Abstract
Tumor seeding after intra-abdominal and head and neck cancer surgery is a well-known entity. The risk of disseminating cancerous cells during surgery is also described for soft-tissue sarcoma of the extremities. Nonetheless, after reconstructive surgery using flaps, the risk of recurrence at the donor site is extremely rare. Up to this date, the literature describes only three cases, but none of them reported a translocated recurrence after a reconstruction with a propeller flap. Here, we report a case of high-grade pleomorphic sarcoma of the knee, which recurred at the proximal edge of a propeller flap 28 months after the first excision surgery. The reasons for such local recurrences are not clear and previous works have advocated different theories: direct contamination by tumor cells, physical manipulation of the tumor and creation of surgical wounds with tumor supportive properties. Although these particular cases of recurrence are exceedingly rare, certain precautionary meticulous surgical techniques and a thorough preoperative planning are pivotal to avoid the contamination of “clean” areas during the first excision surgery.
Introduction
Sarcomas of the extremities are rare malignant tumors of mesodermal origin. Among soft-tissue sarcomas (STSs), they are characterized by a high local recurrence rate of 9%–22%. Tumor spillage into the operative field is one of the most important factors for local recurrence. For this reason, it is mandatory to plan the site of the first biopsy inside and the area that afterwards will be radically resected in case of histological evidence of STS. The final en bloc oncological resection needs to be conducted with appropriate margins (final margins > 1.0 cm or intact fascial plane) and minimal dissection of the surrounding healthy tissues. 1 The risk of local recurrence after either preoperative or post-operative adjuvant radiotherapy is increased when surgery is performed with positive margins.2,3 In effect, an optimal first surgical resection of STS is considered of primary importance for the prevention of local recurrences. 1 The literature reports cases of recurrences on surgical wounds that are far distant from the primary malignancy. These works have found no other connection or explanation but the intraoperative seeding of the tumor cells.4–6 This phenomenon is well described after intra-abdominal7–9 and head and neck cancer resection,6,10 but recurrences of STSs in the donor sites after a reconstructive procedure have been rarely reported. Only three cases have been reported so far,4,5 but no one describes the spreading of the disease after using a propeller flap technique. Literature found no differences in the wound complication rate and the oncologic outcomes among patients who underwent immediate or staged STS resection. 11
For lower limb reconstruction, muscular flaps (~58%), fasciocutaneous (~42%) and conventional fascial flaps (~1%) remain the workhorses in the plastic surgeon’s tool box. 12 Since their first description in 1991 by Hyakusoku et al., 13 pedicled perforator propeller flaps have been proposed and used with great enthusiasm in the last decade.
Subsequently refined by Teo 14 and classified in the consensus of Tokyo in 2011, 15 propeller flaps have become increasingly popular thanks to their advantages, such as “like-with-like” reconstruction using adjacent tissues and a low donor site morbidity.11,16–18
Here, we describe a case of STS recurrence in the donor site of a propeller flap probably due to surgical tumor seeding that occurred during the first resection.
Case report
In June 2015, a 43-year-old woman presented at another hospital with a swelling on the lateral side of the right knee, which clinically resembled a cyst of the lateral meniscus. A magnetic resonance imaging (MRI) scan revealed a cystic mass lying over the lateral meniscus, the femoral epiphysis and the tibial condyle. These findings seemed to be consistent with the clinical diagnosis of a cyst. For this reason, an arthroscopy was planned. A first attempt to decompress the cyst arthroscopically through a medial incision failed. The doctors then accessed the mass through a lateral incision and found that the formation had a solid consistency rather than fluid. Considering the macroscopic aspect of a malignant lesion, the tumor was enucleated and a drain was placed several centimeters below the lateral scar. The histopathologic examination demonstrated that the lesion was a high-grade pleomorphic sarcoma. In September 2015, the woman approached our tertiary referral center for musculoskeletal oncology, which boasts the presence of a multidisciplinary team. We planned the oncological re-excision on new computerized tomography (CT) scans to achieve wide healthy resection margins. 19 The oncology–orthopedic surgeon performed the surgical re-excision, while the plastic surgeon harvested an adipo-cutaneous propeller flap based on a peroneal artery perforator at the middle third of the same leg. In addition, we used a random local flap harvested from the popliteal region to cover part of the donor site (Figures 1–3).

A multidisciplinary approach was used to plan the demolition on computerized tomography (CT) images. The oncology–orthopedic surgeon, performed the surgical re-excision following the surgical marking and respecting wide margins ensuring the resection of the surgical field of the previous surgery.

In reconstructive time, an adipo-cutaneous propeller flap based on peroneal-perforator of the middle third of the right side and a local-random flap from the popliteal region were planned to cover the defect.

