Abstract
A 63-year-old male receiving hemodialysis for renal insufficiency developed severe and widespread pruritus, which was unresponsive to antihistamines and severe depression with insomnia, agitation, and anxiety. The oral administration of 7.5 mg mirtazapine daily alleviated his severe pruritus after 4 days and severe depression after 14 days. Mirtazapine has potential as a therapeutic option for patients receiving hemodialysis with depressive disorder and severe pruritus unresponsive to antihistamines.
Introduction
Chronic pruritus is a common and unpleasant sensation that affects the quality of life of patients due to disturbances in mood, sleep, and social relationships. 1 It may be associated with dermatosis, hepatic diseases, renal failure, and malignancies. 1 A large number of patients receiving chronic hemodialysis for end-stage renal disease develop pruritus. 2 Therapies recommended for pruritus include topical corticosteroids, systemic antihistamines, phototherapy, gabapentinoids, ondansetron, and nalfurafine; 3 however, they have limited efficacy for hemodialysis patients with severe and persistent pruritus. 4 The antidepressant mirtazapine was reported to be an effective treatment for pruritus in patients with malignant cholestasis, lymphoma, and uremia. 5 Recent studies demonstrated that mirtazapine effectively attenuated pruritus in patients receiving hemodialysis;6,7 however, it currently remains unclear whether mirtazapine exerts differential effects on depression and pruritus in patients receiving hemodialysis.
Therefore, to clarify whether mirtazapine exerts differential effects on depression and pruritus, we prescribed mirtazapine for a dialysis patient with depressive disorder and severe pruritus unresponsive to antihistamines and other medications.
Case report
A 63-year-old male receiving hemodialysis for more than 20 years for renal insufficiency developed severe and widespread pruritus and a rash that covered the surfaces of both the lower limbs (Figure 1). The rash had appeared on the proximal parts of both limbs approximately 4 months previously and gradually spread to the distal parts. From 3 months or longer before, the patient reported depression characterized by depressed mood, anxiety, inability to concentrate, difficulties with attention, initial and intermediated insomnia, and restlessness associated with irritability. He met the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criteria for a major depressive episode. 8 Physical examination ruled out contributing causes of pruritus and computed tomography head scans were normal. Furthermore, his creatinine, urea nitrogen, complete blood count, hemoglobin, C-reactive protein, and serum IgE level were normal. The patient had no other medical problem and was not taking any kind of drugs.
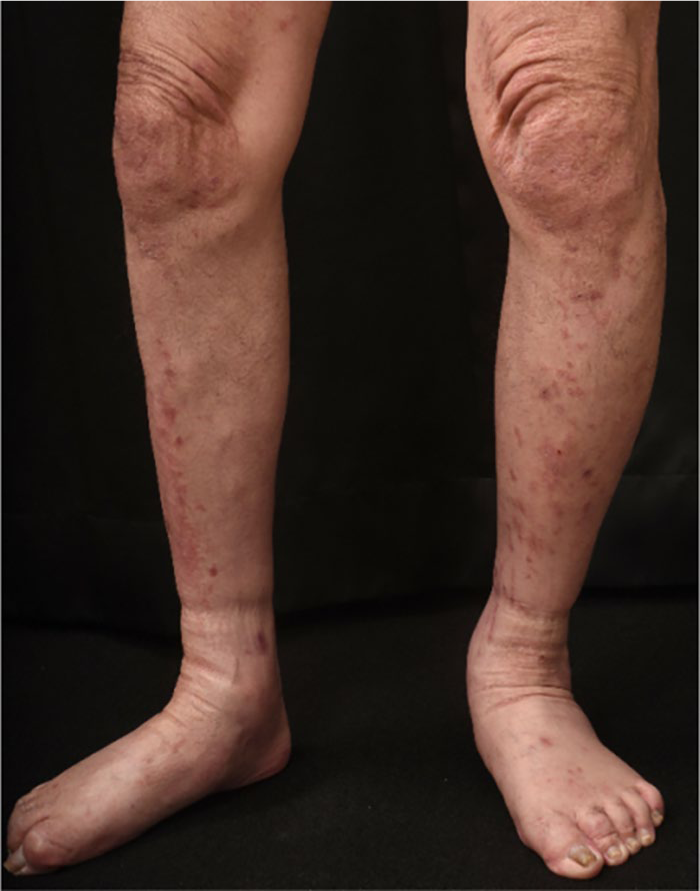
A rash on both lower limbs of the patient receiving hemodialysis.
