Transient ST-segment elevation shown on the ECG was considered to be caused by repeated DC shocks. Coronary angiography was performed 5 days later and showed mild-to-moderate stenosis of the vessel, which also confirmed our hypothesis.

ECG immediately after defibrillation showed sinus tachycardia with a prolonged QT interval and a giant T-wave inversion in leads V1–V6, I and AVL.
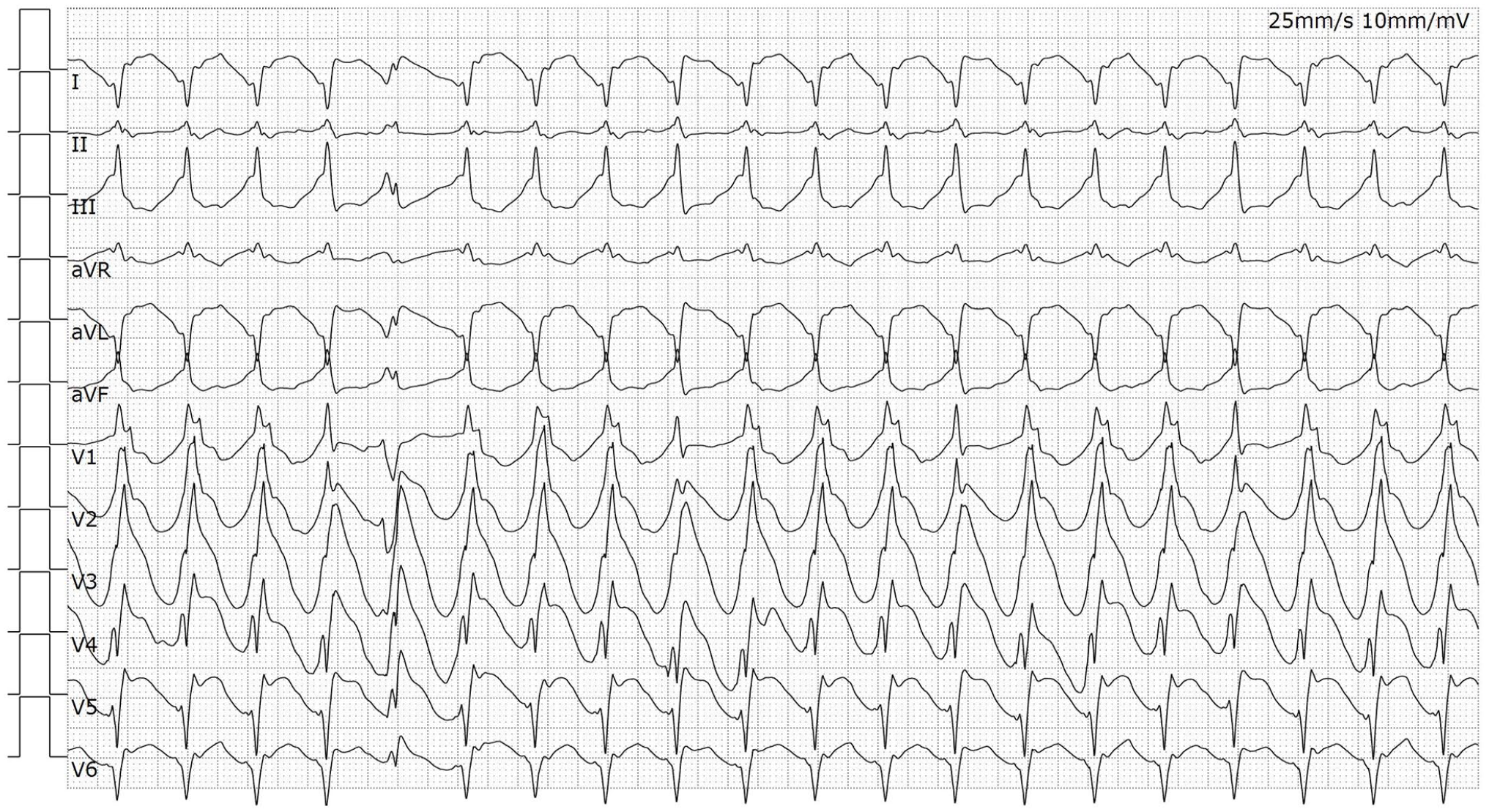
ECG after 2 h showed ventricular tachycardia.