Immediate final result of reconstructive surgery. Using different types of loco-regional flaps, it was possible to perform an immediate and safe coverage allowing an early adjuvant radio- and chemotherapy.
The histopathologic examination demonstrated the complete resection of the tumor with more than 3 cm cuff of healthy tissue. The patient spent 1 year and 9 months without significant complications after adjuvant radio- and chemotherapy. The woman underwent a trimestral follow-up until she suffered from a tibial plateau fracture in June 2017. The injury was treated by open reduction and internal fixation (ORIF) through the incision of the medial margin of the propeller flap. We assisted to a delayed wound healing probably due to the previous radiotherapy. After 4 months, the patient noticed a painless swelling that gradually increased in size over her right external distal third of the leg; this spot corresponded to the original proximal edge of the propeller flap (Figure 4). Positron emission tomography (PET)–CT scan revealed a subcutaneous nodule, with no other relevant standardized uptake value (SUV) focuses. In the same month, we performed a wide local excision of the suspected recurrence and repaired the defect with a split-thickness skin graft (STSG). During the same procedure, we revised the proximal wound dehiscence and repaired it with a proximally based lateral gastrocnemius flap. We used STSG to cover the muscular flap (Figures 5 and 6). Histology confirmed the complete excision of the recurrent tumor within the soft tissue of the flap compatible with a recurrence from the previously excised sarcoma. We speculated that the cause of the recurrence was the implantation of tumor cells at the time of the first surgery in correspondence of the exit point of the drainage. This spot probably fell within an area not covered by a significant dose of radiations. Clinical examination and repeated MRI in November 2019 did not demonstrate any further evidence of the disease (Figure 7).

After 4 months, (white arrow) a painless swelling gradually increasing in size nodule appeared over her right external middle third of the leg into the original proximal part of propeller flap. At the same time, there was a delayed healing of the wound (white asterisks), radiotherapy related, in the previous access for ORIF.
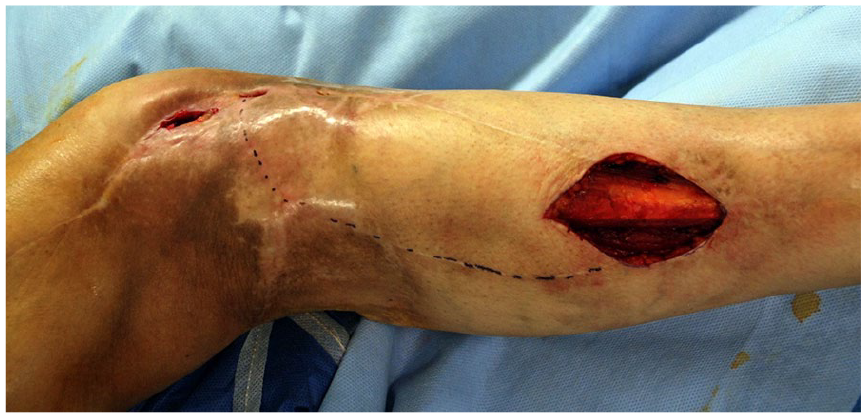
A wide local excision of the suspected translocated recurrence and revision of the wound of the knee was performed.