The daily administration of white petroleum, a skin emollient, and antihistamines, including 20 mg of bilanoa, 10 mg of ebastine, and 30 mg of diphenhydramine, for 6 weeks did not attenuate his symptoms.
After the treatment including antihistamines, he was prescribed half of a 15 mg tablet of mirtazapine orally, the standard dosage of mirtazapine, once daily to minimize adverse events. The response of pruritus to the oral administration of mirtazapine was assessed using a simple visual analog scale (VAS). 9 VAS was evaluated 0, 4, 7, 10, and 14 days after the initiation of mirtazapine. The VAS score before the administration of mirtazapine was 80, indicating severe pruritus (Figure 2(a), baseline). Within 4 days, the VAS score markedly decreased to less than half than that before the administration of mirtazapine and remained stable for 14 days (Figure 2(a)).

Effect of mirtazapine on pruritus and depression in a patient receiving hemodialysis. (a) Time-dependent changes in pruritus evaluated by VAS after the administration of mirtazapine. (b) Time-dependent changes in depression evaluated by HDRS-17 after the administration of mirtazapine.
The depressive state was assessed using the 17-item Hamilton Depression Rating Scale (HDRS-17), 10 in which a total score of “0–7” represents the normal range and “above 23” represents the greatest severity of depression. The total HDRS-17 score before the administration of mirtazapine was 25, indicating very severe depression with insomnia, agitation, and anxiety (Figure 2(b), baseline). The HDRS-17 score was measured on the same day after the VAS score had been assessed and in the subsequent days. The results obtained showed that the HDRS-17 score gradually decreased after the initiation of mirtazapine and reached a minimum on day 14 (Figure 2(b)). The administration of mirtazapine for 6 months resulted in the sustained and significant attenuation of pruritus and depression. The patient transferred to another hospital after 6 months of mirtazapine treatment.
Discussion
Previous studies reported the efficacy of mirtazapine for the treatment of pruritus in patients with cancer, cholestasis, and renal failure.1,5 In this study, mirtazapine alleviated uremic pruritus in a patient receiving hemodialysis, which is consistent with previous findings.6,7 Therefore, mirtazapine has potential as a novel treatment for pruritus in hemodialysis patients.
Previous case reports showed that mirtazapine at a daily dose of 15 mg or more exerted beneficial effects on the pruritus associated with atopic skin disease and other conditions5,11 and also on pruritus in patients receiving hemodialysis.6,7 This case was treated with mirtazapine at a dose of 7.5 mg per day, which attenuated pruritus after 4 days. Therefore, 7.5 mg of mirtazapine daily may be a sufficient dose to exert antipruritic effects in patients with uremic pruritus.
Mirtazapine has been shown to have antidepressant and antipruritic effects in patients with chronic pruritus; however, the relationship between the onsets of antidepressant and antipruritic effects has not been examined in detail. In our patient, the treatment with mirtazapine exerted antipruritic effects before the amelioration of depressive symptoms, indicating that the onset of antipruritic effects after the treatment with mirtazapine was faster than that of antidepressant effects. Hence, attenuation of pruritus by antidepressants may ameliorate the depressive state because pruritus generally induces a depressive state. Alternatively, chronic pruritus may induce the neuronal plasticity in the brain resulting in severe depression. Rogóz et al. 12 and Harmer et al. 13 reported that neuronal plasticity returned to normal by the repeated administration of antidepressants, although the underlying mechanisms remain unresolved. Thus, the neuronal changes in the brain derived from chronic pruritus and depression appear to be normalized at differential onset times after the repeated administration of mirtazapine.
Conclusion
A patient with severe pruritus and depression receiving hemodialysis was successfully treated with mirtazapine, indicating its potential as a therapeutic option for hemodialysis patients with depressive disorder and severe pruritus unresponsive to antihistamines.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting the individual cases.
Informed consent
Written informed consent was obtained from the patient for their anonymized information to be published in this article.
