Abstract
The purpose of this article is to present a case demonstrating the treatment of epulis fissuratum due to a poorly adapted prosthesis using a single surgical procedure involving conventional excision and free gingival graft. We, herein, present a case involving a 58-year-old patient with epulis fissuratum. Treatment of this case was essential due to the masticatory problems. This technique can be effective to deepen the height of the residual alveolar ridge and to increase the amount of keratinized tissue.
Introduction
Epulis fissuratum (EF) is an inflammatory pseudo-tumor characterized by fibrous connective tissue hyperplasia in the gingivobuccal region. It is most often caused by persistant irritation, especially by poorly adapted dentures. 1 However, its excision reduces the vestibule depth, thus compromising the stability of the denture. 2 In such cases, excision of the epulis with vestibuloplasty in combination with gingival graft is the preferred treatment. Actually, this surgical procedure is mainly performed to optimize the jaws for prosthetic integration and to increase the height of the vestibular sulcus. This procedure is also carried out to improve the quality of the soft tissue. 3
Case report
A 58-year-old male patient with no particular pathological history presented to the department of Oral Medicine and Oral Surgery at the University dental clinic of Monastir, Tunisia, for the removal of fibrous hyperplasia in the mandibular vestibule resulting from ill-fitting prostheses, suggestive of epulis fissuratum and vestibular deepening.
He had been wearing the current badly-adapted set of dentures for the last 4 years. Extra-oral examination showed a reduction in the vertical dimension of occlusion.
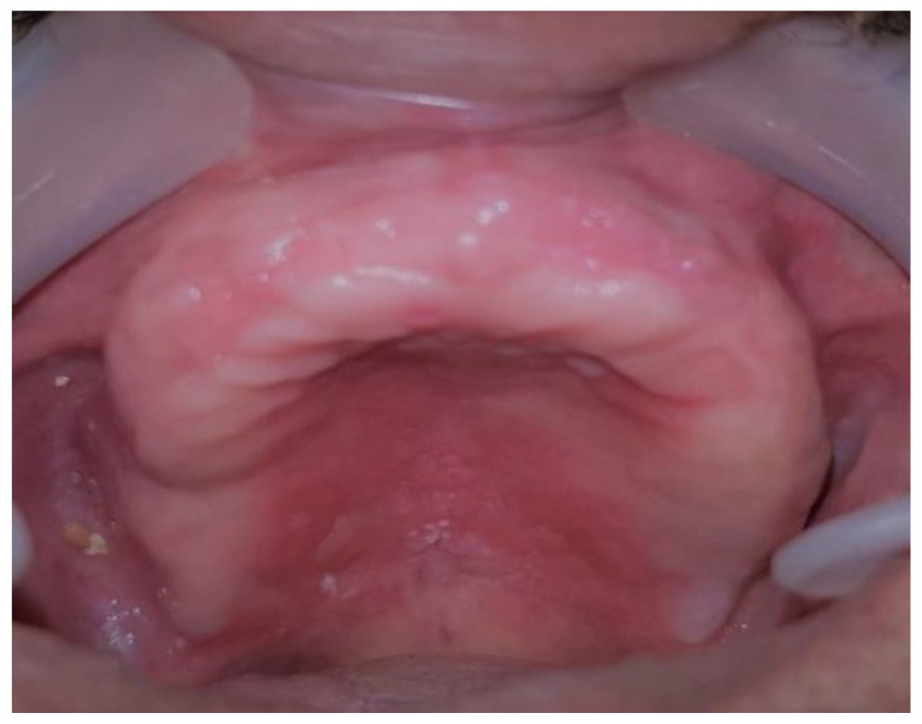
Intra-oral examination revealed hyperplastic mandibular lesion of the anterior alveolar mucosa, extending to the vestibular sulcus. This lesion was covered with non-inflammatory mucosa. On palpation, the lesion was firm in texture and non-hemorrhagic. The alveolar ridge was highly resorbed at the mandibular level, with insufficient keratinized mucosa (Figure 1). On the palate, examination revealed the presence of erythema contrasting with the normal pallor of the mucous, delimited by the level of the posterior edge of the maxillary prosthesis (Figure 2). This lesion was suggestive of prosthetic candidiasis. As the total removable prosthesis was badly adapted and the lesion was neither ulcerated nor indurated, no other differential diagnosis was made.