At the same time, a lateral gastrocnemial proximally based muscular flap was harvested for the revision of ORIF wound and a split-thickness skin graft was used to repair the loss of substance in the left part.
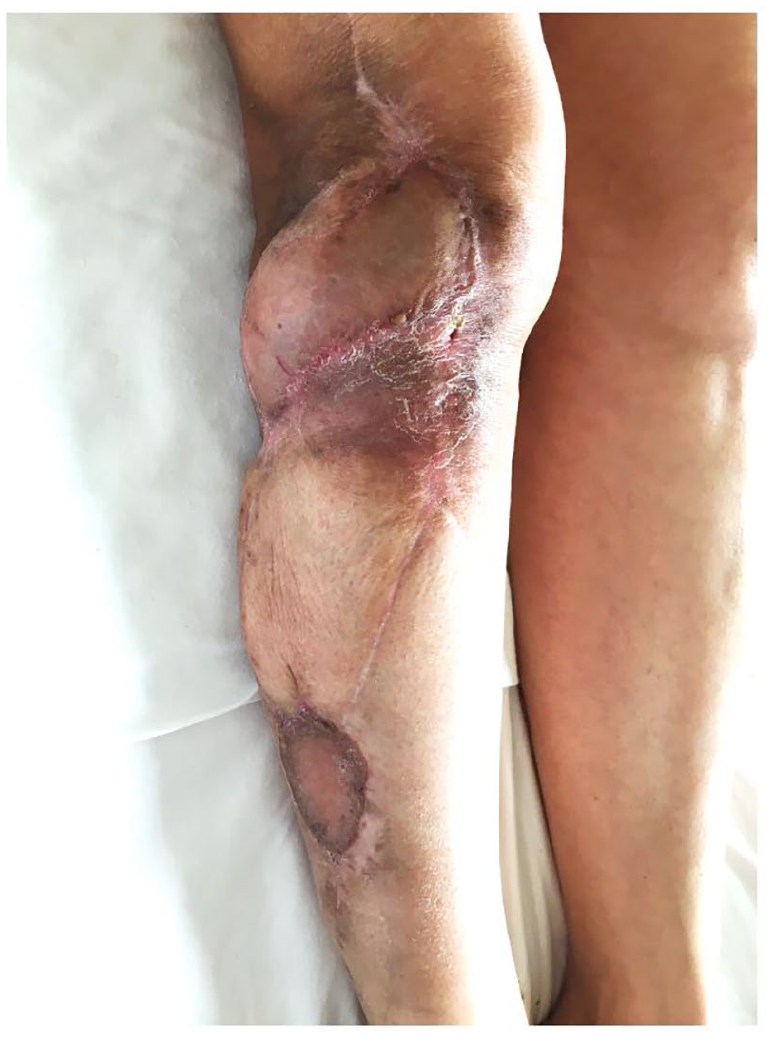
Follow-up: after 2 years and 5 months, no signs of local recurrence or distant localizations. A clinical follow-up every 6 months was planned due to a high risk of recurrence.
Discussion
Radical resection and limb salvage in sarcoma surgery are a challenge for reconstructive surgeons because of the lack of local tissue. 20 This anatomical feature combined with the frequent bone and joint exposure after the demolition surgery prompted majority of surgeons to consider free flaps as the first-line treatment.21,22
Propeller flaps base their vascularization on a solitary perforator of the deep fascia reaching the subcutaneous layers. In propeller-flap planning, a specific perforator needs to be identified as the basis of the flap.23,24 This allows the restoration of an “
In the literature, we found only three similar case reports. Hughes et al. in 2000 reported two patients with sarcoma metastasis due to iatrogenic tumor implantation. One was a low-grade fibromyxoid sarcoma of the knee that recurred in an arthroscopic port site; the other was an intermediate spindle cell sarcoma of the thigh that recurred at the contralateral unaffected limb, from which a vein had been harvested for vascular repair. 4 In 2017, Parija 5 reported a case of a low-grade sarcoma of unknown differentiation with metaplastic ossification of the foot, which recurred at the flap donor site (located at the calf level) 14 months after surgery. The reasons of tumor recurrence in surgical wounds remote from the primary operative field are yet to be clarified. Two theories have been proposed so far: (1) tumor occurring due to direct transplantation of tumor cells through surgical instruments and gloves, (2) chemokines and cytokines (Platelet-Derived Growth Factor (PDGF) and Epidermal Growth Factor (EGF)) may act as wound-homing-delivery free tumor cells after tumor excision.29,30 Despite their rarity, these local dislocated recurrences have an important prognostic significance. Adjuvant radiotherapy after complete limb sparing STS resection provides a fundamental benefit on preventing local recurrences. In our case, the post-operative radiation therapy did not prevent the recurrence of the disease at the original proximal margin of the propeller flap. The insetting of the propeller flap could have rotated 180° of the distal excision margin where the disease eventually recurred. As suggested by Cha et al., 31 a multidisciplinary approach in planning oncologic resection and method of reconstruction to inform the radiation oncologist for an increase in target volume radiotherapy after propeller flap reconstruction to include proximal margin of the flap that was the nearest to sarcoma side.
Conclusion
Propeller perforator flaps are a useful reconstructive option in sarcoma reconstruction surgery.
The oncological literature reports several recommendations to prevent iatrogenic tumor cell dissemination. We report a very rare case of STS recurrence dislocated in a distal margin of a propeller flap, which once corresponded to the boundary of the tumor dissection. The reasons of this recurrence are unknown, but we speculate that tumor cells were disseminated through the exit point of the drainage during the first ablative surgery. We believe in this hypothesis because the exit point was located far away from the resection margins but it was near the edge that was eventually involved by the recurrence. Another explanation could be a non-radical primary excision. We rejected this hypothesis because of the macro and microscopic evidence of residual disease on the resection margins. This report reinforces the need for meticulous preoperative planning and surgical technique to prevent contamination of “clean” areas that might not be included in adjuvant radiotherapy fields. In addition, it might be worth to radiate the new distal margin of the propeller flap in case of immediate reconstruction. The case also highlights the pivotal importance of a correct initial management of these uncommon tumors.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
