Abstract
Microcystic adnexal carcinoma is a rare cutaneous neoplasm believed to arise from pluripotent keratinocytes capable of adnexal differentiation. Due to its insidious growth and appearance, diagnosis is often delayed. A deep incisional or excisional biopsy for histopathology is the gold standard for diagnosis. Different treatment modalities have been described in the literature, including the Mohs micrographic surgery, standard excision, radiation, chemotherapy, and observation. Currently, Mohs remains the treatment of choice. We present a unique case of a 12-month history of an extensive progressive centrofacial cutaneous induration diagnosed as microcystic adnexal carcinoma in an 83-year-old female. Due to the extensive nature of the tumor, she received radiation therapy and continues to receive ongoing assessment with no evidence of clinical recurrence at 2-year post-treatment including negative scouting biopsies. To date, there is no consensus on the optimal treatment for microcystic adnexal carcinoma.
Introduction
Microcystic adnexal carcinoma (MAC) is a rare cutaneous neoplasm that most commonly presents on the face.1–26 It is characterized as a malignant, aggressive, and locally invasive tumor with a high recurrence rate.2–4,8,9,11–17,19 MAC typically does not metastasize; however, there are reports of local and distant progression of the disease.1,13,15 Although recognized as a distinct clinicopathologic entity, 3 MAC has proven to be diagnostically challenging as it can mimic other similar neoplasms.3,6,16,17 Consequently, in addition to its rarity, there is often inadequate initial treatment. Clinically, MAC typically manifests as an indurated, growing flesh-colored plaque although variations of clinical morphology have been reported.1,4,11–18 Microscopically, the tumor often extends beyond clinical margins, spreading locally into the dermal, subcutaneous, and occasionally perineural tissues. 4 Histological features of MAC include infiltrated well-differentiated nests and cords of keratinocytes displaying follicular and ductal differentiation in a sclerotic stroma. 5 Treatment modalities that have been used for MAC include excision, the Mohs surgery, radiation therapy, and chemotherapy. 12
Case report
An 83-year-old Caucasian female initially presented to the Dermatology clinic incidentally while accompanying her husband for his appointment. She presented with progressive centrofacial induration of several centimeters, in which she did not pay much attention to until it was pointed out by the dermatologist that her nose appeared quite vascular and large, and was found to be extremely hard on palpation. Although history was vague, she had noted that her nose appeared to develop a more vascular appearance over the past 12 months or longer. The patient had no previous history of skin cancer, however was also diagnosed with squamous cell carcinoma (SCC) in situ of the right cheek and basosquamous carcinoma via skin biopsy of the right upper forehead at the same time of her initial visit, and these were subsequently excised without consequence. She has fair skin with a history of multiple sunburns as a child and background of long-standing chronic sun exposure. She denied the past use of tanning beds. She had a past medical history of malignancy of the colon, long-standing hypertension, osteopenia, and atrial fibrillation.
On examination, the patient’s nose and perinasal area were noted to be extremely indurated with prominent telangiectasia. This would be certainly atypical for phymatous rosacea. Other than an indurated raised plaque and prominence of the border of the lesion extending beyond the left lateral nasal sidewall, there was no clear solitary nodule or plaque other than a grossly large and firm, telangiectatic nose. The induration extended beyond the borders of the nose up toward the medial canthi, laterally beyond the nasolabial folds, and then lowers onto the lip bilaterally, as roughly drawn in Figure 1. No cervical or supraclavicular lymphadenopathy was detected on examination.
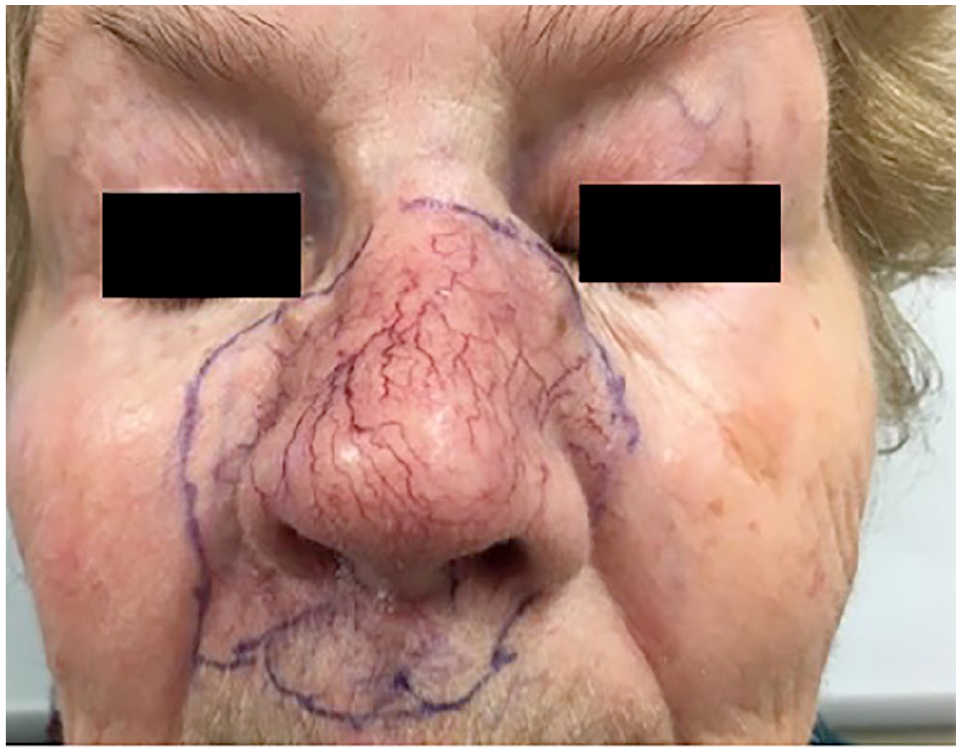
Deep clinical palpable margins of the MAC neoplasm prior treatment.
Three punch biopsies were taken from indurated areas of the left nasal sidewall, nasal bridge, and right nasolabial fold. Histopathology revealed features consistent with MAC and consisted of infiltrative dermal ductal structures with cords, squamous nests with horn cysts, and basaloid cells with surrounding sclerotic stroma with a mild chronic inflammatory infiltrate (Figures 2 and 3).