ECG after 2.5 h showed marked ST-segment elevation in leads V1–V6, I and AVL.
Laboratory findings.

T3: triiodothyronine; T4: thyroxine; TSH: thyroid-stimulating hormone; FSH: follicle stimulating hormone; LH: luteinizing hormone.

Pituitary MRI and the red arrow show that the pituitary gland was replaced by cerebrospinal fluid.

ECG after 1 month showed that corrected QT interval had returned to normal.
Discussion
To our knowledge, LQTS caused by hypopituitarism and transient ST-segment elevation has not been reported in cardiac arrest patients. Importantly, in this case, severe electrolyte disturbances and drugs, which are commonly associated with acquired LQTS, were not present.4,5 Hypopituitarism should be considered an unusual cause of reversible LQTS.
In 1914, the German physician Maurice Symonds first discovered a decrease in pituitary function. 6 Since then, knowledge about the management and pathophysiology of this disease has greatly increased. However, a lack of understanding of the disease and the atypical clinical manifestations often delay the diagnosis and treatment time and sometimes even lead to extremely serious consequences, as shown in this case. Hypopituitarism is known to be associated with various nonspecific ECG abnormalities, such as severe T-wave inversion, ST-segment depression and QTc prolongation.7,8 Decreased ACTH levels have been considered to be a possible cause of ECG changes in hypopituitarism. 9 Severe hypothyroidism can lead to worsening of myocardial contractions, decreased heart rate and slow conduction in cardiac tissue. In addition to thyroxine, steroid hormones are also associated with ventricular tachycardia. 10 Glucocorticoids could upregulate Kv1.5 channel gene expression in rat ventricles. 11 Sex hormones may play a potential role in modulating arrhythmia risk in LQTS, and adult females with congenital 1 and 2 LQTS have been reported to be at high risk of sudden cardiac death and polymorphic ventricular tachycardia. 12
This cardiac arrest patient had transient ST-segment elevation shown on the ECG. Should coronary angiography have been performed immediately? We considered the transient ST-segment elevation to be caused by repeated DC shocks rather than myocardial ischaemia, so we did not immediately perform coronary angiography. The reasons are as follows: (1) Subsequent ECG showed that the ST-segment had completely subsided and that there was no pathological Q wave. (2) The troponin I level peaked at 5.51 ng/mL, and the elevated level could not explain widespread anterior myocardial infarction. (3) Cardiac ultrasound showed decreased left ventricular EF but no significant segmental abnormality. (4) The patient had a longer QTc, and myocardial ischaemia was unlikely to be the primary cause of QT prolongation. Subsequent coronary angiography also confirmed our hypothesis. ST-segment elevation after DC selective cardioversion is a short transient-state phenomenon; the DC impact is large, the average duration is 1 min, and it usually resolves within 5 min after the shock. 13 However, in our case, the ST-segment elevation time was longer than 5 min, which may have been related to repeated electric shocks and the use of propofol. 13
Conclusion
This case highlights the importance of awareness of hypopituitarism; early identification and intervention can prevent the occurrence of this life-threatening arrhythmia. ST-segment elevation is not always due to acute myocardial infarction, and a variety of other causes, especially cardioversion with DC, should be considered.
Footnotes
Author contributions
All authors contributed to investigating, writing, reviewing and editing.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This research was funded by the Wenzhou Administration of Science and Technology (Y2020102).
Ethics approval
Ethical approval to report this case was obtained from the ethics committee of Wenzhou People’s Hospital (2021.69).
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