Hyperplastic tissue folds in the mandibular buccal.
Palatal erythema.
Diagnosis of denture-induced hyperplasia was made. Topical mouthwashes with Fungizone (4 times per day) and chlorhexidine (0.12%, 4 times per day) were therefore prescribed. Then, follow-up sessions for prosthetic candidiasis were carried out to evaluate the decrease or disappearance of clinical signs, including the sensation of burns and the regression or not of the palatine erythema. After 3 weeks of the first consultation, complete resolution of erythema and absence of symptomatology were noted. Surgical resection combined with gingival graft was therefore planned. Local anesthesia (mepivacaine 2% with adrenaline 1: 80 000) was administered. A partial thickness incision using a scalpel holder and blade n◦15 (euromedis) was performed. The incision followed the limits of the fibrous hyperplasia which was excised over a width of approximately 10–12 mm, going from the 2nd right mandibular premolar to the contralateral side (Figure 3), exposing the underlying connective tissue (Figure 4).

Excision of the epulis.

Exposure of the underlying connective tissue.
The lower boundary of the incision was sutured in its new position with interrupted periosteal sutures, first at the midline, then at other locations along the incision, using Vicryl 3-0 non-resorbable suture (Figure 5).

Interrupted periosteal sutures.
Free gingival graft was carried out from the palate, and it was dissected in partial thickness in order to preserve a layer of connective tissue on the bone surface of the donor site. The graft consisted of an epithelium and a thin layer of underlying connective tissue.
Then, the graft was immobilized with sutures using simple stitches (at each upper corner). Later, vertical mattress sutures with periosteal anchorage were performed to ensure the graft immobilization in case of lip traction at the lateral borders and at the underlying periosteum (Figure 6).

Immediate aspect of the treated area.
The specimen was fixed and sent for anatomopathological examination, which confirmed the clinical diagnosis of epulis fissuratum.
No periodontal dressing was put in place. The patient was asked to have a soft diet, limited facial movement for 14 days, no brushing around the surgical site for 3 days after the procedure, and to place an ice pack on the lower lip. Chlorhexidine mouth rinse (0.2%) was prescribed twice a day for 2 weeks. Antibiotics and non-steroidal anti-inflammatory drugs were administered for 5 days. The patient’s prosthesis was relined using a tissue conditioning material “Fit de kerr” (Figure 7).

Relining of the prosthesis with the “fit de kerr”
Favorable postoperative healing was observed 2 weeks later during the removal of sutures. However, the patient reported discomfort, especially at the donor site. Two months later, the final total prosthesis was delivered to the patient. Perfect integration of the prosthetic volume, and the resulting retention and stability were observed (Figures 8 and 9). Vestibuloplasty resulted in a well-extended, stable, and retentive total mandibular prosthesis.

A well-–extended and retentive new prosthesis.