Histology image of MAC at 600 µm.

Histology image of MAC at 200 µm.
Due to the extent of centrofacial involvement, it was considered that surgical management would be quite disfiguring and difficult, such that it would require removal of the entire nose, surrounding tissue, and possibly requiring skin grafting as well as prosthesis. Radiation therapy was therefore chosen as the treatment modality. The patient was sent for a computed tomography (CT) scan of the neck, as well as a magnetic resonance imaging (MRI) of the area in question to better delineate soft tissue involvement prior to starting treatment.
CT scan revealed a destructive lobulated soft tissue mass invading the left nasal bone extending posteriorly into the nasal septum and anteriorly into the subcutaneous fat and the skin causing skin thickening, and crossing the midline to the right side. There was no evidence of cervical lymphadenopathy, no metastasis into the orbits, nasopharynx, oropharynx, laryngopharynx, skull base or into the lungs.
The MRI of the face revealed similar findings. Correlating clinically with the firm plaque of the left upper nasal sidewall, a multicystic soft tissue lesion was highlighted, invading the left nasal bone with involvement of the anterior nasal septum and the overlying skin causing thickening of the skin. The left orbit was spared. There was no imaging evidence of adjacent local structure invasion or distant metastasis.
Due to the physical examination, CT scan, and MRI findings, the patient received a total dose of 66 Gy in 33 fractions of external beam radiation therapy over the course of a month to the entire nose, upper lip, inner canthi, and lower midline of the forehead with a custom mold. During the treatment course, she experienced significant erythema, moderate desquamation, and mild irritation to the eyes (Figure 4). Overall, the patient responded well to the treatment and, as a result of the radiation, the neoplasm had started to soften and regress.

Radiation dermatitis during the course of radiation treatment.
Unfortunately, 2 months later, following the completion of the radiation treatment, she presented with post-radiation obstructive fibrosis of the nasal cavities, leading to breathing difficulty and underwent a septorhinoplasty 1 year later. One-month post-radiation and 1-year post-radiation photos are shown in Figures 5 and 6.

1-month post-radiation therapy.