Two months post-operative surgical site.
Discussion
Epulis fissuratum, also called inflammatory fibrous hyperplasia, is a reactive tissue alteration in response to poorly adapted dentures on the vestibular oral mucosa. 4 The lesion is mainly caused by persistent trauma and irritation. 1 However, ill-fitting dentures, poor oral hygiene, wearing dentures all the time, smoking, age-related changes, and systemic conditions are also considered as factors responsible for the occurrence of epulis. 5 It more frequently occurs in the edentulous maxilla, which is not the case for our patient. 6 The lesion may appear in different dimensions. It can range from a few millimeters to several centimeters, thus involving the entire vestibule. 7 It is generally asymptomatic but it is sometimes accompanied by the occurrence of severe inflammation and ulceration. Clinically, it has a variety of features. It is usually presented as a soft and smooth lesion in the vestibular sulcus with normal or erythematous overlying mucosa next to the edges of the prosthesis. 8
Alveolar bone atrophy is a consequence of this permanent irritation. This can lead to alterations in the anatomic characteristics and dimensions of the jaws. 9 The relationship between the width of the keratinized mucosa and the degree of bone atrophy is confirmed. In fact, the mucogingival junction shifts in the coronary direction, thus reducing the width of the keratinized mucosa. 10 This is typically associated with a shallow vestibule. Besides, due to the ridge resorption, muscle attachments become more prominent and closer to the seat of the total prosthesis, which may compromise the stability of the prosthetic bases.
As a consequence of the lesion removal, an atrophy of the alveolar bone may occur. Moreover, primary closure tends to roll the lip inward, thus decreasing the vestibular depth in many instances. Retention and stability of the denture could therefore be compromised, which is the case of our patient. 11
Many techniques have been used successfully for the excision of epulis fissuratum. These techniques can be classified into two types: conservative and surgical. 12 The conservative approach is non-invasive. For this reason, it is considered as the treatment of choice. However, it is time-consuming. It requires relining of the prosthetic bases using tissue conditioning material. Conventional scalpel, electro-cauterization, soft tissue lasers, and liquid nitrogen cryosurgery can be used in the surgical approach. Electro-cauterization is used because it ensures hemorrhage control and post-operative healing. 13 CO2 laser, Er: YAG laser, Nd: YAG laser, diode laser, argon laser, and potassium-titanylphosphate- lasers are some of the lasers used in dentistry for the same purpose. Carbon dioxide laser is considered as one of the most promising techniques for soft tissue surgery. The use of carbon dioxide laser (CO2) in the treatment of those lesions has many advantages compared to conventional surgery, including good hemostasis, minimal surgical aftercare, and good patients’ satisfaction. 14 Recently, liquid nitrogen cryosurgery has become promising in minimally invasive dentistry. It assures excellent hemostasis with minimal post-operative edema and pain. 12 When reapproximation of the remaining tissue is performed, loss of vestibular depth and insufficiency of the keratinized mucosa will be noted.
In these cases, the use of vestibuloplasty combined with the excision of the epulis is the treatment of choice to optimize prosthetic integration by increasing the residual alveolar ridge height and generating a sufficient band of keratinized mucosa. Vestibuloplasty expands the denture-bearing area, thus reducing the denture load per square unit of the supporting bone and the bone resorption caused by the transfer of occlusal forces. 15
Several other methods have been described for vestibuloplasty. They are classified into submucosal vestibuloplasty, secondary epithelization, and grafting vestibuloplasty. 16
The availability of sufficient alveolar bone and free mobile mucosa is necessary for the success of submucosal vestibuloplasty since it ensures deepening without tension. Submucosal vestibuloplasty is not indicated in the presence of a defect in the quantity or quality of the mucosa. 16 Secondary epithelization is therefore preferred. Grafting vestibuloplasty has the advantage of covering the periosteal surface and accelerating healing while maintaining the sulcous depth. 17 Vestibuloplasty combined with a graft material is considered the therapy of choice to obtain a keratinized tissue size and a sufficient vestibular depth. Numerous graft materials are available, including skin graft, mucosal grafts, allogenic collagen membrane, and placental graft. However, they all have their own limits. Autogenous tissue (free gingival graft, subepithelial connective tissue graft) is currently the gold standard for augmenting the amount of keratinized mucosa. 18
The amount of keratinized mucosa could significantly be increased when combining the conventional surgery with autogenous tissue compared to other alternatives. 19 The use of collagen matrices does not require second wound in the palatal area and it reduces the surgery time. However, gain of keratinized mucosa is not guaranteed compared to the use free gingival graft. 20
Conclusion
Chronic irritation, ill-fitting prostheses, and tobacco use greatly increase the prevalence mucosal lesions, notably epulis fissuratum. Surgical excision as the definitive treatment may lead to shallow vestibule and insufficient keratinized mucosa. Vestibuloplasty combined with free gingival graft as a complementary treatment is therefore required. It is the best alternative to prevent loss of sulcus depth or keratinized mucosa.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patient for his anonymized information to be published in this article.