1-year post-radiation therapy.
MRI of the head and neck 6-month post-radiation treatment reported showed no active or new disease, with only non-specific amorphous enhancement of the area consistent with post-treatment areas. Two years following completion of radiation treatment, the area had softened significantly clinically, and the nose and perinasal area had shrunk with no further activity (Figure 7). Two 3 mm punch biopsies were completed from the right and left nasal sidewall. The scouting biopsies were negative for MAC, but showed residual dense fibrous scar tissue that is likely a result from previous radiation treatments. The patient is continuing to receive ongoing assessment.
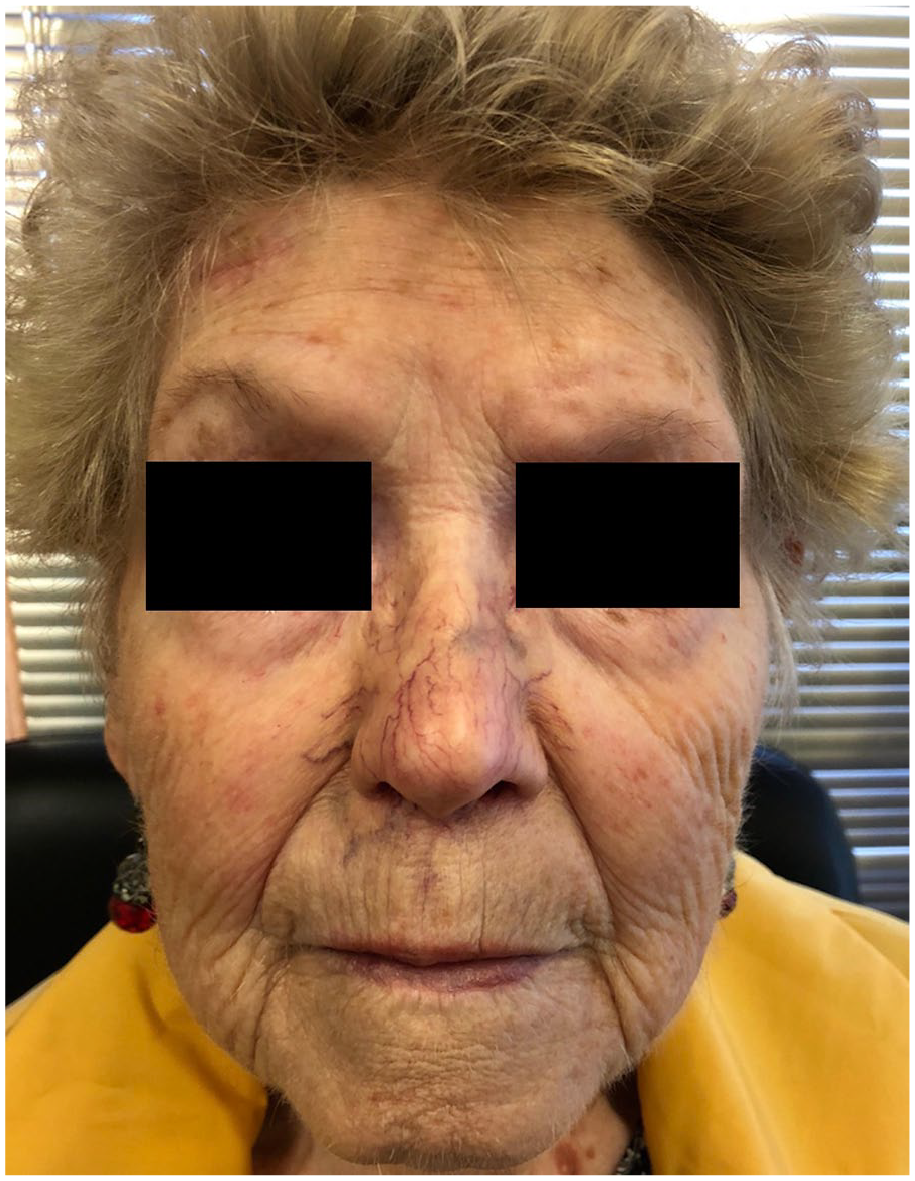
2-year post-radiation therapy.
Discussion
MAC is a challenging entity to diagnose and treat. It often presents as an indolent, non-ulcerated, smooth-surfaced, flesh-colored to yellowish asymptomatic nodule, papule, plaque, or cystic lesion with indistinct margins with a predilection for the head and neck, predominantly arising in the central face.1,4,11–18
It is paramount to include MAC as a differential diagnosis among the other head and neck lesions to enable early diagnosis and treatment to reduce morbidity and mortality. Deep incisional or excisional biopsy for histopathology is the gold standard for initial diagnosis.16,17
Mohs is considered the gold standard of treatment for MAC. To date, there is insufficient evidence whether radiation is an effective monotherapy in patients with MAC due to rarity of the disease and the limited use as a management option.2,4,11–18 Due to radiation therapy resulting in worsening of one MAC case and being a risk factor for MAC, radiation as monotherapy should be considered prudently. 1 Radiation may also be sought as treatment when standard surgical therapy may prove difficult and result in poor cosmetic outcome. In this case report, we have described an atypical case of MAC presenting as progressive centrofacial induration of several centimeters and demonstrated radiation as an effective treatment modality with a 2-year follow-up in our patient including scouting biopsies showing no clinical recurrence of MAC. Given the high rates of false negatives with punch biopsies, if the scouting biopsies are negative and there is still a clinical suspicion of disease, they should be followed up with a deeper excisional biopsy.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Verbal informed consent for patient information and images to be published was provided by the patient.
